
The Hidden Drift: Navigating Orthopedic Pain While Living Alone
Pain can make a person look independent long after daily life has started quietly narrowing. An older adult living alone may still sound fine on the phone while avoiding stairs, skipping showers, gripping furniture, or getting a little too foggy after the “helpful” pill that was supposed to make the evening easier.
That is what makes orthopedic pain management for older adults living alone different from ordinary pain advice. The real problem is not just discomfort. It is the hidden collision between pain, mobility, medication safety, sleep disruption, and fall risk inside an everyday home.
Keep guessing too long, and a manageable flare can turn into a fall, a missed dose, a bad night, or a much smaller life.
This post helps readers build a safer pain routine at home, with better pacing, smarter home setup, clearer medication habits, and a backup plan for the rough days. The goal is not to win a medal for toughness. It is to stay steady, functional, and less vulnerable when no one else is there to notice the drift.
Because pain is rarely the whole story. Because “still managing” can hide a lot. And because the safest plan is often less heroic, and far more effective.
Table of Contents

Start Here: What Orthopedic Pain Management Really Means When You Live Alone
Pain relief is only one goal, safety is the other half
When an older adult lives alone, pain is never just pain. It is also a walking problem, a bathroom problem, a kitchen problem, and sometimes a night problem at 2:13 a.m. when the hallway feels longer than usual. That is why good orthopedic pain management has two jobs at once: lower the pain enough to protect function, and protect function enough to prevent a bigger setback.
Many people begin with a single question: “How do I make this hurt less?” Fair question. But in real homes, the more useful version is this: “How do I make this hurt less without becoming dizzier, weaker, more constipated, more groggy, or more likely to fall?” That second question is less glamorous, but it keeps people upright.
Living alone changes the risk math for recovery, mobility, and medication use
Living alone does not automatically mean someone is unsafe. Plenty of older adults run their households with the grace of seasoned stage managers. But it does mean there is less margin for error. A person who feels sedated after a new medication, misses a dose, sleeps poorly for two nights, or starts favoring one leg may not have another pair of eyes there to notice the drift. The CDC says more than one in four older adults falls each year, and less than half tell their doctor. That matters here because pain and fall risk often braid together more tightly than people expect.
Why the same joint pain feels different when no one is there to notice the decline
I have seen this pattern in ordinary domestic scenes. The kettle is moved to a lower shelf. The laundry basket gets smaller. The upstairs room stops being “worth it.” None of those changes announces itself as danger. They look practical, even wise. But together they can form a quiet map of declining function.
The core idea is simple: pain management in a solo household is not about acting brave. It is about designing the day so pain has fewer chances to become a cascade. For a broader companion guide, see orthopedic pain management for older adults.
- Measure success by walking, bathing, sleeping, and transfers, not pain alone
- Assume small changes in routine matter
- Look for patterns, not heroic one-day efforts
Apply in 60 seconds: Write down the three daily tasks pain disrupts most often.
Who This Is For, and Who It Is Not For
This is for older adults managing orthopedic pain at home without daily in-person support
This guide is for the person with knee pain who now times errands around stiffness, the person with back pain who turns getting out of bed into a negotiation, the person with hip pain who says “I’m fine” while quietly using the furniture as a second skeleton. It is also for people recovering from an orthopedic flare, injury, or surgery who have limited hands-on support at home. If someone is in that in-between season before a procedure or formal treatment starts, pain management for seniors waiting on joint care can also be useful.
This is also for adult children, neighbors, and caregivers building a safer routine from a distance
Distance caregiving often fails in predictable ways. Family asks, “How is the pain?” The older adult says, “About the same.” End scene. But “about the same” does not tell you whether the shower was skipped, the medication was confusing, or the trip to the bathroom now takes twice as long. If you support someone from afar, your job is not to become an amateur detective with a flashlight and panic. It is to ask better functional questions.
Try these instead:
- Did you walk less this week because of pain?
- Are you avoiding stairs, showers, or laundry?
- Have you felt unsteady after taking pain medicine?
- Did you miss or double any doses?
- Has getting to the bathroom at night become harder?
This is not a substitute for urgent evaluation, post-surgical instructions, or diagnosis-specific treatment
Orthopedic pain has many causes, and some situations need prompt medical assessment rather than household problem-solving. New inability to bear weight, deformity, fever, sudden severe swelling, new confusion, or chest symptoms do not belong in the “let’s just monitor it” drawer. A home routine can support recovery. It cannot replace clinician guidance, especially after surgery, after a fall, or when symptoms change sharply. When the question is whether something belongs in same-day care or a specialist visit, a guide on urgent care versus an orthopedic clinic can help frame that choice.
- Yes / No: Pain is affecting daily movement at home
- Yes / No: The person lives alone most of the time
- Yes / No: There is some confusion about medication, mobility, or when to call for help
- Yes / No: The goal is safer function, not self-diagnosis
Next step: If you answered yes to two or more, build a written pain-and-safety routine today.
Pain First, Fall Risk Second? That Order Can Backfire
The wrong pain strategy can reduce pain but increase dizziness, weakness, or nighttime instability
Sometimes pain relief succeeds too narrowly. A medication, sleep aid, or improvised routine may lower pain intensity for a few hours while making balance worse, thinking slower, or nighttime walking shakier. In a shared household, someone may notice. In a solo household, the body and the floor become reluctant conversation partners.
The National Institute on Aging warns that mixing medicines or taking them the wrong way can be dangerous in older adults, and notes that some pain medicines can cause side effects that matter greatly for safety. That warning sounds modest on paper, but inside a dim hallway it becomes very concrete.
Why untreated pain also raises fall risk by changing gait, speed, and confidence
Here is the other half of the paradox: undertreated pain is not “the safe option.” Pain changes how people move. They shorten steps, twist awkwardly, avoid putting weight where they should, and rush through tasks they no longer trust themselves to do smoothly. A person in pain may become both slower and more hurried, which is a wonderfully irritating human contradiction.
That means the target is not maximal pain suppression and not stoic endurance. The target is a workable middle: enough relief to move more normally, think clearly, and complete basic tasks safely. Sometimes that also means understanding whether a pain clinic or an orthopedist is the better next stop for the problem in front of you.
Let’s be honest: many people do not fear the pain itself as much as what happens while trying to live around it
Older adults living alone often describe a more specific fear than pain. They fear falling in the bathroom. They fear becoming “foggy.” They fear being unable to get groceries upstairs or answer the door. In other words, they fear the chain reaction. Good pain management respects that fear because it is often rational.
Ask this each day: Is this strategy helping me move more safely, or only making the pain number smaller?
Show me the nerdy details
Pain management works best when clinicians and patients look at both symptom intensity and function. A strategy that improves a pain score but worsens balance, hydration, bowel function, or alertness may be a poor trade in a solo-living situation. Functional markers like transfers, gait, bathroom access, and medication accuracy often tell a more useful story than a single pain number.
Daily Life Friction: Where Orthopedic Pain Gets Worse in a Solo Household
Morning stiffness, bathroom trips, and kitchen tasks often create the first pain spike of the day
Many people imagine pain as a constant block of misery. In real life, it has favorite rooms and favorite hours. Morning is a common ambush. The first steps to the bathroom, the turn toward the sink, the reach into a lower cabinet, the tiny squat to feed a pet, the half-twist while putting on pants, these are classic pain traps.
A retired neighbor once told me her knee was “not that bad, except during ordinary civilization.” By that she meant chairs, toilets, bed edges, and stovetops. She was joking, but only barely.
Sleep disruption can quietly worsen pain tolerance, balance, and mood
Poor sleep lowers patience with pain. It also makes balance, timing, and decision-making duller around the edges. MedlinePlus notes that chronic pain can last longer than three months and affect daily life in a broad way, which is why nighttime pain is never just a nighttime issue. A bad night often arrives at breakfast wearing a different name. When nighttime pain is centered in the hip, some readers may also find hip pain at night helpful for understanding what deserves closer attention.
The danger of “saving up” chores until the body is already tired
Living alone often means batching tasks. Laundry, trash, groceries, dishes, showering, refilling the pill organizer, and changing the sheets all get bundled into a “productive day.” The trouble is that orthopedic pain usually punishes stacked effort. By late afternoon, movement is less controlled, judgment is more impatient, and the temptation to say “I’ll just do one more thing” becomes expensive.
| Approach | When it works | Risk |
|---|---|---|
| One big chore block | Only if pain is mild and endurance is stable | Fatigue, sloppy movement, next-day flare |
| Two to four smaller clusters | Best for most solo households with orthopedic pain | Requires planning and a little patience |
Neutral action: Test one smaller-cluster day this week and compare pain that evening.
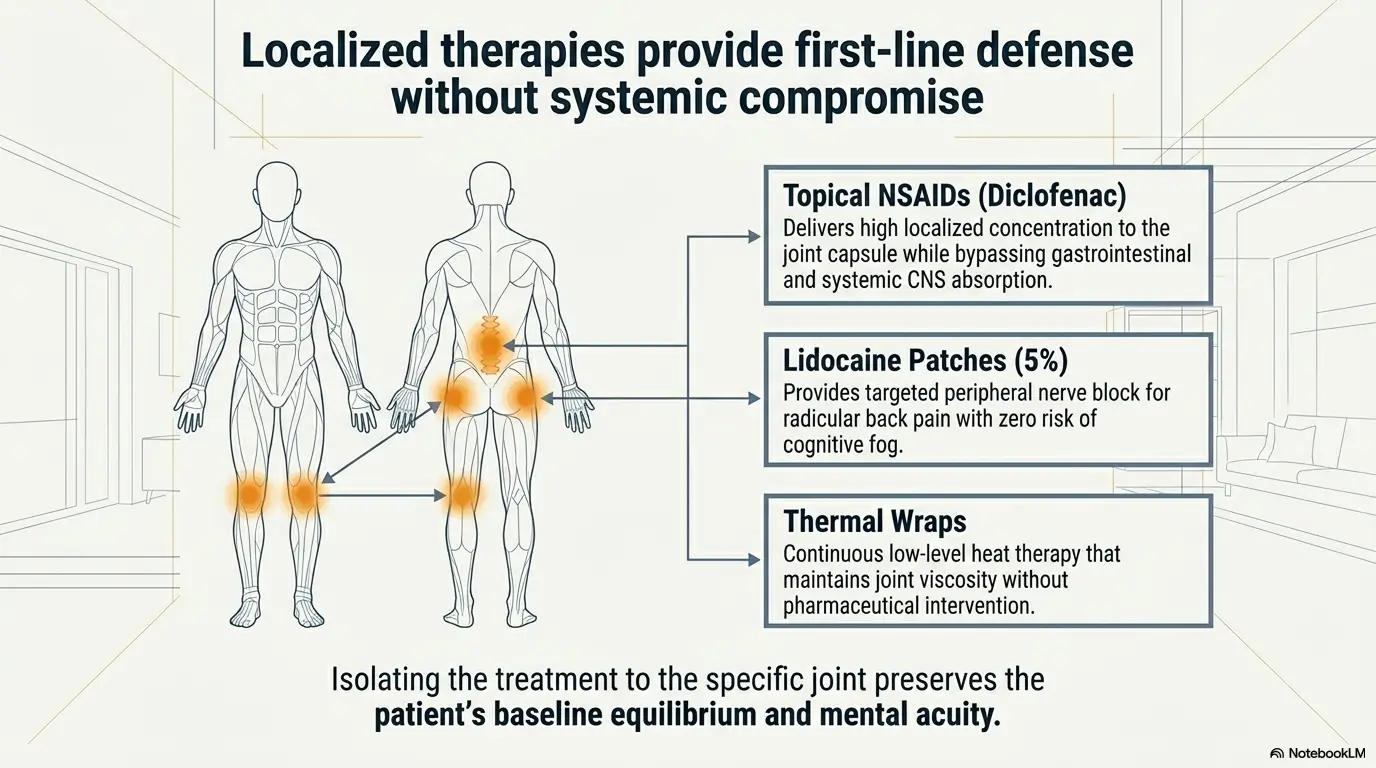
Do Not Build the Day Around Pain Alone
Build around movement windows, energy timing, and medication timing instead
If pain shapes every decision, the day starts to feel like a weather forecast written by a grudge. A better approach is to build around movement windows. Many people have one or two times of day when movement is safer and less guarded. That is when showering, short walks, simple meal prep, and essential errands should happen if possible.
Notice I said if possible. Pain routines should be structured, not militarized. No one needs a domestic drill sergeant in orthopedic shoes.
Why pacing beats the boom-and-bust cycle of good day overuse and bad day collapse
Pacing sounds boring until you compare it with the usual alternative, which is accidental self-sabotage. On a better day, people often do triple the normal activity because they finally can. Then the body sends an invoice the next day. The result is the classic boom-and-bust pattern: one proud productive day followed by a sulking, swollen, stiff day.
A simple pacing frame works better:
- Choose one must-do task
- Choose one helpful-but-optional task
- Stop before movement becomes sloppy or rushed
- Leave something small undone on purpose
Here’s what no one tells you: the worst pain day often begins with yesterday’s “I felt okay, so I did too much”
This is one of the least glamorous truths in pain management. Bad days often do not begin with catastrophe. They begin with confidence. A person walks farther, lifts more, climbs extra stairs, or cleans the whole bathroom because the morning felt decent. By evening, the body has filed an appeal.
- Protect the first 2 to 4 high-value tasks
- Space physically demanding chores
- End activity while control is still good
Apply in 60 seconds: Circle one daily task to move earlier in the day tomorrow.
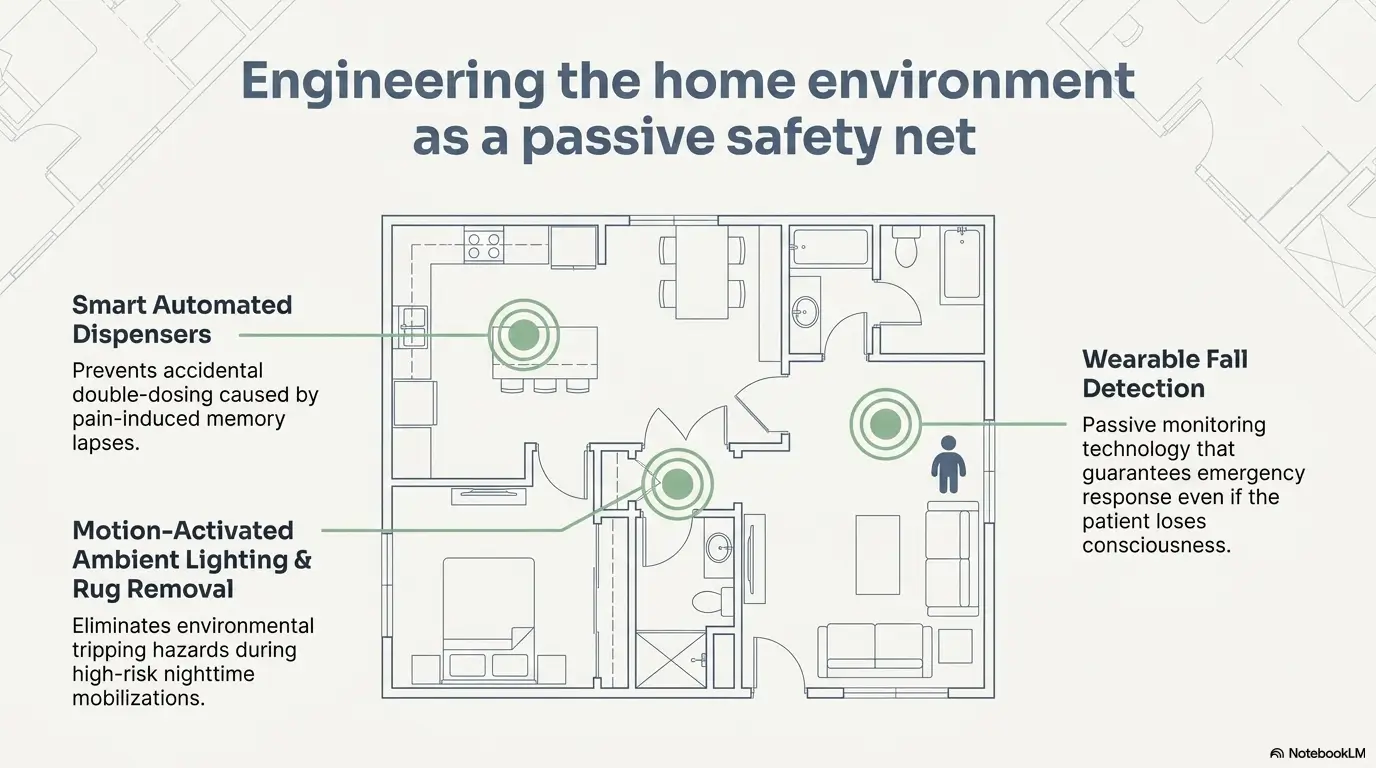
Home Setup Before Heroics: The Environment Can Lower Pain Faster Than Willpower
Chairs, bed height, lighting, and floor clutter shape how painful movement feels
People often treat the home as neutral background, but it is not. It is active equipment. A chair that is too low turns every sit-to-stand into a mini squat. A bed that is too soft makes turning painful and getting up clumsy. Poor lighting steals reaction time. Floor clutter, cords, and rugs add an unnecessary layer of drama. The CDC lists home hazards like clutter and throw rugs among factors that can contribute to falls in older adults.
One of the quickest wins is simply to stop forcing the body through bad geometry. Raised seating, better lighting, and moving frequently used items to waist height can reduce pain before any motivational speech has even tied its shoes.
Support tools only help when they are placed where pain actually interrupts the day
A reacher in the hall closet helps nobody. A grab bar that exists only in theory is a very expensive concept. Support tools work when they are placed at the pain bottleneck itself: the shower entry, the toilet, the bedside, the kitchen prep area, the front step.
Useful environmental supports can include:
- Stable seating with arms
- Night lights along the bathroom path
- Frequently used items stored between shoulder and hip height
- A phone within reach of bed and favorite chair
- Non-slip bath surfaces and thoughtfully placed handholds
Why the bathroom and the path to the bathroom deserve first attention
The bathroom is where pain, urgency, darkness, balance, and pride often meet. Not a charming gathering. A safer bathroom path can reduce night anxiety and lower the chance that a groggy, painful, urgent trip becomes the moment everything changes. For readers dealing with recent hip procedures, practical bathroom logistics in showering after hip surgery may offer useful setup ideas.
- Measure chair and bed height if transfers are hard
- List the three places where support is needed most
- Note any rugs, cords, dim hallways, or slippery surfaces
- Take photos to discuss with family, OT, PT, or clinic staff
Neutral action: Fix the bathroom route before tackling lower-priority rooms.
Medication Mistakes That Happen Quietly When Someone Lives Alone
Skipped doses, doubled doses, and “as-needed” confusion are common trouble spots
Medication errors in solo households are rarely dramatic at first. They are ordinary. A dose is delayed because breakfast ran late. A second dose is taken because pain memory is fuzzier than the pill organizer. A person forgets whether “as needed” meant after walking, before bed, or only on severe days. These are not character flaws. They are systems failures waiting for better systems.
The National Institute on Aging advises older adults to keep track of medicines carefully and notes that taking medicines the wrong way or mixing certain drugs can be dangerous. That matters even more when pain medicine shares the stage with sleep aids, constipation remedies, blood pressure medicines, or other prescriptions.
Side effects matter more when no one else is there to notice sedation, constipation, or confusion
In a shared home, someone might say, “You seem off today.” Alone, that feedback loop can disappear. Sedation may look like fatigue. Mild confusion may look like stress. Constipation may sound unrelated until it worsens pain, appetite, and mobility. The body runs no separate customer service desk for side effects.
Why mixing pain relief with sleep aids can turn one rough night into a bigger safety problem
A rough night tempts people to stack solutions. Pain pill, sleep aid, maybe a second “just this once” decision. That is exactly the kind of improvisation that can lead to morning grogginess, slower reaction time, and unsafe bathroom trips. Medication plans should be reviewed with a clinician or pharmacist, especially when new pain relief is added or nighttime symptoms change. If braces or supports are part of that plan, it may also help to review which braces and supports may be HSA-eligible before buying equipment in a rush.
If the answer is yes to 2 or more questions below, the medication routine needs a safety review:
- Have you missed or doubled a dose in the past 2 weeks?
- Do you feel unsteady, foggy, or extra sleepy after taking pain medicine?
- Are you using pain medicine plus sleep medicine or multiple over-the-counter products?
Output: 0 to 1 yes = keep monitoring carefully. 2 to 3 yes = contact a pharmacist or clinician to review the routine.
Neutral action: Put the current medication list in your wallet and by the bedside.
Movement Matters, But Random Exercise Can Make Things Worse
Gentle orthopedic recovery usually depends on the right type, amount, and timing of movement
Movement matters because stiffness, weakness, and fear can all magnify pain. But random movement is not the same thing as therapeutic movement. A person with knee pain may benefit from one kind of gentle activity and flare badly with another. Someone with back pain may need short frequent motion rather than one ambitious session. This is where clinician guidance, especially from physical therapy or postoperative instructions, earns its keep. If home exercises are stalling or aggravating the problem, what to do when physical therapy is not helping orthopedic pain is worth reading.
Rest pain and movement pain are not always the same message
Some pain eases with gentle movement after the first stiff minutes. Other pain sharpens with load, twisting, or repetition. Some pain says “warm up slowly.” Some pain says “stop and recheck this.” The trick is not to become a heroic interpreter of every twinge. The trick is to notice what patterns repeat, then bring those patterns to the clinician managing the condition.
The goal is not proving toughness, it is protecting function tomorrow
I once heard an older man say, with the dignity of a retired captain, “I’m not going to let my knee boss me around.” Admirable spirit. Terrible strategy. By evening, the knee had in fact chaired the meeting.
A better rule: stop while the movement is still good. If walking becomes limping, if transfers get jerky, if pain starts changing the mechanics of the task, the body is already negotiating from a worse position. And if formal therapy is part of the plan, understanding how Medicare Part B physical therapy coverage works may help people stay consistent instead of stopping early for cost reasons.
Show me the nerdy details
Clinicians often care about movement quality, symptom response, and next-day effect. A brief activity that preserves alignment and control may be helpful; a longer session that creates compensations and delayed flare may not be. For older adults living alone, movement plans should protect function and reduce fall risk, not simply increase effort.
Common Mistakes Older Adults Living Alone Make With Orthopedic Pain
Waiting too long to report a clear change in pain, swelling, weakness, or walking ability
Older adults are often wonderfully stoic and occasionally far too diplomatic with their own symptoms. A clear change in walking, swelling, weakness, or weight-bearing ability should not marinate in silence for a week. Reporting change early is not overreacting. It is maintenance.
Treating every flare as “normal aging” instead of checking the pattern
“It’s just age” is one of the most efficient sentence-stubs ever invented for delaying useful care. Age changes bodies, yes. But sudden changes, one-sided swelling, new instability, marked loss of function, or post-fall pain deserve more than philosophical resignation. Sometimes people need help sorting out what it means when an X-ray looks normal but pain continues rather than assuming nothing important is happening.
Using furniture as a mobility aid instead of using the right support device
This is extremely common. People cruise from counter to table to sofa as if the house were built for hand-over-hand travel. It was not. Furniture moves. Rugs slide. Coffee tables are poor life partners. If a clinician has recommended a cane, walker, brace, or other support, using it consistently is usually safer than improvising with the living room.
Pushing through because asking for help feels harder than hurting
This one is emotional, not merely practical. Some people would rather ache than inconvenience anyone. They would rather carry the laundry badly than ask a neighbor to move it safely. That impulse is understandable and, in many cases, expensive.
- Report meaningful changes early
- Do not substitute furniture for proper mobility support
- Treat “I can manage” as a question, not a conclusion
Apply in 60 seconds: Identify one task you should stop doing alone until it feels safer.
Do Not Treat “Still Managing” as the Same Thing as “Doing Fine”
Independence can hide decline when routines get smaller and smaller
One of the hardest truths in solo living is that independence can hide deterioration beautifully. No one sees that the upstairs room is no longer used. No one notices that shopping now happens only once every two weeks because stairs hurt. No one sees the shower schedule becoming strategic, then optional, then negotiable.
That is why function matters more than image. Someone can still sound sharp on the phone, keep a tidy sentence, and be losing ground inside the day.
Reduced walking, skipped bathing, simpler meals, and missed errands are functional warning signs
Think of pain management as preserving life-space. If pain is steadily shrinking where a person goes, how often they bathe, what meals they can prepare, or whether they attend appointments, the issue is no longer “pain control” in a narrow sense. It is a function problem with safety consequences.
Why shrinking your life to match pain is not the same as managing pain well
People often adapt brilliantly. They sit more. Cook less. Climb stairs less. Leave the house less. Use fewer dishes. Skip the walk. They survive by subtraction. But subtraction is not the same as recovery, and it is not always the same as safety either. Less walking can mean more stiffness. Less cooking can mean worse nutrition. Less bathing can mean other health issues brewing quietly in the wings.
| Tier | What it looks like |
|---|---|
| Tier 1 | Pain is present, but routines stay mostly intact |
| Tier 2 | Tasks take longer; pacing becomes necessary |
| Tier 3 | Some rooms, errands, or chores are avoided |
| Tier 4 | Bathing, meals, meds, or follow-ups become inconsistent |
| Tier 5 | Safety is threatened; urgent reassessment is needed |
Neutral action: Mark your current tier honestly and share it at the next appointment.
Build a Backup Plan Before the Bad Day Arrives
A pain plan should include check-ins, refill timing, transportation backup, and emergency contacts
Good backup plans are gloriously unromantic. They do not wait for inspiration. They answer dull, important questions in advance. Who can drive if walking becomes unsafe? Who can pick up a prescription? What happens if pain spikes on a Sunday? Who gets called if a dose is missed and confusion follows?
The older adults who weather rough patches best are not always the toughest. Often, they are the best pre-planners. They have the phone numbers written down, the refill calendar visible, the walker where it belongs, and one person who knows that silence sometimes means trouble. If specialist access is moving slowly, it can also help to understand typical orthopedic referral wait times so the backup plan is realistic instead of wishful.
When to arrange help for groceries, bathing, laundry, or follow-up visits
Help should not wait until crisis if the warning signs are already visible. If pain is clearly interfering with bathing, laundry, meal prep, stairs, or appointments, bringing in short-term support can prevent a larger setback. This is not “giving up independence.” It is protecting it with better scaffolding.
Small systems reduce panic when pain suddenly spikes at night or on weekends
A written plan lowers cognitive load when pain is loud. On bad days, even small decisions feel oddly slippery. A one-page backup plan can include medication list, clinic numbers, emergency contact, mobility device location, pharmacy number, transportation options, and which symptoms mean “call now.” For some people, especially when travel is difficult, it may also help to weigh telehealth versus in-person orthopedics before the next flare arrives.
Short Story: A woman in her late seventies kept insisting she did not need help because she could still “manage the essentials.” Then one rainy Friday her hip pain flared after a long grocery trip. Nothing dramatic happened. That was the problem. She spent the whole weekend doing tiny workarounds: sleeping in the recliner because bed transfers hurt, skipping a full shower because the tub edge felt risky, eating crackers and tea because standing at the stove was too much, and delaying her medication refill because the pharmacy line seemed impossible.
By Monday she was more swollen, more tired, mildly constipated, and angrier at herself than at the pain. What changed things was not a miracle treatment. It was a list on the refrigerator: one backup driver, one grocery helper, one pharmacy contact, one rule about when to call the clinic, and one promise not to wait until Friday afternoon to need everyone at once.
When to Seek Help
New inability to bear weight, marked swelling, deformity, or sudden severe pain needs prompt evaluation
These are not “watch and see for a week” symptoms. A sudden major change in function, load-bearing, shape, or swelling needs medical attention. After a fall, new pain with clearly changed mobility also deserves more respect than the phrase “just soreness” usually receives.
Fever, redness, worsening confusion, chest symptoms, or medication reactions should not be brushed aside
If pain management comes with fever, spreading redness, significant confusion, breathing symptoms, chest symptoms, or signs of a bad medication reaction, it has moved out of the ordinary home-management lane. Seek prompt medical guidance.
Post-fall pain is not “just soreness” when mobility has clearly changed afterward
Falls deserve a low threshold for reassessment, especially in older adults. The CDC emphasizes that falling once doubles the chance of falling again, which is another reason a new fall should trigger a practical review of pain, mobility, environment, and follow-up needs rather than a quick shrug and a cup of tea. Tea is lovely. It is not a fall plan.
Which task hurts most: bed, toilet, stairs, shower, kitchen, or walking?
Improve lighting, clear clutter, move essentials, and place supports where the task fails.
Use the best movement window. Split chores. Avoid late-day stacking.
New inability to bear weight, severe swelling, confusion, fever, or post-fall change means call.
Use it this way: Pick one trigger, one route, one schedule fix, and one emergency contact today.
- Write down red flags before you need them
- Choose one backup helper for logistics
- Review meds and mobility after any fall or major change
Apply in 60 seconds: Put one emergency contact and one clinic number on the refrigerator.
FAQ
What is the safest orthopedic pain management approach for an older adult living alone?
The safest approach is usually a combined plan: clinician-guided pain treatment, a simpler home setup, pacing, symptom tracking, and a written backup plan. The goal is not just less pain. The goal is safer walking, transfers, bathing, sleep, and medication use.
When does joint pain become serious enough to call a doctor?
Call sooner when pain clearly changes from the usual pattern, especially with new inability to bear weight, marked swelling, deformity, fever, redness, major weakness, new confusion, or a fall followed by worse mobility. A meaningful change in function matters even if the pain number alone does not sound dramatic.
Is it better to rest or keep moving with orthopedic pain?
Usually neither extreme works well. Total rest can increase stiffness and deconditioning, while random or excessive activity can worsen pain and mechanics. Many older adults do best with clinician-guided gentle movement, shorter task clusters, and stopping before movement quality falls apart.
How can an older adult living alone reduce pain at night without increasing fall risk?
Night safety often improves with a clearer bathroom route, better lighting, a phone within reach, carefully reviewed medications, and avoiding risky improvisation with sleep aids or extra doses. If nighttime pain is new or escalating, report it to the clinician managing the condition.
What home changes help most with orthopedic pain and mobility problems?
High-value changes often include better lighting, reduced clutter, safer bathroom access, more supportive chair height, moving frequently used items to easier reach, and placing mobility supports exactly where tasks become difficult. Start with the bathroom and the path to it.
What medication problems are most common for seniors managing pain alone?
Common problems include missed doses, accidental double doses, confusion about “as needed” instructions, combining products without review, and not recognizing side effects like sedation, constipation, or confusion quickly enough. A visible medication list and pharmacist review can help.
How do you know whether pain is getting worse or daily function is getting smaller?
Track function directly. Ask whether walking distance, bathing, meal prep, sleep, stairs, errands, and transfers are becoming harder or less frequent. Sometimes the pain feels “about the same” while life has quietly become much smaller.
When should family members worry about an older parent who says they are “fine”?
Worry more when routines shrink: fewer showers, fewer outings, more skipped errands, simplified meals, delayed refills, furniture used for support, or reluctance to discuss falls, dizziness, or medication confusion. “Fine” should be tested against function, not tone of voice.
Next Step: Make One Small Safety Map Today
Write down three pain-trigger moments, three fall-risk spots at home, and one person to contact if pain suddenly worsens
Here is the honest closing loop: the point was never to build a perfect life around pain. The point was to keep pain from quietly reducing the life that is still very much yours. In the beginning, I mentioned the tiny decisions pain starts making for people. This is how you take some of those decisions back.
Do not start with twelve changes. Start with one page. Write down three moments when pain tends to spike, three places in the home that feel least safe, your current medication list, and one person you can contact if symptoms suddenly worsen. Bring that page to the next clinic visit. It will give the conversation more traction than vague memories and brave-sounding understatements. When the next appointment involves imaging questions, some people also benefit from reading orthopedic pain management before asking for an MRI so the conversation stays practical and focused.
If you have 15 minutes today, use them well:
- Clear one risky path
- Move one frequently used item to easier reach
- Write one emergency contact where it can be seen
- Note one symptom change you have been minimizing
The best pain plan is rarely the fanciest. Usually, it is the one that makes tomorrow morning less precarious than this morning was. And for readers recovering after a major knee procedure, a separate guide to knee replacement pain management may be the more specific next read.
Last reviewed: 2026-04.
Safety / Disclaimer
This article is educational and practical. It is not a diagnosis, a medication dosing guide, or a substitute for professional medical care. Orthopedic pain in older adults can have many causes, and management should follow the guidance of the treating clinician, especially after surgery, after a fall, or when pain, swelling, weight-bearing ability, or mental status changes suddenly. Urgent or emergency symptoms deserve prompt medical evaluation.
