
Navigating Orthopedic Pain After a Denied Second Opinion
A denied second opinion can make orthopedic pain management feel strangely upside down. The body still hurts, the paperwork has already said no, and now every next step seems to cost either money, time, or both.
This is where many people lose traction. They freeze, overspend on the wrong visit, or start chasing scans and specialists before they know what problem actually needs solving. Meanwhile, pain keeps leaking into sleep, work, driving, stairs, laundry, and the thousand small mechanics of ordinary life.
The real risk is not just the denial. It is building the next move badly and paying for confusion twice.
What helps is a cleaner strategy. This guide is built to help you manage orthopedic pain after denied second opinion coverage in a way that protects function, sharpens documentation, and helps you choose between appeal, conservative care, in-network reassessment, or a focused self-pay consult without spiraling into panic spending.
It takes a practical view of medical necessity, referral rules, prior authorization issues, physical therapy notes, imaging decisions, and function loss because those details are usually what make the difference.
Start here. Because the smartest next step is rarely the loudest one, and a calmer case is often a stronger case. More importantly, a stronger case can also be a cheaper one.
Table of Contents
Fast Answer: Orthopedic pain management after denied second opinion coverage is usually not about “doing nothing until insurance says yes.” It is about controlling pain, protecting mobility, documenting what has already failed, and choosing the cheapest next step that still answers a real medical question. In practice, that often means pairing conservative care with a clean appeal or a focused lower-cost consult instead of drifting into panic spending.
Safety / Disclaimer: This article is educational. It is not medical diagnosis, legal advice, or a substitute for your own clinician’s guidance. If you have severe or worsening weakness, numbness, fever, swelling, loss of function, new symptoms after trauma, or a time-sensitive concern your treating clinician is worried about, seek prompt medical care. HealthCare.gov explains that insurers must tell you why a claim was denied and how to appeal, and official appeal timelines can matter.
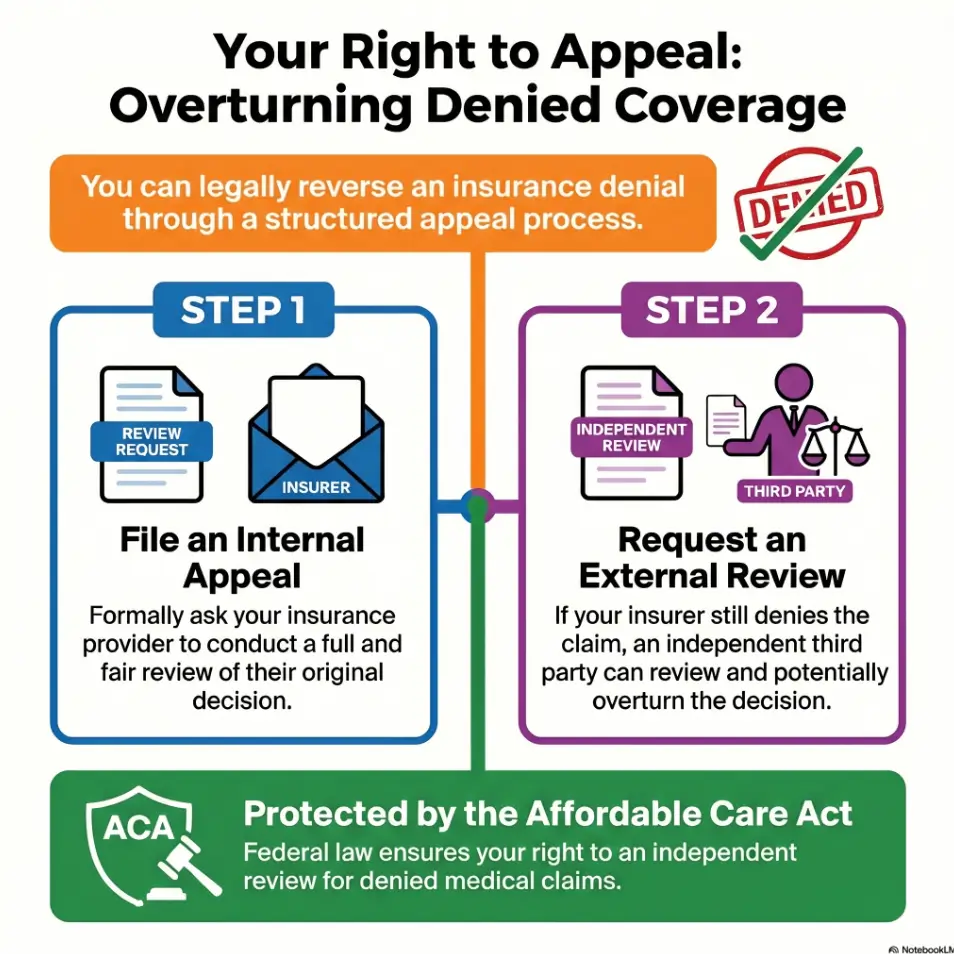
Denied Coverage, Now What Actually Matters First
The first split: pain control versus paperwork panic
The first job is not to win an argument with an insurance company in your head at 1:12 a.m. The first job is to answer a simpler question: Are you medically okay enough to work through this over days, or does something need attention now? When pain spikes, the brain behaves like a smoke alarm with a theater degree. Everything feels urgent. Not everything is.
Start with three lanes. Lane one is body status: pain severity, new weakness, swelling, fever, numbness, or sudden loss of function. Lane two is function: can you walk, sit, lift, sleep, drive, work, or care for yourself better, worse, or much worse than last week? Lane three is paperwork: what exactly did the denial say?
I once watched someone spend 40 minutes doom-scrolling denial forums before noticing the letter was mainly about referral routing, not a judgment that the visit itself was absurd. That is the kind of mix-up that turns a solvable problem into a month-long fog.
How to decide what needs medical follow-up today versus what can wait a few days
If symptoms are stable and familiar, a short delay to organize records is often reasonable. If symptoms are rapidly worsening, unusual, or paired with red flags, stop treating this like a customer-service puzzle and get medical advice promptly. Orthopedic pain can be annoying, stubborn, and expensive. It can also occasionally be a signal that timing matters more than billing strategy.
A useful litmus test is this: are you mostly trying to get a better opinion, or are you suddenly losing function? Those are not the same problem. A denied second opinion may be frustrating but survivable; a leg that suddenly gives out on stairs is a different story entirely.
Why the denial letter is not just admin clutter, but the map for the next move
Read the denial letter like a mechanic reads dashboard lights. You are looking for the exact reason code or wording: out-of-network, no referral, prior authorization missing, not medically necessary, benefit exclusion, duplicate specialist evaluation, or incomplete documentation. HealthCare.gov states that insurers must explain why they denied a claim and how you can dispute it, which makes the letter less like junk mail and more like the instruction card for your next move.
- Red-flag symptoms change the timeline immediately
- Stable pain gives you room to organize evidence
- The denial reason determines the best next step
Apply in 60 seconds: Circle or highlight the exact denial reason on the letter before doing anything else.
Who This Is For, and Who It Is Not For
This is for insured US patients trying to manage orthopedic pain after a denied second opinion
This guide is for the person with knee pain, back pain, shoulder pain, neck pain, joint pain, or post-injury frustration who is trying to act wisely under financial and administrative pressure. You want relief, but you also want to avoid paying $400 for a visit that tells you something you could have learned another way. Fair. Very fair.
This is for readers comparing appeal, self-pay, and conservative-care paths without wasting money
It is also for people trying to decide whether to appeal, ask their primary care doctor for a tighter referral, return to physical therapy, seek an in-network reassessment, or pay cash for one carefully chosen consult. The goal is not perfect health bureaucracy. The goal is a clear next move that protects function and cuts waste.
This is not for emergencies, severe new neurologic symptoms, or post-injury instability that needs urgent evaluation
If you have severe or worsening weakness, major numbness, inability to bear weight, new trauma, fever with swelling, or a clinician warning you that delay may matter, this article stops being enough. Use it later for the insurance maze. Right now, use medical judgment first.
That distinction matters because insurance fights tempt people into a strange pride. We start acting as if being “right” on paper is the same as being safe in a body. It is not. A claim can be improperly denied and still not be the most urgent thing in the room.
Pain Strategy First, Pride Second
How to stabilize daily life while the coverage fight is still unresolved
The honest work of this phase is unglamorous. Reduce aggravating movements. Use the pain plan your clinician already recommended. Protect sleep like it is part of treatment, because it is. Adjust workload, errands, and lifting patterns. Use braces or supports only as directed, not as little pieces of emotional armor you collect at 2 a.m. from online carts. If you are comparing costs, it can also help to understand which HSA-eligible braces and supports may fit into the broader budget picture.
When my own shoulder flared years ago, the hardest part was not the pain itself. It was the humiliating comedy of tiny tasks. Pulling on a T-shirt felt like negotiating with a spiteful octopus. The lesson was simple: function matters more than bravado. If a temporary modification helps you move through the week without making things worse, that is not weakness. That is strategy.
What “conservative care” often includes before a specialist revisit becomes easier to justify
Conservative care often means some combination of rest from provoking activities, guided movement, home exercises, medication counseling from your clinician, physical therapy, follow-up monitoring, and documented response over time. This is important for two reasons. First, it may actually help. Second, it creates the record insurers often want to see before they view a second opinion as medically necessary rather than preference-driven. If you are trying to understand that threshold more clearly, it helps to see how failed conservative care is often framed before MRI approval.
Let’s be honest, the hardest part is often not pain alone but uncertainty layered on top of it
Pain with a plan is tiring. Pain with no plan becomes weather. People start asking, “Should I wait? Should I pay? Is this getting worse? Am I being cheap with my own body?” That uncertainty is where bad spending happens. The fix is not motivation. It is structure.
Eligibility checklist: Is conservative care a reasonable bridge for the next few days?
- Yes if symptoms are stable and you already have a clinician-guided pain plan
- Yes if function is limited but not collapsing quickly
- No if you have new weakness, major swelling, fever, trauma, or sudden loss of function
- No if your treating clinician says delay may change outcomes
Neutral next action: write down what worsens pain, what eases it, and what daily task is most affected.
Show me the nerdy details
From an insurance perspective, conservative care creates a timeline. From a clinical perspective, it tests response and gives later imaging or specialist review more context. From a wallet perspective, it can keep you from stacking duplicate visits that answer the same question poorly.

Denial Language Decoded Before You Spend Another Dollar
What “not medically necessary” usually signals in a second-opinion denial
This phrase often sounds like an insult. It usually is not. In plan language, it often means the insurer does not yet see enough documentation that the second opinion changes management, addresses failed treatment, resolves uncertainty that affects care, or meets plan criteria. That does not mean your pain is trivial. It means the paper trail is weak, incomplete, or misaligned with the rule being applied.
How referral rules, network rules, and prior authorization problems get mistaken for the same thing
These are cousins, not twins. A network issue means the doctor may be outside the approved plan structure. A referral issue means the gatekeeping step was missing or malformed. A prior authorization issue means approval was required before the visit. A medical-necessity issue means the plan is unconvinced the consult is justified under its terms. People blur these together, then write appeals that solve the wrong problem with great passion and zero effect.
A cleaner approach is to write one sentence: “The denial appears to be for X, not Y.” That single sentence can save a week of flailing.
Why one missing note can make a reasonable case look weak on paper
A missing physical therapy progress note, absent functional limitation, or vague referral can make a strong real-world case look flimsy in administrative language. Insurers review documents, not your tone of suffering. Unfair? Sometimes. Important? Absolutely. CMS explains that the ACA appeal framework gives consumers rights to challenge adverse plan decisions, but rights still travel through documentation.
- Network problems need routing fixes
- Authorization problems need process fixes
- Medical-necessity problems need documentation fixes
Apply in 60 seconds: Rewrite the denial reason in plain English on one line.
Common Mistakes That Make the Situation More Expensive
Paying out of pocket too fast without asking what records would strengthen an appeal
There are times when cash pay is the fastest smart move. There are also times when it is just retail therapy in a white coat. Before paying cash for a second opinion, ask what exact question the visit will answer and what missing documents could strengthen either the appeal or the value of that consult. A rushed self-pay visit with incomplete records can become a very expensive shrug. For a broader sense of what patients are often quoted, compare the logic here with typical self-pay cash price ranges for orthopedic care.
Treating the second opinion itself as the only solution instead of clarifying the decision you need made
What decision do you actually need? Whether surgery is necessary? Whether a brace should continue? Whether imaging changes treatment? Whether you should stop PT? The better the question, the more strategic the next visit. A second opinion is a tool, not a sacrament.
Confusing pain escalation with proof that every higher-cost test must happen now
Pain matters, but it does not automatically settle the imaging question or specialist question by itself. A scan can be helpful. It can also become a glittering distraction. Many people burn energy chasing the image because it feels concrete, when the real issue is still a treatment decision that depends on symptoms, function, and progression. That is especially true when there is already a risk of MRI findings not matching the actual pain picture.
One of the costliest patterns I see is the stack: urgent care, duplicate specialist, random telehealth, imaging consult, then back to the original doctor with a bag full of PDFs and no coherent story. The body hurts. The wallet gets dizzy. Nobody is happy.
Decision card: When should you appeal first, and when should you consider a quick self-pay consult?
- Appeal first when the denial looks procedural, your symptoms are stable, and your records are incomplete but fixable
- Consider self-pay first when you need one focused decision quickly, can gather good records now, and the wait itself is causing meaningful function loss
Time/cost trade-off: appeals cost time and attention; cash consults cost money and still may not solve plan coverage later.
Neutral next action: ask the office for the self-pay rate before scheduling anything.
Do Not Build the Case Backward
Why readers lose momentum when they collect bills before they collect evidence
It is tempting to start with receipts because they feel like proof. But bills mostly prove that health care is expensive, which, to be fair, was never in serious doubt. What you need first is a clean sequence: symptom onset, prior evaluation, treatment attempts, function changes, and the decision the second opinion is meant to inform.
Think of this as building a small bridge, not a dramatic bonfire. Each plank should help an insurer, clinician, or you answer the next reasonable question.
The smarter sequence: symptoms, prior treatment, functional limits, denial reason, requested review
A one-page timeline is often more powerful than a stack of emotional paragraphs. Start with date or rough week of symptom onset. Add what you tried. Add what changed. Add the denial reason. Then add why another review would affect treatment decisions. That last step matters. You are not merely asking for validation. You are showing decision impact.
Here’s what no one tells you: vague suffering is emotionally real but administratively weak unless translated into function loss
“It hurts a lot” is true, but “I wake three times a night, cannot sit through a work meeting, and had to stop carrying groceries upstairs” is often more useful. The first sentence expresses pain. The second expresses consequences. Plans, clinicians, and even your own stressed brain respond better when pain is translated into function.
Short Story: A reader once told me her denial made her feel like she had to sound more dramatic to be taken seriously. She almost wrote a two-page appeal full of anger and exhausted honesty. Instead, she made a one-page list: symptoms for six weeks, PT visits completed, pain during stairs, inability to lift laundry, missed work focus, and the exact question the second opinion needed to answer about whether to continue current care or change course.
The result was not magic. The system did not suddenly grow a soul and a cello soundtrack. But the case became legible. Her doctor’s office added two missing notes, the appeal stopped sounding like desperation, and every later conversation became easier because the facts were finally lined up in the same direction.
Infographic: Build the case in this order
When they started and how they changed
What you tried and what happened
Sleep, work, walking, lifting, stairs
Referral, network, authorization, necessity
What decision the second opinion will help answer
Lower-Cost Paths When the Formal Second Opinion Is Not Covered
When a primary care doctor, sports medicine visit, or physical therapy reassessment can move the case forward
Sometimes the bridge is not glamorous, but it is effective. A primary care visit can tighten documentation. A sports medicine or in-network musculoskeletal reassessment may answer enough to guide next steps. A physical therapy reassessment can document progress, plateau, or decline in terms insurers and specialists actually use. In other words, the second opinion may not be the only doorway into clarity. In some cases, continuing or revisiting core orthopedic pain management strategies is the move that keeps the case both medically and financially coherent.
How self-pay pricing for one focused consult may be more strategic than uncontrolled repeat visits
If you do go cash-pay, go with discipline. Ask for the self-pay rate, what records the specialist wants in advance, whether imaging needs to be in hand, and what exact question the visit can answer. One tight consult can be more useful than three cheaper visits that never quite reach the point.
When telehealth chart review or in-network specialist reassessment may be the bridge, not the compromise
Some cases benefit from a chart-review style second look, especially if the question is whether current treatment makes sense or whether a change should be discussed with the original clinician. This is not always available and not always sufficient, but it can be a practical bridge when geography, timing, and coverage all behave like difficult cousins at the same reunion.
I like to think of lower-cost paths as scaffolding, not surrender. They hold things steady while you decide whether to invest more.
Quote-prep list: Gather these before comparing self-pay options.
- Visit type and exact cash rate
- Whether records or imaging are required beforehand
- How long the visit is and whether a treatment recommendation is included
- Whether the office provides a detailed note you can use in an appeal
- How soon you can be seen
Neutral next action: call two offices and compare total value, not just sticker price.
Appeal Without Sounding Like You Are Begging
What a strong appeal angle looks like in orthopedic pain cases
A strong appeal usually sounds calm, specific, and almost boring. That is good. State the denial reason. State the relevant history. State failed or incomplete response to prior care. State the function loss. State what medical decision the second opinion will inform. Drama is satisfying. Clarity is effective.
How to frame medical necessity around function, failed treatment, and decision impact
Medical necessity arguments are stronger when they explain why the additional review affects care. Maybe treatment has plateaued. Maybe two reasonable paths exist and a second specialist evaluation would help avoid unnecessary escalation. Maybe persistent limits after conservative care make another expert assessment relevant. Tie the requested review to the decision, not just the feeling of wanting reassurance.
Which documents usually matter more than dramatic language
Often useful documents include clinician notes, referral notes, PT progress notes, prior imaging reports if any exist, medication or treatment history, and a short patient timeline showing function loss. HealthCare.gov says internal appeals generally must be filed within 180 days after receiving the denial notice, and urgent health situations may follow different timelines, so document gathering should move with enough speed to protect your deadline.
I have seen appeals become dramatically better after one boring addition: a cleaner PT note showing what remained limited after a defined block of therapy. Boring can be beautiful when it changes the administrative picture. If your problem is not just the second opinion but the scan path around it, you may also want to compare this with the logic behind an MRI denial appeal in orthopedic pain management.
- Lead with the denial reason
- Connect symptoms to function loss
- Explain how the second opinion affects next-step care
Apply in 60 seconds: Draft one sentence that begins, “This additional review is needed to help decide whether…”
Show me the nerdy details
Appeals often fail because they answer the wrong question. “I am still in pain” may be true, but “persistent symptoms after documented conservative care are limiting function and another specialist evaluation would guide whether to continue, modify, or escalate treatment” is closer to the logic insurers evaluate.
When to Push, When to Pause, When to Pivot
Signs the appeal path is worth the effort
Push when the denial looks procedural, your records are reasonably strong, the requested second opinion is likely to influence treatment, and your symptoms are serious enough to matter but stable enough to allow a structured process. Push especially when your treating clinician’s notes support the need for more evaluation.
Signs a lower-cost second look may be faster than waiting
Pivot when the appeal timeline is long, the self-pay rate is manageable, the needed question is narrow, and the answer could materially change what you do next. The self-pay consult may still support a later appeal or at least stop you from wasting two more months on indecision.
Signs the current treatment plan itself needs re-evaluation even before another opinion
Pause and reassess when the real issue is not “I need another specialist” but “the current plan no longer makes sense.” If pain management, PT, work modifications, or follow-up strategy have become stale, another second opinion may be less urgent than a more grounded check-in with the clinician already in the picture.
There is a quiet dignity in changing tactics without calling it defeat. The body does not care whether your plan feels elegant. It cares whether the next step is useful.
Mini calculator: Is a focused self-pay consult financially tolerable?
- Estimated self-pay consult cost: $_____
- Estimated lost work/productivity or repeated visit costs over the wait: $_____
- Estimated time to appeal outcome: _____ weeks
Output: If the wait is likely to cost you more than the consult and the consult could change treatment decisions, a cash visit may be strategically reasonable.
Neutral next action: compare one realistic self-pay quote against one realistic month of delay costs.
Do Not Let Imaging Become the Whole Story
Why readers often chase scans when the real problem is decision uncertainty
Imaging feels like truth with a glossy finish. But a scan is only as helpful as the decision it informs. If no one has explained what the result would change, the test can become emotional decor: expensive, seductive, and oddly unhelpful. In orthopedic care, symptoms, exam findings, function limits, and progression still matter. That is one reason many readers benefit from understanding how MRI referral decisions are usually approached in orthopedic pain before assuming a scan is the obvious next move.
How pain, weakness, sleep loss, and activity limits create a fuller clinical picture
A useful clinical picture is broader than a single report. Sleep disruption, inability to climb stairs, worsening walking tolerance, trouble lifting, reduced range of motion, repeated flare pattern, and work limitations all shape what should happen next. Sometimes that picture strengthens the case for more testing. Sometimes it supports a different treatment trial first.
When documenting progression matters more than repeating the same complaint
“Still hurts” is not useless, but “worse after six weeks despite modified activity and PT, now affecting sleep and work concentration” is more clinically and administratively meaningful. Progression is information. Pattern is information. Repetition without detail is mostly a sigh.
I remember speaking with a friend who wanted “just the MRI” because it felt like progress. What she actually needed was a clearer conversation about whether imaging would change treatment. Once that question was asked, the room got much calmer.
- Document progression, not just persistence
- Track function, not just pain score
- Ask what result would actually change care
Apply in 60 seconds: Write down one concrete thing a scan result would change in your current plan.
Money Friction, Family Friction, Work Friction
How denied second opinion coverage spills into job performance, caregiving, and mental bandwidth
Orthopedic pain rarely stays in its lane. It leaks into spreadsheets, school pickup, grocery bags, laundry baskets, commutes, and sleep. It makes a patient feel like a logistics manager for a body that missed a staff meeting. When a denial arrives, that burden doubles. Now you are not only hurting. You are coordinating records, calls, deadlines, and costs.
This matters because the “best” choice medically can become the worst choice practically if it collapses your work week or caregiving capacity. A plan that looks neat on paper may be unusable in real life.
Why a useful article should address time cost, not just bill cost
Bill cost is visible. Time cost hides in plain sight. An hour on hold with an insurer. Two half-days rearranged for appointments. The mental tax of retelling your story to every office. The extra exhaustion from pain-fragmented sleep. All of this belongs in the decision. For readers on cost-sensitive plans, it also helps to think through the broader logic of orthopedic pain management with a high deductible rather than treating this denial as an isolated expense.
Small systems for tracking appointments, symptoms, and insurer calls without burning out
You do not need a gorgeous color-coded life dashboard. You need one page or one note with dates, symptoms, treatment attempts, function limits, and every insurer call. Record who you spoke to, when, and what was said. The point is not perfection. The point is reducing rework.
Coverage tier map: What kind of denial problem are you actually dealing with?
- Tier 1: Missing referral or paperwork. Usually the easiest fix.
- Tier 2: Prior authorization issue. Often fixable with proper resubmission.
- Tier 3: Network mismatch. May require rerouting or stronger justification.
- Tier 4: Medical necessity denial. Requires function-based evidence.
- Tier 5: Benefit exclusion or complex plan limitation. Often the hardest path.
Neutral next action: label your situation by tier before choosing appeal, reroute, or cash pay.
The practical tenderness here is simple: make the system smaller. One page. One question. One next step. Pain loves chaos. Recovery usually prefers order.
When to Seek Help
Severe or worsening pain with sudden weakness, numbness, fever, swelling, or loss of function
If symptoms are escalating fast, becoming neurologic, or showing signs of infection, inflammation, instability, or urgent impairment, do not let a denied second opinion coverage letter become the villain of the whole story. The letter may matter later. Right now the body matters more. If low back symptoms are part of the picture, review the warning signs that can make low back pain an emergency rather than a routine insurance battle.
New symptoms after trauma, surgery, or immobilization
Any meaningful new symptom after a fresh injury, surgery, or immobilization deserves more caution. Timing can matter. The point is not to scare you. The point is to resist the false calm that paperwork can create. A denial is administrative. Your body is not.
A denial situation that is delaying care your treating clinician believes is time-sensitive
If your clinician tells you delay could affect outcomes, make that fact visible immediately in your follow-up and appeal steps. HealthCare.gov notes that urgent health situations may have faster review pathways, and external review rights may apply in eligible cases after internal steps or in some urgent situations.
FAQ
Can I still get orthopedic pain treatment if my insurance denied a second opinion?
Usually, yes. A second opinion denial is not the same thing as denial of all care. You may still be able to continue conservative treatment, follow up with your existing clinician, get an in-network reassessment, or use lower-cost options while deciding whether to appeal.
What is the difference between a second opinion denial and a treatment denial?
A second opinion denial usually concerns coverage for another specialist evaluation. A treatment denial concerns a recommended intervention itself, such as therapy, imaging, injection, or surgery. They can overlap, but they are not identical. Read the denial language carefully before responding.
Can I appeal a denial for a specialist second opinion?
Often, yes. HealthCare.gov explains that consumers generally have internal appeal rights when a claim is denied, and some denials may later qualify for external review. The strength of the appeal usually improves when it explains why the second opinion affects treatment decisions and includes clean documentation.
Is it worth paying cash for a second opinion after insurance says no?
Sometimes. It may be worth it when the question is narrow, the clinician is well chosen, records are ready, the self-pay rate is clear, and the answer could materially change what you do next. It is less worth it when the visit would simply duplicate what you already know. If your main hesitation is financial, it may help to compare expected visit costs with the broader pattern described in HDHP imaging cost estimates.
What records help prove medical necessity in orthopedic pain cases?
Helpful records often include prior clinician notes, PT progress notes, referral documentation, prior imaging reports, treatment history, and a short timeline showing function loss and symptom progression. Specificity usually beats drama.
Can physical therapy notes help an insurance appeal?
Very often, yes. PT notes can show what has been tried, whether function improved, plateaued, or worsened, and how symptoms affect daily tasks. That kind of detail can make a case look more medically grounded. Readers dealing with cost questions around rehab may also find it useful to understand the difference between physical therapy copay and coinsurance.
What should I do if my pain gets worse while I wait?
Reassess the situation medically, not just administratively. If symptoms are worsening significantly, new red flags appear, or function drops quickly, contact your clinician or seek prompt care. Waiting is only a sensible strategy when the body is stable enough to support it.
Does an external review apply to second-opinion denials?
It can in eligible cases, but not every denial follows the same path. HealthCare.gov states that external review is a formal step available for certain denials after the insurer’s process or, in some urgent situations, on an expedited basis. The exact path depends on your coverage type and the nature of the denial.
Next Step
Pull the denial letter, highlight the exact denial reason, and build one one-page timeline of symptoms, prior treatments, function loss, and what decision the second opinion is needed to answer
This is the move that turns indignation into traction. In the next 15 minutes, do four things. Pull the denial letter. Highlight the exact reason. Start a one-page timeline. Then write one sentence beginning with: “The second opinion is needed to help decide whether…” That sentence becomes the spine of almost everything that follows, whether you appeal, reroute in network, or pay cash for a focused consult.
That is the curiosity loop from the beginning, closed honestly: the goal was never to become a better insurance philosopher. The goal was to stop freezing. Once the case is legible, the next step gets smaller, cheaper, and less haunted.
Last reviewed: 2026-04.
