
The Right Tool for the Right Moment: Orthopedic Home Care Reimagined
Orthopedic pain management at home rarely falls apart because a family does not care. It falls apart because the wrong tool shows up for the wrong moment. A sturdy walker will not fix a painful toilet transfer, and an expensive chair will not help much if the real disaster happens when someone turns in bed at 2 a.m.
“That is where families get stuck. They compare home care equipment by category, price, or panic, while the actual problem lives in a narrower place: shower entry, sit-to-stand strain, nighttime bathroom trips, caregiver back stress, or a bed that is simply the wrong height.”
Keep guessing, and the house gets more crowded while daily life gets harder. This guide helps you compare orthopedic pain management equipment by function, room, and repeat use, so you can choose what actually reduces pain, protects mobility, and lowers caregiver strain without turning the home into a medical supply maze.
The best setup is not the one that looks impressive online. It is the one that works on a tired Tuesday.
Start with the hardest moment. Then fix what repeats.
Table of Contents
Fast Answer: Orthopedic pain management for families comparing home care equipment works best when you match the tool to the pain problem, mobility limit, and daily routine, not just the diagnosis. The right equipment can reduce strain, improve transfers, protect sleep, and lower fall risk. The wrong setup can waste money, crowd the home, and make pain management harder instead of easier.

Start With the Real Job: What Problem Does the Equipment Need to Solve?
Pain relief equipment and mobility equipment are not always the same purchase
Families often start by searching for a category. “We need something for pain.” “We need a walking aid.” “We need a chair.” But categories are fuzzy, and bodies are not. A wedge pillow can help with positioning pain. A transfer bench can help with bathing pain. A walker may help with movement, yet do very little for the hardest part of the day if the real agony happens while standing up from the toilet or turning in bed.
The house usually reveals the truth faster than a product page does. Watch where the face tightens, where the pause happens, where the helper braces with one hand on a dresser and the other on a shoulder. That is your starting point.
Families often compare products before defining the hardest moment of the day
Many households buy from fear. That is understandable. Fear is loud. It makes large equipment feel morally superior, as if a bigger purchase must equal better care. But the hardest moment is often much smaller and much more repetitive. It may be putting on socks. It may be lowering onto the toilet. It may be getting back into bed without twisting a healing knee, hip, shoulder, or spine.
I have seen families proudly wheel in a major piece of equipment, only to discover the real daily villain was a six-inch height difference between chair and body. Pain has a talent for hiding in angles.
The better question is not “What is best?” but “Best for which task, at which stage, for which body?”
That question sounds less glamorous, but it saves money and chaos. Recovery changes. Early-stage needs are often about protection and safe transfers. Mid-stage needs may shift toward endurance and reducing household friction. Later-stage needs may focus on confidence, independence, and not keeping the living room looking like a small medical supply warehouse.
- Name the exact motion that hurts
- Identify the room where it happens most
- Match the tool to that motion first
Apply in 60 seconds: Write one sentence that begins, “The hardest moment is when…”
Eligibility Checklist: Are you ready to compare equipment yet?
- Yes / No: You can name the top 3 painful tasks.
- Yes / No: You know which room causes the most strain.
- Yes / No: You know whether the problem is walking, transferring, bathing, sleeping, or reaching.
- Yes / No: You measured at least one key dimension in the home.
Next step: If you answered “no” to two or more, pause the shopping tab and do a 10-minute home walk-through first.
Who This Is For, and Who It Is Not
This is for families comparing walkers, lift chairs, shower seats, wedges, braces, reachers, bedside aids, and transfer supports
This guide is for households trying to make real-life care less clumsy. Not idealized care. Not showroom care. Real care. The kind where someone is tired, the hallway is narrow, towels are in the way, and dinner still has to happen.
If you are looking at walkers, canes, transfer poles, shower chairs, tub benches, wedges, braces, reachers, bedside rails, overbed tables, raised toilet seats, leg lifters, and similar tools, you are in the right room.
This is for households trying to reduce pain, protect movement, and make caregiving less physically chaotic
Sometimes families think equipment is only about the patient. It is not. Good equipment protects the caregiver too. If your back is already muttering dark poetry after a week of awkward lifting, that matters. A device that reduces strain for both people is often worth more than a device that looks medically impressive and gets used twice. For households caring for an older adult, many of the same room-by-room decisions also show up in orthopedic pain management for older adults living at home.
This is not for diagnosing a new injury, replacing surgical instructions, or choosing emergency equipment without medical guidance
If pain is suddenly worse, swelling is dramatic, weight-bearing changes sharply, or something feels unsafe in a new way, that is not a shopping problem. It is a follow-up problem. Likewise, if there are specific post-surgical precautions, those instructions outrank any generic home-care advice. This article is educational, practical, and grounded in household decision-making, but it does not replace clinician guidance.
Think of this guide as a lamp, not a license.
Pain Trigger First: Match Equipment to the Moment Pain Spikes
Bed-to-bathroom pain needs different equipment than sit-to-stand pain
Orthopedic pain is not one thing. It behaves more like weather inside the house. One room gets foggy at night. Another gets stormy during transfers. Another only turns hostile when water is involved. Bed-to-bathroom pain often points toward night lighting, stable footwear, bedside commode options, clearer pathways, or support surfaces that reduce the first standing strain. Sit-to-stand pain points toward seat height, arm support, transfer technique, and the difference between pushing from something solid versus dragging yourself upward from soft furniture.
A family once told me they were “fine during the day.” It turned out “fine” meant terrible only four times, every day, in the same four moments. That is not fine. That is a pattern wearing a disguise.
Night pain, shower pain, stair pain, and car-transfer pain usually point to different tools
Night pain may be about positioning, swelling management, or the effort of turning. Shower pain may be about standing tolerance, slippery fear, or the difficulty of stepping over a tub wall. Stair pain can involve balance, confidence, rail support, and pacing. Car-transfer pain is its own odd little opera: low seat, twisting, timing, and too many limbs moving at once. If nighttime discomfort keeps dominating the house, it can help to read more specifically about why hip pain gets worse at night or, for spine-driven patterns, how sleep setup changes sciatica at night.
When families separate these moments, the equipment list becomes calmer and more accurate.
Let’s be honest: many families buy for the scariest scenario, then struggle with the everyday one
The scariest scenario gets all the drama. The everyday one gets all the wear. If the patient showers every day and struggles every single time, bathroom equipment may deserve more attention than a dramatic emergency-style purchase that sits unused in a corner like a very expensive coat rack.
Decision Card: Buy for pain spike or buy for worst-case fear?
Choose pain-spike-first when the same task causes strain daily and safe repetition matters more than theoretical scenarios.
Choose worst-case-ready when falls, inability to transfer, or post-op restrictions create a serious short-term safety issue.
Time trade-off: pain-spike-first gives faster day-to-day relief. Worst-case-ready may feel safer emotionally but can overfill the home.
Neutral action: Circle the one task repeated most often in a 24-hour period.
Walker, Cane, or Transfer Aid? Choose by Function, Not Hope
A walking aid helps with movement, but not every device helps with transfers
A cane or walker may help with walking tolerance, balance, or offloading weight depending on the clinical context. But walking is not the same as transferring. A person can walk 20 careful steps and still struggle badly getting out of bed, rising from a recliner, or pivoting into a bathroom.
This is where households often get tricked by overlap. A walker looks supportive, so people assume it will support everything. It will not. In some situations it helps. In others it simply becomes a prop the body clings to while doing the real hard thing badly.
Transfer poles, bed rails, and gait belts solve different problems than canes and walkers
Transfer tools are about leverage, direction, hand placement, and controlled movement. They are not general mobility heroes. A bed rail may help repositioning, but it will not fix a too-low sofa. A transfer pole may help with standing from a favorite chair, but not with shower entry. A gait belt can improve caregiver control during movement, but only if the task and training are appropriate. Tools have personalities. Some are good at lifting the plot. Some are only good in one chapter.
Why “more support” can still be the wrong support in a narrow hallway or crowded bedroom
Home layout matters. A device can be objectively good and practically terrible in a cramped apartment, around a thick rug edge, beside a crowded bed, or in a bathroom where the door swings inward like it owns the place. More support can mean more width, more turning radius, and more snag points.
That is why function beats hope. Hope says, “This looks sturdy.” Function asks, “Can we actually use it three times before breakfast?”
Show me the nerdy details
When comparing movement equipment, measure usable clearance, not just room size. Include door trim, furniture corners, bed overhang, and the actual angle needed for turning or pivoting. A device that fits in theory can still fail in motion.
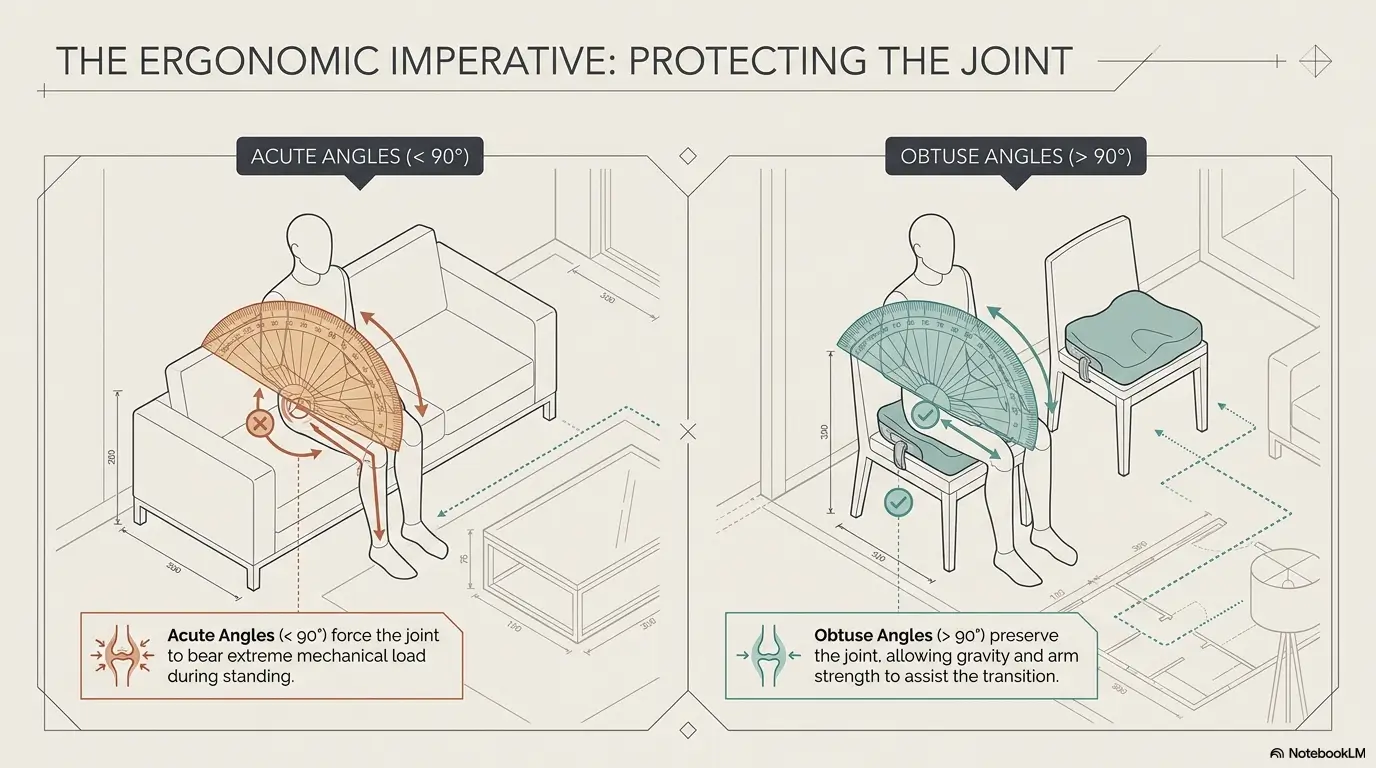
Bedroom Setup Matters More Than People Think
Wedges, leg lifters, overbed tables, and bedside commodes each change pain in different ways
The bedroom is where pain becomes less polite. Daytime adrenaline fades. The mattress either helps or betrays you. Repositioning takes effort. Toileting at night adds urgency and wobble. This is why bedroom equipment deserves more respect than it usually gets.
Wedges can change angle and ease certain positioning challenges. Leg lifters can reduce awkward bending or pulling. Overbed tables may look unromantic, but they can reduce repeated reaching, twisting, and the nonsense of standing up just to get one glass of water or a medication box. A bedside commode may be unglamorous in the way thunderstorms are unglamorous, but utility is not a beauty contest. For readers weighing whether the sleep surface itself is part of the problem, it may help to compare recliner versus bed recovery setup after shoulder surgery or even how mattress topper height changes comfort and support.
Bed height can quietly shape pain during standing, sitting, and repositioning
This is one of the most overlooked issues in the house. If the bed is too low, standing becomes a squat with consequences. If it is too high, getting in and out becomes a little leap of faith no recovering joint requested. A “nice bed” can still be a bad working surface.
I once watched a family discuss pillows for 20 minutes while the true problem sat there smugly at shin height. Bed height was the villain. Pillows were just the chorus.
Here’s what no one tells you: some pain at night is really a setup problem wearing a medical mask
Not all nighttime pain is mysterious healing pain. Some of it is mechanical. Reaching too far. Turning without leverage. Getting up too often because essentials are scattered. A better bedroom setup can reduce the number of painful repetitions, which matters because repetition is where suffering becomes household atmosphere.
- Check bed height before buying large equipment
- Move essentials within one easy reach zone
- Reduce night walking if safe alternatives exist
Apply in 60 seconds: Sit on the bed edge and notice whether standing feels like pushing up, climbing down, or dropping into space.
Mini Calculator: Which room deserves the first fix?
Add up three numbers for each room: daily painful tasks + near-falls or unstable moments + caregiver assists needed.
Output: Start with the room that has the highest total. That is usually where equipment delivers the fastest relief.
Neutral action: Score bedroom, bathroom, and living room tonight on a scrap of paper.
Bathroom First, Pride Second
Shower chairs, tub transfer benches, grab bars, and raised toilet seats are not interchangeable
The bathroom compresses risk. Water, hard surfaces, urgency, pain, and fatigue all crowd into a very small stage. That is why bathroom tools are often more valuable than families expect and more specific than marketing suggests.
A shower chair helps with standing tolerance while bathing. A tub transfer bench helps with stepping over a tub wall by turning the event into a seated transfer. Grab bars provide stable support when properly installed and placed for the actual motion needed. Raised toilet seats change the sit-to-stand angle. These are not duplicate tools. They solve different mechanical headaches. If the household is dealing with hip recovery, the logic becomes even clearer in guides about showering after hip surgery and support choices for painful stairs when bathroom access includes level changes.
Wet-floor pain management is also fall-risk management
Once water enters the story, pain management and safety management become roommates. A person in pain may move more slowly, brace strangely, or rush because they want the whole ordeal over with. That combination can turn a routine shower into the most dangerous five minutes of the day.
Bathroom dignity matters, but so does not slipping while pretending dignity can substitute for equipment. Pride is lovely. Fractures are not.
A bathroom tool that feels “too much” on day one can become the most-used item by week two
Families often resist bathroom equipment because it feels like a visible admission. But visible admission is not failure. It is adaptation. And adaptation, in a home-care setting, is often the difference between repeated strain and sustainable routine.
Many households later say the bathroom fix was the purchase they resisted most and appreciated fastest. The room that feels emotionally difficult is often the room that is physically honest.
Infographic: Match the Tool to the Moment
Standing from toilet hurts
Look at seat height, arm support, stable grab points, and turning space.
Stepping into tub hurts
Compare transfer bench, hand support, and whether a seated entry reduces twist.
Turning in bed hurts
Check wedge angle, rail support, bed height, and reach zone placement.
Walking to bathroom hurts
Look at path lighting, floor clutter, footwear, and transfer timing.
Do Not Buy the Whole Catalog at Once
The most expensive setup is often the one built from fear instead of routine
Fear shops fast. Routine shops well. When families panic, they buy broad solutions for narrow problems and narrow solutions for broad problems. The result is familiar: a large chair no one sits in, a rail attached to the wrong bed, a walker parked in a house where transfers are the true issue, and six smaller missing tools that would have actually changed the day.
There is a special kind of discouragement that comes from spending a lot and still struggling at breakfast. Avoid that feeling if you can.
Families often overbuy large equipment and underbuy small daily-use helpers
Big items feel like action. Small items feel optional. Yet daily-use helpers often deliver the most practical relief. Reachers, positioning pillows, non-slip supports, dressing aids, bed caddies, long-handled bathing tools, and stable seating changes can dramatically reduce the number of painful reaches, bends, twists, and wobbly improvisations.
Small tools are the commas of caregiving. Not glamorous. Utterly necessary for the sentence to breathe.
Why a phased equipment plan usually beats the panic-cart approach
A phased plan lets the household learn. Start with one or two changes in the highest-friction room. Test them. Notice whether pain episodes, near-falls, or caregiver strain decrease. Then move to the next layer. This approach preserves money, space, and mental clarity.
It also leaves room for recovery to change. What feels essential in week one may be irrelevant in week six. That is not wasteful if you rented smartly or bought selectively. It is simply honest.
Quote-Prep List: Gather this before comparing equipment
- Doorway width and bathroom entry width
- Toilet height, bed height, and favorite chair height
- Tub wall height or shower threshold details
- Daily pain-trigger list in order of frequency
- How long the equipment is likely needed
Neutral action: Put these measurements in your phone notes so you do not shop from memory fog.
Don’t Ignore the Caregiver’s Body in the Math
A device that helps the patient but injures the helper is not a good long-term solution
This deserves more airtime. Family caregiving has a way of turning helpers into invisible equipment. They become the extra hand, the lifting force, the pivot point, the reminder system, the emotional shock absorber. But if the home setup depends on the caregiver twisting, pulling, catching, or half-carrying every day, that setup is already failing.
The body of the helper counts. Back strain counts. Wrist pain counts. Interrupted sleep counts. Quiet dread before the next transfer counts.
Equipment should reduce twisting, lifting, and awkward reaching for everyone in the room
When comparing options, look for what reduces bad mechanics. Does the device improve hand placement? Does it reduce the need to pull upward from a bad angle? Does it shorten the reach? Does it let the patient participate more safely in the movement instead of becoming a passive load? That is a humane question for both people.
I once heard a daughter say, “I just need something for my mom.” What she needed, in truth, was also something for her own spine. Those two needs were not in conflict. They were married.
When family burnout begins as back strain, wrist pain, and interrupted sleep
Burnout rarely announces itself with trumpets. It arrives as little body complaints and resentments nobody wants to admit. The helper starts sleeping lightly. The transfer routine gets shorter and rougher. The patience runs thin. A better equipment choice can protect not just safety, but tenderness.
- Reduce helper lifting whenever possible
- Prefer tools that improve shared body mechanics
- Notice when the caregiver is compensating for bad setup
Apply in 60 seconds: Ask, “What move in this room makes my own body brace?”
Compare by Friction: Which Equipment Makes Daily Life Easier to Repeat?
The best item is often the one that gets used correctly without reminders
Repeatability matters more than aspirational features. The best equipment is often not the fanciest. It is the item that fits the room, fits the body, fits the routine, and gets used without a daily debate. If it requires a speech every time, it may not survive ordinary life.
Low-friction tools win because pain already consumes so much mental bandwidth. The brain in recovery is busy. The family is busy. Simplicity is not laziness. It is engineering for real humans.
Storage, cleaning, portability, and setup time matter more than families expect
A chair that works beautifully but is miserable to clean may get sidelined. A bench that blocks the whole bathroom may create a new household feud. A device that is hard to move from room to room may end up stranded where it is least needed. These practical details are not side notes. They are adoption rates wearing ordinary clothes.
If it is hard to move, hard to clean, or hard to explain, it may quietly fail at home
This is what I mean by friction. Some tools fail loudly. Others fail softly. They remain technically available but practically abandoned. The best comparison question is not “Does this help?” It is “Will this still be used on a tired Tuesday when everyone is annoyed?”
If the answer is no, keep looking.
Show me the nerdy details
In home use, adherence often improves when a tool reduces setup steps and works in the same physical pattern each time. Repetition loves consistency. The fewer micro-decisions required, the better the odds the equipment becomes part of the routine instead of a separate event.
Common Mistakes Families Make When Comparing Home Care Equipment
Buying for diagnosis labels instead of movement problems
“Hip pain.” “Back pain.” “Knee surgery.” Those labels matter medically, but they are not precise enough for shopping. Two people with the same diagnosis can struggle with entirely different tasks. One cannot step into the shower. Another cannot rise from a low chair. Another can walk fairly well but cannot turn in bed without sharp pain. Buy for movement problems, not just diagnosis nouns. That same principle matters when symptoms and imaging do not line up neatly, which is why some readers may also benefit from what to do when an X-ray looks normal but pain continues or understanding MRI findings that do not match the pain pattern.
Assuming temporary pain does not require environmental changes
This is a sneaky mistake. Families tell themselves, “It’s only for a short time.” Sometimes that is true. But short-term pain repeated many times a day is still a large burden. Temporary does not mean trivial. A two-week bathroom problem can feel like two months when it happens on a wet floor.
Choosing compact gear that saves space but creates instability
Minimalism can become a trap. Compact gear may look easier to store, but if it is less stable, harder to use, or mismatched to body size and motion, it may create more risk than value. A home should not become cluttered, but neither should it become a shrine to sleek bad decisions.
Buying online without measuring doorway width, toilet height, bed height, and tub edge
This is the most ordinary expensive mistake. The device arrives. The box is hopeful. Then reality speaks. It does not fit. Or it fits the room but not the turn. Or it fits the turn but not the person’s body mechanics. Measure first. Shopping without measurements is just optimism in shipping form.
Forgetting that pain management also depends on sleep position, reach distance, and transfer angle
Families often focus on the object and forget the choreography. But pain at home is a movement story. Angle matters. Distance matters. Timing matters. Where the hand lands matters. Where the feet start matters. Even where the tissues box lives matters if it prevents three extra standing motions a day.
The home is not static. It is a score. Equipment needs to fit the music.
Cost Traps and Coverage Gaps: What Looks Cheap Can Get Expensive Fast
Low-cost equipment may fail if it must be replaced, upgraded, or supplemented immediately
The cheapest option is not always the lowest-cost outcome. If an item wobbles, fits poorly, or solves only half the problem, families may end up buying twice. Cheap can be expensive when it delays relief, creates frustration, or forces additional purchases right away.
This does not mean you need premium everything. It means false economy is real.
Rental versus purchase can change the decision for short recovery windows
For large items needed for a short period, rental may be worth considering. For smaller, lower-cost items used many times a day, purchase may make more sense. The right answer depends on likely duration, hygiene preferences, storage space, return policies, and whether the recovery path is clear or still evolving.
Sometimes the smartest financial move is not a product choice at all. It is a timing choice.
Why insurance language, prescription requirements, and HSA/FSA eligibility can alter the real cost
Before paying out of pocket for a large item, it may be worth checking whether a prescription, clinician recommendation, or durable medical equipment pathway affects cost. Depending on the situation, some households also look into HSA or FSA rules for eligible purchases. None of this is glamorous, but paperwork occasionally saves more pain than gadgets do. If out-of-pocket costs are shaping the decision, related guides on orthopedic pain management with a high deductible plan, estimating imaging costs under an HDHP, and which braces and supports may be HSA-eligible can help families think more clearly before they buy.
Coverage Tier Map: How the decision changes
Tier 1: Small self-pay items, fast to test, low storage burden.
Tier 2: Medium-cost daily-use tools where fit matters more than features.
Tier 3: Large equipment where room measurements and timeline matter.
Tier 4: Items that may benefit from clinician input or documentation.
Tier 5: Unsafe transfer situations where professional evaluation matters more than bargain-hunting.
Neutral action: Sort each item you are considering into one tier before buying.
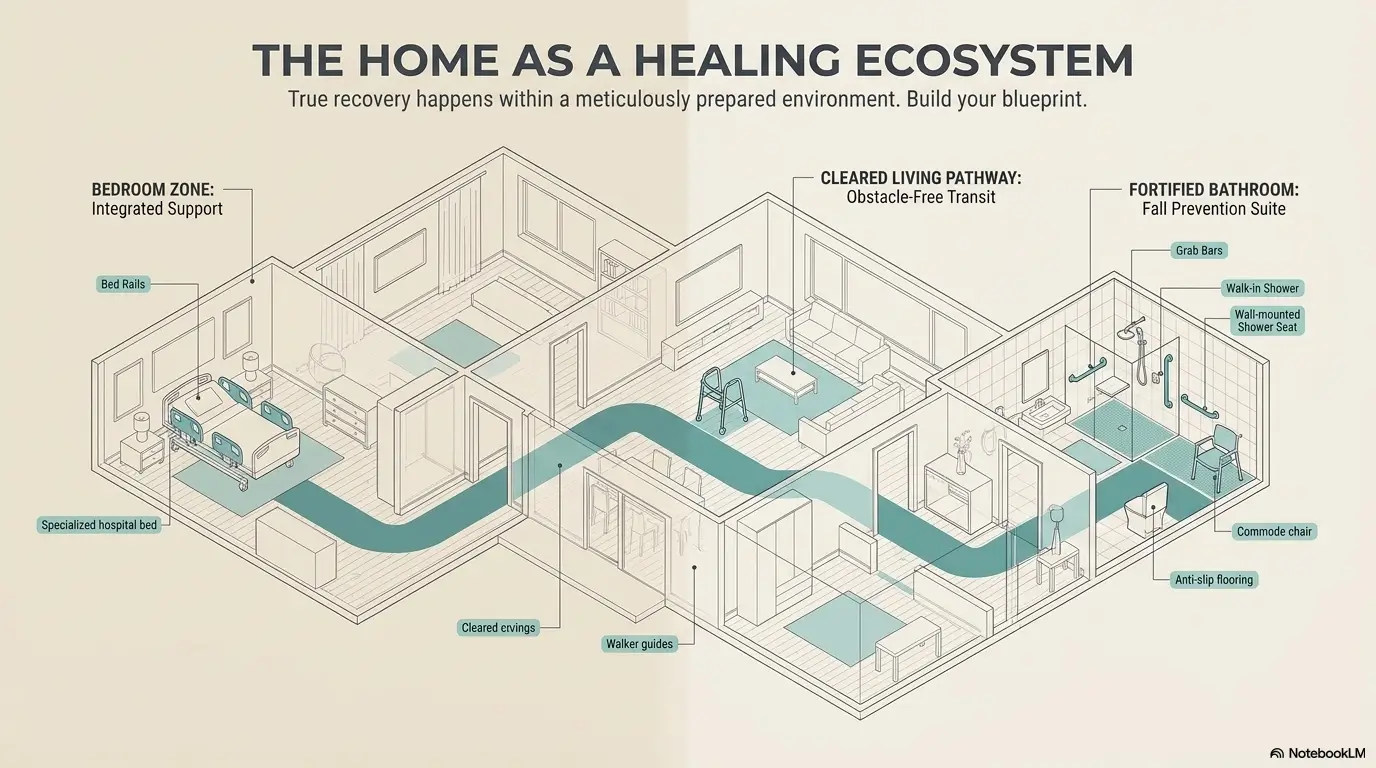
One Room at a Time: How to Build a Smarter Home Setup Without Overwhelm
Start where pain, instability, or caregiver strain happens most often
When a family is overwhelmed, “the whole house” is too much. Start with one room. The smartest first room is usually where pain frequency and risk overlap. That is often the bathroom or bedroom, though not always. Sometimes the real battle is a favorite recliner in the living room because that is where someone spends 8 hours a day and cannot stand without assistance.
Test one or two high-impact changes before expanding the setup
A good first round often includes one primary support item and one environmental change. For example: raised toilet seat plus clearing the bathroom pathway. Or wedge pillow plus bed-height adjustment. Or transfer bench plus moving towels and toiletries into easy reach. Small paired changes can outperform one large purchase made in isolation.
Use a simple comparison sheet: task, pain point, current barrier, likely tool, space needed
This works because it turns emotion into observation. Make a five-column list:
- Task
- Pain point
- Current barrier
- Likely tool
- Space needed
That sheet becomes your filter. It keeps the household from buying a dramatic object that solves no recurring problem. It also helps conversations with a physical therapist, occupational therapist, surgeon’s office, or durable medical equipment supplier go more smoothly because you are describing function, not panic. When formal rehab support is part of the next step, families often find it useful to compare how to choose rehab after surgery or what to do when physical therapy is not helping orthopedic pain the way they expected.
Short Story: A family I once advised kept asking whether they needed a walker upgrade, a new recliner, or a lift chair. Everything felt urgent, and the living room had become a parade of tabs, screenshots, and half-finished carts. We paused and watched the day instead. The hardest moment was not walking across the room. It was getting off the toilet, especially at night, when pain, urgency, and fatigue collided.
The second hardest moment was turning in bed. They changed two things first: bathroom support and bedside setup. Within days, the household felt less frantic. Not perfect. Not miraculous. Just less punishing. The future purchases became clearer after that. The walker question did not disappear, but it stopped pretending to be the only question. That is often what good equipment decisions do. They do not solve the whole story at once. They make the next page readable.
- Fix the highest-friction room first
- Pair one tool with one layout change
- Use observation, not fear, to set priorities
Apply in 60 seconds: Pick one room and write its most painful task at the top of a page.
When to Seek Help
Pain that sharply worsens despite rest, positioning, and prescribed care needs medical follow-up
Home equipment can reduce strain, improve access, and support safer routine. It cannot explain every worsening symptom. If pain escalates sharply, suddenly behaves differently, or stops responding to the plan already given by the treating clinician, that deserves follow-up rather than more shopping.
New numbness, fever, swelling, shortness of breath, falls, or inability to bear weight should not be handled as a shopping problem
There are moments when the question is no longer “Which tool helps?” but “Who do we call?” That threshold matters. Equipment decisions belong to home management. Red-flag symptoms belong to clinical attention. Keeping those categories separate protects everyone. For readers trying to sort urgency, it can help to compare whether symptoms belong in urgent care versus an orthopedic clinic, or whether the situation has crossed into true low-back-pain emergency territory.
If transfers feel unsafe for either the patient or the caregiver, ask a clinician, PT, or OT for equipment guidance
There is wisdom in getting help early. A short professional assessment can prevent a long and expensive chain of trial-and-error purchases. It can also protect dignity. Good guidance is not an admission of incompetence. It is a way of reducing guesswork when the body has become complicated.
Organizations such as AAOS, the National Institute on Aging, and the American Occupational Therapy Association all emphasize, in different ways, the practical value of matching support to function and environment. In real homes, that matters more than heroic improvisation. And when households are stuck not on equipment but on the next clinical step, they may need to think through telehealth versus in-person orthopedics, orthopedic referral wait times, or even how to respond to a denied second opinion for orthopedic pain.
FAQ
What home care equipment helps most with orthopedic pain at home?
The answer depends on the hardest task. Common high-impact items include walkers, shower chairs, raised toilet seats, transfer benches, wedges, braces, reachers, and bedside supports. The best choice usually matches a specific pain-triggering activity, not a generic diagnosis.
Is a lift chair worth it for orthopedic pain management?
Sometimes, especially when sit-to-stand transitions are a major pain point. But a lift chair is not a universal solution. It helps some families most when knee, hip, or back pain makes rising difficult, yet it may not solve walking safety or bathroom access.
Should families rent or buy orthopedic home equipment?
Short recovery windows often make rentals attractive for large items, while daily-use smaller tools may make more sense to buy. The better decision depends on duration of need, storage space, hygiene concerns, and whether the equipment may still be needed after the acute phase.
What is the biggest mistake families make when comparing home-care equipment?
Buying by product category before identifying the exact moment pain spikes. Many families think in terms of “we need support equipment,” when the real issue is something narrower like shower entry, bed repositioning, or toilet transfers.
Can the wrong equipment make pain worse?
Yes. Poor fit, wrong height, awkward angles, and unstable placement can increase strain, stiffness, and fear of movement. Equipment that seems supportive in theory can become painful in actual daily use.
Which room should families fix first for orthopedic pain management?
Usually the room where pain and risk combine most often. For many households, that means the bathroom or bedroom first, because transfers, wet surfaces, and nighttime movement create repeated strain.
Do families need a physical therapist or occupational therapist to choose equipment?
Not always for every small item, but professional input can be especially valuable when transfers feel unsafe, mobility is declining, or multiple devices seem possible. A short visit can prevent expensive trial-and-error buying.
Are small tools sometimes more useful than big equipment?
Very often. Reachers, wedges, non-slip supports, leg lifters, positioning pillows, and toilet aids can shape daily pain more than a bulky purchase that only solves one moment.
Next Step
Walk through the home tonight and write down the three moments when pain, instability, or caregiver strain show up most often, then compare equipment only against those three problems first. That one act closes the loop we opened at the start. The house stops feeling like a vague medical problem and starts becoming a map.
You do not need a perfect setup by tomorrow. You need a truer one. In the next 15 minutes, pick one room, one painful task, one barrier, and one likely tool. That is how clutter loses and care gets smarter.
Safety / Disclaimer
This content is educational and not a substitute for medical advice, diagnosis, or treatment. For new injuries, severe pain changes, post-surgical concerns, or unsafe transfers, follow the treating clinician’s instructions and seek prompt medical guidance.
Differentiation Map
| What competitors usually do | How this article avoids it |
|---|---|
| Lists equipment by category with generic pros and cons | Organizes the article around pain-triggering moments and household tasks |
| Treats pain management as a patient-only issue | Includes caregiver strain, transfer safety, and room-by-room workflow |
| Pushes “best products” language too early | Forces problem-definition before comparison |
| Uses bland sections like benefits, types, and conclusion | Uses differentiated, intent-rich headings built for scanning and passage ranking |
| Focuses on diagnosis labels | Focuses on function, friction, and repeatability in real homes |
| Ignores overbuying and space constraints | Includes clutter risk, phased buying, and home-layout realities |
| Keeps bathroom and bedroom advice shallow | Gives those zones dedicated decision logic because they drive daily pain most often |
Last reviewed: 2026-04.
