
Beyond the Buzz: A Realistic Guide to TENS for Knee Pain
A TENS unit for knee pain can sometimes make the knee feel better for 20 or 30 minutes. That is exactly why it gets over-credited. Relief is easy to confuse with repair, especially when the pain has been hanging around long enough to make every new gadget look like a small rescue.
The real problem is not just pain. It is uncertainty. A stiff, overworked knee, an osteoarthritis flare, and an injury-style knee with swelling or instability do not make the same bargain with a home device, even if the product page treats them like identical roommates. Keep guessing, and you can lose time, money, rehab momentum, and sometimes the chance to catch a problem that should have been evaluated earlier.
This guide helps you use a TENS unit more intelligently for orthopedic pain management, with clearer expectations about knee osteoarthritis, pad placement, red flags, and the difference between a useful symptom-relief tool and a delay tactic with wires. The goal is not to make the device sound magical. It is to help you decide where it fits, where it fails, and what to do next.
The approach here is deliberately practical: evidence check first, pain pattern second, home-use mistakes third. Because this is where people usually get into trouble, not with the machine, but with the story they tell themselves after it buzzes.
So before you buy harder, dial higher, or mistake numbness for progress, start here.
Fast Answer: A TENS unit for knee pain may help some adults get short-term symptom relief, especially when the goal is to make walking, stretching, or basic rehab more tolerable. But it does not fix cartilage, ligaments, meniscus tears, or inflammatory causes of knee pain. For knee osteoarthritis, evidence is mixed, and a 2022 randomized trial found no meaningful advantage over placebo TENS. Use it as a tool, not a verdict.
Table of Contents
Start Here: What a TENS Unit Can and Cannot Do for Knee Pain
What “pain management” means here, not miracle repair
TENS stands for transcutaneous electrical nerve stimulation. In plain English, it sends electrical pulses through pads on the skin. The goal is to change how pain feels, at least for a while. The key word is feels. TENS does not glue a torn meniscus back together. It does not stabilize a loose kneecap. It does not calm a hot swollen joint into being harmless. It may reduce pain perception for a session, much like opening a window in a stuffy room. The room is better. The walls did not move.
Why symptom relief and problem-solving are not the same thing
This distinction is where many smart adults still get tripped. If the knee hurts less during or after TENS, that does not automatically mean the problem is minor. Pain can drop while the underlying issue remains mechanical, inflammatory, or load-related. In osteoarthritis, some people report temporary relief; in injury-style pain, relief can create false confidence and lead to the oldest plot twist in orthopedics: “It felt better, so I did too much.”
The hidden fork in the road: calming pain vs missing the diagnosis
A common home scene goes like this: the knee has been grumbling for weeks, stairs feel rude, a device promises drug-free relief, and the temptation is to make the device the whole plan. That is the wrong fork. The better fork is this: use TENS, if you use it at all, as a small tool inside a larger question. What pattern is this pain following? Is it overuse, arthritis-style, or injury-style? That question matters more than the gadget.
- Temporary relief is not the same as tissue healing
- Less pain does not prove the joint is stable
- Diagnosis still matters when symptoms are new, strange, or escalating
Apply in 60 seconds: Write one sentence that starts with “My knee pain behaves like…” before you ever stick on the pads.
Best Fit, Wrong Fit: Who This Is For and Not For
Best fit: flare-ups, overuse aches, arthritis-related discomfort, post-activity soreness
TENS tends to make the most sense when the pain pattern is familiar, non-emergent, and already somewhat understood. Think of the knee that aches after a long walk, protests after yard work, or stiffens with osteoarthritis and needs a nudge before exercise. These are the moments where symptom relief can be useful because it creates a short “window” for walking, gentle range-of-motion work, or physical therapy homework.
Not a smart first move: new injury, locking, buckling, major swelling, hot joint
Now the other side of the ledger. If your knee just twisted, popped, swelled up, locks, buckles, or feels hot and angry, TENS is not the first move. The American Academy of Orthopaedic Surgeons notes that knee injuries commonly present with pain and swelling, and that some injuries cause catching, locking, or a giving-way sensation. The NHS likewise flags severe swelling, inability to bear weight, locking, giving way, and redness with heat or fever as reasons for urgent assessment. Those are not “try a gadget first” signals.
Who should pause and ask a clinician before trying TENS
Adults with implanted devices, unusual numbness, fragile skin, unexplained swelling, or a knee pain story that keeps changing should slow down and read the labeling with more respect than most online reviews deserve. Consumer-facing device language and FDA-cleared labeling commonly include warnings about pacemakers, implanted defibrillators, and other implanted metallic or electronic devices. That is not fine print; that is the front door.
Eligibility checklist:
- Yes: The pain is familiar and not rapidly worsening
- Yes: There is no major new swelling, locking, or collapse
- Yes: You want temporary relief to help movement, not replace evaluation
- No: You have an implanted cardiac or electrical device unless your clinician has cleared it
- No: The knee is red, hot, feverish, or injured and unstable
Neutral next step: If you checked any “No,” pause the home experiment and get the knee assessed first.
Evidence Check: Why the Promise Sounds Bigger Than the Data
Why TENS remains popular even when results are mixed
The appeal is easy to understand. TENS is visible, immediate, and user-controlled. You can feel it working, which is not the same as it working well. Devices that create sensation often earn loyalty faster than slow, quiet interventions like strengthening, weight management, or movement retraining. Humans are consistent that way. If a knee whispers, we prefer the tool that buzzes back.
For knee osteoarthritis, the research story is not as clean as product pages suggest
The evidence for knee osteoarthritis has never read like a tidy sales page. An older Cochrane-style review found benefit over placebo in some studies, but also pointed to heterogeneity and the need for better-designed trials. A later randomized controlled trial published in 2022 reported that TENS did not improve knee osteoarthritis pain compared with placebo TENS. NICE now advises clinicians not to offer TENS for osteoarthritis because the evidence of benefit is insufficient. That does not mean nobody feels better using it. It means the average evidence picture is much wobblier than the packaging implies.
Relief may be real, but not always reliable
This is the part many readers deserve to hear without hype. A therapy can feel helpful to some people and still fail to show a dependable advantage over placebo in higher-quality trials. Knee pain is full of that drama. Expectation, context, and the relief of “doing something” all matter. In one study, subjective pain ratings during knee osteoarthritis improved similarly with active TENS and placebo TENS, suggesting a strong placebo component for some outcomes. That does not make the relief fake. It makes the interpretation more modest.
Show me the nerdy details
When TENS studies disagree, the problem is often not one single contradiction. It is a stew of small sample sizes, different stimulation settings, inconsistent pad placement, varied treatment schedules, and mixed outcome measures. That is why one review can sound encouraging while a later sham-controlled trial sounds deflating. The mechanism may help some people under some conditions, but the average effect for knee osteoarthritis has not been consistently robust in higher-quality placebo-controlled work.
Pain Pattern First: The Knee Problems That Change the Whole Decision
Arthritis-style pain vs workout-related pain vs injury pain
If you classify the pattern first, your decisions sharpen immediately. Arthritis-style pain is often stiff, irritable after inactivity, and aggravated by load over time. Workout-related pain tends to have a clearer trigger, like stairs, squats, a sudden mileage jump, or a comeback tour your knees did not agree to. Injury pain is different again. It often has a moment. A twist. A pop. A sharp swell. A limp. A story you can point to.
When stiffness points one way and instability points another
Stiffness alone nudges the differential one way. Instability nudges it another. A knee that feels rusty in the morning may be more compatible with osteoarthritis or patellofemoral irritation. A knee that suddenly gives way, catches, or locks is waving a more mechanical flag. That is why the same device can be a tolerable side tool for one person and a time-wasting detour for another.
Why “my knee just hurts” is rarely specific enough
“My knee just hurts” sounds simple, but it hides the useful clues. Where exactly? Front of the knee, inside, outside, behind the kneecap? With stairs, sitting, kneeling, twisting, or getting out of a chair? After 10 minutes or after 10,000 steps? The better your pattern description, the less likely you are to let a temporary pain-relief device drive the whole decision.
Decision card: When does TENS make sense?
- Bucket A: Overuse-style pain → reasonable short-term add-on while you modify load
- Bucket B: Arthritis-style pain → possible temporary relief, but keep expectations modest
- Bucket C: Injury-style pain → evaluate first if swelling, locking, buckling, or sharp instability is present
Neutral next step: Put your knee into a bucket before you spend money or time.
Infographic: The 3-bucket knee pain map
Overuse-style
Triggered by activity, load spike, stairs, squats, or repetitive motion.
Best question: What changed in training, routine, or workload?
Arthritis-style
Stiff, achy, often worse after sitting or with accumulated load.
Best question: What helps me move more consistently?
Injury-style
Pop, twist, rapid swelling, locking, buckling, or sudden loss of confidence.
Best question: Do I need evaluation before self-treatment?
Placement Changes Everything: How TENS for Knee Pain Often Fails at Setup
Pad placement confusion is where many home users lose the plot
Home TENS use often fails for very boring reasons. The pads are placed randomly. They are slapped directly on the most dramatic spot without considering the painful region. The user copies a generic online diagram that seems designed by a committee of elbows. Then the device gets blamed. Pad placement varies by device instructions and pain pattern, but one practical truth survives: if the setup is chaotic, the result usually is too.
Intensity that is too timid vs too aggressive
Another common miss is intensity. Too low, and the session feels like a polite electrical shrug. Too high, and the muscles jump, the experience becomes unpleasant, and the user quits. Many TENS protocols aim for a strong but comfortable sensory intensity, not a macho contest. Knee pain does not award medals for “bravest tingling.”
Session timing mistakes that make users quit too early or expect too much
Then comes timing. Some adults use TENS once for 8 minutes and conclude it is useless. Others expect one 20-minute session to settle a pain pattern that has been rehearsing for six months. Both errors are ordinary. FDA-cleared OTC TENS devices for limb pain often describe temporary relief and include timed sessions, which should be a clue about the category of help on offer. Temporary means temporary.
A familiar anecdotal pattern looks like this: one person uses TENS before a short walk and says, “That helped me get moving.” Another uses it after a week of escalating swelling and says, “It barely did anything.” Both experiences can be true. The knee problem underneath them is not the same creature.
Do Not Do This: 7 Common TENS Mistakes That Waste Time
Using TENS as a substitute for movement rehab
This is the biggest mistake because it feels productive. If TENS helps enough that you can do your walking, range-of-motion work, or strengthening, great. If it replaces those things for weeks, it becomes a stall tactic wearing a wellness costume.
Chasing stronger sensation as if stronger always means better
Intensity is not a trophy. Stronger is not always smarter, and discomfort tends to reduce adherence.
Reusing worn-out pads and blaming the device
Worn pads adhere poorly, conduct inconsistently, and turn the session into static theater. Replacement pads matter more than flashy mode names.
Using it on a knee that is visibly inflamed without asking why
If the knee is red, hot, rapidly swelling, or you feel ill, the right question is not “which mode?” It is “what is going on here?”
Ignoring the manual’s contraindications and device warnings
This is how adults become their own cautionary tale. Read the labeling. Then read it again.
Expecting one session to settle a months-long pain pattern
Longstanding pain usually needs load management, exercise, and clearer diagnosis. The device can help a little. It cannot negotiate with time by itself.
Treating “less pain” as proof the joint is safe to overload
This is the sneakiest error. Less pain after TENS is not permission to sprint, deep squat, or spend three hours in the garden like you are auditioning for a knee replacement brochure.
- Use TENS to support rehab, not dodge it
- Respect swelling, instability, and red-flag symptoms
- Replace pads and follow the device instructions
Apply in 60 seconds: Put “movement after relief” into your plan before every session.
Let’s Be Honest: The Real Reason People Like TENS
It feels active, immediate, and controllable
There is a psychological reason TENS keeps showing up in carts and bathroom drawers. Pain makes people feel passive. TENS gives them a dial, a routine, a sensation, and a sense that they are not just waiting. That matters. Control is not trivial. It can reduce fear and help people re-enter movement, which is often half the battle.
It may help you move enough to tolerate rehab work
This is probably the most defensible use case. If the device gives you 20 to 40 minutes of calmer symptoms and you spend that window walking, stretching, or doing your PT exercises, that is a sensible bargain. CDC arthritis guidance emphasizes physical activity and notes that even short sessions of 5 to 10 minutes can help. If TENS helps you reach those minutes, the value is practical, not mystical.
The emotional benefit of “I can do something right now”
A lot of home care succeeds or fails on whether a person feels capable tonight, not whether the protocol looks elegant on paper. That emotional lift is real. It just should not be mistaken for proof that the diagnosis is settled. A calmer nervous system is useful. A missed meniscus tear is not.
Short Story: The Night-Before-Stairs Problem
A reader-type many clinicians and rehab writers know well is the person whose knee hurts most in the evening after a normal day, not after a spectacular injury. Stairs feel mean. The couch feels good until standing up becomes a negotiation. They buy a TENS unit because it promises relief without a bigger life overhaul. The first session helps enough that the next morning feels less heavy.
That is where the fork appears. In version one, they decide the device “fixed it” and keep loading the knee the same way. Two weeks later, nothing changed except the charger location. In version two, they use the relief window to restart a short walking habit, trim back aggravating activity for a week, and notice the pattern is mostly after load, not random. Same device. Different story. The useful thing was not the buzz. It was what the buzz allowed them to do next.
Here’s What No One Tells You: Relief Without a Plan Usually Fades
Why pain-return cycles happen after the unit is turned off
If the source of knee irritation stays the same, symptoms often return once the session ends. That is not failure. It is category confusion. TENS is often a symptom modulator, not a load-management strategy, not a strengthening program, and not a structural diagnosis.
How orthopedic care usually pairs symptom control with strengthening and load management
Good orthopedic pain management is rarely one thing. It is a small orchestra. Activity modification. Sometimes topical NSAIDs for knee osteoarthritis. Exercise. Weight considerations when relevant. A brace or walking aid in selected cases. Periodic reassessment. NICE recommends topical NSAIDs for knee osteoarthritis and supports therapeutic exercise, while advising against offering TENS for osteoarthritis because of insufficient evidence. That is a useful clue about priorities. Readers trying to build a broader home plan may also benefit from a more general look at orthopedic pain management for older adults, especially when knee pain is part of a bigger function-and-safety picture.
The mistake of measuring success only by what you feel tonight
Tonight matters, but tomorrow matters too. Real progress usually looks like one or more of these: walking farther with less flare-up, needing fewer rescue strategies, climbing stairs with less dread, moving more consistently over one to two weeks, or understanding your triggers better. If the only success metric is “the knee felt strange for 25 minutes less,” you may end up renting relief instead of building it.
Mini calculator: Did TENS create a useful movement window?
- Minutes of relief after session: ____
- Minutes of walking or rehab completed during that window: ____
- Flare-up later that day, 0 to 10: ____
If the first number rises but the second stays at zero, the device may be soothing symptoms without helping your actual plan.
Safety Before Convenience: When a TENS Unit Is a Bad Idea
Pacemakers and implanted devices deserve extra caution
This is the cleanest safety line in the whole article. FDA-cleared labeling for consumer TENS devices commonly warns against use with cardiac pacemakers, implanted defibrillators, or other implanted metallic or electronic devices because of risks including interference and injury. That should end the debate for most home buyers.
Why adults still need to read OTC labeling, not just reviews
Reviews tell you whether the box arrived on time and whether the app was annoying. They do not replace labeling. The FDA notes that legally marketed electrical muscle stimulators and related consumer devices should meet premarket requirements and carry appropriate labeling. Translation: “FDA-cleared” is not a magic stamp of clinical greatness, but proper labeling is still a big deal.
Skin irritation, numb areas, and other reasons to stop and reassess
If pads are irritating the skin, if sensation is altered in the area, or if the session produces more pain, not less, stop and reassess. A small patch of irritated skin is not a moral failing, just a reminder that home devices still interact with actual human tissue. The body, rude but informative, usually votes eventually.
Don’t Miss the Red Flags: When Knee Pain Should Not Be Self-Managed First
Pop, swelling, limp, or giving-way after injury
These symptoms move you out of “self-manage first” territory. They suggest a possible structural injury that deserves evaluation.
Locking, catching, or loss of range of motion
A knee that truly locks or catches is telling you something more specific than “I’m sore.” Mechanical symptoms change the stakes.
Red, hot, swollen, feverish, or rapidly worsening pain
When heat, redness, fever, or rapid deterioration enter the story, infection and other urgent causes climb the list. Septic arthritis is a medical problem, not a consumer-electronics problem.
Pain that keeps returning despite self-care
If the knee keeps coming back with the same complaint despite rest, activity changes, and ordinary self-care, that repetition is data. Recurrent pain deserves a better question, not just a stronger setting on the unit.
- Injury with swelling or instability needs evaluation logic
- Heat, redness, and fever raise the urgency
- Locking and giving-way are not normal soreness language
Apply in 60 seconds: If any red flag is present, move “buy a gadget” below “get assessed” on your to-do list.
Smarter Use: How TENS Fits Into an Orthopedic Pain Management Plan
Use it to create a window for walking, stretching, or PT homework
This is where TENS becomes respectable. Not as a hero, but as a stagehand. If it helps you complete a walk, a short mobility sequence, or a strengthening session you would otherwise avoid, it has done useful work.
Pairing symptom relief with activity modification
If stairs flare the knee, reduce the unnecessary stair volume for a week. If deep bends trigger pain, shorten the range while building strength. If long standing lights up the joint, break it into smaller bouts. TENS can sit next to these changes, but it cannot make them optional. Some readers may also need practical support strategies, such as deciding whether a hinged knee brace for stairs belongs in the plan when stair use is one of the main aggravators.
What progress should look like after one to two weeks
Look for practical markers. Less morning stiffness. Easier sit-to-stand transitions. More walking tolerance. Fewer spikes after normal tasks. Better confidence. A knee that still needs the device daily but is otherwise unchanged may be giving you comfort without momentum.
When the next best step is evaluation, not another gadget
If you have used TENS sensibly for 1 to 2 weeks, paired it with smarter loading, and the knee is not becoming more predictable, that is a nudge toward professional evaluation. AAOS and orthopedic care pathways consistently treat swelling, instability, catching, locking, and persistent functional limitation as reasons to look deeper. If you are already at the stage where the story feels more like failed conservative care before an MRI, it may be time to shift from home trial-and-error toward clearer diagnostic planning.
Buying Without Getting Burned: What to Look for in a Home TENS Unit
Clear labeling, adult indications, and readable instructions
Buying advice gets weird online because features get mistaken for outcomes. Start simpler. Can you easily read the labeling? Does it clearly describe who it is for, what body areas it is intended to treat, basic warnings, and how long sessions should run? If the box sounds like a sci-fi novella but explains contraindications poorly, keep walking.
Why replacement pads and usability matter more than flashy modes
Most home users do not need eleven “massage” modes with names that sound like a nightclub menu. They need a device they will actually use correctly. Pads that are easy to replace. Controls you can understand without graduate school. A timer. Good adhesion. A manual written in normal adult language. Practicality beats sparkle.
The difference between “FDA-cleared” language and exaggerated marketing
“FDA-cleared” usually means the device met regulatory requirements for marketing in a defined category. It does not mean the product is the best option for your knee, and it does not mean every marketing claim around it deserves a salute. Be especially skeptical when the copy drifts from “temporary relief” toward “fixes joint problems” or “replaces therapy.” The bigger the promise, the smaller your wallet tends to feel later. If cost is part of the hesitation, it can also help to understand broader HSA eligibility for orthopedic braces and supports before you buy extra devices around the main problem.
Buying checklist before you compare models:
- Contraindications section easy to find
- Pad replacement cost visible before checkout
- Session timer and intensity controls clearly explained
- Adult use labeling and readable instructions
- Return policy and support easy to understand
Neutral next step: Compare usability and pad costs before comparing “modes.”
- Usability beats gimmicks
- Pad availability matters long after checkout day
- Marketing language should stay smaller than the evidence
Apply in 60 seconds: Before buying, search the manual for “contraindications” and “replacement pads.”
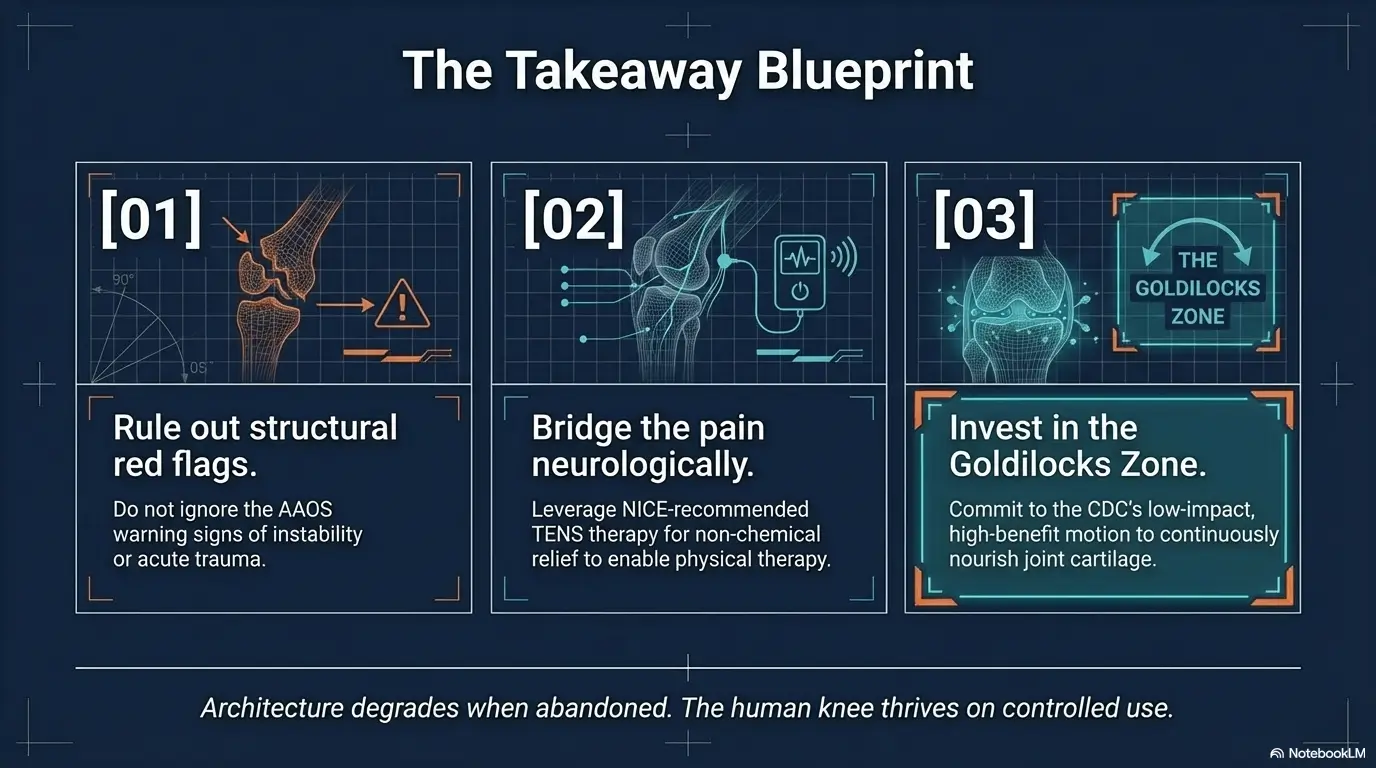
FAQ
Does a TENS unit actually help knee pain or just distract from it?
Sometimes both. It may provide temporary symptom relief for some people, which can be useful if that relief helps you move, walk, or do rehab. But for knee osteoarthritis, higher-quality evidence has been mixed, and placebo-controlled results have not been consistently impressive.
Is TENS good for knee arthritis pain?
It may help some individuals temporarily, but it is not a reliable stand-alone solution. NICE recommends against offering TENS for osteoarthritis because evidence of benefit is insufficient, while still emphasizing other core measures like exercise and appropriate pain management.
Where should you place TENS pads around the knee?
Placement depends on the device instructions and the painful region. What matters most is not improvising wildly. Follow the manual, avoid damaged skin, and stop if the setup is uncomfortable or unclear. Random placement is one of the easiest ways to conclude a device “doesn’t work” when the setup never had a fair chance.
How long should you use a TENS unit on your knee at one time?
Use the session timing in the product instructions, because it varies by device and intended use. Many OTC devices for limb pain frame treatment as temporary relief and include timed sessions rather than unlimited use.
Can you use a TENS unit every day for knee pain?
Some adults do, but daily use only makes sense if the device is being used safely, the labeling allows it, and the knee problem is already reasonably understood. Daily use without any improvement in function or predictability is a sign to reassess the plan.
When should you not use a TENS unit on your knee?
Avoid it if you have an implanted pacemaker, implanted defibrillator, or other implanted metallic or electronic device unless your clinician has specifically cleared it. Also do not make it your first move for a red, hot, swollen, unstable, or newly injured knee.
Can TENS replace physical therapy for knee pain?
No. At best, it may help make movement or exercise more tolerable. It is a supporting tool, not a substitute for evaluation, diagnosis, progressive exercise, or load management.
Why does TENS help during use but the pain comes back later?
Because symptom modulation is not the same as solving the cause. If the joint is still being irritated by mechanics, load, weakness, or inflammation, the pain often returns after the session ends. For readers trying to think beyond one gadget, that is also the logic behind articles on pain management for seniors waiting on joint treatment and what a joint injection consultation may cost when conservative measures stop feeling straightforward.
Next Step: The One Concrete Action That Prevents Most Bad Decisions
Before buying or using TENS, classify your knee pain into one of three buckets: overuse, arthritis-style, or injury-style
This is the simple action that prevents a surprising number of expensive and time-wasting detours. If your knee pain is overuse-style, TENS may be a reasonable short-term add-on while you reduce the aggravating load and rebuild tolerance. If it is arthritis-style, expectations should stay modest and the real engine of progress is usually movement, symptom pacing, and a broader management plan. If it is injury-style, especially with swelling, locking, buckling, or a distinct twist-and-pop story, evaluation rises to the top. Work-related readers may notice that this bucket method matters even more when the knee is being stressed by repetitive demands, as in warehouse worker knee pain patterns where load and repetition blur the story.
If you cannot clearly classify it, book an evaluation before building a home-treatment routine
This closes the loop from the beginning. What can a TENS unit actually do? It can sometimes make the knee feel better for a while. That is useful. It is not enough. The smartest move you can make in the next 15 minutes is not to obsess over waveforms or mode names. It is to write down your pain pattern, list any red flags, and decide whether your knee belongs in the overuse, arthritis-style, or injury-style bucket. If you cannot classify it cleanly, let that uncertainty guide you toward an evaluation rather than a longer romance with symptom relief.
Last reviewed: 2026-03.
