
Start with the Night:
A Senior’s Guide to Safer Hip Pain Management
Nighttime hip pain has a cruel little timing problem: it often shows up when an older adult is least prepared to think clearly. The ache is hard enough, but the real risk is what follows—a stiff turn in bed, a half-awake reach for the lamp, or a guessed dose from a nightstand bottle.
For seniors, orthopedic pain management is not just about sleep. It is about safer positioning, clearer medication routines, and fall prevention. We aim for mornings that do not begin with fear, dizziness, or avoidable stiffness.
“One bad night can turn into a worse pattern: less movement, more pain, and a bedroom-to-bathroom route that feels longer than it is.”
This guide helps you build a calmer nighttime plan without turning your room into a medical supply closet. You will learn how to:
- ✦ Spot useful pain clues for your next appointment.
- ✦ Set up the bedside area to reduce risky 2 a.m. decisions.
- ✦ Ensure pain relief never compromises your balance.
Table of Contents
Safety note: This article helps readers organize safer routines, questions, and home adjustments for nighttime hip pain. It does not diagnose the cause of hip pain or tell anyone to start, stop, combine, or change medications, supplements, exercises, injections, sleep aids, or mobility devices without a clinician’s guidance.
Falls are the leading cause of injury for adults 65 and older in the United States, and the CDC states that more than 14 million older adults report falling each year. That is why a nighttime hip pain plan should always consider balance, lighting, medication effects, and safe movement, not pain relief alone.

Start Here: Nighttime Hip Pain Is Not Just a Sleep Problem
Nighttime hip pain has a way of becoming enormous after the house gets quiet. During the day, noise does some of the carrying. Dishes clink. Phones buzz. Someone asks where the scissors went, again. At night, the pain gets the stage, the spotlight, and a tiny microphone.
But for an older adult, the real problem is rarely “I slept badly” by itself. The bigger issue is the chain reaction: pain wakes the person, the person moves too quickly, the hallway is dim, the walker is two steps too far away, and suddenly the night has teeth. For a broader framework, this fits inside elderly orthopedic pain management, where pain relief and daily safety have to sit at the same kitchen table.
Why hip pain feels louder when the house gets quiet
Pain can feel sharper at night because there are fewer distractions, the body has been still, and certain positions may place pressure on the hip, back, or outer thigh. Even mild pain can feel urgent when it interrupts sleep for the third night in a row.
I have seen families underestimate this because daytime conversations sound manageable: “It’s not too bad.” Then the morning tells a different story. The person is stiff, irritable, afraid to shower, and already tired before breakfast has found the toaster.
The hidden danger is not only pain, but the 2 a.m. bathroom trip
The 2 a.m. bathroom trip is where orthopedic pain management becomes home-safety design. A sore hip can change stride length, slow reaction time, and make someone grab furniture that was never hired for that job.
A safer night means fewer surprises. It means the path is clear, the light is predictable, the assistive device is reachable, and the person knows what to do before pain starts negotiating.
What a “better night” should actually mean for an older adult
A better night is not always pain-free. That is a nice dream, but we are not selling moonlight in a bottle. A better night may mean:
- Fewer pain awakenings.
- Less rushing to stand.
- Safer bathroom trips.
- Clear medication timing.
- A morning with less stiffness, fear, or unsteadiness.
- Do not judge success only by pain score.
- Track whether the person moved safely overnight.
- Look at morning function, not just midnight discomfort.
Apply in 60 seconds: Write one sentence tonight: “A better night means I can get up safely, use the bathroom safely, and wake up steady.”
Who This Is For, and Who This Is Not For
This guide is for the ordinary, frustrating, very human middle ground: hip pain that keeps showing up at night, but not always loudly enough to send someone to urgent care. It is for the senior who says, “I’m fine,” while quietly changing how they sleep, walk, and plan their day.
It is also for the adult child, spouse, neighbor, or caregiver trying not to hover. There is a fine line between helpful and “domestic air-traffic controller.” The goal is not to supervise every breath. The goal is to remove predictable trouble before it gets dramatic.
This is for seniors with recurring hip pain that disrupts sleep
This article may help if nighttime hip pain:
- Wakes the person more than occasionally.
- Makes side-sleeping difficult.
- Causes stiffness when getting out of bed.
- Makes bathroom trips slower or more nervous.
- Leaves the person more unsteady in the morning.
This is for caregivers trying to reduce nighttime risk without hovering
Caregivers often ask the wrong question because they are being polite. “How did you sleep?” gets the standard answer: “Fine.” It is the conversational equivalent of a closed curtain.
Better questions are concrete. Did pain wake you? Did you need to get up? Did you use your cane or walker? Did you feel dizzy? Did you take anything for pain? These questions sound less poetic, but they rescue actual information from the fog.
This is not for sudden injury, severe new pain, fever, or inability to bear weight
Some symptoms should not be handled with pillow experiments and brave little routines. A senior needs urgent medical guidance for severe pain after a fall, inability to stand or bear weight, sudden major worsening, fever, redness, swelling, confusion, chest pain, or symptoms that feel alarming.
Hip pain can come from many places: the hip joint, tendons, bursae, low back, nerves, muscle strain, fracture, infection, inflammatory disease, or referred pain. The safest plan begins with humility. The body is not a filing cabinet. It does not always label the drawer.
- Yes if the pain is recurring, familiar, and not linked to a recent fall or sudden inability to walk.
- Yes if the person can stand, communicate clearly, and move safely with usual support.
- No if there is severe new pain, fever, redness, swelling, major weakness, or inability to bear weight.
- No if medications are being changed without a doctor or pharmacist review.
Neutral action: If any “No” applies, contact a clinician, urgent care, or emergency services based on severity.
Pain Source Clues: Where the Hip Hurts Can Change the Plan
“Hip pain” is a suspiciously simple phrase for a complicated neighborhood. The hip joint sits deep. The outer hip has tendons and bursae. The low back can send pain downward like a badly addressed letter. The knee may complain because the hip changed the walking pattern first.
Location does not diagnose the problem, but it can help families describe the pattern clearly. That matters because clinicians make better decisions when the story has a map.
Groin pain may point toward the hip joint itself
Hip joint problems often show up as pain in the groin or front of the thigh, especially with walking, standing from a chair, or turning. Some people describe it as deep, catching, stiff, or hard to “get moving” after rest.
If a senior says, “It feels like it is inside,” do not dismiss that detail. Write it down. The phrase may be clumsy, but it often carries useful information.
Outer-hip pain may behave differently when lying on one side
Outer-hip pain can become nasty when someone lies directly on the painful side. It may also hurt when the top leg drops across the body and twists the hip. This is where pillow placement can matter, though it should not replace evaluation if pain persists.
One practical clue: ask whether the pain worsens from pressure on the mattress or from the motion of rolling over. Those are different little villains. Readers who sleep on one side may also want to compare these patterns with side sleeper hip pain relief strategies that focus specifically on pressure, pillow support, and hip rotation.
Back, buttock, or leg symptoms may not be “just hip pain”
Pain that travels into the buttock, back of the thigh, calf, or foot may involve the low back or nerves. Numbness, tingling, new weakness, or changes in bowel or bladder control deserve prompt medical attention.
Families sometimes call everything from the waist to the knee “hip.” That is understandable. The body did not come with helpful dotted lines. Still, the more specific the description, the better the appointment. When symptoms blur between the hip and the spine, a guide to hip vs spine pain can help families ask more precise questions before the visit.
The important question: did the pain pattern change suddenly?
Recurring pain that behaves predictably is one thing. Sudden pain that changes the walking pattern overnight is another. A new inability to bear weight, especially after a fall, should not be treated as “probably arthritis acting up.”
Show me the nerdy details
Clinicians often separate hip-region pain by location, triggers, function, and associated symptoms. Groin-dominant pain may raise concern for intra-articular hip conditions, while lateral pain may suggest outer-hip soft tissue irritation. Radiating pain, numbness, or weakness may shift attention toward the lumbar spine or nerve involvement. These clues do not diagnose the condition, but they improve triage and reduce vague reporting.
Before Bed: Build a Pain-Calming Ramp, Not a Last-Minute Rescue
A good nighttime hip pain plan starts before pajamas. Waiting until pain spikes is like waiting until the pot boils over to look for the lid. Possible? Yes. Elegant? No. Also, someone may step on the dog.
The better strategy is a pain-calming ramp: a repeatable 30-minute routine that lowers friction before the person is tired, sore, and squinting at pill bottles under the weak glow of a bedside lamp.
Why waiting until pain spikes can make the night harder
When pain is already high, every choice gets worse. Standing feels more urgent. The bathroom feels farther away. The brain becomes less patient. A person may skip the walker because it is across the room, or take medicine from memory because the label feels too annoying to read.
That is why the routine should happen while the person is still alert. Pain management at night is not just about what helps the hip. It is about what protects judgment.
The 30-minute wind-down check: pain, walking path, water, phone, bathroom
Try this simple pre-bed sequence:
- Rate the pain and location. Use plain words: groin, outer hip, buttock, thigh, back.
- Use the bathroom before bed. Reduce one urgent trip if possible.
- Place water safely. Use a stable bottle, not a glass balanced like a tiny disaster trophy.
- Confirm phone access. Put it in the same reachable spot every night.
- Clear the path. Shoes, cords, laundry, rugs, and pet bowls should not audition as obstacles.
Let’s be honest: “I’ll deal with it if I wake up” is not a plan
That sentence sounds independent. In practice, it often means the person will improvise while stiff, tired, and annoyed. Improvisation is wonderful in jazz. It is less charming beside a bed at 2:17 a.m.
Give one point for each “yes.”
- Is the bathroom path partly dark?
- Is the cane or walker more than one arm’s reach from bed?
- Are there rugs, cords, shoes, laundry, or pet items near the bed path?
Output: 0 means tonight’s setup is calmer. 1 means fix one thing. 2 to 3 means the room is asking for a reset before bedtime.
Neutral action: Remove the easiest obstacle first, because easy fixes actually happen.
Sleep Positioning: Small Pillow Changes Can Prevent Big Pain Spirals
Sleep positioning is the most tempting place to give universal advice. Unfortunately, bodies are not identical chairs. One senior feels relief on the back. Another feels trapped. One side-sleeper needs a pillow between the knees. Another needs support behind the back to stop rolling onto the painful side.
The goal is not to find the “perfect” position. The goal is to reduce the positions that reliably start the pain spiral.
Side-sleeping without support can twist the hip into protest
When side-sleeping, the top leg may fall forward and pull the hip into rotation. For some people, that twist increases discomfort. A pillow between the knees can keep the top leg from dragging the pelvis along for the ride.
For outer-hip pain, lying directly on the painful side may be too much pressure. Lying on the opposite side with a pillow between the knees may help some people, though persistent pain still deserves a clinician’s review.
Back-sleeping may help some seniors but frustrate others
Back-sleeping can distribute pressure more evenly, but it is not magic. Some seniors dislike it, some snore more, and some feel low-back discomfort. A small pillow under the knees may reduce strain for certain people, but anyone with medical restrictions should ask a clinician.
Comfort matters. A routine that looks perfect on paper and causes three hours of grumbling is not a routine. It is furniture-based theater.
The pillow test: support the knee, not just the mattress
Try a three-night pillow test, but keep it simple:
- Night 1: Pillow between knees while side-sleeping.
- Night 2: Pillow supporting the top leg more fully from knee to ankle.
- Night 3: Back-sleeping with gentle knee support if tolerated.
Track only two things: Did pain wake you? Did you get out of bed more safely in the morning? A fancy sleep diary with 19 categories may look impressive, but tired people abandon it faster than a gym membership in February.
When a recliner becomes a clue, not a cure
If a senior can only sleep in a recliner because bed pain is unbearable, that is useful information for a clinician. A recliner may temporarily feel easier for some people, but it can create other problems: stiffness, pressure areas, swelling, or unsafe transfers if the person stands too quickly. If the pain is connected to a recent procedure, sleeping comfort may need a different lens, especially with sleeping discomfort after hip replacement.
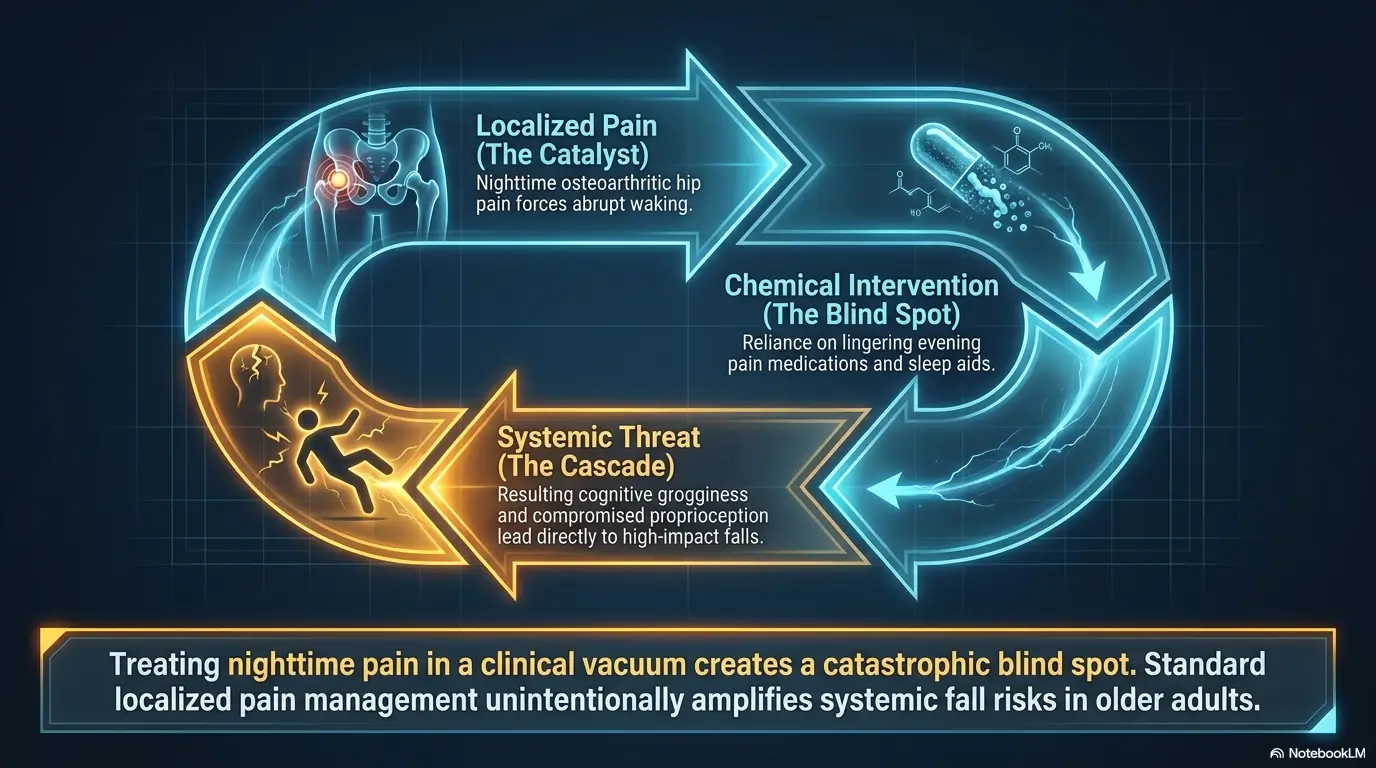
Infographic: The Safer Night Hip Pain Loop
Check pain, bathroom, water, phone, walking path.
Support knees and avoid known pressure triggers.
Sit, pause, stand, then step with support.
Record dose timing clearly. No guessing in the dark.
Ask what woke pain and what made movement safer.
Medication Safety: Nighttime Relief Should Not Create Morning Danger
Medication can be helpful, but nighttime medication decisions need extra care in older adults. The National Institute on Aging warns that taking medicines incorrectly or mixing medicines with certain drugs or supplements can be dangerous, especially as people age.
The key principle is blunt but kind: do not make the hip quieter by making the person less steady.
Why older adults need a medication review before “just taking something”
Older adults may process medicines differently than younger adults. They may also take multiple prescriptions, over-the-counter medicines, vitamins, supplements, or sleep aids. One small bedtime addition can change dizziness, alertness, blood pressure, bathroom urgency, or morning balance.
This is where a pharmacist can be a remarkably practical ally. Pharmacists spend their days in the land of interactions, dose timing, duplicate ingredients, and labels that look harmless until they meet each other at midnight.
Watch the risky stack: pain medicine, sleep aids, alcohol, dizziness
Be especially careful with combinations that may increase sleepiness or dizziness. That includes some pain medicines, sleep aids, alcohol, certain anxiety medicines, muscle relaxers, and other sedating drugs. Even some “natural” supplements can interact with medicines.
No one likes being told to review a medicine list. It feels like homework with smaller print. But it can prevent a bad chain reaction: pain, pill, dizziness, bathroom trip, fall. Seniors waiting for a more definitive joint plan may also need a practical bridge, which is why pain management for seniors waiting on joint care should still keep fall risk and medication timing in view.
Keep a written dose log where tired eyes can still understand it
A bedtime dose log should be simple enough for a tired person to use:
- Medicine name.
- Dose.
- Time taken.
- Reason taken.
- Any dizziness, nausea, confusion, or unusual sleepiness.
Use large writing. Use a dark pen. Keep it in the same place. The best system is not the prettiest one. It is the one that survives Tuesday.
What to ask the doctor or pharmacist before changing the bedtime routine
Ask direct questions:
- Could any current medicine worsen dizziness or nighttime falls?
- Is this pain medicine safe with kidney disease, blood pressure issues, stomach bleeding history, blood thinners, or other conditions?
- What side effects should prompt a call?
- Should pain medicine timing change, or should the treatment plan itself be reviewed?
- Keep one accurate medication list.
- Track bedtime doses on paper.
- Ask a pharmacist about interactions before adding anything new.
Apply in 60 seconds: Put a pen and dose log beside the medication area before dinner, not after the house goes dark.
Common Mistakes: What Makes Nighttime Hip Pain More Risky
Most risky nighttime habits do not look reckless. They look normal. They look like “I’ve always done it this way.” That is exactly why they survive so long.
A senior may know the bedroom perfectly in daylight, but nighttime pain changes the rules. Add stiffness, urgency, medication effects, or low lighting, and the familiar room becomes a tiny obstacle course with curtains.
Mistake 1: walking to the bathroom in the dark “because it’s close”
Close is not the same as safe. A bathroom ten steps away can still be risky if the first two steps are stiff, the rug edge curls, the nightlight is weak, and the walker is parked like a retired bicycle across the room.
The fix is boring, which is a compliment: light the path, clear the floor, use the usual assistive device, and pause before standing.
Mistake 2: saving all movement until bedtime, then stiffening overnight
Some seniors reduce movement all day because hip pain is annoying. Then bedtime arrives and the body feels like an old gate in winter. Too much rest can increase stiffness for some people, while too much activity can trigger a flare. The middle path is less glamorous, but it often works better.
Mistake 3: judging pain only by number, not by function
A pain score can help, but it is not enough. A “4” that prevents safe showering matters. A “6” that improves after movement tells a different story. Function reveals what the number hides.
Ask: Can the person get out of bed safely? Walk to the bathroom? Put on socks? Stand from a chair? Sleep at least a few hours? These are not small details. They are the plot.
Mistake 4: adding gadgets before fixing the walking path
Families may buy wedge pillows, massage tools, bed rails, heating pads, new mattresses, and enough “comfort items” to open a tiny warehouse. Some tools help. But gadgets should not arrive before the basics: clear path, safe light, reachable support, reviewed medications, and a plan for urgent symptoms. When support devices are part of the conversation, it can help to understand which HSA eligible braces and supports may be worth discussing before buying equipment out of frustration.
Here’s what no one tells you: the most dangerous object may be the throw rug, not the hip
A throw rug is very good at pretending to be décor. At night, it may become a trip edge with ambition. If hip pain already shortens steps, even a small rug can matter.
- The person gets up at night.
- The room has rugs, cords, clutter, or dim corners.
- The assistive device is not reachable from bed.
- Transfers are consistently difficult.
- The person avoids bed or bathroom due to pain.
- A clinician or therapist recommends a specific aid.
Neutral action: Spend 10 minutes clearing the route before spending money on a new device.
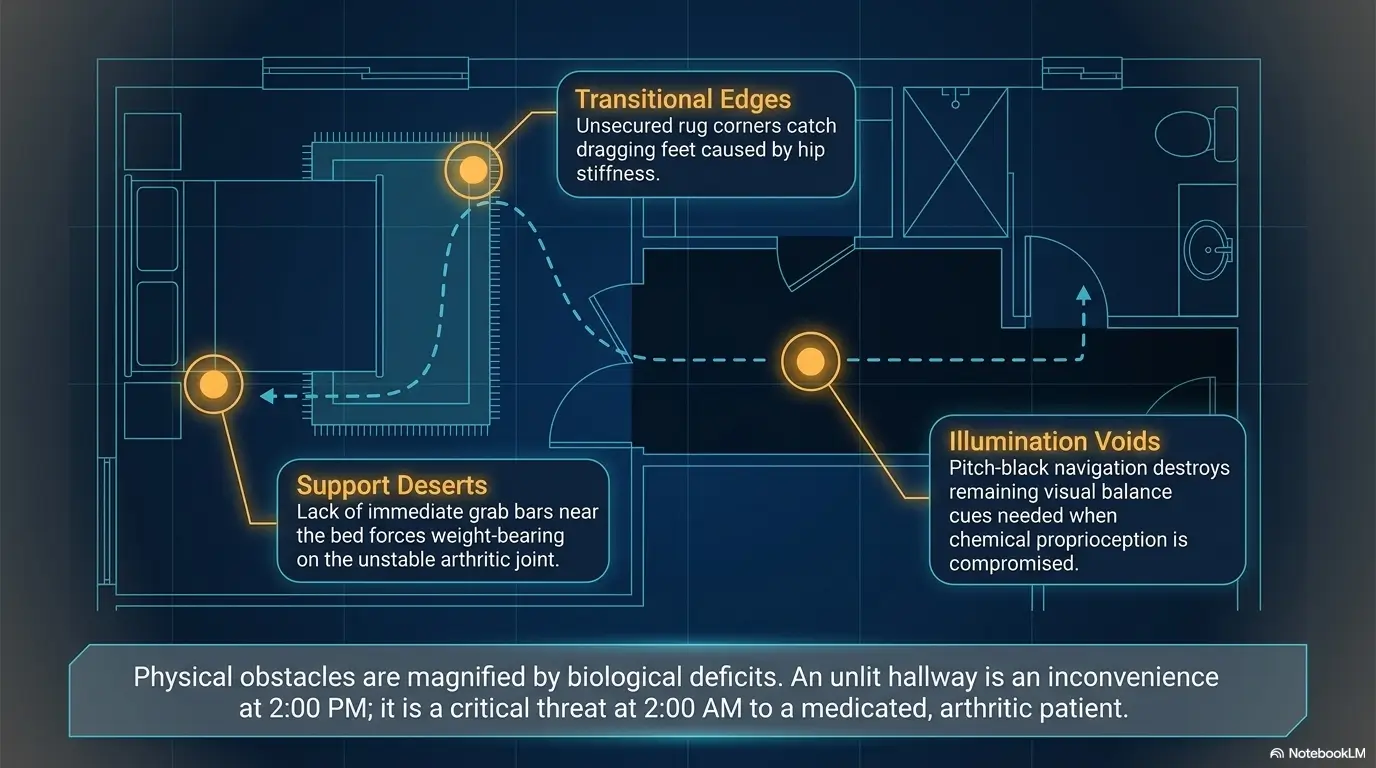
Overnight Setup: Design the Room for a Half-Awake Body
A good overnight setup assumes the person will not be at their sharpest. This is not insulting. It is design with manners. At 2 a.m., nobody should have to solve a small engineering problem just to find their glasses.
The best bedside setup is repetitive, tactile, and slightly boring. Same place. Same order. Same path. Same light. Predictability is the quiet hero of nighttime safety.
Put the cane, walker, glasses, phone, and water in fixed positions
Give important items “addresses.” Glasses live in the same tray. Phone lives in the same charging spot. Cane or walker sits on the same side of the bed. Water is in a stable bottle with a lid.
When I help someone think through a bedside setup, I ask one question: “Could you find this with sleepy hands?” If the answer is no, the system is not ready.
Use low-glare lighting from bed to bathroom
Lighting should help without startling. Bright overhead lights may cause glare or disorientation for some people, especially when waking from sleep. Low-glare nightlights, motion lights, or bedside lamps can help create a visible route.
The light should show edges: bed, floor, doorway, bathroom entrance. It should not turn the hallway into an interrogation room.
Clear the “sleepy shuffle zone” beside the bed
The first two steps matter. Keep the bedside floor clear of slippers, cords, books, baskets, oxygen tubing if used, pet beds, laundry, and that one mysterious tote bag everyone stopped questioning in 2021.
Footwear also matters. If slippers are used, they should be stable, easy to put on, and not floppy. A loose slipper at night is not comfort. It is a banana peel with fleece.
Make the first step out of bed boring, predictable, and slow
Try a four-part transfer cue:
- Sit up.
- Place both feet flat.
- Pause and check for dizziness.
- Stand with the usual support.
The pause is not wasted time. It is a safety feature. Ten seconds can reveal dizziness before the first step turns into a bad surprise.
Movement Windows: Don’t Let Rest Turn Into Rust
Rest has a seductive logic: if movement hurts, move less. Sometimes rest is appropriate, especially after injury or flare-ups. But in many chronic orthopedic pain patterns, too much stillness can make stiffness worse, sleep harder, and confidence smaller.
The trick is not to become heroic. The trick is to create movement windows: small, safe, planned moments of activity before the body stiffens into a complaint committee.
Gentle daytime movement may reduce nighttime stiffness for some seniors
For some seniors with hip arthritis or chronic hip-region pain, gentle movement during the day may help reduce stiffness and support function. The American Academy of Orthopaedic Surgeons notes that hip osteoarthritis care often aims to reduce pain and improve mobility, and that physical therapy may help some people move better and feel less pain.
That does not mean pushing through severe pain. It means asking the clinician what type of activity is appropriate and then keeping it boring enough to repeat.
Balance rest with short, safe walking breaks
A walking break might be two to five minutes indoors, depending on ability and clinician guidance. The goal is not mileage. The goal is circulation, confidence, and reminding the hip that the day has not ended at the recliner.
A timer can help. So can pairing movement with ordinary anchors: after breakfast, after lunch, before dinner. Habit works best when it piggybacks on something already happening.
Stop before the “I felt okay, so I did too much” mistake
This mistake is everywhere. A senior feels better, tackles laundry, changes sheets, carries groceries, waters plants, and then wonders why the night turns sour. Pain relief can create false permission.
Use a stop rule. For example: one chore, then sit. One short walk, then reassess. One task that matters, not five tasks that prove a point to nobody.
Ask whether physical therapy should be part of the plan
Physical therapists can help with strength, gait, balance, transfers, and safe home movement. They can also teach families which activities are useful and which ones are stirring the pot. If therapy has already been tried without enough progress, the next discussion may be closer to what to do when physical therapy is not helping orthopedic pain, rather than simply repeating the same routine louder.
- Use short movement windows.
- Stop before the pain spike.
- Ask whether physical therapy fits the diagnosis and goals.
Apply in 60 seconds: Choose one daytime movement anchor, such as after breakfast, and write it on the routine sheet.
When to Seek Help: Night Pain That Deserves a Clinician’s Eyes
Not every night of hip pain is an emergency. But recurring night pain deserves respect, especially when it changes walking, sleep, medication use, or confidence. Older adults are too often expected to normalize discomfort until it becomes a full production with paperwork.
The practical question is: what kind of help, and how soon?
Call urgently for severe pain after a fall or inability to stand
Severe hip pain after a fall needs urgent medical guidance, particularly if the person cannot stand, cannot bear weight, has obvious deformity, or has sudden severe pain. Do not turn this into a “sleep it off” situation.
Hip fractures and serious injuries are not always cinematic. Sometimes the person simply cannot move normally. Believe the function change. When the decision is unclear, comparing urgent care vs orthopedic clinic can help families think through where to start based on severity, function, and timing.
Get prompt help for fever, redness, swelling, or sudden worsening
Fever, redness, warmth, swelling, sudden worsening pain, confusion, unexplained weakness, or signs of infection should prompt medical attention. Pain that comes with systemic symptoms is no longer just a pillow-placement puzzle.
Ask about evaluation if pain repeatedly wakes the person or limits walking
If hip pain repeatedly wakes a senior, limits walking, changes bathroom safety, or causes new reliance on furniture for balance, schedule an evaluation. Bring a written pattern, not just a memory cloud.
Helpful details include:
- Where the pain is located.
- What time it wakes the person.
- Which side or position makes it worse.
- Whether walking improves or worsens it.
- What medicines were taken and when.
- Any falls, near-falls, dizziness, or morning weakness.
Bring a sleep-and-function log, not just a pain score
A pain score is one tile in the mosaic. The clinician also needs function. Can the person walk to the bathroom? Get out of bed? Sleep on either side? Climb stairs? Shower safely? Stand long enough to prepare breakfast?
These details help the clinician decide whether the plan should involve imaging, medication review, physical therapy, injections, assistive devices, home safety support, or referral to orthopedics. If imaging becomes part of the discussion, it may help to understand orthopedic pain management before asking for an MRI so the appointment is built around function, exam findings, and a clear treatment path.
- Current medication list, including over-the-counter medicines and supplements.
- Three to seven nights of sleep-and-function notes.
- Fall history or near-fall details.
- Photos of the bedroom-to-bathroom path if home setup is part of the concern.
- Insurance card, primary care information, and any prior hip or spine imaging reports.
Neutral action: Put these items in one folder before the appointment, because waiting-room memory is a slippery little fish.
Caregiver Check-In: Ask Better Questions Than “How Was Your Night?”
“How was your night?” is a loving question with weak batteries. Most people answer it with one word. Fine. Okay. Rough. Then the real information slips away like steam from a mug.
Caregivers need questions that reveal function, safety, and patterns without making the older adult feel cross-examined. The tone matters. This is not a courtroom. It is a kitchen-table investigation with tea.
Did pain wake you, or did walking wake the pain?
This question separates two patterns. Pain that wakes someone while still lying down may suggest a different issue than pain triggered by getting up, turning, or walking. Both matter, but they lead to different follow-up questions.
Did you use the bathroom safely, or rush because you were hurting?
Rushing is a risk marker. If pain creates urgency, the plan should address the pre-bed bathroom routine, lighting, assistive device placement, and whether medication timing or medical evaluation needs review.
Did you skip, double, or guess any medicine?
Ask this gently. Medication confusion can happen to careful people, especially when pain interrupts sleep. The purpose is not blame. The purpose is to make the system easier than guessing.
Did the morning feel stiffer, weaker, or more unsteady than usual?
Morning function is a report card for the night. More stiffness, weakness, dizziness, or unsteadiness may point to pain flares, poor sleep position, medication effects, dehydration, or simply a room setup that made movement tense.
“Was last night any easier, or was it one of those stubborn hip nights?”
“Did you get up safely, and did you take any medicine during the night?”
Neutral action: Write the answer in plain language and watch for patterns over one week.
FAQ
Why does hip pain get worse at night in older adults?
Hip pain may feel worse at night because the body is still, distractions are gone, and certain positions place pressure or rotation on painful tissues. Stiffness after rest can also make pain more noticeable when turning or getting out of bed. Recurring night pain should be discussed with a clinician, especially if it affects walking or sleep quality.
What sleeping position is usually safest for hip pain?
There is no single safest position for everyone. Some people feel better on their back with gentle knee support. Others do better side-sleeping with a pillow between the knees. The safest position is the one that reduces pain without making transfers, breathing, dizziness, or morning stiffness worse.
Should a senior use heat or ice before bed for hip pain?
Heat or ice may help some people, but the right choice depends on the condition, skin sensitivity, circulation, medication use, and clinician guidance. Avoid sleeping on a heating pad or ice pack. Older adults should use temperature therapies cautiously to reduce burn or skin injury risk.
Can hip arthritis cause pain that wakes someone up?
Hip arthritis can cause pain, stiffness, and reduced mobility, and some people do notice more discomfort at night or after periods of rest. However, night pain can have other causes too. A clinician should evaluate recurring pain that wakes someone, changes walking, or limits daily function.
When is nighttime hip pain a red flag?
Seek urgent help for severe pain after a fall, inability to stand or bear weight, sudden major worsening, fever, redness, swelling, confusion, new weakness, or symptoms that feel alarming. Do not rely on home routines when the pain pattern changes sharply or function drops suddenly.
Can pain medicine increase fall risk at night?
Some medicines can increase sleepiness, dizziness, confusion, or balance problems, especially when combined with sleep aids, alcohol, or other medications. Older adults should review nighttime pain medicine use with a doctor or pharmacist before changing the routine.
What should caregivers put beside the bed for safer nights?
Useful bedside items may include glasses, phone, water in a lidded bottle, a written medication log, a working lamp, and the usual cane or walker within safe reach. Keep the floor clear beside the bed so the first step is predictable.
Is walking during the day helpful or harmful for nighttime hip pain?
It depends on the diagnosis and the person’s ability. Gentle, clinician-approved movement may reduce stiffness for some seniors, but overdoing chores or walking through severe pain can worsen symptoms. Ask the clinician or physical therapist what level of movement is appropriate.
Next Step: Make Tonight’s Hip Pain Plan Before Dinner
The opening problem was never only the hip. It was the half-awake scramble: pain, darkness, stiffness, guessing, and a bathroom trip that suddenly asks too much from a tired body.
So make the plan before dinner, while the brain is still wearing shoes. Do not wait until bedtime, when every small task feels like a committee meeting held in a closet.
Pick one pain note, one room fix, and one clinician question
Start with three tiny actions:
- One pain note: “Outer hip hurt when lying on right side at 1 a.m.”
- One room fix: “Move walker to bedside and remove rug near bathroom path.”
- One clinician question: “Could any current medicine increase nighttime dizziness?”
That is enough for tonight. A safer routine does not need to be theatrical. It needs to be repeatable.
Write the bedtime routine on paper, not in memory
A written routine lowers the chance of tired improvisation. Place it where it will be seen: beside the bed, on the nightstand, or near the medication area.
Example:
- Use bathroom before bed.
- Set phone, glasses, water, and dose log in fixed places.
- Check walking path and light.
- Use pillow support.
- If waking with pain, sit first, pause, then stand with support.
Review the plan after one week and look for patterns
After seven nights, look for signals. Is pain worse on one side? Does it wake the person at the same time? Does a certain activity make the night worse? Is the person taking extra medicine more often than expected? Is morning balance declining?
These patterns are the gift. They turn vague worry into useful information.
- Fix the walking path first.
- Write medication timing clearly.
- Bring patterns to the clinician, not guesses.
Apply in 60 seconds: Before dinner, remove one obstacle between bed and bathroom and place the usual walking aid within safe reach.
Final 15-minute action: Walk the bedroom-to-bathroom route in daylight. Remove one trip hazard, test one light, place one support item, and write one question for the doctor or pharmacist. That is not a perfect plan. It is better: it is a plan someone can actually use tonight.
Last reviewed: 2026-04.
