
Solve the Movement,
Not the Shopping Cart.
The most expensive mistake families make is often the first one: buying the reassuring device before identifying the painful movement it is supposed to fix.
Orthopedic pain management fails when the real problem hides in ordinary moments: standing from a low bed, reaching the toilet at night, or asking an exhausted caregiver to lift “just this once.”
Guessing costs more than money. The wrong equipment crowds the room and increases fall risks. This guide helps you compare walkers, shower chairs, and home modifications by one practical standard: Which item removes the most repeated pain and caregiver strain in your real home?
Watch the task. Measure the space. Match the body.
Look for the daily pain tax—then choose the tool that actually pays it down.
Table of Contents
Orthopedic pain management for families comparing home care equipment should start with the hardest daily movement, not the biggest product list. The best choices usually reduce pain during repeated tasks: standing from bed, using the toilet, showering, walking safely, reaching essentials, and resting between activity. Prioritize clinician-approved fit, fall prevention, bathroom safety, and caregiver strain before buying bulky equipment.
Safety / Disclaimer: Equipment Helps Only When It Matches the Person
This Guide Is Educational, Not Personal Medical Advice
Home care equipment can be wonderfully practical. It can also be a shiny little trap if it is chosen without the person’s diagnosis, surgery instructions, weight-bearing status, balance, strength, medication side effects, and home layout in mind.
This article is educational. It is not a substitute for advice from a physician, orthopedic surgeon, physical therapist, occupational therapist, pharmacist, home health clinician, or discharge planner. If someone is recovering from hip surgery, knee replacement, fracture care, spine pain, arthritis flare-ups, or a new mobility change, the safest equipment choice is usually the one that matches the care plan already in motion.
Ask the Clinician Before Changing Walking Aids, Transfers, or Weight-Bearing
A family can buy a walker in 12 minutes. A body, sadly, does not read the product description. After many orthopedic injuries and procedures, small details matter: how much weight the person can put on a leg, whether bending is limited, whether twisting is risky, and whether stairs are allowed.
I have watched families bring home equipment with the same hopeful energy people bring to assembling patio furniture. Then the first transfer happens, and everyone realizes the problem was not “lack of equipment.” The problem was that the person needed a clear movement plan.
Why “Looks Helpful” Is Not the Same as “Safe for This Body”
A bed rail may look stabilizing, but it may be wrong for someone who pulls hard, gets confused at night, or risks entrapment. A rollator may look liberating, but it may be unsafe for someone who cannot control brakes, tight turns, or uneven thresholds. A raised toilet seat may reduce knee strain, but if it is too high, feet may not plant firmly.
Equipment is not magic. It is architecture for movement. If the architecture is wrong, the body pays rent in pain.
When Equipment Should Be Fitted by a PT, OT, or Orthopedic Team
Professional fitting is especially important for walkers, canes, crutches, braces, transfer devices, bed rails, and anything used after surgery. A physical therapist often focuses on gait, strength, and safe movement. An occupational therapist often focuses on daily tasks: bathing, dressing, toileting, bed setup, kitchen routines, and energy conservation.
- Do not change walking aids without guidance after surgery or injury.
- Check fit, height, grip, brakes, and room layout before relying on equipment.
- When transfers feel uncertain, ask for PT or OT input before buying more gear.
Apply in 60 seconds: Write down the one movement that feels most unsafe, then ask the care team what equipment is appropriate for that exact task.
Start Here: Buy for the Hardest Repeated Movement
The Best Equipment Solves a Daily Pain Moment, Not a Shopping Category
Most families start with categories: walker, cane, shower chair, grab bar, bed rail, commode, cushion, reacher. That is understandable. Shopping sites are organized by product, not by the miserable little moment when a person stands up from the toilet at 2:13 a.m. and whispers a word the grandchildren should not hear.
A better starting point is the daily pain moment. Ask: where does pain spike, balance wobble, or help become necessary? The answer may be bed height, toilet height, shower entry, chair arms, a cluttered path, or the distance between the couch and the bathroom.
Track the Pain Spike: Bed, Bathroom, Chair, Kitchen, or Car?
Use a simple 24-hour scan. Do not make it dramatic. Just observe.
- Morning: Is getting out of bed the first pain spike?
- Bathroom: Is toileting or showering the riskiest task?
- Chair: Is standing up harder after sitting 30 minutes?
- Kitchen: Does reaching, bending, or carrying trigger pain?
- Car: Is getting in and out the weekly battle?
One family I spoke with wanted a wheelchair because their father “couldn’t get around.” The bigger problem was narrower: he could not stand comfortably from a low recliner. A firmer chair with arms and better seat height changed more than the wheelchair would have. The wheelchair was a thundercloud. The chair was the weather report.
The “Three Times a Day” Rule for Prioritizing Gear
If a painful task happens at least three times a day, it deserves priority over a dramatic task that happens once a week. Toileting, bed transfers, chair transfers, medication access, and walking to the bathroom often beat car transfer gadgets or rare outing equipment.
This is not glamorous. No one writes poetry about toilet height. But the home is built out of repeated moments, and repeated pain becomes a tax on independence.
Tiny Friction, Big Consequences
A rug edge, a cord, a low chair, a faraway lamp, a slippery bathroom floor, or a nightstand placed 8 inches too far away can turn normal movement into a negotiation. Families often underestimate tiny friction because it looks harmless from a healthy body.
Practical rule: if the person says “I can manage,” watch the actual movement once. Not to police them. To see what the room is asking their body to do.
Show me the nerdy details
A useful method is task-frequency mapping. List the day’s repeated movements, then score each one by frequency, pain intensity, fall risk, and caregiver involvement. Equipment that improves a high-frequency task usually creates more real benefit than equipment saved for rare worst-case scenarios.
Authoritative Resources for Safer Home Equipment Decisions
-
CDC: About Older Adult Fall Prevention
Useful for supporting claims about fall risk, independence, and practical fall-prevention steps for older adults. -
MedlinePlus: Getting Your Home Ready After Knee or Hip Surgery
Helpful for bathroom safety, grab bars, raised toilet seats, reachers, walkers, and home preparation after orthopedic surgery. -
AAOS OrthoInfo: How to Use Crutches, Canes, and Walkers
Best matched to the article’s walker, cane, rollator, stair-safety, and mobility-aid fitting sections.
Who This Is For, and Who This Is Not For
This Is For Families Comparing Walkers, Shower Chairs, Grab Bars, Bed Rails, and Raised Toilet Seats
This guide is for the family standing between a discharge packet, a half-open shopping tab, and a hallway that suddenly looks narrower than it did last week. It is for spouses, adult children, siblings, neighbors, and practical friends who want to help without accidentally turning the home into a medical equipment showroom.
It is especially useful when the person has orthopedic pain from arthritis, joint replacement recovery, hip or knee pain, back pain, fracture recovery, tendon issues, or general mobility decline. The common thread is not the diagnosis. The common thread is this: movement hurts, and the home now has to work smarter.
This Is For Adult Children Trying to Help Without Turning the Home Into a Supply Closet
Adult children often buy from love, urgency, and guilt. That combination can produce a garage full of equipment and still leave the bathroom unsafe. The goal is not to buy everything. The goal is to buy or borrow the few things that reduce daily pain, reduce fall risk, and reduce caregiver strain.
I say this gently because many families are doing their best while exhausted. Panic-shopping is still shopping. It deserves a pause.
This Is Not for Choosing Equipment After a Fall, New Weakness, or Sudden Severe Pain
If someone has fallen, nearly fallen, suddenly cannot bear weight, develops new weakness, has new numbness, has severe swelling, seems confused, has fever after surgery, or has chest pain or shortness of breath, do not treat equipment as the fix. That is a medical situation first.
A new device can hide a new problem for a few days. That delay can matter.
This Is Not a Replacement for Post-Surgery Discharge Instructions
After orthopedic surgery, discharge instructions may include movement restrictions, wound care guidance, medication timing, signs of complications, and specific equipment recommendations. Those instructions outrank general advice online, including this article.
When in doubt, bring the product question back to the care team: “Is this safe for her current restrictions?” That sentence is short, boring, and powerful. A good safety sentence often is.
- Yes: Pain is stable, instructions are clear, and the task is routine.
- Yes: You are comparing low-risk supports such as reachers, shower seating, or pathway changes.
- No: There is a recent fall, sudden weakness, new confusion, or unclear weight-bearing status.
- No: The person needs lifting, pulling, or hands-on transfers that feel unsafe.
Neutral next step: If any “No” applies, call the clinician, discharge team, PT, or OT before buying another device.
The Equipment Decision Card: Pain Relief vs. Safety vs. Caregiver Load
Pain Relief Gear Helps the Person Move With Less Strain
Pain relief equipment reduces the strain of a specific movement. A raised toilet seat may reduce knee and hip flexion. A shower chair may reduce the demand of standing through a shower. A reacher may reduce bending. A firmer chair with arms may make standing less punishing.
This category is about repeated effort. It answers the question: “Does this make the painful movement less costly?” For families comparing equipment for an older adult, it can also help to think through elderly orthopedic pain management as a daily-function problem, not only a pain-score problem.
Safety Gear Reduces Risk During Transfers and Wet-Surface Moments
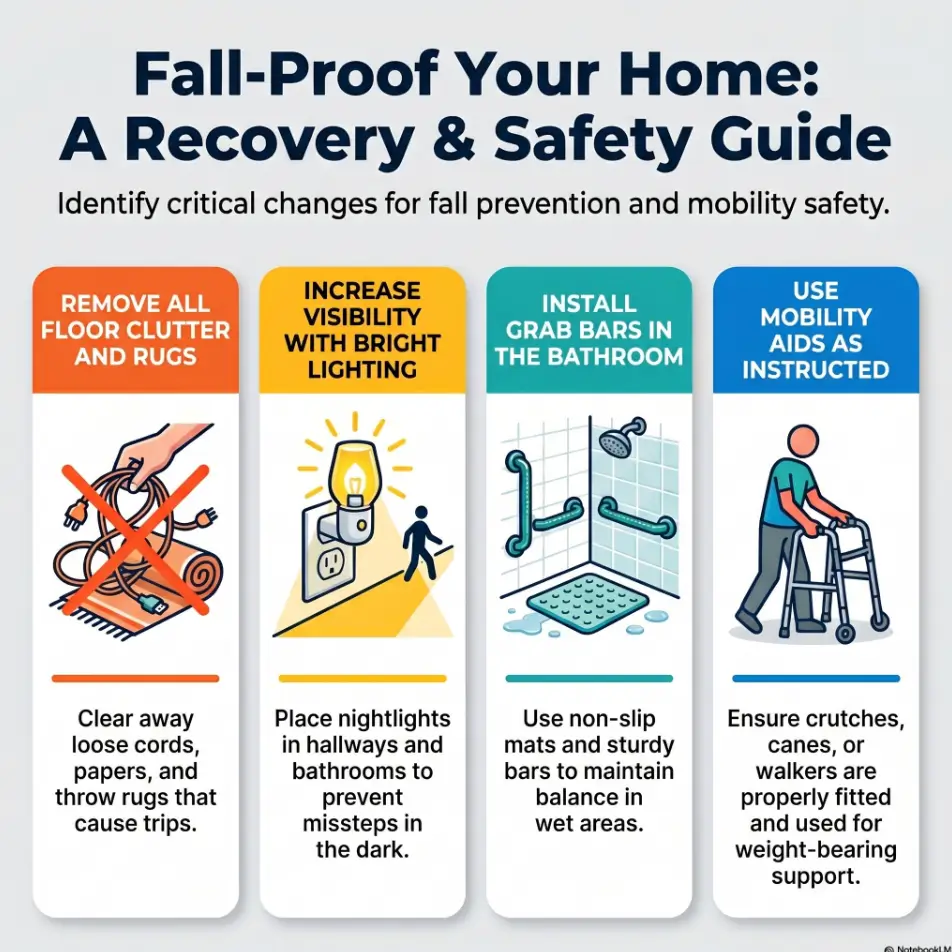
Safety equipment reduces the chance of slipping, tipping, grabbing the wrong thing, or losing balance during transitions. Grab bars, nonslip surfaces, stable seating, proper lighting, clear pathways, and correctly fitted mobility aids belong here.
Falls are a major concern for older adults. The CDC emphasizes that falls can threaten independence, but many fall risks can be reduced with practical prevention steps. In real homes, that often begins with wet floors, nighttime bathroom trips, loose rugs, poor lighting, and rushed transfers.
Caregiver-Load Gear Protects the Helper’s Back, Timing, and Patience
Caregiver-load gear reduces the physical and mental strain on the helper. This matters more than families admit. If one spouse must twist, lift, brace, and hurry twice a day, the home setup is borrowing from that caregiver’s spine.
Good equipment should reduce force. Bad equipment adds steps, confusion, and theatrical sighing.
The Hidden Winner Is Often the Item Used Ten Times a Day
A simple chair placed in the right location may do more than an expensive device used once. A lamp within reach may prevent risky twisting. A basket near the favorite seat may reduce 10 unnecessary trips. The humble item wins because frequency compounds.
Decision Card: What Problem Is This Equipment Solving?
Choose when the same movement hurts every day.
Examples: raised toilet seat, shower chair, reacher, chair with arms.
Choose when balance, wet floors, stairs, or night trips create risk.
Examples: grab bars, lighting, nonslip surfaces, fitted walker.
Choose when the helper must lift, pull, rush, or repeat instructions.
Examples: transfer training, better bed height, commode placement, OT plan.
Neutral action: Label each possible purchase with one main job before comparing prices.

Bathroom First: The Room Where Pain and Fall Risk Collide
Shower Chairs Help When Standing Through a Shower Burns Through Energy
The bathroom deserves first attention because it combines pain, water, privacy, urgency, hard surfaces, and awkward movement. It is not just a bathroom. For someone with orthopedic pain, it is a transfer room with plumbing.
A shower chair can help when standing through a shower drains energy or increases pain. It may also reduce the frantic little dance of balancing while washing feet, reaching soap, or turning toward a towel. Choose a stable chair designed for wet areas, not a random household stool auditioning for danger. For hip-related recovery routines, showering after hip surgery often needs the same route-based thinking: entry, sitting, washing, towel reach, and exit.
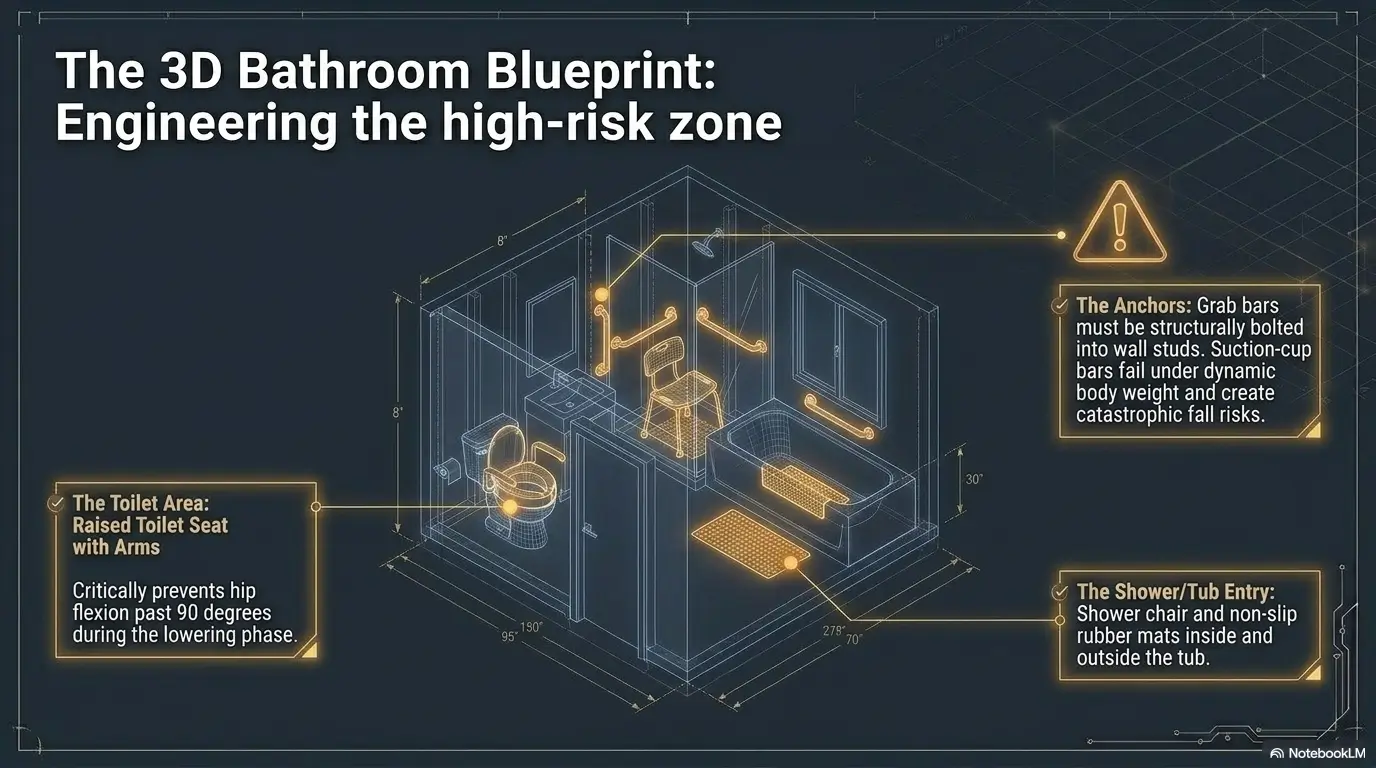
Grab Bars Are Not Decoration; Placement Decides Whether They Work
Grab bars work only when they are where the hand naturally needs support. Placement matters near the toilet, shower entry, and standing area. They should be installed into appropriate structure or according to professional guidance. Adhesive “suction” handles can look convincing, but families should be cautious about relying on them for weight-bearing support.
MedlinePlus describes practical home preparation after hip or knee surgery, including items such as grab bars, raised toilet seats, reachers, walkers, and long-handled tools. That list matters because recovery pain often shows up during ordinary bathroom and dressing tasks, not only during formal exercise.
Raised Toilet Seats Can Reduce Sit-to-Stand Pain, but Height Matters
A raised toilet seat can reduce the bend required at the knees and hips. But height matters. Too low may not help. Too high can leave feet poorly planted, which creates a different safety problem wearing a fake mustache.
Look for stable fit, secure installation, arm support when appropriate, and enough space for safe turning. If the bathroom is narrow, measure before buying. “It should fit” is not a measurement. It is a tiny prayer with a receipt attached.
Do Not Trust Towel Bars, Sliding Doors, or “I’ll Be Careful”
Towel bars are not grab bars. Sliding shower doors are not balance tools. “I’ll be careful” is not a fall-prevention plan. Families often know these things in theory, then ignore them during the Tuesday morning scramble.
Bathrooms punish improvisation. A safe setup should make the correct movement easy and the risky movement unnecessary.
Here’s What No One Tells You: The Bathroom Is a Transfer Room
Think in transfers: sit to stand from the toilet, step into the shower, sit onto the shower chair, stand to towel off, turn to exit, walk to the bedroom. Each transfer is a chance to reduce pain or invite chaos.
- Map toilet, shower entry, standing zone, and towel reach.
- Use real grab bars, not towel bars or sliding doors.
- Measure height and space before buying raised toilet seats or shower chairs.
Apply in 60 seconds: Stand in the bathroom doorway and name the riskiest transfer before adding anything to the cart.
Walker, Cane, or Rollator: Do Not Choose by Vibe
A Walker May Add Stability, but It Must Fit the Person and the Space
Walkers can provide support, but they are not interchangeable metal rectangles. Height, grip, wheels, tips, posture, turning ability, doorway width, flooring, and the person’s strength all matter.
The American Academy of Orthopaedic Surgeons explains safe use of crutches, canes, and walkers, including important cautions about standing, stairs, and proper technique. Their guidance is a useful reminder that a mobility aid is not just purchased. It is learned.
A Cane Can Help Mild Support Needs, but It Is Not a Mini-Walker
A cane can help with mild support and balance needs when recommended and fitted correctly. But a cane is not a walker that went on a diet. It provides less support and requires coordination.
If a person is leaning heavily, dragging a leg, grabbing walls, or using furniture as a secret second cane, the family should not quietly upgrade the cane and hope the problem behaves.
A Rollator Seat Sounds Convenient Until Brakes, Turns, and Doorways Matter
Rollators are appealing because they often include wheels, hand brakes, and a seat. For some people, they are helpful. For others, they move too easily, require too much brake control, or become awkward in small rooms. For people whose walking distance changes because of back or leg symptoms, a rollator for lumbar spinal stenosis is worth thinking about through fit, brake control, rest timing, and clinician guidance rather than convenience alone.
The seat can be useful for rest breaks, but it can also encourage risky parking, turning, or sitting in a poor location. A rollator should fit the person’s balance, judgment, grip strength, and home layout.
Don’t Do This: Buying the Cheapest Mobility Aid Without Measuring
Cheap is not always bad. Unfitted is the problem. Measure doorways, look at flooring, check the person’s height, and ask whether the aid works in the bathroom, bedroom, and kitchen route. A walker that only works in the living room is less a solution and more a hallway sculpture.
The Stairs Problem Families Forget Until Tuesday Morning
Stairs change everything. Some mobility aids should not be used on stairs or escalators. If the home has stairs, steps into the garage, uneven thresholds, or a sunken living room, ask the clinician or physical therapist for a specific stair plan.
Use these three inputs before comparing walker, cane, or rollator options.
- Doorway width: Can the aid pass through without twisting?
- Bathroom turn space: Can the person turn safely near the toilet or shower?
- Rest distance: How far can the person walk before pain or fatigue changes posture?
Output: If any answer is uncertain, pause the purchase and ask for fitting guidance.
Neutral action: Measure the narrowest doorway and the bathroom turning area before comparing models.
Bed Setup: The Morning Pain Spike Starts Before Breakfast
Bed Height Can Make Standing Easier or Turn Every Morning Into a Lift
Morning pain often begins before breakfast, before coffee, before anyone has the emotional resources to be heroic. Bed height can decide whether getting up is a controlled movement or a small wrestling match with gravity.
A bed that is too low may require painful knee, hip, or back effort. A bed that is too high may make sitting unstable or prevent feet from planting. The ideal height depends on body size, strength, restrictions, and transfer ability. This is where an OT’s eye can be worth more than 40 product reviews.
Bed Rails Need Careful Judgment, Not Automatic Approval
Bed rails can help some people reposition or feel supported. They can also create risk if used incorrectly, installed poorly, or relied on by someone who pulls hard, becomes confused, or tries to climb over them.
Families sometimes treat bed rails as gentle equipment because they look quiet. But quiet equipment can still be serious. Ask for guidance if there is confusion, nighttime wandering, significant weakness, or a history of falls from bed.
Nightstand Placement Can Reduce Twisting, Reaching, and “One More Step”
The nightstand is a tiny command center. It should reduce reaching, twisting, and unnecessary standing. Put the phone, water, glasses, medication plan, tissues, light switch, and call device where the person can reach them without a dramatic shoulder expedition.
One caregiver told me her mother kept getting up to turn on a lamp across the room. The family had already bought a walker, a shower chair, and two cushions. The best fix that week was a bedside lamp with an easy switch. Sometimes the hero wears a lampshade.
The Best Bedside System Has a Home for Phone, Water, Glasses, Meds, and Light
A good bedside system is predictable by feel. It does not require searching. It does not bury medication under magazines. It does not send the phone charging cable across the walking path like a tiny tripwire with excellent branding.
- Keep essentials on the stronger or easier-reaching side when appropriate.
- Use a stable water bottle or lidded cup if spills are common.
- Keep medication instructions visible but avoid loose pill chaos.
- Route cords away from feet and mobility aids.
- Use lighting that can be turned on before standing.
- Check whether feet plant firmly before standing.
- Do not assume bed rails are automatically safe.
- Put light, phone, water, glasses, and instructions within easy reach.
Apply in 60 seconds: Sit on the bed and reach for each essential without standing, twisting, or leaning hard.
Kitchen and Living Room Gear: Stop Buying for the Room, Start Buying for the Route
Reachers Help When Bending Hurts, but They Should Not Encourage Risky Overreach
Reachers are useful for light objects, dropped items, and reducing bending. They are not permission to pull heavy pans from the back of a cabinet or rescue a laundry basket from the floor like a crane operator with hip pain.
Move high-use items to waist-to-chest height. Put heavy items where they can be reached with both feet planted. A reacher should reduce risk, not turn the kitchen into a carnival game.
Chair Height Matters More Than Cushion Softness
In the living room, families often focus on comfort. But for orthopedic pain, getting out of the chair may matter more than sinking into it. A soft, low recliner can feel wonderful for 20 minutes and then demand a small rescue operation.
Look for a stable chair with arms, appropriate seat height, firm support, and enough space for the person to position a mobility aid. A cushion that raises height may help in some cases, but it should not slide, wobble, or change posture in an unsafe way.
Clear Pathways Beat Extra Gadgets
Before buying more gear, remove pathway hazards. Scatter rugs, cords, clutter, pet bowls, low tables, unstable ottomans, and poor lighting can sabotage even good equipment.
AAOS home-safety guidance has long emphasized common fall hazards such as throw rugs, cords, slippery surfaces, and clutter. The boring fixes matter because the home does not care how many devices you bought. It cares where the foot lands next.
The One-Trip Trap
Orthopedic pain makes people bargain with themselves. “I’ll carry everything in one trip.” That sentence has launched many bad ideas. Carrying too much can change balance, block the view of the floor, and make a walker or cane harder to use safely.
Use a small basket, rolling cart if appropriate, caregiver staging, or fewer trips planned with rest breaks. Independence should not require a juggling act.
Don’t Do This: Leaving Cords, Rugs, and Clutter Because “They Know the House”
Familiarity is not immunity. People trip in homes they know by heart. Pain medication, fatigue, nighttime bathroom trips, swelling, and distraction can make a familiar pathway behave differently.
Infographic: The 5-Stop Home Equipment Route
Can feet plant and hands push safely?
Are toilet, shower, and towel transfers supported?
Can the person stand without pulling on furniture?
Are essentials reachable without bending or carrying too much?
Are rugs, cords, clutter, and dark spots removed?
Use: Walk this route once before spending money. The weak link usually reveals itself quickly.
Common Mistakes: Where Well-Meaning Families Waste Money
Mistake 1: Buying a Wheelchair Before Fixing the Transfer Problem
A wheelchair may be necessary in some situations, especially with clinician guidance. But many families reach for it before solving the transfer problem: standing from bed, rising from the toilet, getting into the shower, or moving safely from chair to walker.
If the person cannot transfer safely, a wheelchair alone does not solve the hardest part. It may simply move the difficulty to a different location.
Mistake 2: Choosing Equipment for the Worst Imagined Day Only
Fear is a persuasive salesperson. Families imagine the worst day and buy for that day. But if the worst day is rare and the daily problem remains unfixed, the home becomes crowded without becoming safer.
Buy first for the repeated task. Plan separately for flare-ups, bad weather, post-appointment fatigue, and surgery recovery milestones.
Mistake 3: Assuming More Equipment Means More Independence
More equipment can sometimes reduce independence if it blocks paths, confuses routines, or makes the home feel like a storage unit with throw pillows. The question is not “Do we have enough?” It is “Does each item have a clear job?”
Mistake 4: Ignoring Door Width, Floor Transitions, and Bathroom Layout
A mobility aid that does not fit through the bathroom door is not a mobility aid in the moment when it is most needed. Measure narrow doorways, thresholds, rugs, bed-to-bath route, and turning space.
Families often measure the product. They forget to measure the house. The house always has opinions.
Mistake 5: Forgetting the Caregiver’s Body Is Part of the System
The helper is not an infinite resource. If equipment only works when a spouse lifts, twists, and whispers “one, two, three” with terror in their elbows, the system is fragile.
- Diagnosis or procedure type and current restrictions.
- Height and approximate weight of the person using the equipment.
- Doorway widths, toilet height, bed height, and shower entry style.
- Photos of the bathroom, bedroom route, and favorite chair area.
- Insurance, Medicare Advantage, Medicaid, HSA, FSA, or supplier requirements when relevant.
Neutral action: Gather the measurements and photos before calling a supplier or ordering online.
The Caregiver Strain Test: Can the Helper Do This Twice a Day?
If One Person Must Lift, Twist, and Rush, the Setup Is Already Failing
A home setup is not safe just because the person in pain can survive it once. Ask whether the caregiver can help with the same task twice a day, every day, without rushing, pulling, twisting, or risking injury.
Caregiver strain often hides behind devotion. People say, “It’s fine, I can do it,” while their lower back quietly files a complaint.
Transfer Aids Should Reduce Force, Not Add Confusion
Some transfer aids can help when chosen and taught properly. But a tool that nobody understands under stress is not helpful. The best transfer plan is clear, repeatable, and realistic at 6 a.m., not only during a calm demonstration.
If the person needs significant physical assistance to stand, pivot, or sit, ask for professional transfer training. A PT or OT can often identify whether the issue is height, hand placement, weakness, pain timing, fear, or poor room setup. When therapy seems stalled or the home movement problem is not translating into progress, it may help to ask more precise questions about physical therapy not helping orthopedic pain before simply buying another device.
The Safest Equipment Is the One Both People Understand Under Stress
Stress changes movement. Pain spikes, bathroom urgency, medication timing, and fatigue can make even simple tasks feel complicated. Equipment should reduce the number of decisions, not add a puzzle.
- Can both people explain the transfer steps?
- Can the person use the device without rushing?
- Can the caregiver help without lifting?
- Is there enough room for feet, hands, and the device?
- What is the backup plan if pain is worse today?
Let’s Be Honest: Love Is Not a Lifting Technique
Love matters. It gets people to appointments, folds the laundry, makes soup, and remembers which pharmacy has the less chaotic parking lot. But love does not protect a caregiver’s back during a bad transfer.
A safer setup respects both bodies. The person with pain deserves dignity. The helper deserves a plan that does not turn devotion into injury.
Short Story: The Shower Chair That Was Not the Real Fix
Short Story: A daughter bought her father a shower chair after knee surgery because showering exhausted him. Good instinct. But when she watched the routine, the chair was only half the story. He still had to step over a tub edge, reach across the bathroom for a towel, and twist toward a shelf for shampoo.
The chair helped him sit, but the room still made him gamble. They moved toiletries to waist height, placed towels within easy reach, added clinician-approved support, and changed the timing so he showered after pain medication was working as directed. The chair mattered. The route mattered more. That is the quiet lesson of home equipment: the product is only one instrument. The room is the orchestra.
When to Seek Help: Red Flags Before You Buy Another Device
Seek Medical Help for New Weakness, Numbness, Severe Swelling, Chest Pain, Fever, or Sudden Loss of Function
Some signs should not be handled with shopping. New weakness, new numbness, sudden inability to walk, severe swelling, chest pain, shortness of breath, fever after surgery, signs of infection, sudden confusion, or a major change in pain needs medical advice promptly.
Equipment can support recovery. It should not be used to explain away a new symptom.
Call the Clinician After a Fall, Near-Fall, Medication Confusion, or Worsening Pain
Falls and near-falls count. So does new medication confusion, missed doses, double doses, dizziness, or worsening pain that changes function. These issues can affect walking, balance, judgment, and safety.
Families sometimes minimize near-falls because “they caught themselves.” That is useful information, not a reason to shrug. A near-fall is the body tapping the microphone.
Ask for PT or OT Help When Transfers Require Pulling, Lifting, or Guesswork
If standing from bed, sitting on the toilet, entering the shower, getting into the car, or walking across the room requires pulling, lifting, or improvisation, it is time to ask for help. PT and OT guidance can turn a messy movement into a repeatable method.
Get Urgent Advice If Equipment Changes Make Walking Less Safe
If a new walker, cane, rollator, brace, shoe, insert, or chair setup makes walking less safe, stop and ask for guidance. Do not force the person to “get used to it” when the device increases risk. If the question is whether symptoms need faster evaluation, the distinction between urgent care vs orthopedic clinic can help families avoid treating a medical change like a shopping problem.
- Do not use equipment to compensate for sudden weakness or new numbness.
- Report falls, near-falls, confusion, and worsening function.
- Ask for PT or OT help when transfers require lifting or guessing.
Apply in 60 seconds: Write “new, sudden, worse, or unsafe?” on a note near the equipment list.
The Family Comparison Framework: Rank Equipment by “Pain Removed per Dollar”
Score Each Item by Frequency, Pain Intensity, Risk, and Space Fit
To compare equipment without drowning in tabs, use a simple score. You do not need an MBA. You need a pen, a tape measure, and enough honesty to admit the bathroom is the villain.
| Factor | Ask This | Score |
|---|---|---|
| Frequency | How many times per day does this task happen? | 1 to 5 |
| Pain intensity | How much does this movement hurt? | 1 to 5 |
| Risk | Could a slip, fall, or failed transfer happen here? | 1 to 5 |
| Space fit | Will it fit the real room, not the product photo? | 1 to 5 |
| Caregiver load | Will it reduce lifting, rushing, or repeated help? | 1 to 5 |
High scores deserve attention first. Low-frequency, low-risk gadgets can wait, no matter how persuasive their product photos look.
Put Bathroom and Bed Transfers Above Rare “Just in Case” Gear
Bathroom and bed transfers often deserve priority because they happen daily and affect dignity. They also happen when people are tired, undressed, medicated, or half-awake. That combination is not a small detail. It is the whole plot.
Compare Rental, Borrowing, Insurance Coverage, and Short-Term Recovery Needs
Not every item needs to be owned forever. Some equipment is useful for a few weeks after surgery. Some may be covered through insurance or a durable medical equipment supplier when prescribed. Some may be borrowed safely if clean, intact, appropriate, and fitted.
For U.S. families, Medicare, Medicare Advantage plans, Medicaid programs, private insurers, HSA or FSA rules, hospital discharge teams, and local durable medical equipment suppliers may all affect cost and access. The details vary, so verify before assuming. For braces, supports, and related purchases, families may also want to check whether HSA eligible braces and supports apply to their specific situation before counting on reimbursement.
The Best Purchase May Be the One You Use for Three Weeks, Not Three Years
Short-term usefulness is not failure. If a raised toilet seat helps during early knee recovery and then leaves the house after 6 weeks, that may be a successful purchase. The best tool is not always permanent. Sometimes it is a temporary bridge over a painful little river.
- Tier 1: Low-cost household changes, such as moving items and clearing paths.
- Tier 2: Basic aids, such as reachers, shower chairs, and nonslip items.
- Tier 3: Fitted mobility aids, such as walkers, canes, or crutches.
- Tier 4: Installed supports, such as grab bars or modified bathroom features.
- Tier 5: Higher-cost or prescribed equipment, such as wheelchairs or complex transfer solutions.
Neutral action: Ask the clinician or supplier whether the item requires a prescription, fitting, installation, or coverage paperwork.
FAQ
What Home Care Equipment Helps Most With Orthopedic Pain at Home?
The most helpful equipment is usually the item that improves the hardest repeated movement. For many families, that means bathroom supports, safer bed setup, a properly fitted walking aid, a stable shower chair, a raised toilet seat, reachers, better chair height, and clear pathways. The best choice depends on the person’s diagnosis, restrictions, strength, balance, pain pattern, and home layout. A broader orthopedic pain management for older adults plan can help families connect equipment choices to function, sleep, medication timing, and fall risk.
Should We Buy a Walker Before the Doctor Recommends One?
Be careful. A walker can help some people, but it should fit the person and the task. After surgery, injury, or new weakness, ask the clinician, PT, or OT before changing mobility aids. The wrong aid can change posture, increase fall risk, or create unsafe habits.
Is a Shower Chair Worth It for Knee, Hip, or Back Pain?
A shower chair may be worth it when standing through a shower increases pain, fatigue, or balance risk. It should be stable, appropriate for wet use, and fit the shower or tub area. Also check towel reach, soap placement, shower entry, and grab bar needs. The chair helps most when the whole shower routine is safer.
Are Grab Bars Better Than a Raised Toilet Seat?
They solve different problems. Grab bars provide hand support during transfers. A raised toilet seat reduces how far the person must lower and rise. Some people need both. Placement, installation, height, and the person’s movement pattern matter more than choosing one category in isolation.
What Equipment Helps an Older Adult Stand Up From a Chair?
A stable chair with arms, appropriate seat height, firm support, and enough room for foot placement often helps more than a soft cushion. Some people may need clinician-approved transfer training or additional devices. Avoid unstable cushions or furniture that slides, rocks, or encourages pulling.
Should Families Rent or Buy Orthopedic Recovery Equipment?
Renting can make sense for short-term recovery or expensive items needed for only a few weeks. Buying may make sense for ongoing needs, daily-use items, or equipment that must be customized. Compare cost, hygiene, fit, coverage, return policy, and expected recovery timeline.
What Equipment Reduces Caregiver Strain During Transfers?
The best strain reducers are often proper transfer training, correct bed or chair height, stable grab points, enough room to move, and equipment that reduces lifting. If a caregiver must pull, twist, or lift repeatedly, ask for PT or OT guidance. Love should not have to function as a back brace.
How Do We Know If the Home Has Too Much Equipment?
The home may have too much equipment if pathways are narrower, routines feel confusing, devices sit unused, or the person avoids rooms because the setup feels crowded. Each item should have a clear job. If nobody can explain when and how it is used, reconsider it.
Next Step: Do One Room Walkthrough Before Buying Anything
Start With the Most Painful Repeated Task
The loop we opened at the beginning was simple: families often buy the first reassuring item instead of the item that solves the daily pain moment. Now close that loop with one practical test. Pick one room. Watch one repeated task. Measure before you buy.
Do not inspect the whole house in one heroic sweep. That becomes a domestic audit, and nobody wants a clipboard haunting the hallway. Start with the room where pain and risk meet most often.
Measure the Doorways, Bed Height, Toilet Height, and Shower Entry
Measurements turn anxiety into useful information. Measure the narrowest doorway on the route, bed height, toilet height, shower or tub entry, chair seat height, and the distance between key supports. Take photos if you plan to ask a clinician, supplier, PT, OT, or discharge planner for advice.
Write Down Three Pain Moments and One Safety Concern
Use this quick list:
- Most painful repeated movement: ______
- Most unsafe transfer: ______
- Most cluttered or narrow route: ______
- One caregiver strain point: ______
This turns the shopping conversation from “What should we buy?” into “What problem are we solving?” That shift can save money, space, and several family debates conducted in the pharmacy aisle.
Bring That List to the Clinician, PT, OT, Pharmacist, or Discharge Planner
Equipment decisions improve when professionals see the actual problem. Bring your measurements, photos, medication concerns, pain timing, fall history, and daily routine notes. Ask specific questions: “Is this safe for his restrictions?” “What height should the walker be?” “Should we use a raised toilet seat or grab bars here?” “Do we need transfer training?”
- Start with one room, not the whole house.
- Measure before buying bulky equipment.
- Use clinician guidance for mobility aids, transfers, and post-surgery restrictions.
Apply in 60 seconds: Choose the one daily movement you most want to make safer, then write it at the top of your equipment list.
Orthopedic pain management at home is not about filling the house with devices. It is about designing fewer risky moments. The right equipment should make the day quieter: fewer grimaces, fewer near-falls, fewer awkward lifts, fewer “I’m fine” performances delivered through clenched teeth.
Within the next 15 minutes, do one small walkthrough: bed to bathroom, bathroom to chair, or chair to kitchen. Name the hardest movement. Measure the space. Write one safety concern. Then compare equipment from that grounded little map. The best home care choice is rarely the loudest product. It is the one that lets ordinary life move with less pain.
Last reviewed: 2026-04.
