
You don’t need a bigger apartment after knee replacement.
You need a smaller number of risky moments.
A small apartment setup after knee replacement can work beautifully when the route from bed to bathroom, chair, and kitchen is clear enough for a walker, predictable enough for tired mornings, and simple enough for those foggy midnight bathroom trips.
This guide simplifies your recovery. You’ll learn how to build a clean walker route, choose a useful recovery chair, and reduce bathroom risks without turning your living room into a medical supply aisle.
Tiny apartment, calmer recovery.
Table of Contents

Start With the Walking Lane, Not the Furniture
The first recovery “room” is really a route
After knee replacement, the most important space in a small apartment may not be the bedroom, bathroom, or kitchen. It is the route connecting them.
That route is where you take the first sleepy steps of the morning. It is where you carry your body, your walker, your fresh knee, and occasionally your dignity, which may be wearing mismatched socks. The route needs to be simple enough that you can use it when tired, sore, medicated, or half-awake.
Clear a walker-width path from bed to bathroom to kitchen
Before discharge day, walk the path with the actual assistive device if possible. A walker takes more room than your body alone. It also needs a predictable landing place with every step. Tight corners, rug edges, pet bowls, laundry baskets, and little decorative stools become villains with tiny mustaches.
- Clear the bed-to-bathroom route first.
- Then clear the bed-to-recovery-chair route.
- Then clear the recovery-chair-to-kitchen route.
- Leave turning areas open, not just straightaways.
Don’t make the scenic route safer than the urgent route
Many people clean the living room beautifully and forget the 2 a.m. bathroom trip. That is the mistake. The urgent route is the real test. Bathroom urgency plus post-surgical stiffness can turn a harmless ottoman into a tiny upholstered lawsuit.
Tiny apartment rule: fewer turns beat prettier layout
In a small apartment, the safest layout is often the least charming one. Put function ahead of symmetry for a few weeks. If the coffee table has to sit in exile against the wall, let it go sulk there.
- Prioritize bed, bathroom, chair, and kitchen.
- Remove anything that narrows turns.
- Test the path with the real walker, cane, or crutches.
Apply in 60 seconds: Stand at the bed and look toward the bathroom; remove the first object your eye hesitates over.
Mini Infographic: The Small Apartment Recovery Loop
stand safely
transfer zone
rest + elevate
one-reach station
Rule: If an object does not help this loop, it should not live inside it.
Who This Is For, and Who Should Pause Before Copying It
For patients recovering in studios, one-bedrooms, basement units, and senior apartments
This guide is for the person looking around a compact apartment and thinking, “Where exactly am I supposed to put a walker, ice packs, medication, pillows, groceries, and my regular life?” Fair question. Small apartments do not offer much spare space, but they do offer one gift: fewer rooms to tame.
I have helped relatives rearrange “temporary” recovery setups that stayed up for six weeks. The best ones were never fancy. They were plain, repeatable, and almost boring. That is a compliment. Boring is beautiful when your knee is swollen and your brain is running on hospital sleep.
For caregivers setting up a space before discharge day
If you are a spouse, adult child, friend, or neighbor helping before discharge, your job is not to buy every recovery gadget with five stars and a name that sounds like a spaceship part. Your job is to remove decisions. Put important things where they will be used. Make the first day home feel less like a scavenger hunt.
Not for people with unstable symptoms, unclear weight-bearing instructions, or no discharge plan
Pause before copying any home setup if the patient does not understand their discharge instructions, weight-bearing limits, medication plan, or follow-up schedule. That is not a decorating problem. That is a care-team question.
MedlinePlus patient guidance for knee replacement discharge emphasizes precautions such as avoiding twisting or pivoting while using a walker, avoiding ladders or stepstools, and not kneeling to pick things up. Those rules shape the apartment. They are not tiny footnotes wearing sensible shoes.
Here’s what no one tells you: “small” can be safer than “spacious” if the route is clean
A large home with stairs, long hallways, and scattered supplies can be harder than a small apartment with one disciplined route. Space is not the same as safety. Predictability is safety.
Eligibility Checklist: Is this setup approach a good fit?
- Yes/No: Do you have written discharge instructions?
- Yes/No: Do you know which assistive device you will use at home?
- Yes/No: Can the main route avoid stairs for routine tasks?
- Yes/No: Can someone check the setup before or shortly after discharge?
Neutral next step: If one answer is “no,” write it down and ask the discharge nurse, surgeon’s office, or physical therapist before relying on the layout.
The Bedroom Setup That Makes Mornings Less Treacherous
Bed height matters more than decorative pillows
The first stand of the day deserves respect. After knee replacement, getting out of bed can feel like negotiating with a very grumpy hinge. If the bed is too low, standing may require extra knee bend and more arm effort. If it is too high, feet may not plant securely.
The goal is not perfection. The goal is a stable sit-to-stand. Your feet should reach the floor, your walker should be parked close, and the path forward should be clear before you stand. Decorative pillows can wait in a basket. They have had a good run.
Put the walker where the first standing motion happens
Do not park the walker “nearby” in a poetic sense. Nearby should mean reachable without twisting, leaning, or stepping first. The walker belongs where hands naturally go after sitting up and before standing.
A caregiver can tape a small floor marker where the walker should return. It sounds silly until day three, when everyone is tired and the walker has mysteriously migrated six feet away like a metal flamingo. For older adults who need more confidence with mobility equipment, a practical guide to walker pain management for seniors can help frame what “safe and reachable” should look like at home.
Create a no-bend nightstand zone for phone, water, meds, glasses, and light
The nightstand should work like a cockpit, but less dramatic. Put high-use items between shoulder and waist height. Avoid bottom drawers for anything needed daily. If medication is stored at the bedside, follow the care team’s medication safety instructions and keep it secure from children, pets, or confused visitors.
- Phone and charger
- Water bottle with a lid
- Glasses or hearing aids
- Medication list, not loose mystery pills
- Small lamp or reachable light switch
Don’t let charging cords become little ankle snakes
Cords should run behind furniture or along the wall, never across the walking lane. Tape them down only if doing so does not create a raised edge. Better yet, move the charging station so the cord does not cross the route at all.
- Place the walker at the standing point.
- Keep essentials at no-bend height.
- Route cords away from feet and walker legs.
Apply in 60 seconds: Sit on the bed and reach for your phone, light, and walker; move anything that requires twisting.
Show me the nerdy details
Small-apartment recovery design works best when it reduces “transition load.” A transition is any moment when the body changes position or direction: lying to sitting, sitting to standing, standing to turning, walking to sitting. These moments are more demanding than simply resting or walking straight. That is why bed height, chair height, walker position, and bathroom transfer setup often matter more than general neatness.
The Bathroom Is the Boss Battle
Fix the toilet transfer before you worry about the sofa
The bathroom is where small apartments become honest. It is tight, wet, hard-surfaced, and full of awkward angles. After knee replacement, the toilet transfer may be one of the most repeated and least forgiving moves of the day.
Before buying anything, identify the exact problem. Is the toilet too low? Is there nothing safe to push from? Is the walker blocking the door swing? Is the bath mat sliding? Each problem has a different solution.
Use grab bars, raised toilet seats, or approved supports only as directed
Grab bars should be properly installed, not suction-cup optimism. Raised toilet seats and toilet safety frames can help some people, but they should match the patient’s height, balance, bathroom layout, and care-team guidance.
A towel bar is not a grab bar. It may look loyal. It is not loyal. It is decorative metal with commitment issues.
Keep shower supplies between shoulder and waist height
Shampoo on the floor is an invitation to bend, twist, or wobble. Move supplies to a stable caddy or shelf at reachable height. Keep soap, towel, clean clothes, and non-slip footwear planned before showering.
The wet-floor problem: small bathrooms punish tiny mistakes
A narrow bathroom gives you less room to recover from a slip. Place towels where they will not bunch under the walker. Use non-slip bath mats outside the tub or shower only if they lie flat and do not create a raised edge. If the care team recommends a shower chair or tub bench, measure before discharge day. Bathroom doors and tub lips have a talent for ruining beautiful plans.
Decision Card: Raised Toilet Seat vs. Toilet Safety Frame
| Option | Best when | Watch for |
|---|---|---|
| Raised toilet seat | The main issue is a low toilet. | Fit, stability, and whether it changes safe sitting angle. |
| Safety frame | The main issue is safe hand support. | Bathroom width, walker parking, and secure placement. |
Neutral action: Measure the toilet area and ask the discharge team which support matches the patient’s transfer needs. If you are comparing practical supports before surgery, a broader overview of orthopedic home care equipment can help you separate useful tools from expensive floor clutter.
Kitchen Recovery Works Best in “One-Reach” Zones
Build a counter-height breakfast station
The kitchen does not need a full remodel. It needs one honest station. Put breakfast basics, cups, water, snacks, and simple utensils at counter height. The first week after surgery is not the time to rediscover the cast-iron skillet hiding in a low cabinet.
When I once helped set up a relative’s kitchen after surgery, the biggest win was not a gadget. It was moving mugs from a high shelf to the counter. A four-second reach disappeared. Multiply that by six times a day and you have less fatigue, fewer risky bends, and fewer muttered kitchen curses.
Move daily dishes, snacks, and water bottles out of low cabinets
Low cabinets ask for bending. High cabinets ask for reaching. Both can be awkward early in recovery. The middle zone is your friend: counter, waist-height shelf, rolling cart placed outside the walking lane, or a stable table.
Use lightweight meals that do not require carrying hot pans across the room
A walker and a hot pan are not a charming duet. Plan meals that can be assembled, microwaved, or served without long carrying distances. Use containers with lids. Keep heavier groceries divided into smaller portions.
Let’s be honest: the heroic soup pot can wait
Cooking can feel like independence, but the early recovery kitchen should reward restraint. Soup pots, slippery cutting boards, and floor-level pantry raids can wait until mobility is steadier and your care team has cleared more activity.
Common Mistakes That Make a Small Apartment Riskier
Mistake 1: keeping rugs because they “never caused trouble before”
Rugs are sneaky because they feel familiar. But after knee replacement, familiar does not mean safe. A rug edge that never mattered before can catch a walker leg, slipper, robe hem, or tired foot. Remove loose rugs from the recovery route unless the care team says otherwise and they can be secured without raised edges.
Mistake 2: storing ice packs, meds, or chargers across the room
Recovery supplies should live where the task happens. Ice packs near the freezer make sense, but the wrap, towel barrier, timer, and elevation pillows should be near the recovery chair. Medication lists should be easy to read. Chargers should not require a pilgrimage.
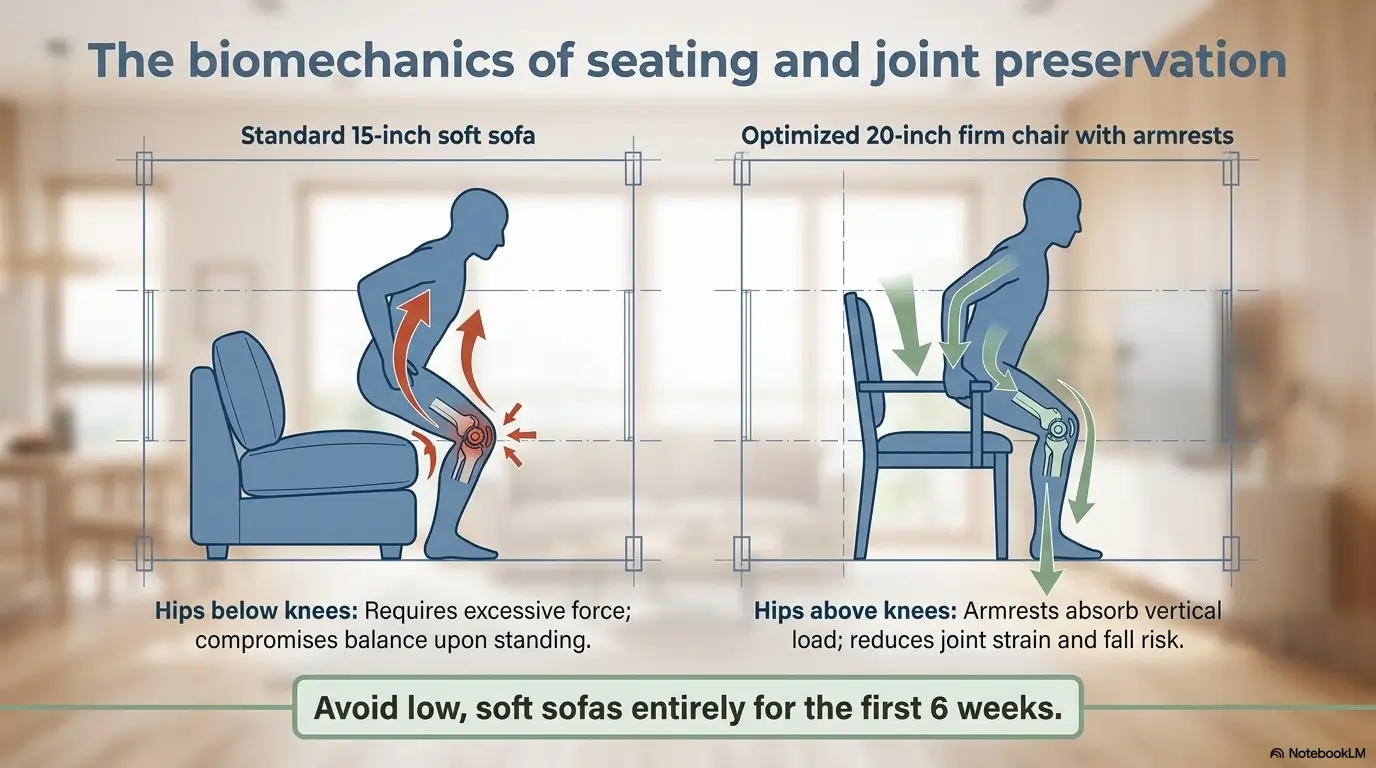
Mistake 3: using rolling chairs, low stools, or soft sinking seats
Rolling chairs move when you need them to stay. Low stools demand deeper knee bend. Soft couches can swallow a recovering patient like a well-upholstered swamp. A firm, stable, higher chair is usually the safer recovery throne.
Mistake 4: trying to clean, cook, and organize on the same “good pain” afternoon
Good pain days can be tricksters. Feeling better does not automatically mean the knee is ready for a domestic marathon. Overdoing it may increase fatigue and swelling. The apartment should make pacing easier, not tempt you into a full heroic montage.
Mistake 5: assuming a narrow space is automatically unsafe
Narrow is not always bad. Narrow and cluttered is bad. Narrow and predictable can work beautifully. One clean lane, one firm chair, one bathroom plan, and one kitchen station can outperform a larger home full of scattered “helpful” objects.
- Remove loose rugs from main routes.
- Replace rolling or sinking seats.
- Store supplies by task, not by category.
Apply in 60 seconds: Take one photo of the bed-to-bathroom path and look for cord, rug, and clutter hazards on the screen.
Don’t Do This: Recovery Clutter Disguised as Help
Too many gadgets can shrink your turning radius
Recovery equipment should earn its floor space. A reacher, walker basket, shower chair, raised toilet seat, or firm chair may be helpful when it solves a real repeated problem. But a pile of “maybe useful” equipment can turn a small apartment into an obstacle course with receipts.
The test is simple: does this item make one daily movement safer, easier, or more predictable? If not, store it outside the walking lane.
Extra chairs become obstacles when they are not placed with a job
A chair beside the bed can help dressing. A chair blocking the kitchen path helps nobody. Place each chair with a purpose: sit to dress, rest after walking, elevate the leg, or support a caregiver task. Chairs without jobs become wooden traffic cones.
Bulk supplies belong off the walking lane, not beside the bed
Bulk paper towels, water cases, and medical supplies can feel reassuring. They also eat precious turning space. Keep a small daily supply near the recovery zone and store the rest elsewhere. A small apartment works better when it uses refilling, not hoarding.
The apartment should feel boringly predictable
Predictability lowers the mental load. The walker returns to the same spot. The water bottle has a home. The phone charger has a path. The ice wrap lives in the same basket. This is not fussy. It is friction management.
Quote-Prep List: What to Gather Before Buying Recovery Equipment
- Toilet height and bathroom width
- Bed height from floor to mattress top
- Doorway width on the main route
- Care-team instructions for assistive devices
- Photos of tight turns, shower entry, and chair options
Neutral action: Use these details when comparing equipment or asking a physical therapist what fits your space. If costs or coverage are part of the decision, review whether certain braces and supports may be HSA eligible before buying equipment that your plan may treat differently.
Pain, Ice, Swelling, and the Apartment Layout
Put swelling-control supplies where resting actually happens
Swelling care is easier when the layout cooperates. If the patient rests in the recovery chair, keep elevation pillows, a towel barrier for ice, a timer, water, and the symptom note nearby. If the supplies are scattered, every icing session becomes a tiny expedition.
AAOS explains that swelling can be moderate to severe in the first days or weeks after knee replacement, with milder swelling sometimes lasting for months. Their patient guidance also says new or severe swelling should be reported because it may be a warning sign of a blood clot.
Use elevation and icing only as your care team recommends
Do not freestyle the medical plan. Ice, elevation, compression stockings, movement, and medication should follow discharge instructions. The apartment’s job is to make those instructions easier to obey. For readers trying to understand how home setup and discomfort management fit together, this guide to knee replacement pain management can provide useful context for conversations with the care team.
Keep a simple symptom note beside the recovery chair
A notebook can prevent vague updates like “I think it was worse yesterday, maybe.” Track basics: pain pattern, swelling changes, medication timing questions, sleep, walking tolerance, and any symptoms the discharge packet tells you to report.
When new or severe swelling changes the plan
New or severe swelling, calf pain, sudden worsening pain, shortness of breath, chest pain, fever, chills, drainage, or sudden inability to walk safely should not be treated as a layout issue. That is when the human backup plan matters.
- Keep ice supplies and elevation support together.
- Use a timer if recommended.
- Track symptom changes in plain language.
Apply in 60 seconds: Put a notebook and pen next to the chair and write today’s date at the top.
The Recovery Chair May Be the Most Important Furniture
Choose firm, high, stable seating over cozy low seating
The recovery chair is not just a place to watch TV. It is a transfer station, rest zone, medication-check zone, elevation spot, and emotional headquarters. It should be firm enough to stand from, high enough to reduce strain, and stable enough not to slide.
I once watched a perfectly kind recliner betray someone by being too deep and too soft. It looked comfortable. It behaved like quicksand in upholstery. Comfort matters, but safe standing matters first.
Set up a side table that prevents twisting and reaching
The side table should sit on the non-chaotic side of the chair, close enough to reach without leaning. Put the most-used items in the same positions every day. Remote front right. Water back left. Medication list in a folder. Phone on a charger that does not cross the floor.
Keep TV remotes, medication lists, water, tissues, and phone within easy reach
Reachable does not mean piled together in a little plastic avalanche. Use a tray, basket, or divided organizer. Labeling can help caregivers return things to the same place. A tiny system beats a heap with ambition.
One chair, one purpose: sit, elevate, reset
During early recovery, the chair should invite pacing. Sit. Elevate if instructed. Ice if instructed. Drink water. Reset. Then walk as directed. The chair should not become a command center for folding laundry, sorting boxes, or assembling furniture purchased during a medication-induced online shopping fog.
Decision Card: Recliner vs. Firm Dining-Height Chair
| Choice | Useful when | Risk to check |
|---|---|---|
| Recliner | It is stable, easy to exit, and supports the care plan. | Too low, too soft, too deep, or hard to operate. |
| Firm chair | Sit-to-stand safety is the main priority. | Needs nearby leg support if elevation is recommended. |
Neutral action: Practice one sit-to-stand with supervision before choosing the main recovery seat.
Fall Prevention in a Small Apartment Starts Before the First Step
Brighten the bed-to-bathroom path
Lighting is not decoration after surgery. It is navigation. The bed-to-bathroom path should be visible without requiring a full-room glare bomb. Night lights, motion lights, or reachable lamps can help, especially if the patient gets up at night.
The CDC’s older adult fall-prevention materials state that more than one in four older adults falls each year, and that falling once doubles the chance of falling again. That statistic is not meant to scare people into bubble wrap. It is meant to make prevention feel practical.
Remove floor clutter from every turn zone
Turn zones are the small patches where the walker rotates, the body pivots, or the patient changes direction. These zones need more room than a straight path. Remove hampers, side tables, shoes, bags, and decorative baskets from corners.
Place shoes, walker, and assistive devices in fixed homes
A fixed home means the object returns to the same spot every time. Shoes by the chair. Walker by the bed or chair, depending on where standing begins. Cane only if prescribed or approved. Do not create a museum of mobility aids in the hallway.
Small night lights, big consequences
Night trips are where confidence gets tested. A dim route, full bladder, stiff knee, and misplaced slipper can create a bad little orchestra. Put light where decisions happen: beside the bed, at the bathroom entrance, and near any turn.
When to Seek Help Instead of “Waiting It Out”
Call your surgeon or care team for new or severe swelling, worsening pain, fever, chills, calf pain, drainage, or symptoms listed in your discharge packet
A good apartment setup reduces avoidable risk. It does not diagnose problems. If symptoms change in a concerning way, use the contact instructions from the discharge packet. Keep that number visible near the recovery chair and bed.
Ask for help immediately after a fall, near-fall, medication confusion, or sudden inability to walk safely
A near-fall counts. Medication confusion counts. A sudden new fear of walking counts. Do not wait until the situation becomes dramatic enough for background music. Early help is often simpler help.
Do not troubleshoot chest pain, shortness of breath, or signs of a possible clot at home
Chest pain, shortness of breath, fainting, sudden severe symptoms, or signs your discharge instructions describe as urgent should be treated as urgent. Call emergency services or follow the emergency instructions given by the care team.
The safest apartment setup includes a human backup plan
A human backup plan can be a spouse, adult child, neighbor, friend, building staff contact, or scheduled check-in. Write down who to call for three levels of need: routine help, same-day concern, and emergency.
Coverage Tier Map: Human Backup Plan
| Tier | Support level | Example |
|---|---|---|
| 1 | Daily check-in | Text or call at the same time daily. |
| 2 | Errand help | Groceries, pharmacy, laundry. |
| 3 | Same-day visit | Concern after near-fall or unsafe task. |
| 4 | Clinical call | Surgeon, nurse line, physical therapy office. |
| 5 | Emergency response | Call emergency services for urgent symptoms. |
Neutral action: Put this list on paper where the patient and caregiver can both see it. If the discharge plan includes rehab options or extra support after surgery, it may also help to compare how to choose rehab after surgery before the first week at home becomes a guessing game.
FAQ
How much space do I need for a walker after knee replacement?
You need enough clear space for the walker to move forward and turn without clipping furniture, rugs, cords, door frames, or baskets. Exact clearance depends on the walker and the patient’s gait, so test the actual route with the actual device before surgery if possible. The most important areas are the bed, bathroom entrance, toilet transfer zone, recovery chair, and kitchen station.
Should I remove all rugs before knee replacement surgery?
Loose rugs on the main walking route are usually worth removing because they can catch feet or walker legs. If a rug is necessary, ask the care team whether it can be secured safely. Avoid raised edges, curled corners, and mats that slide on smooth floors.
Where should I sleep after knee replacement in a small apartment?
Sleep where the bed is easiest to enter and exit safely, the bathroom route is shortest and clearest, and the walker can be placed within reach before standing. For many small apartments, the existing bed works if the height is safe and the route is clean. If the bed is too low or the bathroom path is awkward, ask the care team about alternatives before improvising.
Is a recliner helpful after knee replacement?
A recliner can be helpful if it is firm, stable, easy to get out of, and supports the surgeon’s instructions for positioning and elevation. It can be a poor choice if it is too low, too soft, too deep, or difficult to operate. Test sit-to-stand safety with supervision.
What should I keep next to the bed after knee replacement?
Keep a reachable light, phone, charger, water bottle with a lid, glasses, medication list, and any care-team-approved nighttime essentials. Avoid clutter. The bedside zone should reduce bending and twisting, not become a tiny warehouse.
How do I shower safely in a small bathroom after knee replacement?
Follow your discharge instructions first. In general, reduce wet-floor risk, keep supplies at reachable height, avoid bending for bottles, and use only approved supports. If a shower chair, tub bench, non-slip mat, or grab bar is recommended, measure the bathroom and confirm fit before relying on it.
Can I live alone in a small apartment after knee replacement?
Some people can recover in a small apartment with the right discharge plan, support, equipment, and check-ins. Others need more hands-on help. The answer depends on mobility, pain control, medication safety, bathroom access, stairs, medical risk, and the care team’s instructions. Do not decide based only on apartment size.
What should caregivers set up before discharge day?
Caregivers should clear the walking route, prepare the bathroom transfer area, set up a firm recovery chair, move daily kitchen items to counter height, remove loose rugs and cords, place emergency numbers visibly, and stock a simple bedside and chair-side zone.
Next Step: Do the 10-Minute Walker Route Test
Walk the bed-to-bathroom-to-kitchen path with the actual assistive device
The hook at the beginning was this: you do not need a perfect apartment. You need one that behaves itself. The 10-minute walker route test is how you teach it manners.
Start at the bed. Move to the bathroom. Turn. Return to the recovery chair. Move to the kitchen station. Do not rush. Watch what the walker touches, what your foot almost catches, and where your body wants to twist.
Remove anything your foot, walker, robe, or charger cord can catch
Do not negotiate with trip hazards. Remove them. If something must stay, move it outside the route. The apartment does not need to look empty. It needs to stop grabbing at the patient like a clingy stage curtain.
Put one high-use item in each fixed recovery zone
Place one important item in each zone: water by the chair, light by the bed, towel by the shower plan, easy meal at the kitchen station. This turns the apartment from a storage puzzle into a recovery map.
Write down the one task that still feels unsafe and ask your care team about it
The smartest next step is not buying more equipment. It is identifying the one task that still feels unsafe. Toilet transfer? Shower entry? Getting out of bed? Carrying food? Write it down. Ask the surgeon’s office, discharge nurse, or physical therapist for guidance. If pain control is part of that question, especially for an older adult, it may be worth reading about orthopedic pain management for older adults so the conversation stays specific instead of foggy.
- Test the route before relying on it.
- Remove hazards instead of stepping around them.
- Ask for help when one task still feels unsafe.
Apply in 60 seconds: Write “bed → bathroom → chair → kitchen” on paper, then circle the one segment that needs attention first.
Short Story: The Apartment That Got Safer by Losing Three Things
A family I knew once prepared a tiny one-bedroom apartment for knee replacement recovery. They bought a new organizer, a shower caddy, extra pillows, and a rolling cart. The place looked prepared, but the walker kept bumping into the cart near the bathroom door. The patient smiled politely and said it was “probably fine,” which is usually the sentence a home says before it starts throwing banana peels.
So they removed three things: the hallway rug, the rolling cart, and a low side table near the bed. Nothing glamorous happened. No cinematic reveal. But suddenly the route made sense. The walker turned cleanly. The bathroom door opened wider. The bed stand-up felt less crowded. The apartment did not become bigger. It became quieter. That is the small secret of recovery design: sometimes the best equipment is the empty space where trouble used to stand.
Your 15-minute CTA is simple: run the route test, remove three hazards, and write down one question for the care team. That is enough for today. Recovery is not won by heroic furniture wrestling. It is won by small, sane decisions repeated until the apartment feels calm underfoot.
Last reviewed: 2026-05.
