
Preserving Independence: A Guide to Orthopedic Pain Management
Orthopedic pain management for older adults living alone is not just about getting pain down from a 7 to a 4. It is about protecting the daily movements that keep independence intact: walking to the toilet, bathing without fear, eating before medication, sleeping safely, and knowing when to call for help.
When families guess, small gaps grow teeth. A missed dose, a dark hallway, a curled rug, or one “good day” of overdoing chores can turn manageable joint, hip, knee, or back pain into a fall risk.
This guide helps you build a safer pain-and-function routine without panic-buying equipment or treating grit like a treatment plan. You will learn:
- What to track and which home hazards matter first.
- How to make check-ins more useful.
- Recognizing when mobility changes deserve professional help.
Table of Contents

Safety / Disclaimer
This article is educational guidance, not personal medical advice. Older adults should talk with a doctor, pharmacist, physical therapist, orthopedic specialist, or other qualified clinician before changing medication, exercise, walking aids, or treatment routines.
This matters because pain decisions are rarely isolated. A pill can affect balance. A sore knee can change how someone walks to the bathroom at 2 a.m. A “minor” fall can become a major turning point if nobody hears it happen.
The CDC states that falls are the leading cause of injury for adults 65 and older, and more than 14 million older adults report falling every year. That is not a reason to panic. It is a reason to build a plan before the house becomes an obstacle course with furniture.
- Do not change doses without medical guidance.
- Report falls, dizziness, confusion, or sudden weakness promptly.
- Use routines that protect function, not just comfort.
Apply in 60 seconds: Put your doctor’s office number, pharmacy number, and one emergency contact beside the main phone today.
Start Here: Living Alone Changes the Pain Math
Pain Is Not the Only Problem
When someone lives alone, orthopedic pain becomes more than a sensation. It becomes a logistics problem. Can the person reach the bathroom safely? Can they prepare food? Can they stand long enough to shower? Can they remember whether the morning dose already happened?
I once watched an older neighbor measure her day by the distance between the recliner and the kettle. Her hip pain was real, but the scarier issue was the tiny negotiation before every step: “Can I make it there and back?” That is the pain math of living alone.
The Real Question: Can You Still Move Safely?
A pain score of 6 out of 10 tells part of the story. A person who can still rise from a chair, walk steadily, eat, drink, use the toilet, and sleep may be uncomfortable but functioning. A person with “only” a 4 out of 10 who is skipping showers, avoiding stairs, or leaning on unstable furniture may be at higher risk.
Function is the quiet scoreboard. It shows whether the plan is working in real life, not just on paper.
Why “I’ll Just Push Through” Gets Riskier After 65
Stoicism has good manners, but terrible night vision. Many older adults grew up believing that pain should be endured politely. The problem is that pushing through can lead to overuse, limping, poor sleep, missed meals, and falls.
Independence does not mean doing every task alone at full difficulty. Independence means designing the day so fewer tasks become dangerous. A walking aid, a shower chair, a medication review, or a five-minute family call is not surrender. It is scaffolding.
Pain-and-Safety Loop
Joint, back, hip, knee, or post-injury discomfort changes movement.
Walking, bathing, cooking, stairs, and sleep become the real test.
Fatigue, dizziness, clutter, and poor lighting can turn pain into danger.
Medication review, room setup, check-ins, and therapy close the loop.
Who This Is For, and Who This Is Not For
This Is For Older Adults Managing Joint, Back, Hip, Knee, or Post-Injury Pain at Home
This guide is for someone who can still live at home but notices pain reshaping the day. Maybe the knee complains before breakfast. Maybe the shoulder turns dressing into a small weather event. Maybe a recent fall, sprain, arthritis flare, or surgery has made ordinary routines feel uncertain.
It is also for the person who keeps saying, “I’m fine,” while quietly doing less each week. Fewer walks. Fewer showers. Fewer cooked meals. More time waiting for pain to “settle down.” The body often whispers before it shouts.
This Is For Families Checking In From Across Town or Another State
Adult children and caregivers often hear one sentence: “Everything is okay.” Helpful, yes. Complete, no. A better system asks about function: walking, bathing, eating, medication timing, bathroom trips, and sleep.
A family member does not need to become a hovering helicopter with a medical degree and a clipboard. The goal is a small rhythm of useful questions, clear escalation points, and one nearby backup person when distance becomes a problem.
This Is Not a Substitute for a Doctor, Pharmacist, or Physical Therapist
Orthopedic pain can come from arthritis, fracture, nerve irritation, tendon injury, infection, medication effects, or other causes. Some need rest. Some need guided movement. Some need imaging or urgent care. Some need a medication change that should not be improvised over toast.
Use this article to organize safer questions and routines, then bring those questions to the right professional.
Eligibility Checklist: Is a Home Pain-and-Safety Plan Needed?
- Yes / No: Pain has changed walking, bathing, stairs, cooking, or sleep.
- Yes / No: The person lives alone for most of the day or night.
- Yes / No: Medication timing, dizziness, or drowsiness is unclear.
- Yes / No: There has been a fall, near-fall, or sudden mobility change.
Neutral next step: If two or more answers are “Yes,” make a one-page plan and contact the clinician or pharmacist for the medication and mobility pieces.
The First 24 Hours: What to Track Before You Try to Fix Everything
Write Down Pain, Walking, Sleep, Meals, and Bathroom Trips
The first day is not for solving the whole opera. It is for listening to the instruments. Write down when pain is worst, what makes it better, what makes it worse, and which daily tasks are getting smaller.
Use plain language. “Knee bad after standing at sink for 8 minutes” is more useful than “pain worse.” “Bathroom trip at night felt unsteady” is more useful than “slept poorly.” Clinicians can work with specifics. Vague misery is harder to treat.
Track Function, Not Just Pain Numbers
A simple 0-to-10 pain number is useful, but it should travel with a function note. For example:
- Pain 4, walked to mailbox safely.
- Pain 5, skipped shower because standing felt unsafe.
- Pain 3, woke twice and rushed to bathroom.
- Pain 6, needed both arms to rise from chair.
That small detail changes the conversation. It turns “my back hurts” into “my back hurts and it is changing how I move through my home.” That is a much clearer flare signal.
Tiny Clues Matter: Stairs, Showers, Laundry, and Getting Out of Bed
The risky moments are rarely dramatic at first. They hide in the ordinary: stepping over laundry, turning in the shower, carrying soup, reaching for a dropped cane, or standing too quickly after pain medicine.
In one family I helped organize, the breakthrough was not a new gadget. It was moving clean towels from a high bathroom shelf to waist height. Nobody clapped. Nobody needed to. The shower became less of a stunt.
Show me the nerdy details
Tracking function helps separate pain intensity from safety risk. Two people can report the same pain score but have very different fall risk depending on gait, sleep, medication side effects, bathroom urgency, lighting, and whether they can rise from a chair without grabbing unstable furniture.
Medication Safety: The Part That Needs a Second Pair of Eyes
Keep One Current Medication List in Plain Sight
Medication safety is where a calm second set of eyes earns its keep. The American Academy of Orthopaedic Surgeons advises patients to keep an accurate list of prescriptions, over-the-counter medications, supplements, allergies, and prior surgeries when preparing for orthopedic care.
That list should not live only in a patient portal nobody can find during a stressful morning. Put one copy near the main phone. Put another in a wallet or bag. Include dose, timing, purpose, prescriber, and pharmacy.
Don’t Mix “Old Prescriptions” With New Pain
Old pain pills have a seductive little voice: “Remember me? I helped last time.” Do not let a forgotten bottle become the household pharmacist. Medication that was appropriate after one injury may be unsafe with a new diagnosis, new kidney function, new blood thinner, new sleep aid, or new fall risk.
Expired medications, duplicate prescriptions, and borrowed pills are especially risky for older adults living alone because nobody may notice side effects until function drops.
Ask Before Adding Over-the-Counter Pain Relievers
Over-the-counter does not mean consequence-free. Ibuprofen, naproxen, acetaminophen, creams, patches, sleep aids, and supplements can interact with prescriptions or health conditions. AAOS notes in its osteoarthritis guidance that patients should check with their primary care doctor before starting new medication to avoid possible interactions.
A pharmacist can often review a list in minutes. That short conversation may prevent a long afternoon of dizziness, stomach trouble, confusion, constipation, or a risky overlap.
Here’s What No One Tells You: Relief Can Still Increase Fall Risk
Pain relief can help someone move better. It can also make someone feel bold before balance has caught up. Some medications may cause drowsiness, dizziness, constipation, slower reaction time, or confusion. Add a dark hallway and a full bladder, and suddenly the floor has opinions.
The goal is not “no pain at any cost.” The goal is enough relief to move safely.
- Keep one current medication list visible.
- Ask before adding over-the-counter pain relievers.
- Watch for dizziness, drowsiness, constipation, and confusion.
Apply in 60 seconds: Place all current medication bottles on one table and photograph the labels for your next pharmacist call.
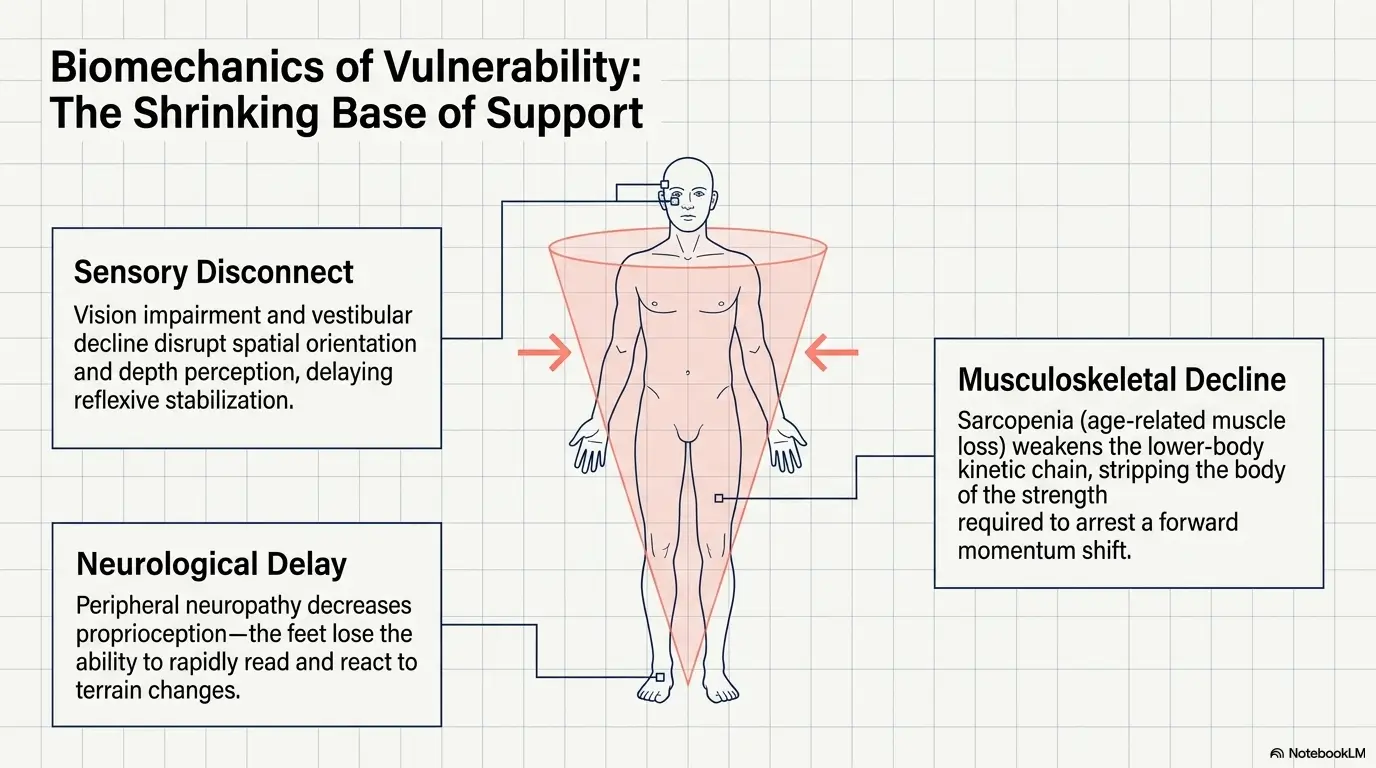
Movement Windows: Use Pain Relief When the Body Is Most Ready
Plan Small Tasks Around the Best Part of the Day
Many older adults have a daily “best window,” even during pain flares. It may be late morning after stiffness eases. It may be early afternoon before fatigue arrives wearing muddy boots. The plan should place harder tasks inside that window, not at the ragged edge of the day.
Think of movement as a budget. Spend it on high-value tasks first: bathroom safety, meals, gentle walking, prescribed exercises, hygiene, and getting to appointments. Low-value tasks can wait. Dust has never called 911.
Sit Before You Are Desperate, Not After You Are Shaking
Rest breaks work best when they arrive early. Waiting until the legs tremble often means the next movement is already less controlled. A simple rule helps: sit after 10 to 15 minutes of standing during a flare, or sooner if pain, dizziness, or weakness appears.
This is not laziness. It is pacing. Athletes call it load management and get entire staff meetings about it. Older adults deserve at least a chair.
The “One Chore Too Many” Trap
A good morning can become a bad evening because the person “felt okay” and did laundry, dishes, groceries, bedding, and a small furniture rearrangement that somehow became a private Olympic event.
Orthopedic pain often punishes delayed accounting. The bill arrives after dinner. A safer approach is to stop while there is still capacity left, not when the body has already filed a complaint.
Let’s Be Honest: Independence Should Not Require White-Knuckle Grit
There is a cultural romance around doing everything alone. It sounds noble until someone falls between the bed and bathroom because they did not want to “make a fuss.” Real independence is quieter. It has a lamp. A phone. A walker adjusted to the right height. A neighbor who can be called. A plan that does not require hero music.
Decision Card: One Big Chore Block vs. Small Movement Clusters
| Option | Best When | Trade-Off |
|---|---|---|
| One big chore block | Rarely ideal during pain flares | Higher fatigue, more rushed steps, more evening pain |
| Small movement clusters | Most safer home routines | Requires planning, but protects balance and energy |
Neutral action line: Choose the hardest repeated task today and split it into two smaller rounds with a seated break between them.
Home Setup: Make the Pain Plan Visible in the Room
Put Supplies Where the Pain Actually Happens
Home setup should follow pain, not interior design. If knee pain is worst at the recliner, keep the phone, water, medication list, glasses, remote, and charger within safe reach there. If back pain is worst in the morning, place supportive shoes, a robe, and a walking aid near the bed.
The best setup feels slightly boring. Boring is good. Boring means fewer surprises. Safety loves predictability the way cats love forbidden laundry.
Build a Safer Path From Bed to Bathroom
The bed-to-bathroom route deserves special respect. Nighttime pain, urgency, medication effects, and low light can turn a familiar hallway into a miniature obstacle course.
Improve the route with:
- Motion night lights or easy-to-reach lamps.
- Clear floor space with no cords, shoes, or loose rugs.
- A stable walking aid within reach before standing.
- A phone or alert device reachable from bed.
- Non-slip footwear that is easy to put on.
Remove the “Almost Fine” Hazards: Rugs, Cords, Low Lighting, Narrow Turns
“Almost fine” hazards are the worst kind because they survive inspection. A rug that only curls a little. A cord that is “usually” out of the way. A hallway that is bright enough during the day but swamp-dark at night.
The National Institute on Aging notes that home hazards can contribute to falls, and taking more medications can also increase fall risk. This is why the room and the medication list belong in the same conversation.
Make the Chair, Bed, and Shower Work Like a Team
A safe routine has stations. The bed supports standing. The chair supports rest. The shower supports hygiene without turning balance into a circus trick. Adjusting one station helps, but the whole route matters.
A chair that is too low can make knee or hip pain worse. A shower without stable support can make bathing feel optional. A bed that is too high or too low can make mornings dangerous before the day has even had coffee.
- Clear the bed-to-bathroom path first.
- Move supplies to where pain actually happens.
- Fix lighting before adding complicated equipment.
Apply in 60 seconds: Walk the bed-to-bathroom route in daylight and remove one trip hazard before tonight.
Common Mistakes That Make Orthopedic Pain Harder to Manage Alone
Mistake 1: Waiting Until Pain Is Severe Before Moving Carefully
People often protect themselves only after pain becomes dramatic. But safer movement works best before the body is shouting. Use supportive shoes, walking aids, lights, and rest breaks early in the flare, not after the hallway starts looking like a mountain pass.
Mistake 2: Saving Every Chore for One Big “Good Day”
The good-day trap is sneaky. Pain is lower, confidence rises, and suddenly the person tries to repay the entire week in one afternoon. By evening, swelling, fatigue, or limping may be worse.
Instead, treat good days as chances to pace well. A good day is not a blank check. It is a coupon with tiny print.
Mistake 3: Treating Sleep Loss Like a Minor Detail
Poor sleep can worsen pain sensitivity, mood, balance, and attention. It also makes medication timing messier. An older adult who sleeps badly may be more likely to rush, forget, or misjudge footing.
Track sleep alongside pain. A pattern of waking every 2 hours, struggling to turn in bed, or rushing to the bathroom deserves attention. For readers recovering from hip surgery, sleeping discomfort after hip replacement can be one of the clearest signals that the recovery setup needs another look.
Mistake 4: Using Furniture Instead of Proper Support
Furniture walking is common: one hand on the table, one hand on the wall, a little grab of the chair, a dramatic reach for the counter. It looks resourceful. It can also be unstable.
If someone is regularly using furniture to move through the home, that is a sign to ask about a proper walking aid, physical therapy, or a home safety review.
Mistake 5: Saying “I’m Fine” When Function Is Quietly Shrinking
“I’m fine” may mean “I’m scared this will change my life.” Families should hear the tenderness underneath it. The answer is not interrogation. It is better questions.
Ask what got harder this week. Ask what was avoided. Ask whether the shower, stairs, laundry, mail, meals, or nighttime bathroom trips have changed. Function tells the truth gently, then all at once.
Mini Risk Pattern Calculator
Count one point for each item that happened in the last 7 days:
- Skipped shower or changed bathing because of pain or balance.
- Used furniture instead of a cane, walker, or stable support.
- Had dizziness, confusion, drowsiness, or a near-fall.
Output: 0 points means keep tracking. 1 point means adjust the routine. 2 or 3 points means contact a clinician, pharmacist, or physical therapist for next steps.
Neutral action line: Write the score on the one-page plan and share it during the next check-in call.
Don’t Do This: Pain Habits That Can Create a Bigger Emergency
Don’t Take Extra Doses Without Medical Guidance
Taking extra medication may feel logical when pain is loud. It can also create overdose risk, interactions, dizziness, constipation, confusion, stomach bleeding, kidney strain, or dangerous sedation depending on the medication and health history.
Use the prescribing instructions. If the plan is not working, call the prescriber or pharmacist. Pain that keeps breaking through the plan is information, not an invitation to improvise chemistry in the kitchen.
Don’t Walk to the Bathroom Half-Asleep Without a Light Plan
Nighttime bathroom trips deserve their own protocol. Turn on a light before standing. Sit at the edge of the bed for a moment. Use the walking aid. Wear stable footwear. Move slowly enough that the body knows it has been promoted from sleeping to walking.
This ritual may take 30 extra seconds. That is cheaper than a fall.
Don’t Ignore New Weakness, Dizziness, Confusion, or a Fall
New weakness, dizziness, confusion, or a fall should be treated as a safety event. It may be related to medication, dehydration, infection, injury, blood pressure, or something more urgent. Do not cover it with optimism and a sweater.
If a person falls and cannot get up, has major injury, chest pain, severe shortness of breath, stroke signs, or sudden severe symptoms, call emergency services.
Don’t Hide Pain Because You Fear Losing Independence
This is the emotional knot. Many older adults underreport pain because they worry family will overreact. Families sometimes overreact because they receive too little information until the situation is already hot.
The better bargain is honesty plus proportion. Report changes early. Make small fixes early. Keep decisions collaborative. Independence is better protected by truthful details than by heroic silence.
Short Story: The Nightstand That Changed the Week
After a knee flare, one older man kept his phone charging across the room because “that’s where the outlet is.” At night, he would stand, shuffle, reach, and sometimes forget why he had gotten up. His daughter wanted a medical alert system immediately. He wanted everyone to calm down.
The first fix was almost embarrassingly small: a longer charging cable routed behind the nightstand, a lamp with a large switch, water with a lid, glasses in a tray, and a written medication schedule. A neighbor kept a spare key. Nothing glamorous happened. No one became a superhero. But the nighttime route shrank from six risky movements to two steadier ones. A week later, his daughter’s calls were shorter because the answers were clearer. The house had stopped arguing with his knee.
Check-In Scripts: What Families Should Ask Instead of “Are You Okay?”
Ask About Walking, Showering, Eating, Sleep, and Medication Timing
“Are you okay?” is a kind question with a trapdoor. It invites a one-word answer. Better questions make daily function visible without making the older adult feel audited.
Try these:
- “Did you walk less today because of pain or balance?”
- “Was the shower safe, or did you skip it?”
- “Did you eat a real meal before taking pain medicine?”
- “Any dizziness, constipation, confusion, or extra sleepiness?”
- “Was the bathroom harder overnight?”
Use “What Was Hardest Today?” Instead of “How Was Your Pain?”
“How was your pain?” often produces a number. “What was hardest today?” produces a scene. The stairs. The shower. The chair. The pharmacy bottle. The laundry basket sitting there with the quiet menace of a tax form.
Scenes are easier to fix than abstract pain. A hard shower may need a shower chair, grab bars, non-slip surfaces, or a clinician’s advice. A hard medication schedule may need a pill organizer or pharmacist review.
The Five-Minute Call That Reveals More Than a Long Lecture
A useful check-in can be short:
- Ask one function question.
- Ask one medication question.
- Ask one safety question.
- Agree on one next action.
The tone matters. Curiosity works better than command. “Let’s make tomorrow easier” lands softer than “You need to stop doing that.” Nobody enjoys being parented by their own child. Even when the child is right. Especially then.
When Distance Caregiving Needs a Backup Person Nearby
If family lives far away, choose one nearby backup person: neighbor, friend, building manager, faith community contact, home health worker, or local relative. That person does not need every detail. They need permission and a clear threshold for action.
For example: “If I do not answer by 9 a.m. after two calls, please knock and call my daughter.” Simple beats elaborate. In an emergency, the best plan is the one people can remember while wearing slippers.
Quote-Prep List: What to Gather Before Comparing Help Options
- Current medication list and pharmacy name.
- Recent fall, surgery, injury, or diagnosis details.
- Hardest daily tasks: shower, stairs, meals, bathroom, bed transfer.
- Insurance card and preferred clinic or orthopedic office.
- Photos of risky home areas, if the older adult agrees.
Neutral action line: Gather these before calling a home safety service, physical therapy office, medical alert company, or care coordinator.
When to Seek Help: Red Flags That Should Not Wait
Call 911 for Chest Pain, Severe Shortness of Breath, Stroke Signs, Major Injury, or Inability to Get Up After a Fall
Some symptoms do not belong in a wait-and-see basket. Call 911 for chest pain, severe shortness of breath, signs of stroke, major injury, severe bleeding, loss of consciousness, or inability to get up after a fall.
Stroke signs can include face drooping, arm weakness, speech difficulty, sudden confusion, sudden vision trouble, sudden severe headache, or sudden trouble walking. When symptoms are urgent, politeness should not slow the call.
Call a Doctor Promptly for New Severe Pain, Fever, Swelling, Wound Changes, or Sudden Mobility Loss
Orthopedic pain should be evaluated promptly when it is new, severe, worsening quickly, linked with fever, paired with redness or swelling, associated with wound drainage, or causing sudden loss of mobility.
After surgery or injury, follow the surgeon’s discharge instructions. If the instructions are unclear, call. “I didn’t want to bother anyone” has never been a reliable medical strategy. When the decision feels murky, families may also need to understand the difference between urgent care vs. orthopedic clinic visits before choosing where to seek help.
Ask a Pharmacist About Drowsiness, Dizziness, Constipation, Confusion, or Medication Overlap
Pharmacists are often underused safety allies. They can help identify duplicate medicines, sedating combinations, constipation risk, timing problems, and over-the-counter conflicts.
Ask directly: “Could any of these increase fall risk?” and “What side effects should make us call the doctor?” These are ordinary questions. No cape required.
Request Physical Therapy or Home Safety Support When Daily Tasks Are Shrinking
If walking distance, showering, stairs, meal preparation, or getting out of bed is shrinking, ask about physical therapy, occupational therapy, mobility aid fitting, or home safety support. The goal is not to force more activity. The goal is safer capacity. If therapy is already part of the plan but daily function keeps shrinking, it may help to review what to do when physical therapy is not helping orthopedic pain.
The CDC’s older adult fall data reinforces the scale of the issue: falls are the leading cause of injury among adults 65 and older. That makes prevention part of pain management, not a decorative extra.
- Call emergency services for major or sudden symptoms.
- Call a doctor for worsening pain, fever, swelling, wound changes, or mobility loss.
- Ask a pharmacist about side effects and overlap.
Apply in 60 seconds: Write “When to call” on the top of the one-page plan, then list the first three red flags that apply to the current situation.
FAQ
What is the safest way for an older adult living alone to manage orthopedic pain?
The safest approach combines clinician-approved pain treatment, medication safety, fall prevention, pacing, home setup, and check-ins. Pain relief should support safer movement, not encourage risky overactivity. A one-page plan with medication timing, red flags, emergency contacts, and the hardest daily tasks is a practical starting point.
How can I tell if pain is becoming a safety problem?
Pain is becoming a safety problem when it changes function. Warning signs include walking less, skipping showers, avoiding stairs, using furniture for support, missing meals, sleeping poorly, rushing to the bathroom, feeling dizzy, or having a fall or near-fall.
Should an older adult use heat or ice for orthopedic pain?
Heat and ice can help some orthopedic pain, but the right choice depends on the condition, timing, circulation, skin safety, sensation, and clinician guidance. Many people use ice for swelling or recent irritation and heat for stiffness, but older adults should ask a clinician if they have diabetes, reduced sensation, fragile skin, circulation problems, wounds, or recent surgery.
What should be kept near the bed for pain and mobility safety?
Useful bedside items may include a phone, charger, lamp or large-switch light, glasses, water with a lid, medication list, emergency contacts, stable footwear, and any prescribed walking aid. Keep the floor clear so reaching for these items does not create a trip hazard.
How often should family members check in after a fall, injury, or surgery?
The right frequency depends on the person’s risk, clinician instructions, medication effects, and home support. After a recent fall, injury, surgery, or medication change, daily check-ins may be reasonable until walking, sleep, bathroom trips, and medication timing are stable. Ask the clinician what monitoring schedule fits the situation.
What questions should caregivers ask about pain medicine?
Ask what the medicine is for, when it should be taken, what should not be mixed with it, whether food is needed, what side effects matter, and whether it can increase fall risk. Also ask what to do if pain is not controlled and when to call the doctor.
When should orthopedic pain be evaluated by a doctor?
Orthopedic pain should be evaluated when it is new, severe, worsening, follows a fall or injury, causes sudden mobility loss, comes with fever or swelling, affects wound healing, or prevents basic daily tasks. Pain that forces major changes in walking, bathing, sleeping, or eating deserves medical attention.
How can an older adult stay independent without ignoring pain?
Independence is best protected by early, practical support: safer room setup, honest tracking, medication review, appropriate mobility aids, physical therapy when needed, and a check-in plan. The goal is not to give up control. The goal is to reduce avoidable risk so daily life remains possible.
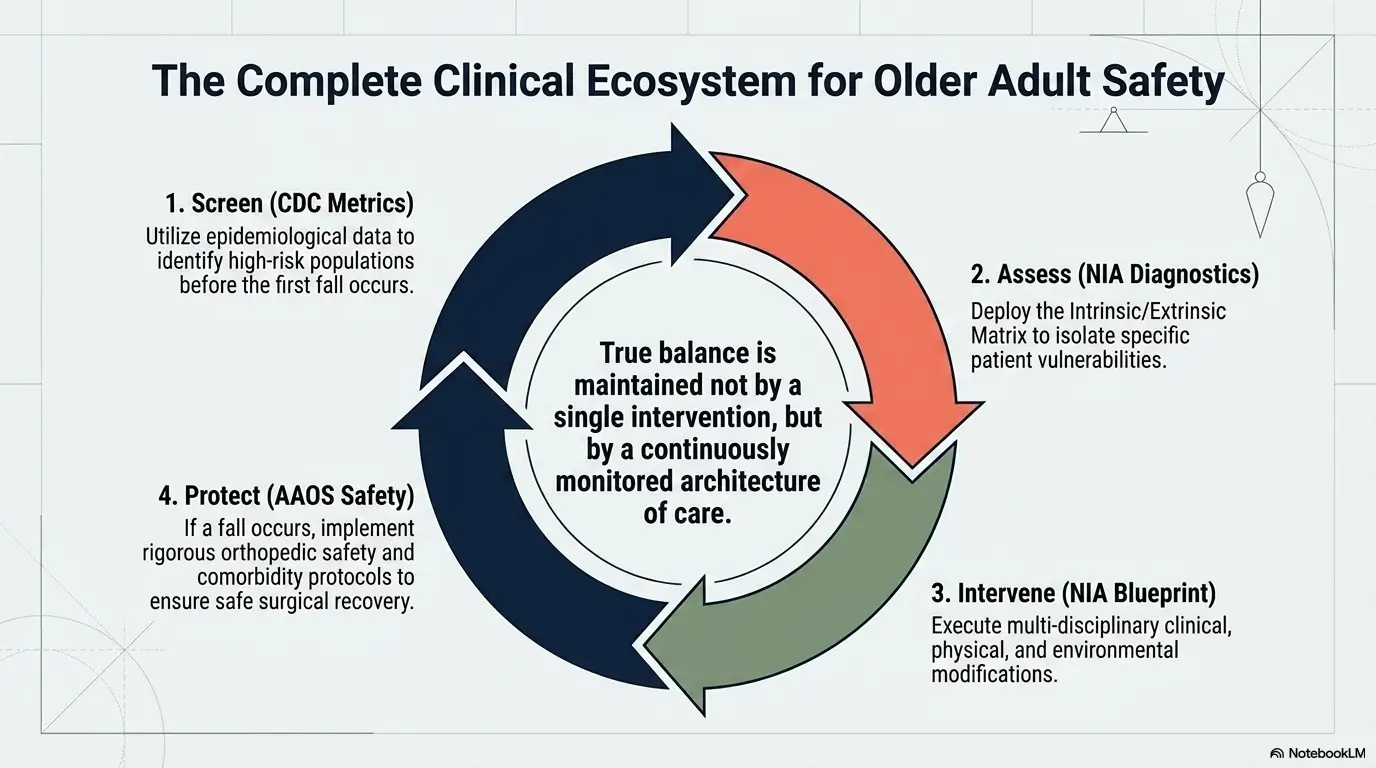
Next Step: Build a One-Page Pain-and-Safety Plan Today
Write Down the Current Pain Pattern
Start with one sheet of paper. Write the pain location, usual pain level, worst time of day, what helps, what worsens it, and whether there was a recent fall, injury, surgery, or medication change.
This does not need to be elegant. It needs to be findable. Tape it inside a cabinet, keep it by the phone, or place it in the folder used for medical visits.
List the Three Riskiest Daily Moments
Choose three moments where pain and safety collide. Common examples include getting out of bed, walking to the bathroom at night, showering, carrying meals, using stairs, doing laundry, or standing at the sink. If showering has become one of the riskiest moments after surgery, a focused guide to showering after hip surgery can make the bathroom part of the safety plan instead of an afterthought.
For each moment, write one fix. Not seven. One. The brain is more likely to use a small plan than admire a large one from a safe distance.
Choose One Room Fix, One Medication Question, and One Check-In Person
The one-page plan should include:
- One room fix: remove a rug, add a night light, move supplies lower, clear the path.
- One medication question: ask about dizziness, overlap, timing, constipation, or over-the-counter pain relievers.
- One check-in person: family member, neighbor, friend, caregiver, or building contact.
This is the loop from the opening: pain made the house feel too large. A plan makes the house smaller again, in the best way. Shorter reaches. Clearer paths. Better questions. Fewer risky gaps.
Keep the Plan Where It Will Be Used, Not Where It Looks Neat
A perfect plan in a drawer is home decor. Put the plan near the phone, medication area, or main chair. If family calls, use the plan as the shared script. If a doctor visit is coming, bring it along.
Coverage Tier Map: From Basic Tracking to More Support
| Tier | Support Level | What Changes |
|---|---|---|
| 1 | Self-tracking | Pain, function, sleep, and medication notes |
| 2 | Family check-ins | Daily function questions and backup contact |
| 3 | Pharmacist review | Medication overlap and side-effect screening |
| 4 | Therapy or home safety help | Movement, transfer, equipment, and room setup support |
| 5 | Urgent medical response | Used for red flags, major injury, or unsafe sudden changes |
Neutral action line: Pick the lowest tier that fits today, then move up quickly if function keeps shrinking.
Final 15-minute action: write the one-page plan now. List the pain pattern, the three riskiest moments, one room fix, one medication question, and one check-in person. That small page is not a cure. It is a handrail made of decisions.
Last reviewed: 2026-04.
