
2:07 A.M. Survival: The Log Roll Technique
At 2:07 a.m., you don’t need willpower—you need a move that doesn’t light up your leg like a live wire.
Most “normal” rolling is a two-part twist: shoulders go first, hips lag behind, and your low back becomes the hinge. When sciatica is already irritated, that small torsion can turn a simple rollover into a full-blown flare—lost sleep, stiff mornings, and that anxious “don’t move wrong” feeling.
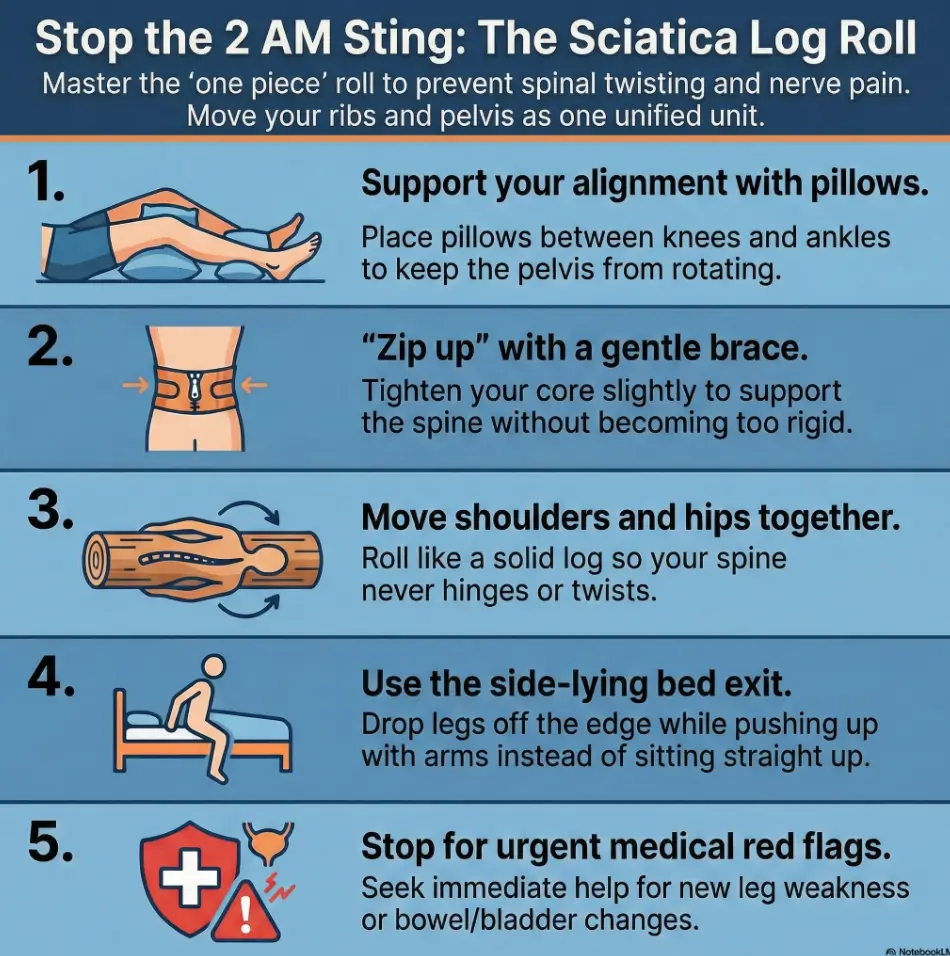
The log roll technique is designed to change your position without spinal twisting. By moving your shoulders and hips together as one unit, keeping your knees stacked, and letting your arms and legs do the work, you reduce the mechanical triggers that keep poking the nerve.
This is the same bed-mobility pattern taught in professional rehab settings, incorporating practical cues and pillow setups for the knees and ankles to keep your nights calmer.
Slow is a safety feature. And the pause is part of the technique.
Table of Contents
Log roll first: Why rolling hurts (and what you’re unknowingly twisting)
The “hidden twist” that spikes sciatica at 2 a.m.
Rolling over seems like a simple torso move… until you watch what actually happens. Most people do a “two-part roll”: shoulders go first (because you’re sleepy and impatient), then the pelvis follows late. That lag creates a torsional twist through the low back. If a nerve root is already irritated, that twist can feel like you just poked a live wire.
A small confession: the first time I learned this, it wasn’t from a fancy clinic. It was from a nurse who looked at me like, “Yes, we are absolutely going to practice rolling. No, you don’t get to be dramatic.” Two tries later, I realized the “technique” was basically: stop moving like a folding chair.
Sciatica vs low-back strain: why both hate sloppy rotation
“Sciatica” is often used like a bucket term, but medically it’s describing symptoms—leg pain, tingling, numbness, or weakness—linked to irritation of the sciatic nerve or its roots. MedlinePlus (National Library of Medicine) describes sciatica as pain (and sometimes numbness/weakness/tingling) in the leg related to pressure or injury affecting the sciatic nerve pathway. That matters because rotation + bending + load is a classic way to annoy sensitive tissues—whether it’s a nerve root, a disc, or just an angry muscle group that’s tired of your midnight acrobatics. If you want a quick “language reset” on what people mean by sciatica, this primer on sciatic nerve pain and sciatica symptoms helps separate the buzzword from the pattern.
Curiosity gap: The one body part that “cheats” first (it’s not your hips)
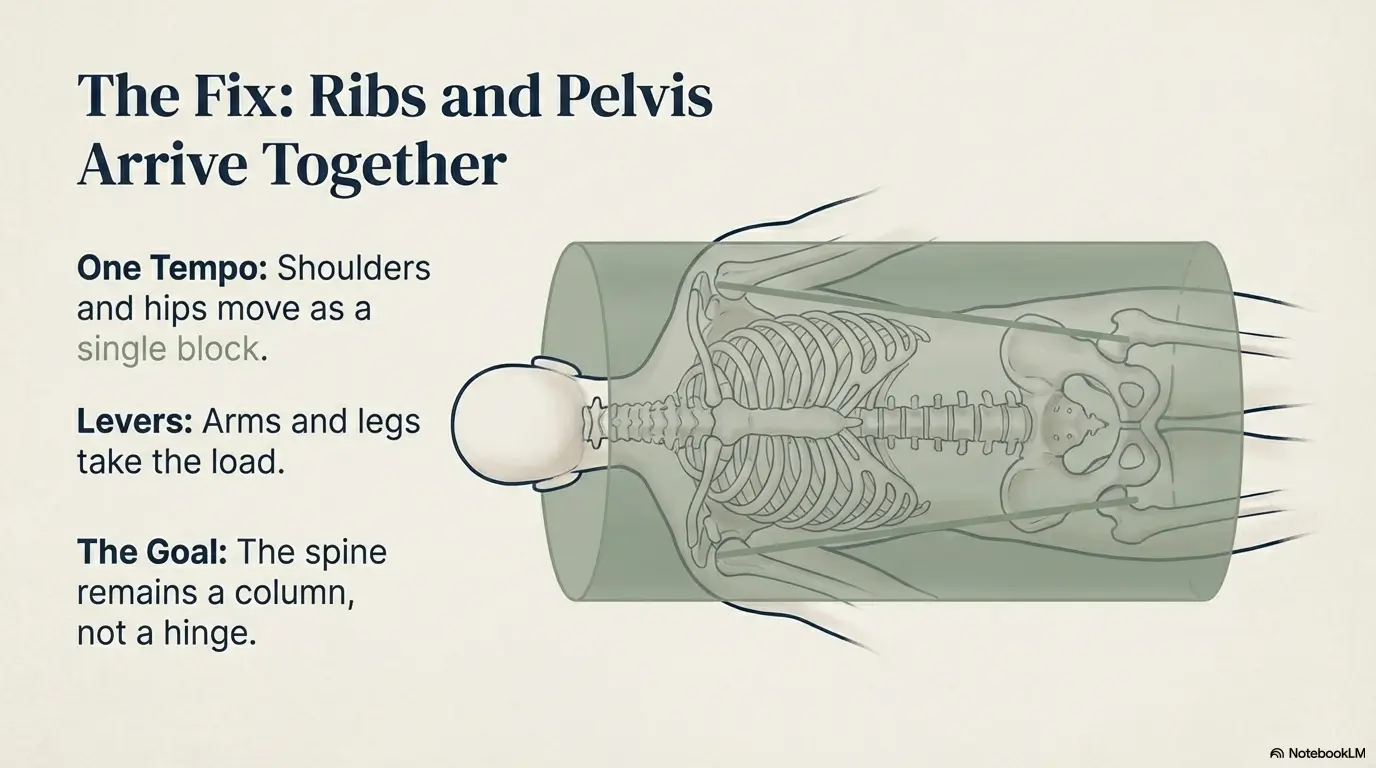
It’s your ribs. Specifically: your ribcage tries to “lead” while your pelvis stays parked. When your ribs rotate and your pelvis doesn’t, your low back becomes the unwilling hinge. The log roll technique solves this by making the ribs and pelvis arrive together.
Show me the nerdy details
Rolling is a coordination problem more than a strength problem. In bed, friction from sheets and the soft surface makes segments move at different speeds. If the thorax rotates while the pelvis lags, the lumbar spine takes the torsion. The log roll reduces segmental shear by asking the trunk to move as one unit and shifting effort to the arms and legs (bigger levers, less spinal twist).
- Most flare-ups happen during the lag (shoulders first, hips late).
- The goal is one tempo: ribs and pelvis move together.
- Arms and legs do more work so your spine does less.
Apply in 60 seconds: Next time you roll, whisper “one piece” and move slower than you think you need.
Who this is for / not for: Quick self-check before you try it
Good fit: leg pain with turning, sensitive low back, post-flare nights
This is for you if:
- Turning in bed triggers leg pain or a sharp “jolt.”
- Your low back feels fragile after a flare.
- You wake up and think, “If I move wrong, I’m toast.”
- You want a safe how-to, not a motivational speech.
A small lived-experience note: the night after I overdid a long walk, I didn’t need a miracle. I needed a way to roll over without paying for it for the next 6 hours. This technique is that kind of unglamorous win.
Not for: recent major injury/surgery, severe osteoporosis risk, unexplained night pain
If you’ve had recent spine surgery, a major fall/accident, or you’ve been told you’re at high fracture risk, you should get individualized instructions first. The log roll is commonly taught in post-op settings—but your version may be different depending on restrictions.
Also: if you’re having unexplained night pain that’s worsening, fever/chills, or cancer history with new back pain, don’t “DIY” your way through it. That’s not a “technique” problem—that’s a “get evaluated” problem.
When to stop immediately: new weakness, saddle numbness, bowel/bladder changes
This is the serious part. Major medical organizations emphasize urgent evaluation if you develop new leg weakness or bowel/bladder control problems with sciatica symptoms. Mayo Clinic lists red flags such as sudden weakness/numbness in a leg and trouble controlling bowels or bladder as reasons to seek immediate medical care. If you want the “don’t tough it out” version in plain language, keep this bookmarked: when low back pain is an emergency.
- Yes — Your main trigger is rolling/bed transfers, not constant severe pain.
- Yes — You can bend both knees comfortably (even a little).
- Yes — No new progressive weakness, no saddle numbness, no bowel/bladder changes.
- No — Pain is from a recent major injury, or you have strict post-op restrictions you haven’t been taught.
Next step: If you’re a “yes” on the first three bullets, try the bed setup section first—then do two slow practice rolls in daylight.
Setup matters: The 30-second bed prep that makes log roll easier
Pillow placement: knees, ankles, and why “one pillow” often fails
If your knees drift apart, your pelvis rotates. If your pelvis rotates, your low back gets pulled into the drama. So your pillow strategy is basically: help your legs behave. If you’ve ever wondered whether a compact knee pillow beats a long body pillow for control, this breakdown—knee pillow vs body pillow for sciatica—maps the tradeoffs without the fluff.
- Side sleeping: pillow between knees (and sometimes between ankles) so the top leg doesn’t slide forward.
- Back sleeping: pillow under knees to reduce low-back tension for many people.
- If one pillow slips: try a longer pillow or add a small towel roll at the ankles.
Personal note: I used to “rage-pillow” at night—throw one between my knees and hope for the best. It helped… until it didn’t. The moment I supported the ankles too, the roll felt less like wrestling.
Mattress friction hacks: sheets, clothing, and reducing “stickiness”
Friction is a silent villain. If your shirt grabs the sheet, your shoulders move slower than your hips. If your hips stick, your ribs twist ahead. Quick fixes:
- Use smoother sleepwear (or a smoother sheet material) to reduce “stopping” mid-roll.
- If you’re overheating, don’t fight friction with sweat-soaked fabric—change the layer.
- Keep a small “slide” layer nearby (a thin towel or silky scarf) only if it feels stable and safe.
Curiosity gap: One small height change that makes rolling feel “automatic”
If your mattress is very soft, your hips sink deeper than your shoulders. That uneven sink is basically a twist generator. Sometimes a tiny change—like adding a thin topper, or even moving to a firmer side of the bed—reduces the “ditch” effect. It’s not about luxury. It’s about your pelvis not falling into a hole. If you’re debating thickness, 2 vs 3 inch mattress topper is the most practical rabbit hole you can go down.
- Pillows keep knees stacked so your pelvis doesn’t twist.
- Less friction = fewer “stuck” moments mid-roll.
- Soft mattresses can create a twisty “sink gap.” If you’re still unsure, this guide to mattress firmness for sciatica helps you pick “supportive” without turning it into a luxury purchase crisis.
Apply in 60 seconds: Put a pillow between knees and ankles, then do one slow practice roll before you fall asleep.
Step-by-step: Log roll from back → side (the classic sciatica-safe turn)
Step 1: Bend knees, feet planted—set your “hinge”
Start on your back. Bend both knees so your feet are planted (or lightly contacting the bed). This puts your legs in a position where they can guide the roll without yanking your pelvis.
Step 2: Brace gently—think “zip up,” not “crunch”
Gently tighten your core like you’re zipping up snug jeans—supportive, not rigid. Over-bracing makes you stiff, and stiffness increases friction (and frustration).
Step 3: Arms lead without dragging the spine
Bring your arms slightly forward in the direction you’re rolling. Your arms help initiate the turn, but the goal is not “shoulders first.” It’s “whole trunk together.”
Step 4: Shoulders + hips move together—one unit, one tempo
Here’s the key: move your shoulders and hips as one “log.” Imagine your ribcage and pelvis are taped together (in a good way). If you feel your shoulders arrive first, slow down and restart.
Step 5: Land and breathe—don’t “re-adjust” with a twist
Once on your side, pause. Take one breath. Many people do a perfect roll… then ruin it by “fine-tuning” their position with a little spinal twist. Treat the landing like a stop sign.
- Cue: “Knees together.”
- Cue: “Ribs over hips.”
- Cue: “One tempo.”
Anecdote: the first time I tried this, I rolled so slowly it felt ridiculous—like I was auditioning for a sloth documentary. But the next morning, my leg symptoms were calmer. Turns out, sleep doesn’t care if you look cool.
Step-by-step: Log roll from side → back (the move most people botch)
Step 1: Knees stay stacked—no top knee drifting forward
From your side, stack knees (and ideally ankles). If the top knee slides forward, your pelvis rotates and you’re back in Twist City.
Step 2: Elbow/forearm helps you guide—not yank
Use your arms as steering, not brute force. Press lightly into the mattress with your forearm/hand to begin the roll. Think “guide and glide,” not “heave and hope.”
Step 3: Return as a block—shoulders don’t arrive first
Let your trunk rotate as one unit. If you notice your chest opening to the ceiling while your hips stay stuck, pause. Reset. Roll again with a smaller range and slower tempo.
Let’s be honest… the “halfway twist” is the real villain
Most people don’t twist a lot. They twist just enough—that little halfway moment where you’re neither on your side nor on your back. That’s where the nerve irritation loves to shout. Your fix is boring but powerful: commit to one direction and move in one smooth block.
- Stack knees (and ankles if needed) to protect pelvic alignment.
- Use arms to guide the roll, not to yank your torso.
- Avoid the “halfway twist” by moving continuously and slowly.
Apply in 60 seconds: Put one hand on your top hip and feel it move with your ribs—no lag allowed.
Step-by-step: Getting out of bed (where sciatica flares love to happen)
Side-lying first—then legs off the edge as you push up
This is the bed-transfer classic taught in many rehab settings: roll to your side first, then let your legs drop off the edge as you push your upper body up with your arms. The point is to avoid sitting straight up by bending and twisting through your low back.
Use your arms like a lever, not your low back
Place your hand(s) in front of you and press into the mattress to help lift your torso. Your arms are strong levers. Your low back is not a lever. It’s the thing we’re trying to keep calm.
Curiosity gap: Why sitting up straight in bed can be worse than rolling
When you “sit straight up,” many people unknowingly do a combo move: flex spine, twist slightly, then push. That’s three irritations in a trench coat. Side-lying exit reduces that by keeping your trunk aligned and outsourcing effort to arms and legs.
- Best when turning or sitting up spikes pain
- Uses arms/legs as levers
- Lower twist risk
- Risky during flares
- Often mixes bend + twist + push
- Can provoke a jolt down the leg
Neutral action: If you’ve had a nighttime flare this week, choose A for 7 nights and track whether mornings feel less “grabby.”
Anecdote: the first time I used the side-lying exit, I realized I’d been “sitting up” like I was trying to win a sit-up contest at a sleepover. No prize. Only pain.
Don’t do this: Two moves that feel “normal” but spike pain
Mistake #1: Upper body turns first (shoulders win, hips lose)
This is the classic: you twist your shoulders toward the new position while your hips stay put. You’re basically wringing out your low back like a towel. If your sciatica is sensitive, it’s going to complain.
Mistake #2: One knee leads like a windshield wiper
If one knee swings across your body while the other stays behind, your pelvis rotates. That rotation often pulls the lumbar area into torsion. It can feel “small,” but nerves are drama queens about small twists.
Quick fix cues: “knees together,” “ribs over hips,” “move as one”
- Knees together: use a pillow if your legs won’t cooperate.
- Ribs over hips: don’t let your chest open before your pelvis follows.
- Move as one: slow the roll and keep one tempo.
Common mistakes: The checklist that prevents 80% of flare-ups
Rushing the turn: speed creates twist
When you rush, segments move at different speeds. That’s where torsion sneaks in. In bed mobility, slow is a safety feature, not a personality trait.
Over-bracing: stiffness creates friction and strain
If you brace like you’re about to deadlift, you get rigid. Rigid bodies stick to sheets, then jerk past the sticky point. Instead, brace at about 20–30% effort—supportive, not locked.
Repositioning after landing: the sneaky second twist
Many flare-ups happen after a good roll. You land on your side, then rotate your shoulders to “settle in.” That little twist is often the straw that wakes the nerve.
Here’s what no one tells you… the pause is part of the technique
That one breath after the roll isn’t optional fluff. It’s the moment you check: “Did I stay aligned?” And it’s the moment you decide not to do the second twist. (Yes, it’s boring. That’s why it works.)
- Try this: Count “one-one-thousand” after landing before adjusting anything.
- Then: If you must adjust, move your whole body as a unit again.
Neutral action: If your result is “High caution,” do the bed prep and practice 2 slow rolls before sleep—then stop.
Make it stick: Nighttime cues, reps, and what progress feels like
The 3-cue mantra (simple enough at 3 a.m.)
At night, your brain is not here for a lecture. Give it three cues:
- Knees together.
- Zip up (gentle brace).
- One piece.
Micro-practice in daylight (yes, for bed mobility)
Practice when you’re calm, not when you’re panicking. Do 2 slow log rolls in daylight once a day for a week. It takes under 2 minutes. The payoff is that your body remembers the pattern at 2 a.m.
What “good” feels like: less grabbing, fewer jolts, calmer leg symptoms
Progress is not “I can roll like a gymnast.” It’s:
- Less “grab” in the low back mid-roll.
- Fewer sharp leg zings when changing positions.
- Less need to readjust after landing.
Anecdote: my first sign of improvement wasn’t pain-free sleep. It was confidence. I stopped holding my breath every time I moved. If mornings are when symptoms feel the most “wired,” pairing safe nights with a gentle AM routine can help—see morning sciatica nerve glides for an option that’s built around irritability, not heroics.
When to seek help: Red flags + the “don’t wait” symptoms
Same-day evaluation signals: worsening weakness, foot drop, severe numbness
If you notice worsening weakness (like your foot slapping the ground, or you can’t lift your toes like usual), severe or spreading numbness, or pain that escalates rapidly, don’t “out-technique” it. That’s a medical conversation.
Mayo Clinic’s sciatica guidance highlights urgent evaluation for symptoms like sudden leg weakness/numbness and bowel/bladder control trouble. It’s not to scare you—it’s to protect you.
Urgent signs: bowel/bladder changes, saddle anesthesia
If you have new bowel or bladder control problems or numbness in the saddle area (groin/inner thighs), seek urgent medical care. These symptoms can be associated with serious nerve compression syndromes that are treated as emergencies.
If it’s been weeks: what to ask PT/clinician (sleep pain, turning triggers, nerve symptoms)
If this has been dragging on for weeks, bring specifics:
- What position hurts most (back → side, side → back, or getting up)
- Where symptoms travel (buttock, calf, foot)
- What changes them (walking, sitting, coughing, rolling)
- What you’ve tried (pillow setup, log roll practice, heat/ice)
- Your 0–10 pain level during rolling and on waking
- Any numbness/tingling map (where exactly)
- Any weakness changes (stairs, toe lift, heel walk)
- What positions worsen/improve symptoms
- How long this episode has lasted (days/weeks)
Neutral action: Write this on one note in your phone so your appointment is faster and more useful.
FAQ
Does log rolling help a herniated disc or just sciatica?
Log rolling doesn’t “fix” the cause, but it can reduce twisting that irritates sensitive structures. If your sciatica is related to disc irritation or nerve root sensitivity, minimizing torsion during bed mobility often helps symptoms stay calmer. If you’re trying to make sense of overlapping labels, sciatica vs herniated disc explains the common patterns without turning it into a diagnosis quiz.
Should my knees be bent or straight when I log roll?
Bent knees usually work best because they help your legs guide the roll and keep your pelvis from rotating awkwardly. Straight legs tend to make people swing one leg and twist.
What if log rolling still hurts—am I doing it wrong?
Not necessarily. Try (1) slower tempo, (2) add pillow support at knees and ankles, and (3) stop the “second twist” after landing. If pain spikes sharply, or you notice new numbness/weakness, pause and get evaluated.
Is it better to sleep on my back or side with sciatica?
It depends. Many people do better with a pillow under knees on the back, or a pillow between knees (and sometimes ankles) on the side. The best position is the one that reduces symptoms and lets you change positions without flare-ups. If you want the most practical “choose-your-own-night” map, read how to sleep with sciatica and then zoom in to side sleeper sciatica at night if that’s your default position.
Do I need a pillow between my knees for log rolling?
You don’t “need” it, but it often makes the technique easier by keeping knees stacked and pelvis aligned. If your top knee always slides forward, a pillow is a simple fix.
Can log rolling make sciatica worse?
If you rush, twist halfway, or over-brace and jerk against friction, it can aggravate symptoms. Done slowly with knees stacked and trunk moving as one unit, it’s generally a safer way to roll than twisting.
How long should it take to roll over using the log roll technique?
In a flare, aim for 5–10 seconds. That sounds slow—because it is. Speed creates lag and lag creates twist.
Can pregnant people use a log roll for back pain and sciatica?
Often, yes—especially because pregnancy can make twisting uncomfortable. The key is comfort and safety: use pillows, move slowly, and follow guidance from your OB/midwife if you have restrictions.

Next step: One concrete action tonight
Do this once before sleep: set pillows + rehearse 2 slow log rolls
Tonight’s goal isn’t perfection. It’s rehearsal.
- Put pillow between knees (and ankles if needed).
- Do 2 slow log rolls: back → side → back.
- After each landing, take one breath and refuse the second twist.
Keep a 10-second note: pain level before/after turning (0–10)
This is how you turn “I think it helps?” into “Yes, it helps.” Track two numbers: pain during rolling, and pain on waking. You’re looking for a trend, not a miracle.
If pain spikes: stop and switch to a supported side-lying reset
If you feel a sharp spike, stop. Reset on your side with knees supported and take 3 slow breaths. If symptoms are escalating or you notice new numbness/weakness, don’t push through.
If you’re building a “calm night kit,” keep it simple and test one variable at a time. Some people do better with targeted warmth; if that’s you, read sleeping with a heating pad for sciatica so you’re not improvising at 2 a.m. Others prefer gentle, evenly distributed pressure—here’s a practical take on weighted blankets for sciatica (including when they’re a bad idea).
Conclusion
Remember the curiosity gap from the beginning—the body part that “cheats” first? Your ribs. That’s the sneaky move that turns a simple roll into a spinal twist. The log roll technique works because it stops the cheating: ribs and hips move together, knees stay stacked, and your arms do the heavy lifting. It’s not magic. It’s mechanics.
If you want a calm, practical 15-minute win: do the pillow setup, practice two slow rolls, and write a 10-second note with your pain score. That’s it. If the numbers trend down over a week, you’ve found a low-effort lever that makes nights less scary.
- Knees together (pillow helps)
- Gentle brace (“zip up”)
- Ribs + hips together (one tempo)
- Pause after landing (no second twist)
- Shoulders first, hips late
- One knee swings like a wiper
- Over-bracing → sticking → jerking
- “Just one little readjust” twist
Last note (operator-to-operator): if you ever see the big red flags—new weakness, saddle numbness, bowel/bladder changes—don’t workshop your pillow setup. Get help quickly. And if side-sleeping is your default battleground, this guide to side sleeping with sciatica can help you keep alignment without turning your bed into a physics lab.
Last reviewed: 2026-01-24
