
The Hidden Logic of Spine Decisions
Most spine decisions don’t break on “severe stenosis.” They break on one boring line you don’t have yet: stable on flexion-extension.
If you’re weighing spinal stenosis decompression without fusion, you’re likely stuck between two fears that don’t talk to each other: “What if I under-treat and regret it?” vs “What if I over-treat and live with hardware I didn’t need?”
Guessing here is expensive in the currency you actually feel: walking distance, sleep, and confidence in your own body.
Decompression without fusion relieves nerve pressure by removing tissue that crowds the spinal canal (via laminectomy or foraminotomy) without adding screws or rods. It’s typically considered when symptoms are leg-dominant and the spine is stable enough that freeing the nerve won’t create a new instability.
The Strategy
- • Get your case into three bullets.
- • Stop worshipping MRI adjectives.
- • Start measuring the right things.
What You’ll Leave With
- • A candidate self-sort that doesn’t overpromise.
- • Stability questions that force plain answers.
- • A short document checklist for any clinic.
Decompression without fusion is typically considered when spinal stenosis symptoms come from nerve compression and the spine is stable (no meaningful spondylolisthesis/instability on imaging) and the main issue is leg-dominant pain or walking limits that haven’t improved with conservative care. Candidates often have limited levels involved and no major deformity requiring stabilization. Final eligibility depends on imaging, stability tests, and a surgeon’s assessment of risk.
Table of Contents

The “Fusion or Not” Decision Tree: What the Logic Actually Checks
The core question: compression problem or stability problem?
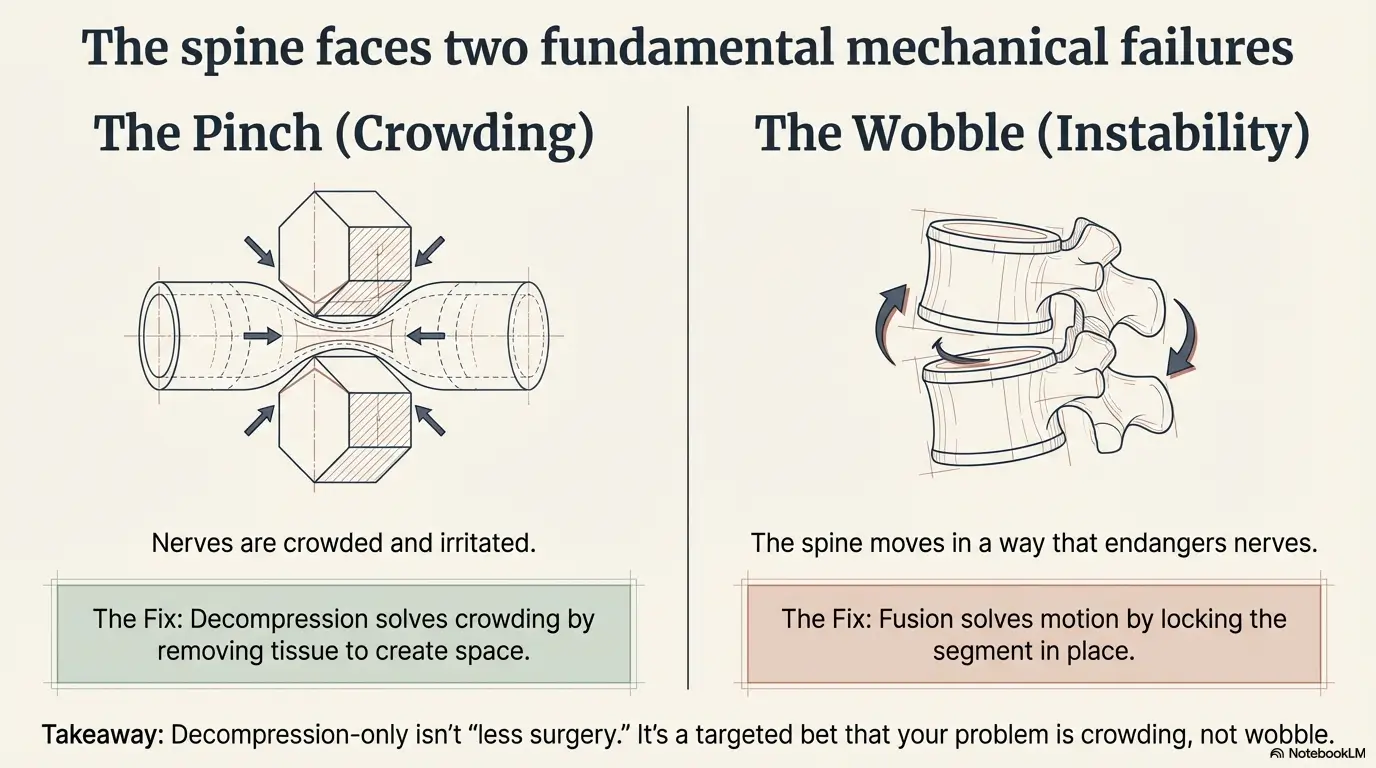
Here’s the fork in the road that matters more than your MRI adjectives. Is your suffering mainly a pinch problem (nerves crowded) or a wobble problem (spine moving in a way that irritates or endangers nerves)? Decompression solves crowding. Fusion solves motion. Sometimes you have both, but most “fusion or not” debates are really about whether you’re stable enough to remove tissue safely without tipping you into a new instability. If you want a deeper side-by-side on that trade, see lumbar fusion vs decompression (what each surgery is actually “for”).
A surgeon who recommends fusion is often saying: “If I remove what I need to remove to free the nerve, I’m worried the joint won’t hold up.” A surgeon who recommends decompression-only is often saying: “We can free the nerve while preserving enough structure to keep your spine behaving.”
Three gates most surgeons evaluate (symptoms, imaging, motion)
- Symptoms gate: Do your symptoms behave like stenosis (especially leg-dominant pain and walking limits), and are they severe enough to justify surgical risk?
- Imaging gate: Do MRI/CT findings match your symptom pattern at specific level(s)?
- Motion gate: Is there evidence your segment is unstable (or likely to become unstable after decompression)?
- Symptoms point to leg limits more than pure back pain.
- Imaging shows the pinch at the level that matches your pattern.
- Motion testing suggests the segment is stable enough to stay stable.
Apply in 60 seconds: Write one sentence: “My worst symptom is ______ and it happens most when I ______.” Bring that sentence to every consult.
A quick lived-experience note: the first time I sat with a family member’s spine consult notes, I expected a dramatic verdict. Instead, it was quietly boring. “Leg symptoms. L4-5. Low-grade slip. Flex/extension.” The boring details were the entire decision.
Symptoms That Fit Decompression-Only: The Leg-Pain Pattern
Neurogenic claudication: the “walking shutdown” that resets with sitting
Classic lumbar stenosis often shows up as neurogenic claudication: you walk or stand, then your legs start protesting. You stop, you sit, you lean forward on a shopping cart, and the whole system calms down like a dimmer switch. That “reset with flexion” pattern is a big reason decompression works. You’re making room for nerves that hate being crowded when the spine is extended. For some people, a mobility aid becomes a practical bridge, not a defeat, and this guide on using a rollator for lumbar spinal stenosis can help you think through that choice.
- Walking tolerance drops in a predictable way (often within minutes).
- Standing still can be worse than walking (because you’re extended).
- Sitting or bending forward reliably helps.
Leg-dominant pain vs back-dominant pain (why it matters)
Decompression is best at improving leg symptoms, numbness/tingling, and walking distance when those symptoms come from nerve compression. If your pain is mostly deep axial back pain, the logic changes. Back pain can improve after decompression (especially if it’s “referred” from nerve irritation), but it’s less predictable. Your surgeon is trying to avoid offering you an expensive, risky solution to the wrong problem.
Pattern interrupt: Let’s be honest… back pain alone changes the math
Back pain is real. It’s also a messy signal. It can come from discs, facets, muscles, posture, hip arthritis, stress, sleep deprivation, and the special chaos of being a human with a spine. If your case is “back pain only,” a surgeon may be more cautious about promising big wins from decompression-only. This doesn’t mean you’re doomed. It means the “candidate” definition is stricter. If you suspect you’re sorting the wrong source of pain, start with hip vs spine pain (how to tell what’s driving your symptoms).
- Yes/No: My main limitation is walking/standing, not only back ache.
- Yes/No: Sitting or leaning forward reliably improves symptoms.
- Yes/No: I’ve tried conservative care long enough to know my baseline (PT for sciatica and what “enough” looks like, meds, injections when appropriate).
- Yes/No: Imaging shows stenosis at a level that matches my symptom map.
- Yes/No: No clear instability on motion studies (or it’s convincingly stable).
Neutral next action: Bring this checklist to your appointment and ask which “No” items would change the plan.
Small personal anecdote: I once watched someone try to “push through” leg heaviness on a grocery run, then spend the evening on the couch bargaining with their own nervous system. The next week, their surgeon asked one question: “How far can you walk before you have to sit?” That number was the story.
Imaging Clues: What MRI/CT Is Really Being Used For
Where the pinch is: central canal vs lateral recess vs foraminal stenosis
Imaging isn’t about proving you “deserve” surgery. It’s about locating the pinch so the operation has a target. If you’re still deciding what imaging answers what, compare MRI vs X-ray for sciatica and back/leg symptoms.
- Central canal stenosis: crowding in the main tunnel; often linked with neurogenic claudication.
- Lateral recess stenosis: where nerve roots travel before exiting; can mimic classic sciatica patterns.
- Foraminal stenosis: the exit tunnel is tight; often more position-dependent and can be stubborn.
A practical clue: if your pain shoots down a specific path (outer calf, top of foot, big toe), surgeons are often thinking in “which root, which level” terms, not “which scary MRI sentence.” If you want that map in plain language, use L4 vs L5 vs S1 sciatica patterns as your cheat sheet for discussions.
Level count: single-level vs multi-level decompression and risk tradeoffs
More levels can be decompressed, but each level is another place where bone, ligament, and facet decisions matter. Multi-level decompression-only is common, but it increases the importance of preserving stabilizers. This is why surgeon technique and judgment become the plot twist.
Facet joints, ligamentum flavum, and the “how much bone can we remove?” constraint
Many stenosis cases are a slow pile-up: thickened ligamentum flavum, enlarged facets, disc bulge. Decompression creates space by removing some of that crowding. But facets are also part of your stability system. If too much facet is removed, instability risk rises. So “candidate for no fusion” often means: we can free the nerve without gutting the stabilizers.
Show me the nerdy details
Think of the motion segment (two vertebrae plus disc and facet joints) as a tripod. Decompression removes part of the roof (lamina) and sometimes trims hypertrophied ligament and facet overgrowth. The surgical challenge is balancing adequate neural decompression while maintaining enough posterior elements and facet integrity to resist shear and rotation. This is why “how much facet removal” is a high-value question.
Timely, truthful evidence in normal prose: Large randomized trials have tested decompression with and without fusion for degenerative lumbar conditions, including stenosis with or without low-grade spondylolisthesis. A major New England Journal of Medicine trial (the Swedish Spinal Stenosis Study) found no meaningful difference in outcomes at 2 years between decompression alone and decompression plus fusion, and long-term follow-up still showed similar rates of additional surgery. Another NEJM trial in 2021 (NORDSTEN-DS) reported decompression alone was noninferior to fusion for many patients with degenerative spondylolisthesis, with slightly different reoperation patterns between groups over time.
A lived-experience moment: I’ve seen people spiral after reading “severe stenosis” on a report at 11:47 PM. Then they meet a surgeon who says, calmly, “Your symptoms are mild. Let’s watch.” Imaging is a map, not a prophecy. If you’re living that mismatch, this explainer on MRI pain mismatch (why the picture and the suffering don’t always line up) can make the uncertainty feel less personal.
Stability Checks: The Make-or-Break Factor for “No Fusion”
Spondylolisthesis: when a small slip is “stable enough” and when it isn’t
Spondylolisthesis (a vertebra slipping relative to another) sounds terrifying because the word itself feels like a slipping banana peel. In reality, some slips are stable and behave like a fixed alignment issue. Others move with posture and load. Decompression-only is more plausible when any slip is low-grade and stable, and when the decompression can be done without removing too much of the structures that prevent further slip.
This is where second opinions are genuinely useful. Not because one surgeon is “right” and the other is “wrong,” but because they may estimate the stability risk differently based on technique, comfort, and what they expect to remove.
Flexion-extension X-rays: what they’re trying to catch
Flexion-extension X-rays are the “motion gate.” They look for meaningful translation or angulation that suggests instability. If the segment is already moving too much, fusion may be protective. If it’s stable, decompression-only becomes a serious contender.
Red flags for instability: pars defects, significant motion, severe facet destruction
Some patterns raise eyebrows: pars defects, clear dynamic movement, severe facet joint compromise, and deformity drivers like scoliosis/kyphosis. In those scenarios, decompression-only can be a short-term win that becomes a long-term regret if the segment collapses or slips more after bone removal.
| Year / evidence type | Population | Reported pattern (range or example) | Practical note |
|---|---|---|---|
| 2016 RCT (major journal) | Lumbar stenosis, with/without low-grade slip | Additional surgery rates were similar over years of follow-up (roughly low-20% range in both groups) | Fusion didn’t automatically “protect” everyone from future surgery. |
| 2021 RCT (major journal) | Degenerative spondylolisthesis + stenosis | Decompression-alone was noninferior; reoperation within 2 years was a bit higher in decompression-only in that trial (about 9–13% vs ~9% in fusion) | Ask which reoperation risk matters more to you: early index-level fusion vs later adjacent-level issues. |
| 2024–2025 follow-up reports | Similar degenerative populations | Reoperations can “shift” over time: slightly more early conversions to fusion after decompression, but more later new-level surgery after fusion in some datasets | The time horizon (2 years vs 5+ years) changes how “best” is defined. |
Neutral next action: Ask your surgeon which time window they’re optimizing for (2 years, 5 years, 10 years) and why.
A small anecdote: one friend said, “I just want the permanent fix.” Their surgeon replied, kindly, “Spines don’t do permanent. They do trade-offs.” That sentence should be embroidered on every MRI CD sleeve.
The “Not For” List: When Decompression Alone Is Usually a Bad Bet
Significant deformity: scoliosis/kyphosis driving symptoms
If your stenosis is being driven by deformity, decompression-only can be like widening one lane on a bridge whose supports are already tilted. Some deformities need stabilization to keep the decompression from failing mechanically.
High-grade slip or clear instability (fusion is often protective here)
When there’s clear instability, fusion is often chosen to reduce the chance of worsening slip or post-decompression collapse. In these cases, fusion isn’t “extra.” It’s the part that prevents the decompression from backfiring.
Prior surgery, recurrent stenosis, or anatomy that demands larger removal
Revision surgery can require more removal of bone/ligament due to scar tissue and altered anatomy. Sometimes a wide decompression is necessary, and that can push the stability math toward fusion. This is also where surgeon experience really matters, not as marketing, but as risk management.
Operator reality: minimally invasive approaches can reduce muscle disruption, but they don’t change physics. If your segment is unstable, a smaller incision doesn’t magically stabilize it.
Procedure Menu Without the Hype: Laminectomy, Laminotomy, and Friends
Laminectomy vs laminotomy: same goal, different footprint
Both aim to create space. A laminotomy removes part of the lamina; a laminectomy removes more of it. The choice depends on where the compression is and how much access is needed. Reputable patient-facing sources like Mayo Clinic and MedlinePlus describe laminectomy as a way to enlarge the spinal canal by removing the lamina to relieve pressure on nerves.
Foraminotomy: when the exit tunnel is the real culprit
If foraminal stenosis is the main issue, the “exit tunnel” is tight, and foraminotomy focuses on enlarging that pathway. This can matter a lot if your symptoms are radicular, position-sensitive, and match a single nerve root distribution.
Minimally invasive decompression: what it changes (and what it doesn’t)
Minimally invasive decompression often changes muscle disruption, blood loss, and sometimes early recovery. It does not remove the need for a good plan: identify the correct level, decompress enough, preserve stabilizers, and confirm the spine remains stable. It’s a tool, not a guarantee.
A lived detail: the phrase “minimally invasive” can make families relax too early. I’ve watched that relaxation collapse into confusion when the surgeon says, “You still need restrictions for a while.” Small incision, still major biomechanics.
“Who This Is For / Not For” (Quick Self-Sort, Not a Diagnosis)
Likely “for”: stable spine + leg symptoms + imaging match + failed conservative care
If you check these boxes, decompression without fusion is often on the menu:
- Leg-dominant symptoms (pain, heaviness, numbness) and reduced walking tolerance.
- Symptoms improve with sitting or bending forward.
- MRI/CT shows stenosis at a level that matches your pattern.
- Motion studies don’t show meaningful instability.
- Planned decompression doesn’t require removing too much facet/bone.
Likely “not for”: instability/deformity + back-dominant pain + wide decompression need
- Clear dynamic instability on flexion-extension X-rays.
- Significant deformity driving the stenosis.
- Back-dominant pain without a strong leg/walking pattern.
- Revision anatomy or wide decompression needs that threaten stabilizers.
Pattern interrupt: Here’s what no one tells you… “borderline stability” is a gray zone
Borderline stability is where anxiety lives rent-free. A low-grade slip can be stable in motion studies yet still be a risk if extensive facet removal is needed. This is why surgeon-specific planning matters. “Candidate” isn’t a label. It’s a forecast: “We think we can decompress you and keep you stable.”
- Stable segment on motion testing
- Leg/walking symptoms dominate
- Limited facet removal expected
Trade-off: Small chance of later needing fusion if instability develops or symptoms recur.
- Instability is present or likely
- Decompression must be wide
- Deformity or high-grade slip is driving symptoms
Trade-off: Bigger operation, longer recovery, and potential adjacent-level stress over time.
Neutral next action: Circle one bullet in each box that matches you. Ask the surgeon to confirm or correct your circles.
Common Mistakes: Fusion Panic, MRI Worship, and Other Expensive Detours
Mistake #1: Choosing based on a single word in a radiology report
“Severe.” “Advanced.” “Marked.” These words are not treatment plans. Ask: Which level? Which type of stenosis? Which nerve? Does it match my symptoms?
Mistake #2: Ignoring stability because “the MRI looks awful”
MRI is great at showing crowding. It’s not the best tool for showing motion. That’s why flexion-extension X-rays exist. Stability is a behavior, not just a picture.
Mistake #3: Skipping a second opinion when recommendations don’t explain the logic
If the recommendation arrives without reasoning, get a second opinion. Not because you’re difficult. Because spine decisions should be explainable. You’re allowed to ask for a logic chain.
Mistake #4: Confusing “minimally invasive” with “risk-free”
Small incision does not equal small stakes. Nerves don’t care how pretty the scar is. Ask about risks you can actually feel: persistent numbness, weakness, infection, spinal fluid leak, and the possibility of future surgery. And if you’re trying to separate nerve pain from “everything else that hurts,” this guide on what sciatica nerve pain actually feels like can keep your symptom description sharp.
A lived moment: I once heard someone say, “I want the surgery that lets me drive in a week.” The surgeon, deadpan but kind: “I want you to walk in ten years.” Different time horizons create different answers. If driving and sitting are your biggest fear points, read microdiscectomy sitting and driving guidance for the “how bodies behave in chairs” reality check.
Questions to Ask Your Surgeon: Get the Logic in Writing
“What level(s) are you decompressing, and why those?”
Ask for a level-by-level map. If they can’t connect your symptoms to levels, your plan is guessy. And guessy is not a vibe you want near your nerve roots.
“What’s my evidence of stability (or instability)?”
Make them name the test: flexion-extension X-rays, CT findings, facet integrity, slip grade, pars defects. You’re not asking to play surgeon. You’re asking for the reason you’re betting on “no fusion.” If your workup includes nerve testing, it helps to know when EMG timing is actually useful for sciatica.
“How much facet/bone removal do you anticipate?”
This is a sneaky-powerful question. The more facet removed, the more stability risk rises. Your surgeon’s answer will often reveal whether decompression-only is a confident plan or a tentative one.
“What would make you convert to fusion during surgery?”
Sometimes the plan changes if the anatomy forces wider removal or if the segment looks less stable than expected. Knowing the “convert triggers” helps you consent with eyes open.
The patient came in with a folder thick enough to qualify as a small textbook. MRI discs. Old PT notes. A handwritten pain diary. They’d been told “fusion” by one surgeon and “no fusion” by another, and the family was quietly unraveling at the edges.
The third surgeon didn’t start with a verdict. He asked for two numbers: “How far can you walk before you have to sit?” and “How long does it take to recover after sitting?” Then he pulled up the imaging and pointed, not at the dramatic phrases, but at a single level. “This is the pinch. Now let’s talk stability.”
They watched flexion-extension films together. “See how this barely moves? That’s why decompression-only is reasonable here. If it moved more, I’d fuse.” The room exhaled. Not because it was easy, but because it finally made sense.
Recovery Reality Check: What Outcomes to Expect (And What to Track)
Success is often walking distance + leg symptoms, not a perfect back
Many patients define success as: “I can walk again without that electric leg shutdown.” That’s a good definition. A perfect, silent back is not always realistic, especially if there’s arthritis, disc wear, or facet pain in the background. Decompression’s most reliable win is often leg function and tolerance.
Timeline markers: early nerve calm vs slow function rebuild
Nerves can calm quickly, but strength and endurance rebuild more slowly. Some people feel leg relief early. Others feel “different weird” first, then gradual improvement. Your surgeon will give specifics, but a useful mental model is: early symptom relief plus longer rehab for stamina and mechanics. If injections are part of your timeline, it helps to know the epidural steroid injection relief timeline and what “too soon to judge” really means.
What recurrence means: scar, progression, or missed level?
If symptoms recur, it doesn’t automatically mean “the surgery failed.” It can mean scar tissue, progression at adjacent levels, or an incomplete decompression. This is why documenting your symptom pattern before surgery matters. It gives you a baseline story that’s harder to dismiss later. (And if your symptoms jump back after an operation, this explainer on post-op sciatica rebound can help you frame what’s happening without panic.)
A lived recovery note: the most helpful tracker I’ve seen is embarrassingly simple, like something you’d scribble on a receipt. “Walked 6 minutes. Sat 2. Walked 6.” When the numbers start improving, your brain stops catastrophizing quite so loudly.
When to Seek Help: Red Flags You Don’t Monitor at Home
New bowel/bladder changes, saddle numbness, rapidly worsening weakness
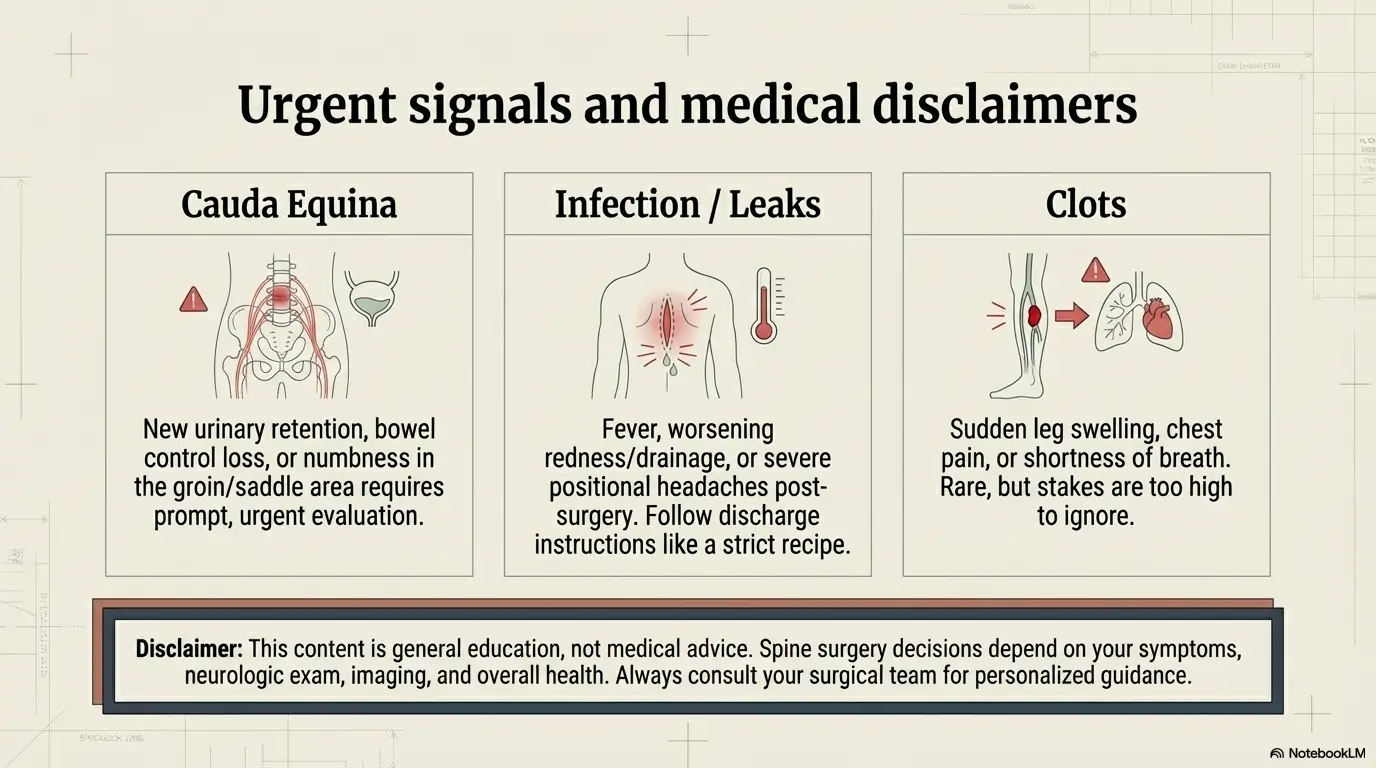
Some symptoms are “call now” symptoms, not “wait and see” symptoms. New urinary retention, loss of bowel control, new numbness in the groin/saddle area, or rapidly worsening weakness can signal cauda equina syndrome, which many spine and emergency guidelines treat as an urgent situation requiring prompt evaluation. If you want a clean checklist to keep near your phone, see cauda equina syndrome red flags.
Fever, wound drainage, severe headaches, uncontrolled pain after surgery
After surgery, fever, worsening redness/drainage, severe headache especially with positional changes, or pain that’s escalating rather than settling should be evaluated. Your discharge instructions will be specific. Follow them like they’re a recipe you don’t want to freestyle.
Sudden leg swelling/shortness of breath (urgent clot symptoms)
Sudden leg swelling, chest pain, or shortness of breath after surgery can signal a clot and needs urgent care. It’s rare, but the stakes are high enough that “rare” doesn’t mean “ignore.”
FAQ
Is decompression without fusion the same as laminectomy?
Often, yes in spirit: decompression is the goal, and laminectomy (or laminotomy) is a common way to achieve it. But “decompression without fusion” is broader and can include foraminotomy, laminotomy, and other targeted approaches depending on where the nerve is compressed.
How do doctors decide if I “need” fusion for stenosis?
The key driver is stability. Surgeons look for evidence of instability (including on flexion-extension X-rays), deformity drivers, and how much bone/facet needs to be removed to decompress the nerve. Fusion is more likely when instability is present or likely after decompression.
Can you have decompression only with spondylolisthesis?
Sometimes. Many patients with low-grade degenerative spondylolisthesis are treated successfully with decompression alone, especially when motion testing suggests stability and when decompression can preserve stabilizing structures. Some cases still benefit from fusion depending on instability risk and surgical plan.
What does “spinal instability” mean on flexion-extension X-rays?
It means the segment moves more than expected between bending forward and backward, suggesting the vertebrae aren’t holding a consistent relationship under motion. Your surgeon interprets this alongside symptoms, slip grade, facet integrity, and planned decompression extent.
Will decompression help back pain or mostly leg pain?
Decompression is most reliable for leg symptoms and walking tolerance when nerve compression is the main problem. Back pain can improve, especially if it’s tied to nerve irritation, but it’s less predictable because back pain has more possible generators than leg-dominant stenosis symptoms.
How long does decompression-only surgery take and is it outpatient?
Timing and setting vary by levels, approach, and health factors. Patient education sources like MedlinePlus note laminectomy often takes a few hours. Some cases are outpatient or short-stay, while others need longer observation, especially with multi-level decompression or medical complexity.
What are the chances I’ll need fusion later?
It depends on your stability risk, how many levels are decompressed, and how much facet/bone is removed. Studies show some patients later undergo additional surgery, sometimes conversion to fusion. Ask your surgeon for a personalized estimate and what would make that risk higher in your anatomy.
Next Step: One Concrete Action (Do This Before You Decide)
Request (or bring) MRI report + images + flexion-extension X-ray report and ask one surgeon to explain your case using: compression site + stability evidence + planned bone/facet removal in 3 bullets.
This is the highest-leverage move you can make in under 15 minutes: gather the documents and force the explanation to be specific. If a recommendation can’t be summarized in three bullets, it’s not ready to live in your body.
- Name the level(s) and the exact pinch location.
- Name the stability evidence (motion testing) in plain terms.
- Name how much facet/bone removal is expected and why.
Apply in 60 seconds: Draft an email subject line: “Please send MRI report + images and flexion/extension X-ray report.” Send it now.
Safety / Disclaimer (Short)
This content is general education, not medical advice. Spine surgery decisions depend on your symptoms, neurologic exam, imaging, and overall health. If you have new weakness, bowel/bladder changes, or numbness in the groin/saddle area, seek urgent evaluation.
Last reviewed: 2026-03-02.
