
The Side Sleeper’s Guide to Orthopedic Hip Pain Management
For side sleepers, hip pain is rarely just a pain problem. It is usually a pressure problem, an alignment problem, and a timing problem that waits until 2 a.m. to introduce itself.
Many spend money in the wrong category, blaming the mattress or stacking pillows, while the body reacts to hours of compression and twisting. This guide helps you identify what is actually driving your discomfort, from knee pillow placement to mattress support, and fits into a broader orthopedic pain management strategy instead of a midnight shopping spree.
“The smartest fix is usually smaller than people expect. Start with the variable that matches the pain, and make the bed stop arguing back.”
Learn to recognize the patterns of nighttime load and positioning to regain your sleep quality and protect your long-term mobility.
Table of Contents
Fast Answer: Orthopedic pain management for side sleepers with hip pain usually works best when pain relief is approached as a positioning problem, a pressure problem, and a timing problem all at once. The goal is not only to reduce pain at bedtime, but to protect the hip from overnight compression, improve sleep quality, and avoid habits that quietly make morning stiffness and irritation worse.
Safety / Disclaimer: This content is educational and not a substitute for medical advice, diagnosis, or treatment. Hip pain while side sleeping can come from several causes, including bursitis, arthritis, tendon irritation, referred back pain, or post-injury changes. Severe pain, inability to bear weight, fever, sudden swelling, new weakness, numbness, recent trauma, or pain that rapidly worsens should be evaluated by a licensed clinician.
Side-sleeper hip pain is usually a pressure problem before it feels like a sleep problem
Why the mattress is not always the villain, even when it feels that way
When your hip throbs at 2 a.m., it is tempting to blame the mattress with courtroom confidence. Sometimes that is fair. Often, though, the mattress is only the stage. The real drama is the way your body settles into it for 6 to 8 hours. A side sleeper places a concentrated load on the outer hip, and that load can irritate already sensitive tissue long before the mattress itself deserves the full blame.
I once spent two weeks convinced a guest-room bed was the problem, only to realize my hips were twisted forward every night because I was hugging one pillow and forgetting the one between my knees. The mattress was mediocre. My setup was the true little saboteur.
How direct compression turns one sore hip into a long, restless night
Direct compression matters because tissues do not negotiate well with repeated pressure. If the painful side is down, the outside of the hip may absorb that pressure all night. If the painful side is up but the top leg drops forward, the hip can still be pulled into an irritated position. Either way, the hip is not getting a clean break. It is simply arguing in a different dialect.
That helps explain why nighttime pain can feel sharper than daytime discomfort. During the day, you shift. You stand up. You sit down badly, then redeem yourself by walking to the kitchen. In bed, the body lingers. It marinate-sleeps in one posture.
The real issue may be what the hip endures for six unbroken hours
Many people judge a sleep position by the first 2 minutes. That is understandable and often misleading. A position can feel fine at lights-out and still become a problem by 4 a.m. because small misalignments accumulate. What matters is not just comfort at entry. It is load over time.
A smarter question: “What is my hip enduring for the next six hours?” That question changes everything. It shifts the goal from instant comfort to sustainable positioning.
- Pressure builds slowly, even in positions that feel fine at first
- Small alignment errors become louder after hours
- The best fix usually targets body setup before it targets shopping
Apply in 60 seconds: Notice whether the pain feels more like direct pressure on the outside hip, twisting through the pelvis, or stiffness after staying still.
Before bed first: why pain management often starts 30 minutes earlier
What to change before your head hits the pillow
Good sleep positioning begins before the body meets the bed. A hip that has spent the evening stiff, compressed, or inflamed does not magically become cooperative at bedtime. The 20 to 30 minutes before sleep can lower the friction of the whole night. That might mean a short walk around the house, a warm shower, a prescribed medication taken exactly as directed, or simply not collapsing into bed after 3 hours on the couch in a crooked pose that deserves its own apology letter.
The point is not to build a spa routine with candles and impossible discipline. The point is to avoid entering bed already irritated. Think of bedtime as the final scene of a play that started at dinner.
Why late-night stiffness can sabotage even a good sleep position
Stiffness changes how your body lands. A hip with reduced mobility or guarded muscles often drops into side sleeping less smoothly. That can increase pressure on one spot or create rotation through the pelvis. The result is a position that looks reasonable from across the room but feels expensive by sunrise.
Organizations like the American Academy of Orthopaedic Surgeons often explain joint pain in practical terms: mechanics, inflammation, tissue irritation, activity load, and function all matter together. That matches what many side sleepers notice in real life. The hip that had a long car ride, an evening on a soft couch, or a sedentary day often protests more once the body finally stops moving.
Let’s be honest… most people judge the position without fixing the setup first
This is where impatience sneaks in. You try side sleeping once, it hurts, and you conclude the position is impossible. But sometimes the problem was the setup, not the category. Your hip was already stiff. The pillow stack was random. You climbed into bed like a folding chair. Then the position gets blamed for sins it did not commit alone.
Try this instead for 3 nights: spend 5 to 10 minutes unwinding the hip before bed, then enter the same position with deliberate alignment. That gives the experiment a fair trial.
Eligibility checklist: Is a pre-bed routine worth trying first?
- Yes: your pain feels worse after sitting still for long stretches
- Yes: the first 10 minutes in bed feel rigid or pinchy
- Yes: you go from sofa to bed without moving much in between
- No: pain is severe, sudden, or linked to recent injury or fever
Next step: If you checked 2 or more “yes” items, test a 10-minute pre-bed reset before changing your mattress.
Show me the nerdy details
Position tolerance is affected by tissue sensitivity, joint angle, and time under load. A modest improvement in pre-bed mobility or symptom settling can reduce the peak irritation reached overnight, even when the sleep position itself remains largely the same.
Pillow strategy matters more than people expect for side sleepers with hip pain
How a knee pillow can reduce hip twisting instead of merely adding comfort
A pillow between the knees is not a decorative bedtime accessory. It can reduce the amount of pelvic rotation and inward pull on the top hip. That matters because the top leg is heavy enough to drag the pelvis out of neutral. When the leg falls forward, the hip may twist into a position that irritates the outer hip, the front of the joint, or even the low back.
The best knee pillow is not always the fluffiest. Sometimes a firmer pillow works better because it actually keeps the knees separated. Soft pillows can compress into a sentimental pancake by midnight.
Why ankle-to-knee alignment can calm the outside of the hip
Many people place a pillow only at the knees and leave the ankles hanging in space. That can still allow rotation. Ideally, the support should help keep the top leg from collapsing forward from thigh to ankle. You do not need a special gadget to do this. A regular pillow folded lengthwise can work. The goal is alignment, not luxury branding in a zippered case.
When the leg is supported more evenly, the outer hip often feels less “pinched” or overworked by morning. It is not magic. It is mechanics wearing slippers.
The difference between “soft support” and support that actually changes load
Support must alter load to matter. If your pillow is so thin that the top knee still dives forward, the hip will not care that the pillow exists. If the pillow is too thick, you may create a different strain. This is why testing matters more than internet certainty.
A quick home rule: when you settle into side sleeping, your top knee, ankle, and pelvis should feel supported without having to grip or brace. If you have to hold yourself together, the setup is not doing its job.
Practical cue: A useful pillow setup should make the hip feel quieter within 5 to 10 minutes, not merely softer under your face.
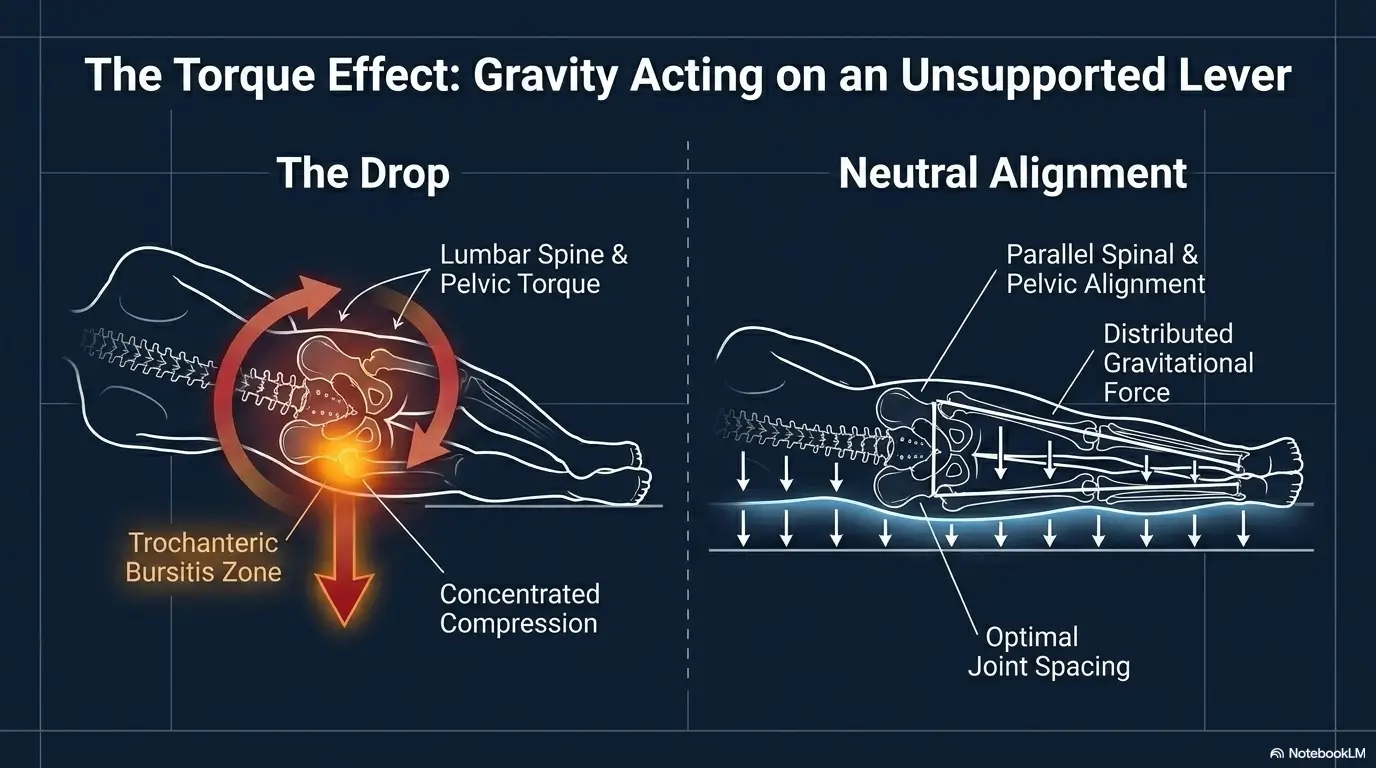
Sleep on the painful side or not? The answer is less simple than people hope
When avoiding the sore side helps
If the painful side hurts mainly from direct pressure on the outside hip, avoiding that side is often the first sensible move. This is especially true when the pain is sharp, tender to the touch, or clearly worse when the sore hip is down on the mattress. In that situation, sleeping on the non-painful side with strong leg support may reduce irritation quickly.
That said, the non-painful side is not a magical kingdom. It can become problematic too if the top leg drags the pelvis forward or if the painful top hip hangs without support.
When switching sides creates a different kind of strain
Some people switch away from the painful side and then feel a different ache in the front of the top hip, the buttock, or the low back. That does not always mean side sleeping is doomed. It may mean the new position introduced rotation, strain, or unsupported weight through the top leg. Pain has a way of moving one chair over and pretending to be a new person.
I have seen this pattern in people who say, “I stopped sleeping on the painful side, but now both sides feel wrong.” Often the body is not asking for a complete sleep identity crisis. It is asking for better support and fewer extremes.
How to test positions without turning bedtime into a guessing game
Do not test 5 different positions in one night. That produces confusion, not insight. Pick one setup and give it 2 to 3 nights unless it is clearly intolerable. Track three things: pain while falling asleep, awakenings during the night, and how the hip feels in the first hour after waking.
Those three markers are more useful than a dramatic midnight verdict. A position that reduces awakenings and morning soreness is often worth more than one that feels momentarily perfect at lights-out.
Decision card: Painful side down vs non-painful side down
Choose the non-painful side first when direct pressure on the sore hip is the main trigger, tenderness is on the outside hip, or pain spikes quickly when you lie on that side.
Re-test the painful side carefully only if the non-painful side creates major twisting strain, the painful side tolerates soft pressure better than expected, or you can unload it with strategic padding.
Neutral action: Run one setup for 2 to 3 nights before you promote or fire it.
Who this is for, and who it is not for
Who this helps: side sleepers with nighttime hip pain, pressure pain, or morning soreness
This guide is for adults whose hip pain is most noticeable in bed, especially when side sleeping creates pressure, pulling, or stiffness. It is for the person who wakes up sore on the outside of the hip, feels better after moving around, and suspects that sleep mechanics are part of the problem. It is also for the person who does not want to buy three expensive products before understanding what the body is actually complaining about. If the pattern feels broader and more persistent, it can also help to compare it with a fuller guide to hip pain at night.
Who may need a different plan: recent injury, post-surgical recovery, severe arthritis, or nerve-like symptoms
This is not the whole plan for everyone. People with a recent fall, new inability to bear weight, suspected fracture, fever, major swelling, post-surgical restrictions, cancer history, progressive weakness, or numbness deserve tailored medical guidance. Likewise, if the pain shoots, burns, or clearly travels from the back down the leg, the hip may not be the sole headline act.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases explains joint and musculoskeletal symptoms in ways that remind us of a basic truth: pain location and pain source do not always match perfectly. The body is occasionally a gifted ventriloquist.
When self-management makes sense, and when it should not be the whole plan
Self-management makes sense when the pain is mild to moderate, mechanical, somewhat position-dependent, and not paired with red flags. It should not be the whole plan when sleep is consistently ruined, function is worsening, or the pain keeps expanding its territory despite careful changes.
That line matters. Home strategies are excellent servants and poor monarchs.
- Better candidates notice clear links to posture, pressure, and bedtime habits
- Poor candidates have red flags, major functional loss, or new neurologic symptoms
- Position-based pain can still deserve professional evaluation if it persists
Apply in 60 seconds: Ask whether your pain changes meaningfully with pressure, position, or movement. If not, do not assume a pillow-only fix will carry the whole load.
Don’t do this: common side-sleeping fixes that quietly make hip pain worse
Why sleeping twisted at the waist can irritate more than it relieves
One of the most common mistakes is turning the upper body one way and the pelvis another. It can feel cozy for 4 minutes and treacherous by dawn. Twisting at the waist while side sleeping often drags the hip and low back into a long, low-grade complaint. The body may tolerate brief twists during the day. Overnight is a different contract.
The problem with stacking random pillows without checking alignment
More pillows do not automatically create more wisdom. I have seen people build a pillow architecture that looked ready for a design magazine and still left the top leg dropping forward. Random stacking can create odd angles, neck strain, or too much elevation through one segment of the leg while leaving the rest unsupported.
The fix is not fewer pillows by principle. It is purposeful pillows. Each pillow should solve a specific problem: reduce pelvic rotation, cushion direct pressure, or support the torso so you are not folding into the mattress like a closing map.
Why “just stay still” can backfire by morning
Some people become so afraid of triggering pain that they try to hold one perfect position all night. That can backfire. Tissues often dislike unbroken stillness, especially when already sensitive. Micro-adjustments are normal and healthy. The goal is not to become a museum statue. The goal is to reduce harmful load, not abolish motion itself.
A better target is fewer pain spikes and easier return to sleep after natural position changes.
Quote-prep list: What to notice before buying any sleep accessory
- Where exactly does the pain start: outer hip, front groin, buttock, low back?
- Does pain worsen more from direct pressure or from the top leg dropping forward?
- Is morning stiffness worse than bedtime pain?
- Do you wake from pain once, or multiple times each night?
Neutral action: Gather these observations first, then decide whether you need a pillow change, surface change, or clinical evaluation.
Mattress, topper, or body position? Fix the right problem first
How to tell whether the pain comes from surface firmness or joint compression
A too-firm surface may increase direct pressure. A too-soft surface may let the body sink and twist. Both can bother the hip, but not in the same way. If the pain feels sharply pressure-based on the outer hip, surface cushioning may matter more. If the pain feels like pulling, rotation, or front-of-hip strain, positioning and support may matter more.
Many people spend money in the wrong category because discomfort and surface feel are easy to confuse. “This bed feels hard” is not the same as “this bed is the main reason my hip hurts.” The hip likes precision. The wallet does too.
Why expensive sleep products can distract from a positioning mistake
The mattress industry is excellent at selling universal promises to highly specific problems. A topper can help. So can a different pillow. But if your pelvis is still rotating and your top leg still dives forward, you may simply be purchasing a softer version of the same mistake. If you are torn between surface changes, a more focused comparison like how to think about 2-inch versus 3-inch mattress topper choices can help keep the experiment grounded.
I remember testing a memory foam topper years ago for shoulder discomfort and discovering that my pain was mostly coming from the way I tucked my arm under the pillow like I was hiding from taxes. The surface was not innocent, but it was not the mastermind either.
A simple way to test one variable at a time
Use a 3-night test when possible. Change one thing only: knee pillow height, added thin topper layer, torso support, or which side you sleep on. Keep the rest the same. Track bedtime pain, night awakenings, and first-hour morning soreness. The body gives clearer answers when you do not interrogate it with 5 questions at once.
| Variable | Best for | Warning sign |
|---|---|---|
| Knee pillow | Top leg drift, pelvic twist | Too soft or too thick |
| Thin topper | Direct outer-hip pressure | Body sinks and twists more |
| Torso support pillow | Waist rotation, slumping | Neck or shoulder feels worse |
Neutral action: Match the tool to the problem. Do not ask a topper to solve a twisting issue or a knee pillow to fix severe pressure from a concrete-like bed.
Here’s the catch: the hip you feel at night may not be the only issue involved
How glute weakness, tightness, or gait changes can show up most loudly in bed
The hip that protests at night may have been collecting grievances all day. Changes in walking pattern, reduced hip strength, protective limping, or tight surrounding muscles can all change how the body lands in bed. By nighttime, the tissue may be less tolerant of pressure or stretch. That makes the bed look guilty when the entire day wrote the script.
Clinicians often talk about load tolerance. It is a useful phrase because it explains why one night feels manageable and the next feels theatrical. Sleep is not separate from the rest of your movement life. It is the final receipt.
Why daytime sitting habits can echo into nighttime pain
Long hours of sitting can leave the hips stiff and the glutes underactive. Then side sleeping asks the hip to tolerate compression and alignment demands it is not ready for. The result is a body that lands in bed already cranky. A short evening walk, standing breaks during the day, or simply reducing long slumped sitting can make night pain less dramatic. The same principle shows up in guides for orthopedic pain management for remote workers, where daytime mechanics quietly set the terms for nighttime comfort.
This does not mean you need a flawless ergonomic life. It means the hip remembers how it was treated at 2 p.m. even if you are trying to negotiate with it at 10:30 p.m.
Here’s what no one tells you… the hip that hurts in bed may be arguing with your back, not working alone
Back-related pain can show up in the hip area, buttock, or outer thigh. If lying down changes the pattern, if the pain radiates, or if numbness and tingling join the ensemble, the story may be broader than the hip alone. That does not mean doom. It means be humble about the map. Pain sometimes wears the wrong name tag. In those cases, it helps to think through the overlap between hip pain versus spine-related pain before assuming the mattress is the entire culprit.
Short Story: A friend once spent months calling something “hip pain” because it appeared only in bed and when rolling over. She bought a new pillow, then a topper, then one of those devices that looks futuristic enough to require its own docking station. What finally changed things was noticing that long days at the laptop made the pain worse, and short walks made nights easier.
A clinician later confirmed the hip was involved, but not alone. The back and pelvic mechanics were part of the quarrel. Nothing dramatic happened overnight. She just stopped fighting the wrong enemy. That is often the quiet turning point: when the body stops being one body part in your mind and becomes a conversation between several.
- Walking pattern, stiffness, and sitting habits can shape bedtime symptoms
- Back-related issues can masquerade as hip pain
- Sleep changes work better when daytime load is also considered
Apply in 60 seconds: Notice whether your worst nights follow long sitting, limping, unusually busy days, or low-back irritation.
Common mistakes people make when managing hip pain as a side sleeper
Changing sleep positions too often to learn what actually helps
Restless experimentation feels proactive and often produces useless data. If you try one side, then the other, then no pillow, then two pillows, then a blanket rolled into a burrito of optimism, you may end the night with no clear lesson. A good test needs repetition.
Treating all hip pain like inflammation when the trigger may be mechanics
People often assume all pain means swelling and all relief means reducing inflammation. But mechanical irritation can be the bigger driver at night. That means alignment, pressure distribution, and movement patterns deserve equal attention. The wrong model leads to the wrong plan. Ice and anti-inflammatory strategies may help some people, but not if twisting and compression are the main culprits.
Waiting until bedtime to respond to pain that has been building all day
This is the classic error of late-stage negotiation. By bedtime, the hip has already tallied your sitting, walking, climbing, carrying, and posture. Waiting until lights-out to solve everything is like trying to learn piano in the 5 minutes before a recital. When conservative care starts to feel confusing or stalled, it can also help to read what to do when physical therapy is not helping orthopedic pain so the next step is based on pattern, not panic.
Mini calculator: how many wake-ups is your setup costing you?
Input 1: average number of pain-related awakenings per night.
Input 2: average minutes needed to fall back asleep.
Multiply them. A person waking 3 times and losing 12 minutes each time loses about 36 minutes of sleep opportunity a night.
Neutral action: Use that number to decide whether a systematic 3-night test is worth doing. It usually is.
Show me the nerdy details
Repeated awakenings matter because symptom severity is not only about peak pain. Sleep fragmentation changes perceived pain, next-day fatigue, and tissue tolerance. Small reductions in night disruption can produce outsized improvement in function.
When side sleeping is still possible, and when temporary change is the smarter move
How to modify side sleeping without giving it up completely
For many people, side sleeping does not need to be abandoned forever. It often just needs stricter rules for a while. That might mean sleeping on the non-painful side with better leg support, using a small towel or thin cushion to reduce direct pressure, or switching sides more deliberately rather than collapsing into whichever position wins the coin toss of exhaustion.
This matters because sleep preference is not trivial. People who strongly prefer side sleeping often sleep worse when forced into unfamiliar positions. A plan that is biomechanically perfect but impossible to maintain at 2 a.m. is not a plan. It is a brochure.
When back sleeping for a short stretch may help reset irritation
If side sleeping keeps reproducing pain despite reasonable adjustments, a temporary stretch of back sleeping may help calm the irritated tissues. Many people tolerate this better with a pillow under the knees. It is not glamorous. It is sometimes effective. Temporary change is not betrayal. It is strategy.
One caution: if back sleeping increases back pain, breathing discomfort, or overall poor sleep, it may not be the right substitute. The goal is not to win a posture contest. It is to reduce irritation while preserving enough sleep to feel human the next day.
The goal is not perfection. It is fewer pain spikes and better recovery
Improvement may look modest at first. Maybe you still notice the hip at bedtime but wake less often. Maybe morning pain drops from an 8 to a 5. Those changes matter. Bodies often improve in gradients, not symphonies.
Coverage tier map for home changes
Tier 1: Pillow alignment and side choice
Tier 2: Pre-bed movement or symptom-settling routine
Tier 3: Surface adjustment such as topper or support tweak
Tier 4: Temporary sleep-position change for 3 to 7 nights
Tier 5: Clinical evaluation when sleep disruption persists or symptoms escalate
Neutral action: Move one tier at a time instead of upgrading your whole bedroom in a single burst of frustration.
When to seek help for hip pain that keeps ruining sleep
Red flags that should not be brushed off as “normal soreness”
Some symptoms deserve prompt evaluation: fever, redness, major swelling, inability to bear weight, recent trauma, rapidly worsening pain, new weakness, numbness, or pain linked to a fall. Night pain that is severe, constant, and not clearly position-related also deserves more caution. A body that will not let you rest is sometimes sending a message more serious than “buy another pillow.”
When nighttime pain points to a bigger functional problem
If you are limping more, avoiding stairs, losing range of motion, or noticing pain during daily activities as well as at night, the issue has moved beyond bedtime technique. Sleep often reveals the problem first, but function tells you how big the problem is becoming.
Trusted institutions like Mayo Clinic and the NHS describe hip pain in ways that reinforce a practical point: persistent symptoms, reduced function, or symptoms that spread beyond one simple pattern should not live forever under the label of “just how I sleep.”
Why pain that wakes you consistently deserves more than pillow experiments
If the pain wakes you multiple nights a week for more than a couple of weeks despite careful changes, it is reasonable to seek professional guidance. Repeated sleep disruption affects pain sensitivity, mood, concentration, and recovery. The hip does not exist in isolation from the rest of your life. It is attached to your patience, your workday, and the way coffee starts looking like a moral necessity. If the next step starts drifting toward imaging questions, a practical piece on what to try before asking for an MRI can help you escalate more thoughtfully.
Infographic: What to change first for side-sleeper hip pain
1. Identify the pattern
Pressure pain, twisting pain, or morning stiffness?
2. Fix alignment
Knee pillow, ankle support, torso support.
3. Fix timing
Pre-bed routine before judging the position.
4. Escalate wisely
Surface changes next. Clinical help if sleep keeps breaking.
FAQ
Why does my hip hurt more at night than during the day?
Night pain often feels worse because pressure stays in one place longer, movement decreases, and tissues that were irritated during the day finally get quiet enough to complain audibly. Less distraction also makes pain more noticeable.
Is it better to sleep on the painful hip or the non-painful side?
For many people, starting on the non-painful side is more comfortable, especially if direct pressure on the sore outer hip is a trigger. But the non-painful side can still create trouble if the top leg drops forward and twists the pelvis. Support matters more than slogans.
Does putting a pillow between the knees really help hip pain?
It can, especially when the main problem is pelvic rotation or the top leg pulling the hip into a strained position. The pillow needs to be supportive enough to change alignment, not merely decorative.
Can a mattress topper reduce side-sleeper hip pain?
Sometimes. A topper may help when direct pressure from a firm surface is the main problem. It is less helpful if the real issue is twisting, poor support, or referred pain from elsewhere. Match the tool to the pattern.
Why is my outside hip sore when I wake up?
Outer-hip soreness in the morning can happen when that area takes too much direct pressure overnight or when surrounding tissues become irritated by prolonged compression and alignment problems. Side sleeping can magnify both.
Could side-sleeping hip pain be bursitis, arthritis, or something else?
Yes. Hip pain can come from several causes, including tendon irritation, bursitis-like irritation around the outer hip, arthritis, referred low-back pain, or post-injury changes. That is why symptom pattern and red flags matter. If the findings feel mixed or the pain story is not lining up neatly, it can also be useful to read about what it can mean when an X-ray looks normal but pain continues.
When should I stop trying home changes and call a doctor?
Seek medical care sooner for red flags like fever, trauma, inability to bear weight, rapidly worsening pain, numbness, or weakness. Even without red flags, it is reasonable to seek help if pain wakes you repeatedly for weeks or function is slipping.
Can back pain cause hip pain only when I lie down?
It can. Some back-related issues refer pain into the hip or buttock area and may become more obvious in certain lying positions. If the pattern includes radiating pain, tingling, numbness, or low-back symptoms, the hip may not be working alone.
Next step: change one variable tonight, not five
Pick one test: knee pillow, side switch, pre-bed routine, or mattress layer
The most useful next step is not a dramatic reinvention of your sleep life. It is one deliberate test. Choose the variable most likely to match your pattern. If the pain feels pressure-based, start with cushioning or side choice. If it feels like twisting, start with the knee pillow and leg support. If the hip feels rigid before bed, start there. Give the body a fair experiment, not a chaotic festival of interventions.
Track what happens in the first 20 minutes and the first hour after waking
These two windows reveal a lot. The first 20 minutes tell you whether the setup reduces immediate irritation. The first hour after waking tells you whether the overnight load was gentler. Those are better metrics than your mood at 2:13 a.m., though that mood may be eloquent.
Small, consistent adjustments beat dramatic bedtime experiments
That is the real answer to the hook. The bed feels like an argument because the hip is reacting to accumulated load, not just one bad pillow or one unlucky night. The quiet win is to reduce the argument’s fuel. Better alignment. Better timing. Less compression. Enough patience to learn what helps.
- Pick the variable that matches your pain pattern
- Track bedtime response and morning aftermath
- Escalate thoughtfully if sleep keeps breaking
Apply in 60 seconds: Choose tonight’s single test now and put the needed pillow or support in place before you get tired.
Last reviewed: 2026-04.
