
Mastering the Morning:
Safer Independence After Hip Surgery
You do not realize how dramatic a sock can become until your hip has rules.
After hip surgery, one small morning task involves balance, bending limits, and the quiet panic of not wanting to do something wrong. Putting on socks is not really about socks—it is about protecting your new hip from deep bending, awkward twisting, and risky reaches.
This guide provides a calmer, no-bend routine using professional methods from occupational therapy. Learn to set up your dressing station, use the right tools, and avoid common hip-precaution mistakes.
- ✔ Start with a firm chair.
- ✔ Let the tool do the bending.
- ✔ Keep the morning boring—that is where safety begins.
Table of Contents
Fast Answer
After hip surgery, the safest way to put on socks without bending too far is usually to sit in a firm, high chair and use a sock aid, reacher, or caregiver help instead of folding forward toward your foot. Many hip-replacement instructions warn against bending the hip past 90 degrees, crossing legs, or twisting, especially with posterior hip precautions. Always follow your surgeon’s or physical therapist’s specific rules.
- Sit in a firm chair with armrests when possible.
- Use a sock aid instead of bending toward your foot.
- Stop if you feel sharp pain, dizziness, or a shifting sensation.
Apply in 60 seconds: Put one easy pair of socks, your sock aid, and your phone beside your dressing chair tonight.

Safety / Disclaimer Block
Your surgeon’s discharge instructions outrank any general dressing tip online. That sentence deserves a little brass plaque above the laundry basket.
Some people leave the hospital with strict hip precautions. Others have fewer restrictions depending on surgical approach, implant type, medical history, balance, age, and recovery progress. A person recovering from a posterior total hip replacement may be told to avoid bending the hip past 90 degrees, crossing legs, or twisting. Another patient may receive different guidance. The sock does not know your surgical approach. Your care team does.
The American Academy of Orthopaedic Surgeons describes using a higher chair when posterior hip precautions are given, and MedlinePlus patient instructions describe avoiding leg crossing and deep hip bending after hip replacement. These are general guardrails, not a personal permission slip. If you are comparing broader recovery supports, a practical guide to orthopedic home care equipment can help you separate useful tools from clutter.
When to seek help
- New sharp hip pain while dressing
- A sudden “pop,” shifting feeling, or inability to move the leg normally
- New leg shortening, severe weakness, or the foot turning unusually inward or outward
- Dizziness, near-falls, or needing to hold your breath to reach your foot
- Swelling, redness, fever, wound drainage, or worsening pain after activity
Practical rule: if dressing makes you feel unsafe, stop the task before your body starts improvising.
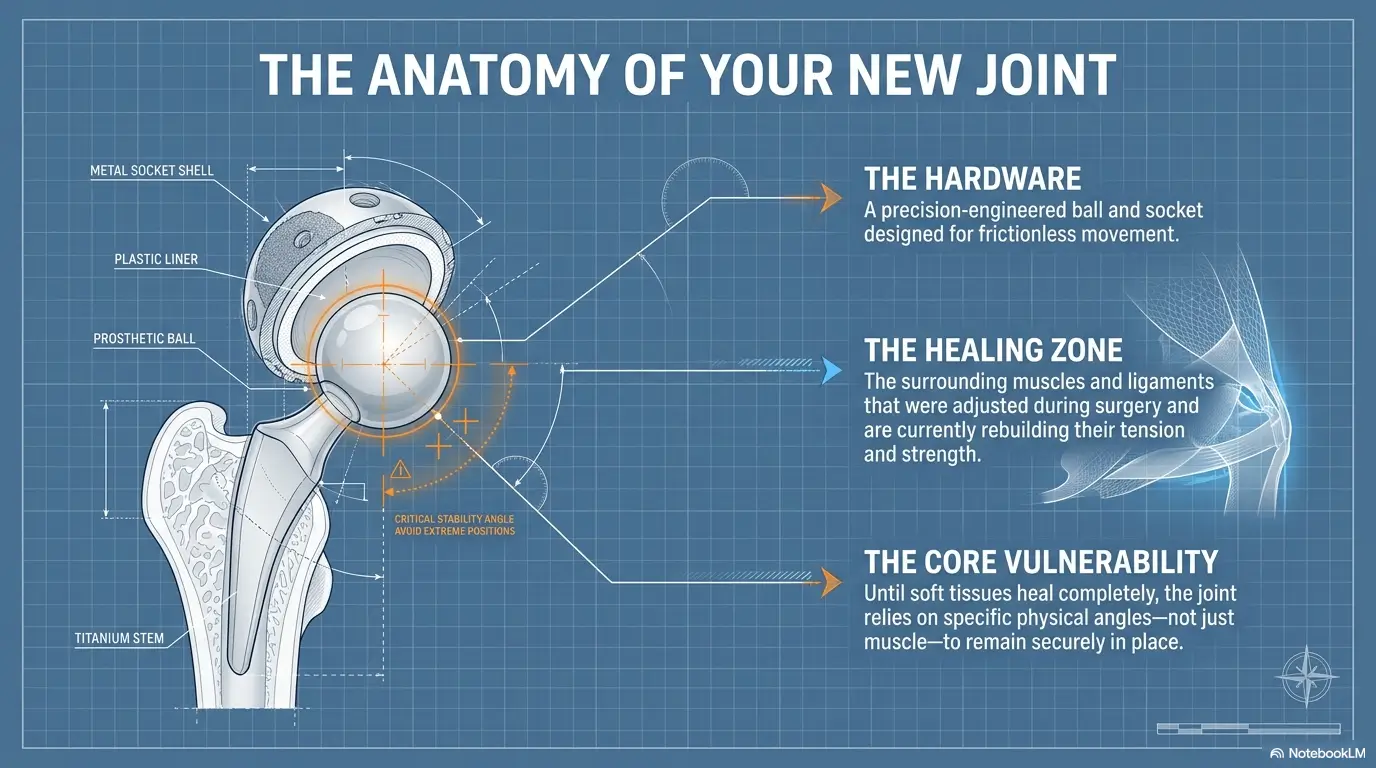
Start Here: The Sock Problem Is Really a Hip-Angle Problem
Socks feel like the problem because they are the visible object. They sit there on the floor with their tiny elastic mouth, looking innocent. But after hip surgery, the real issue is often the angle between your torso and thigh.
Before surgery, you may have put on socks while bent forward on the bed, standing on one leg, or crossing one ankle over the opposite knee. Those moves are so normal that your brain files them under “morning nonsense.” After hip surgery, the same moves can bring your hip into positions your care team may have told you to avoid.
Why socks become strangely hard after surgery
Putting on socks usually requires three things at once: bending, reaching, and controlling the foot. That is a lot of small machinery for a healing hip.
I once watched a family member stare at a sock aid like it was a suspicious kitchen gadget. Thirty seconds later, they said, “So the tool does the bending for me?” Exactly. The tool is not about weakness. It is about outsourcing the risky angle.
The hidden risk: reaching feels small, but the hip angle is not
A reach can feel tiny in the upper body while becoming large at the hip. This is why “I only leaned a little” can be misleading. Low chairs, soft beds, and socks that fall near the toes can quietly increase the bend.
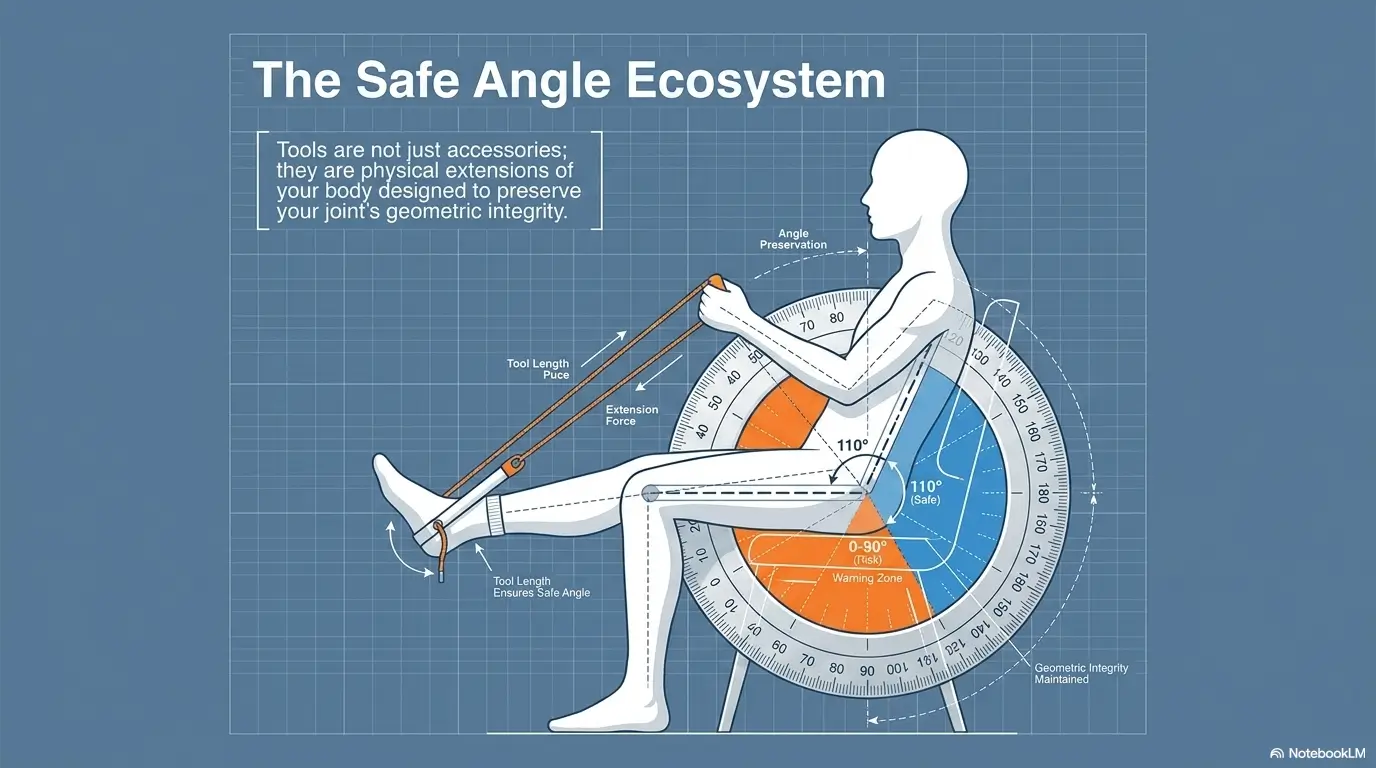
The 90-degree rule, explained without turning your morning into geometry class
If your care team gave you a 90-degree bending limit, imagine your hip as a hinge that should not close too tightly. Sitting upright with your knees lower than or level with your hips is usually less risky than sitting low with your knees high and your chest drifting toward your thighs.
You do not need a protractor. You need a better setup.
Pattern interrupt: the sock is not the villain
The villain is the rushed, low-seat, bent-forward, half-awake reach. The sock is merely the little cotton witness.
Show me the nerdy details
Many common hip precautions focus on avoiding combined positions that can stress the healing joint or increase dislocation risk, especially after certain surgical approaches. For sock dressing, the practical concern is not the sock itself. It is the combination of hip flexion, rotation, and adduction that can happen when a person bends forward, crosses the leg, or twists the foot to chase the heel into place.
Who This Is For / Not For
This guide is for the person who can walk past a kitchen table with dignity but gets humbled by one sock. It is also for the caregiver trying to help without turning a simple morning routine into a small wrestling match.
This is for early recovery patients with bending limits
If you are in the first weeks after hip replacement or another hip procedure and were told to avoid bending too far, crossing your legs, or twisting, this article is for you. The focus is home dressing, not athletic stretching, yoga poses, or proving anything to the furniture.
This is for caregivers setting up a safer morning routine
Adult children, spouses, home health aides, and friends can use this as a setup guide. The best help often happens before the person sits down: choosing the chair, clearing the floor, placing tools nearby, and making the sock easy to reach without bending.
This is not for people cleared to bend normally again
Once your surgeon or physical therapist clears you to return to normal bending, your routine may change. Until then, “I feel flexible today” is not the same as clearance.
This is not a substitute for occupational therapy instructions
An occupational therapist can show you how to dress based on your actual body, home, surgery, balance, and equipment. That kind of instruction is gold. This article is the map. Your therapist is the local guide who knows where the sidewalk cracks are.
- Use this as a conversation starter with your care team.
- Keep surgeon instructions visible near your dressing area.
- Ask for a demonstration before guessing at home.
Apply in 60 seconds: Write down this question: “What is my safe dressing position for socks and shoes?”
First Setup: Build a “No-Bend Dressing Station”
A safer sock routine starts before your foot goes anywhere near the sock. Think of it as building a tiny launchpad for your morning. Not glamorous, perhaps, but neither is getting stuck halfway into a sock with one hand on the dresser and regret in your eyes.
Choose a firm chair with arms, not a soft couch
A firm chair helps keep your hips higher and your posture steadier. Armrests give you something stable to use when sitting and standing. Soft couches, low recliners, and squishy mattresses can make your knees rise higher and your torso fold forward.
MedlinePlus patient instructions for hip replacement commonly warn against soft chairs, rocking chairs, stools, and sofas during recovery. That advice makes sense in real life. Soft seats swallow people. A firm chair gives the body a clearer exit plan.
Keep the operated leg forward before you start
When sitting down or standing up, many hip-precaution instructions recommend keeping the operated leg slightly forward. This can reduce deep bending at the hip. Do not force the position. Just avoid tucking the operated foot far under the chair.
Put socks, shoes, reacher, and sock aid within easy reach
Place everything on a side table, tray, or chair beside you. Not on the floor. Not across the room. Not in the mysterious drawer where batteries go to retire. This same task-first thinking also applies when families compare home care equipment that actually helps after orthopedic surgery.
- Sock aid
- Reacher or grabber
- Loose socks
- Long-handled shoehorn
- Phone or call button
Keep the floor boring: no rugs, no laundry piles, no tiny obstacle theater
The safest floor is a boring floor. Remove throw rugs, cords, pet toys, slippers, laundry, and anything that requires a little side-step. Recovery does not need surprise choreography.
Eligibility checklist: are you ready to dress without bending?
Yes/no checklist
- Yes / No: Do you know your current hip precautions?
- Yes / No: Can you sit in a firm chair without sinking?
- Yes / No: Are your sock aid and reacher within arm’s reach?
- Yes / No: Is the floor clear within 3 feet of your chair?
- Yes / No: Can you stop and ask for help without rushing?
Neutral next step: If any answer is “No,” fix that item before attempting socks alone.
Sock Aid Method: The Tool That Saves the Bend
A sock aid looks humble, almost too simple. That is its charm. It holds the sock open so your foot can enter without your torso chasing your toes.
The Royal National Orthopaedic Hospital patient guidance for hip precautions notes that occupational therapists may recommend equipment such as a stocking or sock aid and a long-handled shoehorn after hip replacement. In the home, that little tool can become the difference between “I dressed safely” and “I accidentally invented a dangerous yoga pose.”
Slide the sock onto the aid before it touches the floor
Load the sock while the sock aid is in your lap. The heel of the sock should face the correct direction, and the toe should be pulled snugly over the end. If the sock is twisted before your foot enters, it will not become more cooperative later. Socks are rarely moved by moral persuasion.
Lower the sock aid with straps instead of leaning forward
Hold the straps or handles and lower the sock aid to the floor. Your hands move. Your torso stays tall. This is the entire magic trick.
Guide the foot in slowly, without twisting the hip
Keep your knee and toes pointed in a safe direction based on your instructions. Slide your foot into the sock aid without crossing the operated leg over the other side or turning the foot inward aggressively.
Pull upward evenly until the sock is seated
Pull both straps evenly. If the sock catches on the heel, pause. Do not yank. Try a smaller pull, check your foot position, and continue. If the sock aid pops off dramatically, take a breath. The sock has not won. It has merely filed a complaint.
Here’s what no one tells you: loose socks are easier than heroic socks
Choose socks that open easily, slide smoothly, and do not demand a wrestling contract. Tight athletic socks may be fine later, but early recovery often rewards practical softness.
No-Bend Sock Routine: 4-Part Safety Map
1
Sit tall
Firm chair, arms available, operated leg not tucked under.
2
Load in lap
Put the sock on the aid before lowering it.
3
Lower by straps
Let the tool travel down, not your chest.
4
Pull, pause, check
Stop if pain, twisting, dizziness, or panic enters the room.
Chair Height Matters: Low Seats Make Socks Riskier
A low chair can turn a reasonable sock routine into a hip-angle ambush. The chair may look comfortable. It may even look friendly. But after hip surgery, comfort and safety are not always on speaking terms.
Why a low bed can quietly break your precautions
When you sit low, your knees often rise higher. Your hip closes more. Then, when you reach toward your foot, you may bend even deeper. A low bed can be especially sneaky because it feels familiar. Familiar is not always safe.
I have seen people reject a firm chair because the bed felt “easier.” Then they tried to stand up from the bed, sank backward, and made the exact face people make when a shopping cart wheel locks sideways. The body likes predictability. A firm chair gives it more.
How to tell whether your knees are too high
Use this simple visual check if your care team has not given you a different rule: when sitting, your knees should not be much higher than your hips. If your thighs slope sharply upward, the seat may be too low.
Use armrests so standing up does not become a second problem
Socks are only half the task. After dressing, you still need to stand. Armrests reduce the temptation to push off a walker, pull on furniture, or twist sideways.
The “one inch too low” trap
A seat does not have to be dramatically low to become annoying. One or two inches can change how much you bend, how hard you push to stand, and whether you feel steady while using a sock aid.
- Choose firm over soft.
- Choose armrests over armless style.
- Choose a higher seat over a low, cozy trap.
Apply in 60 seconds: Test your dressing chair before bedtime by sitting once and standing once without reaching for the walker.
Common Mistakes That Turn Sock Time Into a Fall Risk
The dangerous part of sock dressing is rarely one dramatic mistake. It is usually a stack of tiny shortcuts. A soft seat. A dropped sock. A twist. A little rushing. Suddenly the morning has teeth.
Mistake 1: bending from the waist “just for a second”
“Just for a second” is the unofficial anthem of home recovery trouble. If you were told not to bend past a certain limit, the time spent bending does not make the position safe. A brief unsafe position is still a position your care team likely wanted you to avoid.
Mistake 2: crossing the operated leg over the other knee
Many people used this move for years before surgery. It is efficient. It is familiar. It may also violate hip precautions for some patients, especially if it brings the leg across the midline or rotates the hip.
Mistake 3: twisting the foot inward while chasing the sock
If the sock heel is off-center, do not torque your foot around to fix it. Use a reacher, ask for help, or start again. A crooked sock is annoying. A twisted hip position is a worse bargain.
Mistake 4: standing on one leg to fix the heel
This is where the fall risk enters wearing tap shoes. Standing on one leg after hip surgery can be unstable, especially when pain medicine, fatigue, or morning stiffness is involved. For older adults, the safest routine often combines pain control, pacing, and home layout, not just one dressing tool; see this broader guide to orthopedic pain management for older adults.
Mistake 5: trying compression socks without approved help
Compression socks can require more force than regular socks. Some people are prescribed them after surgery, but putting them on may require caregiver help, special equipment, or therapist instruction. Do not treat them like ordinary socks with a tighter personality.
| Shortcut | Why it matters | Safer swap |
|---|---|---|
| Bending forward | May exceed hip precautions | Use sock aid straps |
| Crossing the leg | May combine crossing and rotation | Keep the foot forward |
| Standing to adjust | Raises fall risk | Sit and use a reacher |
Don’t Do This: The Moves That Look Harmless Until They Aren’t
Some risky moves look perfectly ordinary because they were ordinary before surgery. Recovery asks you to mistrust a few old habits for a while. This is not fear. It is temporary respect for healing tissue, new mechanics, and a body doing repair work under the floorboards.
Don’t sit on the edge of a soft mattress and fold forward
The edge of a soft mattress is a poor dressing station. It can slope, sink, and shift. If you lean forward from there, you may have no stable armrests and no clean way to reverse the movement.
Don’t pull your knee toward your chest to reach your foot
This can create deep hip flexion. If you have been told to avoid bringing the knee too high, this move belongs on the no-fly list.
Don’t use slippery socks on smooth floors
A sock that slides beautifully into a shoe may slide beautifully across the kitchen floor. If you walk indoors in socks, choose grip carefully and make sure the sock does not bunch under the foot.
Don’t rush because someone is waiting at the door
Rushing makes people skip the chair, skip the tool, and skip the pause. Doorbells are not medical authorities. Let them wait.
Pattern interrupt: pride is a terrible dressing aid
Pride has no straps, no handle, and no non-slip base. It has never once helped a heel settle correctly.
Quiet rule: If the move requires breath-holding, twisting, or bargaining with pain, it is not your best dressing method today.
Sock Types: Pick the Pair That Cooperates
Not all socks are equally friendly after hip surgery. Some socks glide on like reasonable citizens. Others behave like tiny fabric traps with elastic ambitions.
Loose crew socks: easiest for most sock aids
Loose crew socks are often easier to load onto a sock aid and easier to pull over the foot. They give you more margin for clumsy mornings, swollen feet, or imperfect aim.
Non-slip socks: helpful indoors, risky if they bunch
Non-slip socks can reduce sliding on smooth floors, but they should fit well. If the grippy bottom bunches under the foot, it can feel unstable or uncomfortable. Check the heel and sole position before standing.
Compression socks: ask first, because they need more force
Compression socks are in a different category. They may be medically recommended, but they often require stronger pulling and more careful technique. Ask your surgeon, nurse, or therapist how they want you to put them on.
Thick winter socks: cozy, but not always recovery-friendly
Thick socks can be harder to load into some sock aids and may make shoes tighter. Early recovery is not the moment to fight a boot sock with the temperament of a wool carpet.
Decision card: regular socks vs. compression socks
Choose regular loose socks when:
- Your care team has not prescribed compression.
- You need easier daily dressing.
- Your sock aid works smoothly with them.
Ask about compression socks when:
- They were prescribed after surgery.
- Your leg swelling plan includes them.
- You need help applying them safely.
Neutral action: Bring both sock types to therapy and ask for a real demonstration.
Caregiver Help: How to Assist Without Creating Awkward Leverage
Caregiver help should make the task safer, not louder. The best helper does not yank, rush, or lift the leg like a suitcase being shoved into an overhead bin.
Place the sock on the foot without lifting the leg too high
If you are helping, keep the person seated and stable. Bring the sock to the foot rather than bringing the foot high toward the sock. Ask the patient what their care team told them about leg position.
Keep the knee and toes pointed safely forward
Do not twist the foot to force the sock heel into place. If the sock is wrong, remove it and reload. A fresh start is often faster than a stubborn correction.
Let the patient control pace and pain signals
Use plain check-ins: “Is this angle okay?” “Any sharp pain?” “Do you want to pause?” Avoid cheerleading that sounds like a gym teacher trapped in a hallway.
Use help as a bridge, not a permanent loss of independence
The goal is not to take over forever. The goal is to protect the early recovery window while the patient builds a safer routine. A sock aid, reacher, and chair setup can gradually return control to the person healing.
Short Story: The Sock at 7:12 A.M.
At 7:12 one morning, a daughter stood beside her father’s dressing chair holding a sock like it contained a riddle. He wanted to do it himself. She wanted him not to fall. For a minute, both of them were right and both of them were irritated.
Then they changed the task. She loaded the sock onto the aid in his lap. He lowered it with the straps. She watched his foot position instead of grabbing his leg. He pulled, paused, and laughed when the heel landed crooked. They started again. The second try worked. Nothing dramatic happened, which was exactly the victory. Recovery often improves in these small rooms: not through grand speeches, but through one ordinary task made less risky.
Mini Routine: A Safer 3-Minute Sock Sequence
A routine reduces decision fatigue. When you are sore, foggy, or worried about being late, you do not want to invent a sock strategy from scratch. You want a small script.
Step 1: Sit tall before reaching for anything
Back against the chair if comfortable. Feet supported. Operated leg positioned according to your instructions. Take one breath. This is not theater. It is how you keep the first move from becoming messy.
Step 2: Load the sock aid in your lap
Place the sock on the aid while everything is close to your body. Smooth the sock as much as possible. Make sure the toe and heel are aligned.
Step 3: Lower, place, pull, pause
Lower the aid using the straps. Slide your foot in. Pull evenly. Pause if the sock catches or if you feel yourself leaning forward.
Step 4: Check heel position without bending forward
Use a reacher or caregiver help if the heel needs adjusting. Do not fold forward to inspect it. A mirror may help some people, but only if it does not tempt twisting.
Step 5: Stand only after both feet feel stable
Before standing, check that the socks are not slippery, bunched, twisted, or half-on. Use the chair arms. Stand slowly. Let your balance arrive before you walk. If your walking aid is part of the morning sequence, this guide on walker pain management for seniors at home can help you think through turns, transfers, and pacing.
Mini calculator: is your sock setup rushed?
Neutral action: Use the result to decide whether to simplify the routine or ask for help today.
Equipment Decision Card: What Actually Helps
Recovery equipment can either solve a real problem or become a plastic museum in the corner. Buy or borrow based on the task you actually struggle with, not the category name on the package.
Sock aid vs. reacher: different jobs, different wins
A sock aid helps put the sock on. A reacher helps retrieve, position, or adjust items without bending. They work well together, but one does not fully replace the other.
Long-handled shoehorn: the sock aid’s quiet partner
A long-handled shoehorn helps with shoes after the sock is on. It can reduce bending and heel wrestling. Slip-on shoes may help, but only if they are secure and approved for your walking needs.
Dressing stick: useful for pants, less magical for socks
A dressing stick can help move fabric, guide pants, or manage clothing without reaching. For socks, it is usually less direct than a sock aid.
Grabber tool: helpful nearby, not a substitute for balance
A grabber is excellent for retrieving dropped socks or moving light items. It should not become a cane, a brace, or a way to lean dangerously far.
| Tool | Best for | Watch out for |
|---|---|---|
| Sock aid | Putting on regular socks without bending | Very tight socks may be harder to load |
| Reacher | Picking up dropped items | Not for body weight or balance |
| Long-handled shoehorn | Sliding heel into shoe | Shoes still need stable soles |
| Dressing stick | Moving clothing fabric | Less ideal as the main sock tool |
- Start with a sock aid if bending is restricted.
- Add a reacher for dropped items.
- Use a long-handled shoehorn for shoes.
Apply in 60 seconds: Put the tools in one basket or tray beside the dressing chair.
Recovery Timeline: When Sock Dressing May Get Easier
Most people want to know when this stops feeling absurd. Fair question. The answer depends on your surgery, precautions, strength, pain, flexibility, balance, swelling, and therapist guidance.
Why the first weeks feel clumsy
Early recovery includes pain, stiffness, swelling, sleep disruption, medication effects, and fear of doing something wrong. That is a crowded little committee. Even simple tasks can feel clunky.
Why “I can reach it” is not the same as “I should”
One of the trickiest recovery moments happens when you begin feeling better. Pain drops, confidence rises, and suddenly the old habits start knocking. But flexibility is not clearance. Ask before changing the routine.
When to ask your therapist about changing the routine
Ask during a follow-up visit or therapy session. Bring the actual question: “Can I put on socks without the aid now?” Better yet, demonstrate your current method and let the therapist correct it.
The clearance question to bring to your follow-up visit
Try this: “For my surgery and current stage, what sock and shoe positions are safe, and which should I still avoid?” Specific questions get better answers than “Am I okay now?”
Quote-prep list: what to gather before buying dressing aids
- Your exact hip precautions and surgical approach, if known
- Chair height and whether you have armrests
- Type of socks you need: regular, non-slip, or compression
- Whether you also need shoe help
- Whether a caregiver will assist daily or only sometimes
Neutral action: Compare tools only after you know the task they need to solve.
FAQ
Can I put on socks by myself after hip surgery?
Many people can put on socks by themselves after hip surgery by using a sock aid, sitting in a firm chair, and avoiding restricted bending or twisting. However, your surgeon’s or therapist’s instructions decide what is safe for you. If you feel dizzy, unstable, or tempted to bend deeply, ask for help.
What is the easiest way to put on socks after hip replacement?
The easiest safer method is usually to use a sock aid while seated in a firm, higher chair with armrests. Load the sock onto the aid in your lap, lower it with the straps, slide your foot in, and pull evenly without leaning forward.
Can I bend forward to put socks on after hip surgery?
Not unless your care team has cleared that movement. Many hip-replacement precautions warn against bending the hip past 90 degrees, especially after certain surgical approaches. Bending forward to reach socks can break that limit quickly, especially from a low chair or bed.
Do I need a sock aid after hip replacement?
You may need a sock aid if you have bending restrictions, pain, stiffness, or difficulty reaching your foot safely. Some people use one only during early recovery. Others use it longer because it makes mornings safer and less exhausting.
Can I cross my leg to reach my foot after hip surgery?
Do not cross your leg unless your surgeon or physical therapist says it is safe for your recovery stage. Crossing the operated leg can violate common hip precautions for some patients and may combine bending, crossing, and rotation.
Are compression socks safe to put on by myself?
Compression socks can be difficult to apply because they require more force. If they were prescribed, ask your nurse, surgeon, or therapist whether you should use a special aid or caregiver help. Do not strain, twist, or bend deeply to force them on.
What chair should I use when getting dressed?
Use a firm chair with a straight back and armrests when possible. Avoid low, soft couches or mattress edges if they make your knees rise high or cause you to lean forward. Your therapist can advise the best seat height for your body.
How long will I need help putting on socks?
It varies. Some people need help for a few weeks. Others need tools or assistance longer due to precautions, swelling, balance, strength, or other health issues. Ask at follow-up when you can safely change your sock routine.
Next Step: Make Tomorrow Morning Safer Tonight
The sock was never the villain. The real problem was the hidden chain: low seat, deep bend, twisting foot, rushed morning, and a body still healing. Break that chain tonight and tomorrow gets easier.
Put one pair of easy socks, your sock aid, shoes, reacher, and phone beside a firm chair before bed
Do not wait until morning. Morning has enough little gremlins already. Place the tools where your hand can reach them without leaning.
Ask your PT or surgeon one specific question: “What is my safe dressing position?”
That one question can prevent weeks of guessing. Ask for a demonstration if possible. A 30-second correction can spare you a dozen awkward mornings. If sleep is also making recovery harder, review these practical notes on sleeping discomfort after hip replacement, because tired mornings are where small safety shortcuts tend to sneak in.
Practice once when you are not rushed, not wet from the shower, and not already tired
Practice at a boring time. Dry floor. Good light. Phone nearby. No appointment countdown. No one honking outside like a goose with a calendar. For the bathroom side of recovery, especially when dressing overlaps with bathing, this guide to showering after hip surgery can help you think through slippery floors, transfers, and tool placement.
- Set the chair and tools before bed.
- Use the sock aid before bending becomes tempting.
- Ask for help before a small task becomes a risky moment.
Apply in 60 seconds: Create your no-bend dressing station now, then test it once without rushing.
Last reviewed: 2026-05.
