
From Holding On to Moving Forward:
A Proactive Guide to the Surgical Wait
The hardest part of waiting for joint replacement is not always the bad knee or aching hip. It is the daily math: walk enough to stay strong, rest enough to avoid a flare, and somehow make it to the bathroom at night without turning the hallway into an obstacle course.
Don’t let the wait quietly steal your strength, sleep, or confidence. This guide transforms your waiting period into a strategic pre-surgery plan, focusing on:
- ✓ Smarter medication questions & gentler pacing
- ✓ Fall-risk checks & home setup fixes
- ✓ A 7-day pain-and-function snapshot for your care team
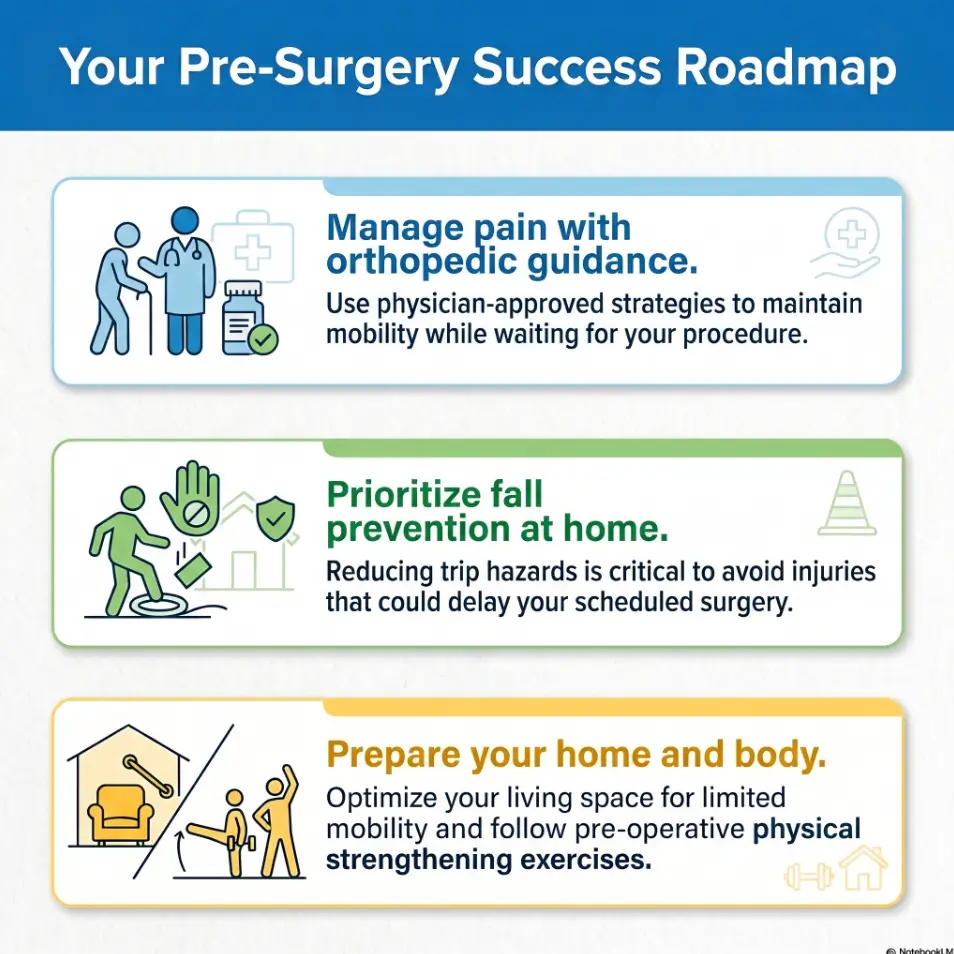
The Strategy
Start the pattern. • Lower the risk. • Inform the experts.
The goal is not to be heroic before surgery.
The goal is to arrive safer, steadier, and less worn down.
Table of Contents
Start Here: The Waiting Period Is Part of the Treatment Plan
Why “just get through it” can quietly make recovery harder
Waiting for hip or knee replacement can feel like standing in a long hallway with a locked door at the end. You know help is coming, but today still has stairs, laundry, groceries, showers, and that rude little trip from the bed to the bathroom at 2:13 a.m.
The mistake is treating the waiting period as empty time. It is not empty. It is where strength can be protected, fall risk can be lowered, sleep can be defended, and the home can be made less hostile to a painful joint.
I once watched a family spend 40 minutes debating which recliner to buy, then step over a curled hallway rug three times during the conversation. That is the waiting-period problem in miniature: we often chase the big purchase while ignoring the small hazard waiting like a banana peel with upholstery.
The real goal is safer function, not perfect pain control
Perfect pain control may not be realistic before surgery. Safer function usually is. That means asking a better question: Can the person still move through the day without creating a bigger risk?
- Can they reach the bathroom safely at night?
- Can they shower without rushing or twisting?
- Can they eat without standing at the counter too long?
- Can they take medicine correctly without doubling up?
- Can they walk enough to preserve confidence?
What changes when surgery is weeks or months away
If surgery is next week, the priority may be final instructions, skin prep, transport, and recovery logistics. If surgery is 2 or 3 months away, the priority shifts. The plan needs rhythm: medication review, pacing, gentle movement, home preparation, and earlier reporting of changes.
- Protect walking ability.
- Lower fall hazards.
- Track changes before they become crises.
Apply in 60 seconds: Write down the one daily movement that hurts most: standing, walking, stairs, showering, or getting into bed.
Who This Is For, and Who It Is Not For
For seniors waiting on hip or knee replacement with daily pain
This guide is for older adults living with hip or knee arthritis pain while waiting for joint replacement. Some are using a cane. Some are pretending they do not need a cane. Some have a freezer full of ice packs and the patience of a saint with a parking ticket.
It is also for people who feel stuck between two bad options: move and hurt, or rest and get weaker. The safer middle path is usually built from small decisions repeated daily.
For adult children trying to help without taking over
Adult children and spouses often want to help, but the line between support and command can get blurry fast. “Did you take your medicine?” can sound caring on Monday and like a parole check by Friday.
A better approach is to ask about function. Function is less accusatory and more revealing. Instead of “How bad is your pain?” ask, “Was the bathroom harder last night?” or “Did you skip anything today because standing hurt?”
Not for sudden injury, infection signs, or unexplained severe symptoms
This is not a substitute for urgent medical care. Sudden severe swelling, fever, chest pain, fainting, new confusion, a fall with injury, or new weakness should not be filed under “arthritis being dramatic.” Those symptoms need prompt medical attention.
Not for medication changes without a prescribing clinician
Medication decisions before surgery can be complicated. Some medicines affect bleeding risk, blood pressure, sedation, kidney function, stomach irritation, constipation, or interactions with anesthesia. Even over-the-counter pills can matter.
- Yes if pain is chronic arthritis-related and surgery is already being discussed or scheduled.
- Yes if the main concern is safer daily function while waiting.
- No if symptoms are sudden, severe, unexplained, or linked with fever, confusion, chest pain, or fainting.
- No if you are looking for personal medication instructions.
Neutral action: If any “No” item fits, contact the care team or urgent services rather than trying to solve it with home tactics.
Pain Patterns First: Know When the Joint Usually Betrays You
Morning stiffness, first steps, and the “rusty hinge” window
Many painful joints have a daily personality. Some are crankiest in the morning. The first 5 to 20 minutes can feel like the body has opened for business before the lights are on.
This is where a routine helps. Sit up. Let the feet settle. Stand with support. Take the first few steps without carrying laundry, a coffee mug, or the entire emotional burden of Western civilization.
Late-day pain after errands, chores, or too much standing
Late-day pain often tells the story of the afternoon. A senior may say, “I did nothing,” but “nothing” included standing at the sink, walking through a store, carrying groceries, feeding the dog, and moving a chair that should have stayed right where it was.
The joint does not care whether the activity was meaningful. It counts load, repetition, stairs, twisting, and standing time.
Night pain that turns the bed into a negotiation table
Night pain can make every pillow arrangement feel like a diplomatic summit. Hip pain may object to side sleeping. Knee pain may complain about full extension. Back pain may join the meeting uninvited.
Instead of changing 12 things at once, note what changed during the day. Was there more walking? Less rest? New medicine timing? A missed meal? More stairs? The bed may be reporting an earlier decision, especially when hip pain at night keeps rewriting the sleep plan.
The pain diary that actually helps the surgeon
A useful pain diary is short. Nobody needs a Victorian novel about Tuesday’s knee. Track 4 items for 7 days:
- Hardest movement of the day
- Best pain-control method used
- Any stumble, dizziness, missed dose, or near-fall
- Any skipped activity, such as showering, cooking, or walking outside
Before-Surgery Safety Loop
When does the joint flare: morning, errands, stairs, or night?
What gets skipped: shower, meals, walking, laundry, sleep?
Any dizziness, near-falls, extra doses, or unsafe rushing?
Adjust pacing, home setup, support, or clinician questions.
Medication Safety: Relief Can Come With a Fall Risk
Why seniors should review every pain medicine before surgery
Pain relief is not automatically safer just because it reduces pain. For older adults, a medicine that dulls pain may also increase dizziness, sleepiness, constipation, confusion, blood pressure drops, or unsteady walking.
The CDC emphasizes that falls can be prevented with risk-reduction steps, and medication review is one of the practical conversations many clinicians use when fall risk is part of the picture. The quiet danger is not one dramatic mistake. It is the small pileup: a pain pill, poor sleep, dehydration, a dark hallway, and slippers that gave up in 2019.
NSAIDs, opioids, sleep aids, and blood pressure dips
Older adults waiting for surgery may be using prescription medications, over-the-counter pain relievers, topical products, sleep aids, or supplements. Each category can have trade-offs. Some can affect bleeding risk. Some can irritate the stomach. Some may interact with blood pressure medicine. Some can make nighttime bathroom trips more dangerous.
Do not change the plan alone. Ask the surgeon, primary care clinician, or pharmacist what is safe before surgery and what should be avoided close to the operation date.
Don’t stack “small” medicines like they are harmless
One extra pill can feel small. One “PM” product can feel harmless. One supplement can seem natural enough to float in wearing linen. But bodies do not read marketing labels. They process ingredients.
A medication list should include prescriptions, over-the-counter drugs, creams, patches, vitamins, supplements, and sleep products. Bring the bottles or take clear photos of the labels.
Let’s be honest: “I only took one extra” still matters
People often underreport extra doses because they feel embarrassed. But clinicians are not there to scold. They need the truth because surgery, anesthesia, bleeding risk, constipation, falls, and pain control all live in the same crowded apartment.
- Prescription pain medicines and dose schedule
- Over-the-counter pain relievers and sleep aids
- Supplements, vitamins, creams, patches, and herbal products
- Any dizziness, constipation, confusion, falls, or near-falls
- Questions about what to stop before surgery and when
Neutral action: Put everything in one bag or one phone album before the next appointment.
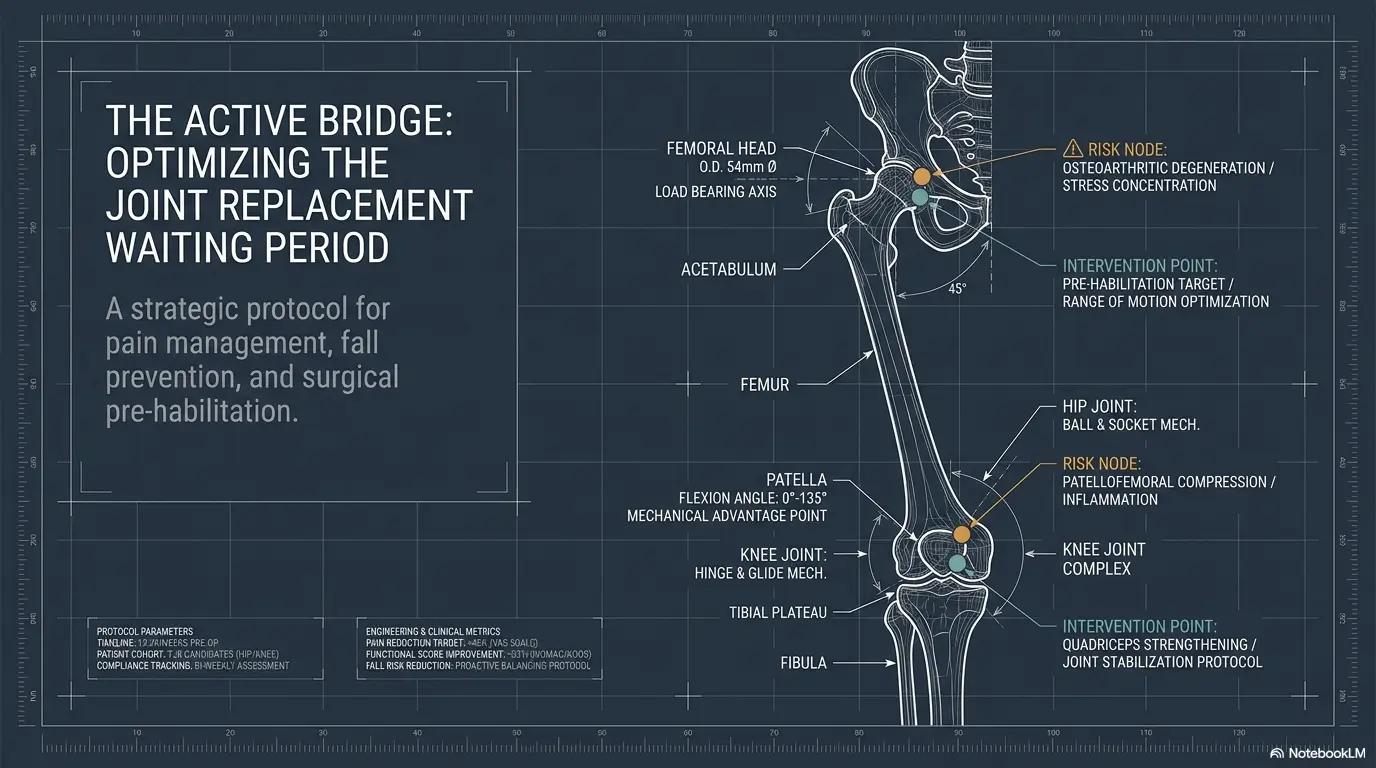
Movement Windows: Use the Best Hours, Don’t Worship the Clock
Why one long chore block can punish the joint later
A painful joint may tolerate 10 minutes of standing, then object to 35. That does not mean the person is lazy. It means the joint has a load budget, and the household keeps trying to pay with a declined card.
One of the biggest waiting-period mistakes is saving chores for a “good” day. The day begins with hope, then becomes laundry, dishes, groceries, clean sheets, and “while I’m up…” By evening, the joint has written a strongly worded letter.
How to pair pain relief timing with walking, bathing, and meals
Some seniors have better movement windows after breakfast, after prescribed medication has had time to work, or after a warm shower. Others do better late morning. The point is not to obey a perfect schedule. The point is to notice when movement is safest.
Pair higher-risk tasks with better windows:
- Shower during the steadiest part of the day, not when exhausted.
- Prepare meals before late-day pain peaks.
- Walk short distances before stiffness returns.
- Place rest breaks between errands, not after the whole parade.
The 10-minute reset between tasks
A 10-minute reset is not surrender. It is maintenance. Sit. Hydrate. Check pain. Let the joint calm down before the next task. This tiny pause can prevent the “I was fine until suddenly I was not fine” spiral.
Here’s what no one tells you: stopping early is a skill
Stopping before pain becomes loud is hard because it feels wasteful. But seniors waiting on surgery are not training for a trophy in countertop endurance. They are preserving function for tomorrow.
Feels efficient, but may trigger late-day pain, swelling, limping, or a risky nighttime bathroom trip.
Uses shorter bursts with rest between. Less heroic, often safer, and easier to repeat.
Neutral action: Break tomorrow’s hardest chore into 2 or 3 smaller pieces before starting.
Exercise Without Bravado: Keep Strength Without Starting a Flare
Why gentle movement may matter more than rest-only coping
When pain is persistent, rest can feel sensible. And sometimes rest is needed. But rest-only coping can quietly shrink the day: fewer walks, weaker legs, less confidence, more fear, and eventually a chair that starts acting like a tiny island.
The American College of Rheumatology and Arthritis Foundation guideline strongly supports exercise and self-management for osteoarthritis care, with treatment choices made through shared decision-making. That does not mean every exercise is right for every person. It means movement belongs in the conversation.
Ask about safe prehab before the operation date
“Prehab” simply means preparing the body before surgery. It may include safe strengthening, walking, flexibility, balance, breathing practice, or education. A physical therapist can help match exercises to the joint, pain level, balance, and surgical plan.
I have seen one-page exercise handouts become fridge decorations because the routine was too long. A better starter question is: “What are the 2 or 3 safest exercises I should prioritize until surgery?” If the current plan feels stuck, it may help to ask what to review when physical therapy is not helping orthopedic pain the way everyone hoped.
Chair-based strength, short walks, and balance work
For some seniors, a safe plan may include chair-based movements, short walks, gentle range-of-motion work, or balance practice near a sturdy support. For others, pain, heart conditions, dizziness, or nerve symptoms may require a more supervised approach.
When exercise pain means “pause and call,” not “push harder”
Discomfort and danger are not the same thing. But new sharp pain, sudden swelling, new weakness, numbness, fever, chest pain, or pain that changes walking significantly should not be pushed through.
Show me the nerdy details
Useful pre-surgery movement planning often tracks function rather than just pain intensity. For example: sit-to-stand ability, safe walking distance, stair tolerance, nighttime bathroom safety, and whether pain changes the person’s gait. These markers help clinicians understand whether the plan is protecting independence or merely masking symptoms.
- Ask for clinician-approved prehab.
- Favor consistency over intensity.
- Stop and report concerning changes.
Apply in 60 seconds: Write one question for your clinician: “Which movements should I protect, and which should I avoid until surgery?”
Walking Aids: The Cane or Walker Is Not a Defeat
Why the right device can protect the painful joint and the good one
A cane or walker is not a public announcement that independence has expired. It is a tool. The right tool can reduce strain, improve confidence, and make the home less like an obstacle course designed by a bored raccoon.
The danger is waiting too long. Some people will limp for months rather than use a cane for 2 weeks. Pride is understandable. Falling is less romantic.
The hidden danger of borrowing equipment that does not fit
Borrowed equipment often comes with borrowed problems. A cane from a taller neighbor, a walker from the garage, or crutches last used during the Clinton administration may not fit the person’s height, hand strength, balance, or home layout.
Assistive devices should be fitted and taught properly. Wrong height or wrong technique can strain the shoulder, wrist, back, or the “good” leg.
How hallway turns, thresholds, and rugs change the safety math
A walking aid that works beautifully in a clinic hallway may behave differently at home. Tight bathroom turns, raised thresholds, loose rugs, pets, cords, and narrow kitchen paths all change the safety math.
Don’t wait for a fall to “earn” a mobility aid
A near-fall is already useful data. Reaching for walls, furniture-walking, avoiding rooms, or feeling unsafe on turns are all signs to ask about a cane, walker, physical therapy, or home modifications. If stairs are part of the daily problem, a discussion about a hinged knee brace for stairs may also belong on the clinician question list.
Count how many are true this week:
- You touched furniture or walls to steady yourself.
- You avoided stairs, showering, or errands because walking felt unsafe.
- You had a stumble, near-fall, or dizziness episode.
Output: If 1 item is true, mention it at the next visit. If 2 or more are true, call sooner and ask whether a device, fitting, or physical therapy evaluation is appropriate.
Neutral action: Do the count tonight and write the result in your 7-day snapshot.
Home Setup: Make the House Kinder Before Surgery
Bathroom first: where pain, water, and balance collide
The bathroom is often the highest-stakes room because it combines water, hard surfaces, turning, stepping, reaching, and privacy. Privacy is lovely. Privacy plus dizziness is less lovely.
Before surgery, ask whether grab bars, a shower chair, nonslip surfaces, raised toilet options, or a handheld showerhead make sense. Do not install random gadgets just because the internet shouted. Buy for the repeated hard movement, especially if showering after hip surgery is already part of the recovery conversation.
Bed height, chair height, and the painful sit-to-stand moment
Sit-to-stand is one of the great hidden pain events. A chair that is too low can turn standing into a wrestling match. A bed that is too high or too low can make nighttime movement less safe.
Test the main chair and bed before surgery. Can the person stand without rocking 3 times? Can they place both feet flat? Is there a sturdy armrest? Is the path clear?
Kitchen shortcuts that prevent standing marathons
The kitchen can quietly punish a painful joint. Standing to chop, cook, wash, and clean may create more load than a short walk. Use a stool if approved and safe, prep simple meals, move frequently used items to waist height, and stop treating the top cabinet like a character test.
The one-room recovery rehearsal before the hospital calls
Do a one-room rehearsal. Choose the room where the person will spend most recovery time. Place phone, charger, water, medications, tissues, glasses, light, walking aid, and instructions within easy reach.
Short Story: The Rug That Lost Its Job
A daughter once told me her father refused every “senior safety” suggestion because the phrase made him feel old. So they stopped calling it safety. They called it surgery prep. Together they moved one rug, raised one lamp, placed a chair near the entry, and put a basket beside his recliner for glasses, remote, and medication notes.
He grumbled for 12 minutes, then admitted the room felt easier. The rug was rolled up in the garage, looking offended but unemployed. Two weeks later, he said the best change was not the equipment. It was not having to think so hard every time he stood up. That is the point of home setup: fewer tiny negotiations with gravity.
- Start with bathroom safety.
- Fix sit-to-stand trouble.
- Rehearse the recovery room before surgery.
Apply in 60 seconds: Walk the route from bed to bathroom and remove one trip hazard today.
Sleep Protection: Pain Feels Louder After Bad Nights
Why night pain can distort daytime decisions
Poor sleep makes pain feel louder. It also makes balance, mood, patience, and decision-making wobblier. A senior who slept 3 broken hours may be more likely to skip breakfast, rush a bathroom trip, take medicine incorrectly, or decide the walker is “too much trouble.”
Sleep protection is not a luxury before joint replacement. It is part of safety planning.
Pillow positioning questions to ask before improvising
Some people find relief with pillows between the knees, under the knee, behind the back, or supporting the operated-side plan after surgery. But positioning advice may differ for hip versus knee problems and before versus after surgery. For people who sleep on their side, side sleeper hip pain relief may require a different setup than daytime walking pain.
Ask the care team what positions are safe now and what will change after the procedure. Improvising with six pillows can turn the bed into a fabric swamp.
Safer nighttime bathroom routes for stiff joints
Night routes should be boring. Boring is beautiful. Use clear paths, reachable lights, sturdy footwear, and a walking aid placed where it can be used before the first step.
Do not store the cane across the room like a museum exhibit. It needs to be where the body needs it.
The midnight mistake: rushing before the legs are awake
After lying down, stiff joints and sleepy blood pressure can make the first minute risky. Sit at the edge of the bed. Turn on the light. Let the body arrive before the walking begins.
Common Mistakes: What Makes the Waiting Period Riskier
Mistake 1: saving all chores for one “good” day
A good day is not a blank check. It is a chance to do the right amount, not all the amount. Seniors often overdo it because they feel guilty, hopeful, or tired of asking for help.
Try this instead: choose 1 priority chore, 1 optional chore, and 1 rest window. The rest window is not negotiable. Put it on the day like an appointment with gravity’s supervisor.
Mistake 2: using stronger medicine to preserve an unsafe routine
If medicine is being used mainly to keep an unsafe routine alive, the routine needs review. Pain control should help a person function safely, not power through a setup that is already too demanding.
Mistake 3: ignoring new swelling, redness, fever, or weakness
Do not assume every new symptom is ordinary arthritis. New swelling, redness, fever, sudden weakness, or major functional change deserves attention. Older adults sometimes underreport symptoms because they do not want to “make a fuss.” Health problems do not become smaller because they were politely ignored.
Mistake 4: waiting too long to ask about cancellations or earlier dates
If pain is worsening or function is dropping, ask the surgeon’s office whether a cancellation list exists and what changes should trigger a call. The answer may be “no earlier date,” but asking gives the team better information. For many families, understanding orthopedic referral wait times can also make the waiting period feel less like a locked room and more like a process with questions to ask.
Mistake 5: assuming pain alone is the only problem
Pain matters. But the bigger picture includes sleep, appetite, walking, bathing, stairs, mood, medication side effects, and caregiver strain. A pain score of 6 means less than: “I stopped showering because I am afraid I will fall.”
- Tier 1: Pain is stable; daily function mostly intact. Keep tracking and pacing.
- Tier 2: Chores or errands are shrinking. Ask about prehab, equipment, and task changes.
- Tier 3: Near-falls, skipped showers, or nighttime trouble appear. Call the care team for a safety review.
- Tier 4: New weakness, sudden swelling, fever, confusion, fainting, or fall occurs. Seek prompt medical guidance.
- Tier 5: Chest pain, severe shortness of breath, severe injury, or dangerous confusion. Use emergency services.
Neutral action: Circle the tier that best describes this week and share it with the person helping coordinate care.
When to Seek Help: Red Flags Seniors Should Not Sleep On
Call the surgeon or clinician for worsening pain that changes function
Call when pain changes what the person can safely do. That may include new inability to walk usual distances, sudden difficulty with stairs, skipped meals because standing hurts, or needing much more help than last week.
Seek urgent help for fever, sudden severe swelling, chest pain, or confusion
Fever, sudden severe swelling, chest pain, severe shortness of breath, fainting, or new confusion should not wait for a routine appointment. These can signal problems beyond ordinary joint pain.
Treat new falls, fainting, or medication-related dizziness as serious
A fall is not just “one of those things.” The CDC states that falls are a threat to older adults’ independence, but they are not inevitable and can often be reduced through practical prevention steps.
Report new numbness, weakness, or loss of bladder or bowel control promptly
New numbness, weakness, or loss of bladder or bowel control deserves prompt medical attention. It may not be related to the joint at all, which is exactly why it should be reported.
- Report sudden changes.
- Take falls and fainting seriously.
- Do not hide extra doses or dizziness.
Apply in 60 seconds: Save the surgeon’s office number and after-hours instructions in the phone today.
Questions to Ask Before Surgery Day Gets Close
What pain medicines are safe for me until surgery?
Ask specifically about prescription medicines, over-the-counter products, topical treatments, supplements, and sleep aids. Also ask when each should be stopped before surgery, if applicable.
Should I use ice, heat, topical medicine, injections, or physical therapy?
These options are not interchangeable. What helps one person may be unsafe or unhelpful for another. Ask what fits your joint, health history, surgery timing, and current medication list. If injections are being discussed, ask what should happen before a cortisone injection rather than treating it as a simple calendar item.
Which activities should I limit, and which should I protect?
This is one of the most useful questions. Many people only ask, “What should I avoid?” Add the second half: “What should I keep doing so I do not lose strength?”
What should I do if pain suddenly worsens before my date?
Ask for a plan before the bad day arrives. Who should you call? What symptoms matter? When should you use urgent care? What information should you report?
Who should I call after hours?
After-hours instructions prevent panic. They also prevent the classic family group text where six people answer with seven opinions and one cousin recommends turmeric with the confidence of a minor prophet.
What home equipment should I arrange now?
The American Academy of Orthopaedic Surgeons explains that people often need several weeks to prepare physically and emotionally before joint replacement. Home preparation may include removing loose rugs or cords, placing frequently used items within reach, planning help, and setting up safer spaces.
- Bring the medication list or bottle photos.
- Bring the 7-day pain-and-function snapshot.
- Ask what symptoms should trigger a call.
- Ask what equipment should be arranged before surgery.
- Ask who to contact after hours.
Neutral action: Print or screenshot this list before the next visit.
FAQ
What can seniors do for joint pain while waiting for replacement?
Seniors can focus on clinician-approved medication, pacing, gentle movement, assistive devices, sleep protection, and fall prevention. The safest plan usually combines several small supports rather than relying on one stronger pain solution.
Is it better to rest or keep moving before joint replacement?
Most seniors should avoid both extremes. Too much rest can reduce strength and confidence, while overdoing activity can trigger pain spikes. The right middle path should be individualized with a clinician or physical therapist.
Can a cane or walker help while waiting for surgery?
Yes, when properly fitted and used correctly. A cane or walker can reduce stress on the painful joint, improve confidence, and lower fall risk. Poor fit or wrong technique can create new problems.
Should seniors avoid stairs before hip or knee replacement?
Not always, but stairs may need a safer plan. Railings, pacing, proper footwear, and limiting unnecessary trips can matter. New difficulty with stairs should be mentioned to the care team.
Why does joint pain get worse at night?
Night pain may reflect inflammation, positioning, daytime overuse, stiffness, or poor sleep cycles. Persistent or worsening night pain deserves a clinician conversation, especially if it changes mobility or mood.
What should adult children ask instead of “How’s your pain?”
Ask functional questions: “Did you avoid the shower today?” “Was the bathroom harder last night?” “Did you skip meals because standing hurt?” Function often reveals risk better than a 1-to-10 pain score.
Can waiting too long for joint replacement make things worse?
A long wait may affect strength, mobility, confidence, sleep, and fall risk. Readers should ask their surgeon what changes should trigger a call, whether earlier dates or cancellation lists are available, and how to stay as strong as safely possible.
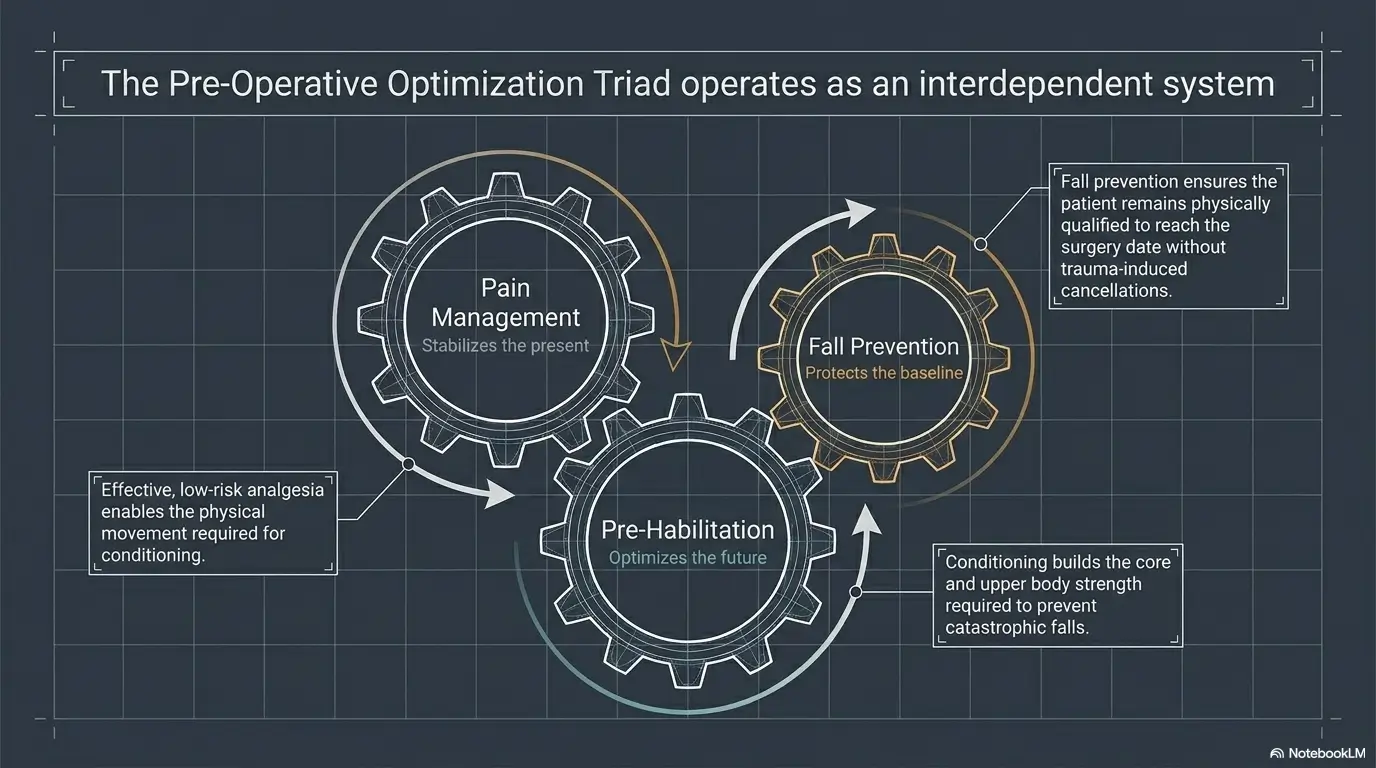
Next Step: Build a 7-Day Pain-and-Function Snapshot
Track pain, walking, sleep, medication timing, and near-falls
The best next step is not a heroic overhaul. It is a 7-day snapshot. One page. Seven evenings. Three minutes each night.
Track pain, walking, sleep, medication timing, dizziness, stumbles, and skipped activities. The goal is not to impress the doctor with tidy handwriting. The goal is to replace foggy memory with useful patterns.
Bring one page to the surgeon, not a fog bank of memories
Appointments are short. Pain memories are slippery. A one-page summary helps the care team see what changed, what is risky, and what needs attention before surgery.
Choose one fix this week: bathroom, bed, walking aid, or medication review
Do not fix the whole house in one weekend. Choose one high-impact area. Bathroom safety. Bed-to-bathroom route. Walking aid fit. Medication review. Chair height. Kitchen standing time. One good fix beats 14 half-fixes and a garage full of regret.
- Track the hardest movement.
- Record stumbles, dizziness, and skipped activities.
- Bring the page to the care team.
Apply in 60 seconds: Start tonight with one line: “The hardest movement today was ___.”
Conclusion: Make the Wait Safer, Not Just Shorter
The waiting period before joint replacement can feel like dead time, but it is not dead. It is a narrow bridge. What happens on that bridge can shape strength, sleep, confidence, fall risk, and the first steps into recovery.
The goal is not to become fearless or perfectly pain-free. The goal is to make each day a little less risky: fewer rushed bathroom trips, fewer medication guesses, fewer marathon chore days, fewer mystery flares, and more useful information for the people helping you.
Start small today. In the next 15 minutes, choose one action: remove one trip hazard, write down your hardest daily movement, gather medication bottles, or call the care team with one clear question. Pain may still be present, but the plan no longer has to be vague.
Last reviewed: 2026-04.
