
Navigating Orthopedic Pain Management for Aging Parents
Orthopedic pain management for aging parents rarely falls apart because families do not care. It falls apart because the first few decisions get made in a fog of half-explained pain, crowded medication lists, delayed appointments, and one parent insisting they are “fine” while gripping the furniture like a handrail.
That is the hard part for adult children. You are not just dealing with knee pain, back pain, or arthritis. You are trying to figure out whether the real problem is pain, weakness, fall risk, poor sleep, unsafe stairs, or a growing loss of independence that nobody wants to name out loud.
Keep guessing too long, and families often lose time, money, and function before they ever get a clear plan.
This guide helps you sort what needs urgent attention, what can wait for a regular visit, what to track before the appointment, and when conservative care, imaging, physical therapy, or a specialist referral actually makes sense.
The goal is simple: help your parent move more safely and help you make calmer, smarter decisions with less waste.
It is built around real caregiving logistics, not fantasy medicine.
Less panic. • More traction.
Start with the symptoms that change the plan fastest. Then make the next appointment count.
Table of Contents

Start Here: Orthopedic Pain Management Gets Harder When You Are Helping Someone Else
Why adult children often inherit the logistics before they understand the pain
Orthopedic pain gets complicated the moment it stops being only about pain. You are not just noticing a sore knee or stiff back. You are watching what it does to stairs, sleep, bathing, car transfers, grocery trips, mood, pride, and family routines. Most adult children are handed the logistics first. The diagnosis arrives later, if it arrives clearly at all.
That is why this role feels so tiring. You are often building the bridge while standing on it. One parent says, “It’s fine,” while gripping the counter like it owes them money. Another says everything hurts, which is emotionally true but not medically specific. Somewhere in the middle, you are supposed to figure out what matters now, what can wait, and which next step is worth the effort.
The hidden challenge: your parent may describe pain, fear, and function as if they are the same thing
Older adults do not always separate symptoms neatly. “My hip is terrible” may mean pain in the joint, fear of falling, weakness from avoiding movement, poor sleep, or frustration at losing independence. Those are different problems. They may overlap, but they do not always point to the same next action. When families are sorting this out, a broader guide to orthopedic pain management for older adults can help frame the bigger picture without rushing to the wrong conclusion.
I have seen families lose two or three weeks arguing about the wrong thing. Everyone debated whether the pain was “bad enough,” but nobody asked whether the parent could get to the bathroom safely at night. That small functional question would have told the truth much faster than the debate did.
What “helping” should actually mean in this season of life
Helping does not mean taking over the steering wheel and calling it love. It means organizing information, noticing risk, protecting autonomy where possible, and making the next decision clearer. Good help is structured. It is not loud. It is not theatrical. It does not require a family summit every Tuesday.
- Ask what movement has become harder this week
- Notice what time of day the problem is worst
- Focus on the next useful step, not the entire future
Apply in 60 seconds: Ask your parent, “What one daily task feels hardest because of this?”
First Filter: What Needs Urgent Care and What Can Wait for a Regular Appointment
Red flags that should move you faster, not just worry you more
Not every orthopedic complaint is urgent, but some symptoms deserve faster evaluation because they can signal fracture, infection, significant nerve involvement, vascular compromise, or a sharp change in safety. The trick is to avoid two common family mistakes: panicking at everything and underreacting to the wrong thing.
Urgent evaluation matters more when pain follows a fall or injury and your parent cannot bear weight, when a limb suddenly becomes weak or numb, when new bowel or bladder changes show up with back symptoms, when fever appears with joint pain, or when swelling, redness, and worsening pain are moving fast. These are not “let’s see how tomorrow goes” situations. If the pain pattern has a spine component, the red flags in low back pain emergency signs and cauda equina syndrome red flags are especially worth knowing.
When swelling, weakness, falls, fever, or sudden loss of function changes the plan
Function is often the most honest alarm bell. A parent who could stand from a chair three days ago but now cannot do it safely has changed in a clinically meaningful way. A person who used to shuffle to the kitchen but now avoids walking altogether has crossed a line, even if they keep insisting it is “just old age.”
Falls deserve special respect here. Falls are not just background static in later life. They often create a loop: pain reduces movement, reduced movement weakens balance, weaker balance raises fall risk, and a fall makes everything harder. That loop can tighten quietly if nobody names it.
The quiet trap: assuming all age-related pain is “normal”
Many families lose time because they narrate symptoms as inevitable instead of evaluating them. Yes, osteoarthritis and degenerative change become more common with age. No, that does not mean severe pain, rapidly worsening weakness, repeated falls, or marked loss of self-care ability should be waved away like weather.
Normal aging is not the same thing as new disability. That sentence alone can save families from a lot of accidental neglect dressed up as realism.
- Yes: recent trauma plus inability to bear weight
- Yes: sudden numbness, weakness, or new bladder/bowel changes
- Yes: fever with joint pain or rapidly worsening swelling
- No: familiar chronic pain with no major change in function
- No: slow stiffness that is annoying but stable
Next step: If any “yes” item is present, escalate same day rather than trying to optimize a future appointment.
Before Booking Anything: Define the Real Goal of the Visit
Pain relief, walking tolerance, sleep, stairs, dressing, bathing, and independence are not the same target
Families often say they want “the pain fixed.” That sounds sensible, but it is not specific enough to guide care. Are you trying to help your parent sleep through the night, walk to the mailbox, get safely on and off the toilet, cook dinner without sitting every four minutes, or keep attending church without panic on the steps? Each target changes the shape of the plan.
A parent with knee pain who mostly wants to sleep may need a different first move than a parent whose main problem is unsafe transfers in the bathroom. Same body part. Different decision tree. In real life, the question can be even more specific, especially when the problem is night discomfort or bathroom safety, as in guides on hip pain at night or safer showering after hip surgery.
Why the best next step depends on the function your parent wants back
When function goals are clear, appointments get better. A clinician can work more efficiently when the question is concrete: “She cannot climb the six steps into her house without pulling on the railing and stopping halfway,” tells a richer story than “Her leg hurts a lot.” The second sentence is true. The first sentence is useful.
I once helped someone condense a messy five-minute pain monologue into one sentence: “He wants to walk from bedroom to kitchen without holding the wall.” The room changed. The appointment got practical. Everyone stopped orbiting vague distress and started talking about balance, strength, pain control, and home setup.
Let’s be honest: many appointments go sideways because nobody named the actual goal
It is very common to leave a visit with a recommendation that is technically reasonable and emotionally unsatisfying because the real family goal never made it into the room. If your parent’s deepest fear is falling in the shower, and the visit becomes a generic discussion of “joint pain,” everyone will leave with paperwork and very little relief.
Define the target before you define the treatment. It sounds simple because it is simple. It is also oddly rare.
Don’t Start Here: Common Mistakes Adult Children Make in Orthopedic Pain Management
Pushing for scans too early when the first question is still basic assessment
Adult children often arrive with admirable energy and a slightly chaotic shopping list. MRI, orthopedic referral, second opinion, braces, injections, surgery consult. The instinct makes emotional sense. Pain is upsetting. Movement loss is scary. Everyone wants to skip to the answer key.
But imaging early, before the first clinical question is clear, can add cost and noise without improving direction. Many musculoskeletal problems still need a careful history, focused exam, medication review, and function assessment first. A shiny scan cannot replace a foggy question. Families who are tempted to jump ahead may benefit from reading about when an MRI referral for orthopedic pain actually makes sense and what MRI pain mismatch can look like in practice.
Mistaking louder pain language for a clearer diagnosis
Some parents underreport pain because they do not want to “make a fuss.” Others report it in sweeping, intense terms because they are overwhelmed. Neither style gives a clean diagnostic map on its own. Families sometimes mistake emotional intensity for clinical precision. They are not the same thing.
Your job is not to police tone. It is to translate the story into concrete details: where it hurts, what movement triggers it, what has changed, how long it lasts, whether it radiates, whether weakness is present, and what daily task has become difficult.
Taking over so completely that the parent stops participating in their own care
This one arrives disguised as devotion. You fill every silence, answer every question, book everything, manage every pillbox, and suddenly your parent becomes a passenger in their own care. That can backfire. People are more likely to follow through when they feel respected, not managed like a late package.
The sweet spot is collaborative help. Not abandonment. Not command-and-control. More like: “I’ll help organize this, but your goals matter most.”
Show me the nerdy details
Orthopedic pain in older adults can overlap with medication side effects, neurological conditions, deconditioning, and fear-driven movement avoidance. That is one reason a careful symptom timeline and medication review often matter as much as the body part itself.
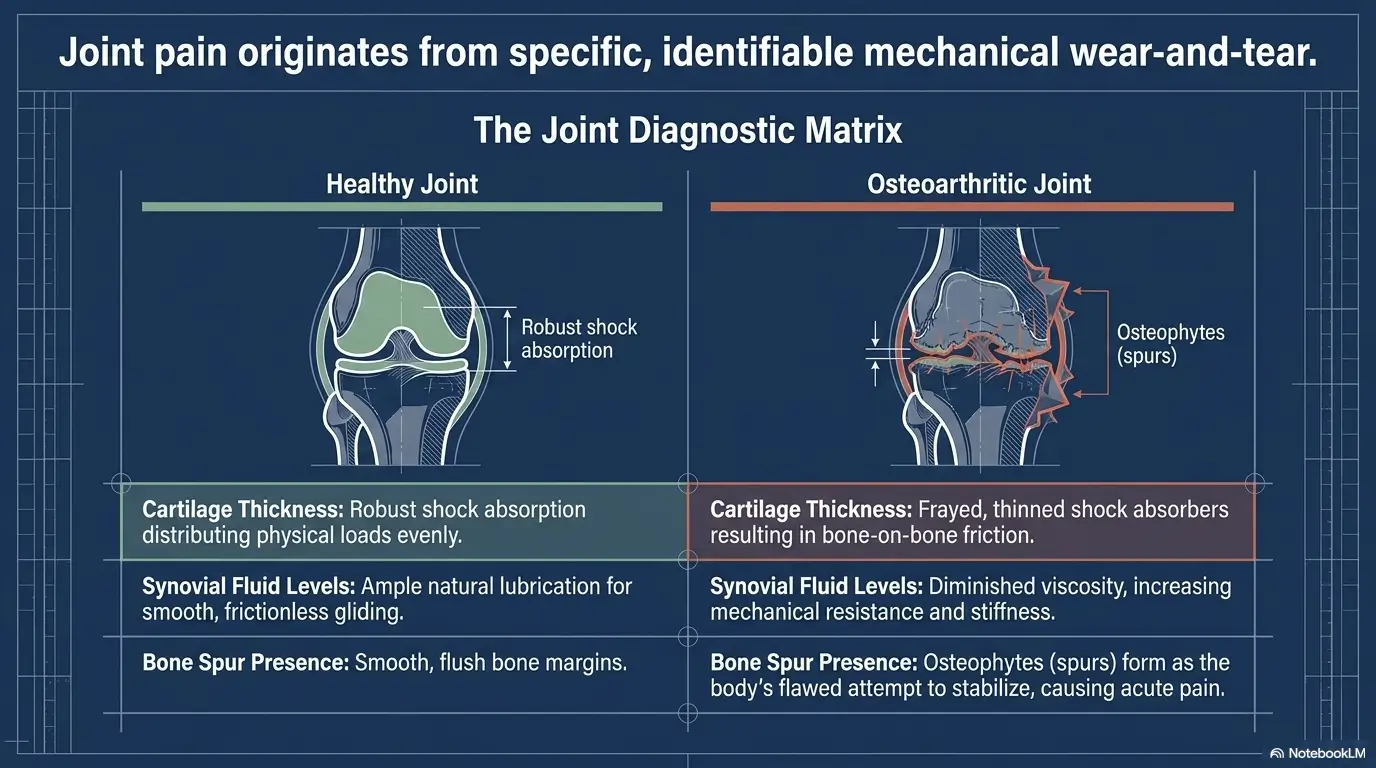
The Money Leak: How Families Overspend Before They Even Understand the Problem
Where costs pile up first in orthopedic care for older adults
Costs tend to leak in boring places. Duplicate visits. Imaging that does not change the plan. Brand-name gadgets bought in a 2 a.m. panic. Transportation arranged last minute. Prescriptions that clash with existing medications and then have to be reworked. None of this feels dramatic. That is exactly why it is expensive.
There is also the hidden cost of poor sequencing. If your parent sees three different clinicians without a clean pain story, medication list, and function goal, each visit starts near midfield instead of in scoring position. You pay in money, time, and energy.
Why “let’s just see a specialist” can be efficient or expensive depending on the situation
Sometimes seeing a specialist early is sensible. Clear joint instability, failure of conservative care, persistent function loss, or concern about fracture can justify a faster handoff. Other times, a primary care visit or geriatric-focused evaluation is the best starting point because the problem is not purely orthopedic. It may involve medication burden, balance risk, neuropathy, sleep loss, or several things at once.
A specialist is not automatically the premium lane. Sometimes it is simply a more expensive place to learn that the first question should have been different. Cost awareness matters even more for families navigating orthopedic pain management with a high deductible or trying to estimate HDHP imaging costs before agreeing to the next step.
How to ask what each visit, image, or therapy referral is meant to clarify
One sentence can reduce a lot of waste: “What question will this next step answer?” Ask it about X-rays, MRI, therapy, braces, injections, referrals, and follow-up timing. If the answer is fuzzy, that is information. If the answer is crisp, families usually feel calmer even when the plan is modest.
| When A | When B | Trade-off |
|---|---|---|
| Start with primary care when the picture is mixed, meds are complex, or function decline is broad | Start with orthopedics when there is strong suspicion of a structural joint problem or failure of initial care | Primary care may coordinate better; orthopedics may narrow body-part decisions faster |
Neutral action: Before booking, write down the one question you need answered by that appointment.
Who This Is For and Who It Is Not For
Best fit: adult children coordinating care, transportation, scheduling, and follow-up for aging parents
This guide fits the son, daughter, stepchild, in-law, niece, nephew, or family friend who has somehow become the default organizer. You are tracking appointments, asking follow-up questions, reviewing after-visit summaries, and trying to help a parent stay safe without making them feel infantilized. It also fits care coordinators and practical siblings who are tired of group texts that contain plenty of concern and very little usable information.
Not a fit: emergency situations, severe trauma, or symptoms that need immediate medical evaluation
If there is major trauma, inability to bear weight after a fall, sudden severe neurological change, fever with joint symptoms, chest symptoms, or acute confusion, this article is not the tool. That is not failure. It is just the wrong tool for the moment. A butter knife is helpful, but not for brain surgery. Same principle.
Also not a fit: families looking for a one-size-fits-all diagnosis from generalized internet advice
Orthopedic pain in older adults is shaped by comorbidities, existing medication use, prior surgeries, baseline mobility, cognition, home layout, fall history, and what the parent values most. A tidy internet script can support the process, but it cannot replace individualized medical care.
- Use it to prepare for visits
- Use it to notice risks and track function
- Do not use it to ignore red flags
Apply in 60 seconds: Decide whether your parent needs guidance, coordination, or urgent evaluation. Those are different jobs.
Pain Story First: What to Track Before the Appointment So the Visit Actually Helps
Location, duration, triggers, timing, mobility loss, and sleep disruption that matter clinically
The best home tracking is short, boring, and useful. Write down where the pain is, when it began, what makes it worse, what relieves it, whether it radiates, whether numbness or weakness appears, and which daily task is now harder. Add timing: morning stiffness, evening flare, pain after walking, pain at night, pain with stairs, pain when standing up, pain after sitting too long.
Sleep deserves a line of its own. Night pain changes the caregiving burden because it steals recovery, worsens irritability, and makes everything feel more catastrophic by breakfast. A parent who slept badly for four nights will describe the world differently than one who slept well.
Which home notes are useful and which turn into clutter
You do not need a spreadsheet worthy of a space launch. In fact, too much tracking often becomes clutter. Twenty-three screenshots and a six-minute voice memo are not the triumph they appear to be. Useful notes usually fit on one page.
- Pain location
- Function problem
- Start date or timeline
- Triggers and relief
- Falls or near-falls
- Current meds tried and effect
Here’s what no one tells you: a clean two-minute pain summary can save an entire visit
A clean summary sounds like this: “For three weeks, her right knee hurts mostly when standing up and going down stairs. She has had two near-falls, sleeps worse because turning in bed hurts, and acetaminophen helps a little. Her goal is to walk from the bedroom to the mailbox safely.”
That is gold. It tells the room what changed, how it behaves, how serious the functional impact is, and what success looks like. It also keeps the visit from dissolving into family weather reports.
- A current medication list, including over-the-counter pain relievers
- Prior imaging or surgery history if known
- One-page symptom summary
- One functional goal
- One safety concern, such as stairs or falls
Neutral action: Put the page in your phone notes and print one copy if possible.
Don’t Confuse Speed With Progress: When Imaging Helps and When It Mostly Adds Noise
What X-rays, MRI, and other tests may answer in common orthopedic complaints
Imaging can be useful, but it should answer a question. X-rays may help evaluate fractures, alignment issues, or degenerative joint change. MRI may help when soft tissue injury, persistent neurological symptoms, or a more detailed look at structures is needed. Other tests may enter the picture when symptoms suggest something broader than a straightforward orthopedic problem.
That said, more detail is not always more clarity. A scan can produce impressive language while leaving the practical question untouched: what should we do next, and will it help this parent function better? Families wrestling with this choice often benefit from a plain-English comparison of MRI versus X-ray and a guide to what counts as failed conservative care before MRI.
Why age-related findings on imaging do not always explain the pain
Older adults often have age-related changes on imaging, and not every abnormal-looking image explains today’s symptoms. This is one reason clinicians often care so much about symptom pattern and exam findings. The picture on the screen is part of the story, not the whole plot.
I think of this as the haunted attic problem. If you go looking hard enough, you will find old stuff. The presence of old stuff does not always explain the noise downstairs.
How to ask whether a test will change treatment, not just produce more paper
Ask, “If this test shows what you suspect, how would treatment change?” That question protects families from testing that is interesting but not actionable. It also helps distinguish reassurance-testing from decision-shaping testing.
Imaging is a tool, not a trophy. Families do better when they remember that.
Show me the nerdy details
For older adults, the value of imaging depends heavily on red flags, duration, neurological findings, trauma history, and whether conservative care has already been tried. A good ordering question is not “Can we get a scan?” but “What management decision depends on the result?”
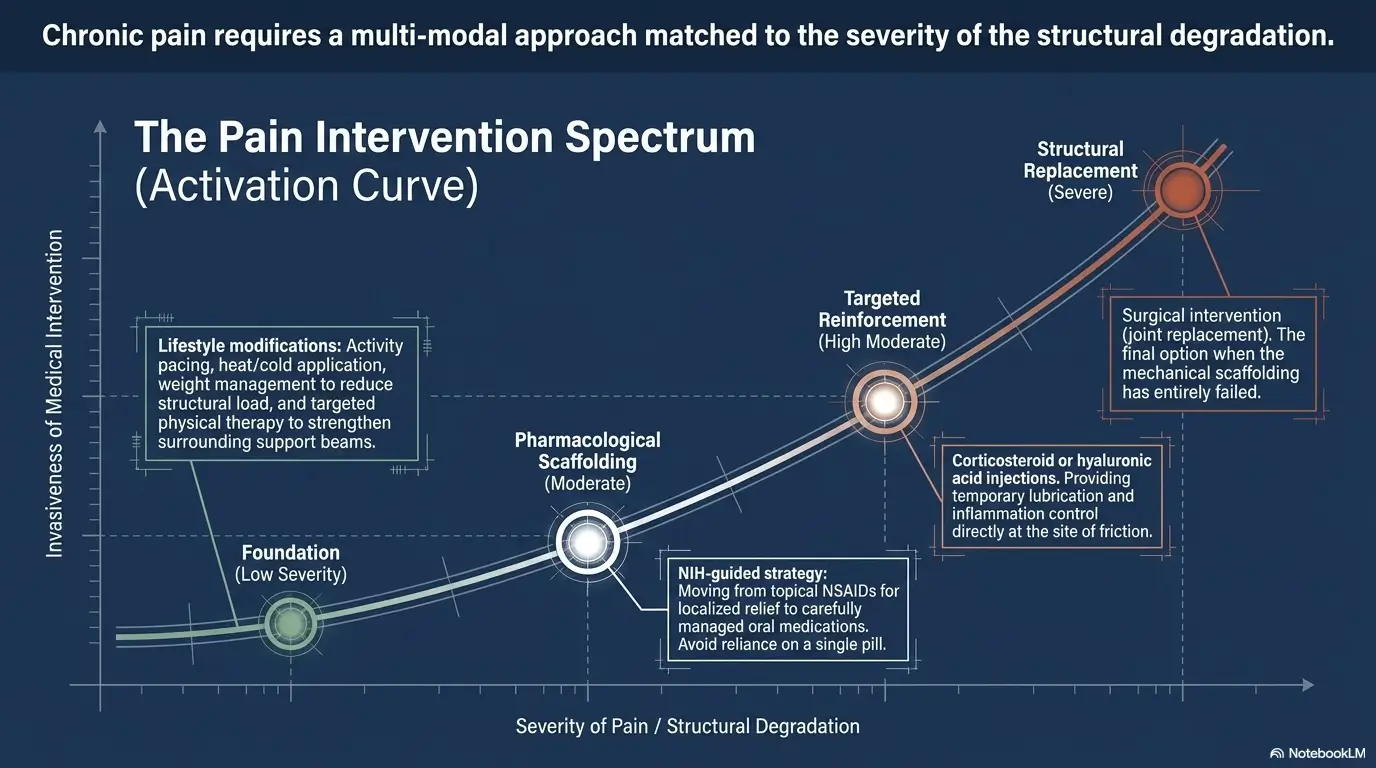
The Care Ladder: What Conservative Orthopedic Pain Management Often Looks Like First
Activity modification, medication review, physical therapy, assistive devices, and home adjustments
Conservative care is not a consolation prize. For many older adults, it is the most sensible first ladder: adjust aggravating activities, review medications for safety and interaction issues, consider physical therapy, use assistive devices appropriately, and make small home changes that reduce risk and strain.
Those home changes are rarely glamorous. Better lighting. A steadier chair. Fewer throw rugs. A railing that actually deserves the name. Shoes that stop auditioning as banana peels. But these details often matter more than families expect, especially when pain and fall risk are tangled together. When braces or supports enter the conversation, it also helps to know what HSA-eligible braces and supports or a hinged knee brace for stairs can and cannot realistically do.
Why small changes in movement and setup can matter more than dramatic treatment ideas
The internet loves drama. Real caregiving often runs on modest improvements. A parent who can transfer more safely, sleep one hour longer, and walk ten extra steps without bracing against the wall may not feel like a cinematic success story, but those gains can change the week. Sometimes they change whether the family can keep supporting care at home.
When “watch and reassess” is responsible rather than dismissive
Families understandably dislike plans that sound passive. “Watch and reassess” can feel like the medical version of a shrug. But when the clinician has looked for urgent problems, clarified function, and started a measured plan, reassessment can be responsible. It creates room to see what actually changes with time, therapy, safer movement, or medication adjustment.
The key is that the reassessment plan should be concrete. Not “good luck out there.” More like: what to try, what to avoid, what warning signs change the timeline, and when to follow up if function is not improving. If therapy becomes part of that first ladder, families may also want to understand Medicare Part B physical therapy coverage and the difference between physical therapy copay versus coinsurance.
- Review current pain medicines and interactions
- Protect safety during walking, transfers, and bathing
- Measure success by function, not by dramatic language
Apply in 60 seconds: Pick one home friction point, such as stairs or getting out of bed, and write it down as a treatment target.
Family Dynamics Matter: How to Help Without Slipping Into Parent-Child Warfare
Respecting autonomy when your parent resists advice, exercises, or follow-up
Pain can make people prickly. So can fear. So can being told what to do by someone they still remember driving to kindergarten. Many adult children run straight into this wall. They become more urgent. The parent becomes more resistant. Suddenly everyone is arguing about a walker like it is a political ideology.
The answer is not to become passive. It is to shift from command language to choice language where possible. Adults usually tolerate guidance better when it sounds like collaboration instead of correction.
How to speak in choices instead of commands
Instead of “You need to do physical therapy,” try “Would you rather start with one visit to learn safe exercises, or talk first with your doctor about what would make therapy feel worth it?” Instead of “Stop doing that,” try “Which feels safer right now, the hallway rail or a chair closer to the bed?”
These are not soft, decorative phrasing changes. They are practical tools for preserving dignity. Dignity is not extra credit in caregiving. It affects follow-through.
The emotional layer: pain can sound like stubbornness when it is really fear
Fear hides in strange costumes. Sometimes it looks like avoidance. Sometimes it looks like irritability. Sometimes it looks like, “I’m not going to some doctor just for this,” when what the person means is, “I am afraid of hearing what this could become.”
One of the most useful shifts a family can make is asking, “What feels scary about this?” You may hear something practical, like fear of surgery, or something tender, like fear of losing independence. Either answer changes the care conversation in a way brute efficiency never will.
Good caregiving is part logistics, part translation, part diplomacy. A little less courtroom. A little more jazz trio.
Common Mistakes That Make Follow-Through Collapse After the Appointment
Leaving without clear instructions on timing, dosage, activity limits, or return precautions
Many families survive the appointment and then trip over the aftermath. Nobody is quite sure how long to try the plan, whether a medication is scheduled or as-needed, what activity should be limited, or which warning signs should speed up follow-up. This is how “We thought we were doing what they said” enters the chat.
Before leaving, make sure you can answer these questions in plain English:
- What are we trying first?
- For how long?
- What should improve if this is working?
- What should we stop doing?
- What symptom means we should call sooner?
Forgetting to reconcile orthopedic advice with existing medications and other conditions
Older adults rarely arrive as blank slates. They may already have kidney concerns, blood pressure issues, anticoagulant use, sleep medications, diabetes, balance problems, or memory issues. Those realities can change what is safe, practical, and tolerable. A decent pain plan on paper can become a terrible plan in context if nobody checks the bigger picture.
This is one reason bringing a current medication list matters so much. “I think she takes the little white one” has not yet matured into a medical record.
Treating one better day as proof that the whole problem is gone
Families love hope. Sensible families also love patterns. One good day does not always mean recovery, and one bad day does not always mean disaster. Look for trend lines in pain, walking, transfers, sleep, and stability. That broader view protects against both premature victory laps and unnecessary doom spirals.
- How many days was walking clearly worse than baseline?
- How many nights did pain disrupt sleep?
- How many near-falls or unsafe moments happened?
Output: If two or more of these categories are worsening, the current plan may need reassessment rather than more patience.
Neutral action: Bring this 7-day snapshot to the next visit.
The Specialist Question: When It Is Time to Escalate Care
Signs that conservative care is not enough
Escalation makes sense when the current plan is not restoring function, when weakness or instability is growing, when falls keep happening, when pain remains severe despite reasonable first-line care, or when the diagnostic picture stays muddy after initial evaluation. Families often ask, “How long should we wait?” The better question is, “What has improved, and what has not?”
If the answer is “almost nothing,” and the parent is still struggling with basic movement or self-care, it is time to rethink the lane. In some cases that means comparing a pain clinic versus an orthopedist, and in others it means learning what pain management before a cortisone injection should look like before moving further up the ladder.
How worsening weakness, instability, repeated falls, or persistent function loss changes the threshold
Weakness is a particularly important turning point. Pain alone can slow someone down. Pain plus true weakness, instability, or repeated falls changes the stakes. The threshold to escalate should also drop when the parent’s world is shrinking fast: they stop leaving the house, stop bathing safely, stop cooking, or stop trusting their own movement.
What to bring so the referral visit starts further down the field
Bring the symptom timeline, current medication list, past imaging if available, a short record of what treatments have already been tried, and one clear functional goal. If you show up with organized information, the referral visit often starts at a more useful depth. That matters. Specialist visits can feel like short windows in a windy hallway.
The purpose of escalation is clarity and better function, not the emotional thrill of “finally seeing someone.” That thrill wears off quickly if the handoff is sloppy.
When to Seek Help
Seek urgent medical care for severe injury, inability to bear weight after trauma, sudden numbness or weakness, new bowel or bladder changes, fever with joint pain, or rapidly worsening symptoms
This is the bright-line section. If your parent has severe injury, cannot bear weight after trauma, develops sudden numbness or weakness, has new bowel or bladder changes with back symptoms, or develops fever with joint pain, do not rely on home optimization. Seek urgent medical care.
Contact a clinician sooner if pain is interfering with walking, sleep, self-care, or safe movement at home
Even when it is not a same-day emergency, earlier evaluation matters when pain is clearly interfering with walking, sleep, bathing, dressing, transfers, or safe movement around the home. Those are not minor quality-of-life footnotes. They are decision signals. When sleep disruption becomes part of the burden, families often also need strategies used in pain management for seniors waiting on joint care.
Reassess the plan if treatment is continuing but daily function is not improving
Persistence deserves respect, but persistence without progress should trigger reevaluation. If treatment is underway and daily function is still flat or worsening, ask whether the diagnosis, treatment sequence, home setup, or referral pathway needs to change. The goal is not to be impatient. It is to avoid losing a month to inertia.
Good caregiving is calm, but it is not sleepy.
FAQ
Should I take my parent straight to an orthopedic specialist or start with primary care?
It depends on the question you need answered. Start with primary care when the picture is mixed, medications are complicated, or the issue may involve more than one system. Start with orthopedics sooner when there is clear joint-specific dysfunction, suspected structural injury, or poor response to initial conservative care.
When is an MRI actually necessary for an older adult with joint or back pain?
An MRI is most helpful when the result will change management. It is often more useful after a clinician has clarified symptoms, examined the parent, and decided what question the scan needs to answer. It is less useful as a reflex when the problem is still broadly defined. If insurance becomes the obstacle, a practical next read is what to do after an MRI denial appeal for orthopedic pain.
What questions should I ask at the first orthopedic appointment for my parent?
Ask what diagnosis is most likely, what urgent problems have been ruled out, what the first treatment target is, what the parent should avoid, what would count as improvement, and what warning signs should trigger earlier follow-up. Also ask what the next step would be if the first plan does not work.
How can I help my aging parent describe pain more clearly to the doctor?
Focus on location, timing, triggers, relief, weakness or numbness, falls, sleep disruption, and the one daily task that has become hardest. A short function-based summary is usually more useful than a dramatic but vague description.
What if my parent refuses physical therapy or home exercises?
Try to find out what they are resisting. Sometimes it is pain, sometimes transportation, sometimes embarrassment, and sometimes fear that the exercise will make things worse. Ask what would make it feel more doable. One visit for coaching may feel less threatening than an open-ended commitment.
How do I know whether pain is serious or part of normal aging?
Age-related pain can be common, but new disability, repeated falls, rapidly worsening symptoms, marked weakness, fever, or major changes in function are not things to dismiss as normal aging. Function loss is often the clearest signal that more evaluation is needed.
Can orthopedic pain cause falls even if the pain seems manageable?
Yes. Even moderate pain can alter gait, confidence, reaction time, and willingness to move normally. That can raise fall risk, especially when combined with weakness, balance issues, sedating medications, poor lighting, or clutter at home.
What should I track at home before a visit for knee, hip, shoulder, or back pain?
Track the body area involved, when symptoms started, what movements trigger pain, what relieves it, whether sleep is affected, whether numbness or weakness occurs, whether falls or near-falls have happened, what medications have been tried, and what daily task has become difficult.
Next Step: Build a One-Page Orthopedic Visit Sheet Before the Next Appointment
Write down the pain location, function problem, symptom timeline, current meds, prior imaging, and top three questions
This is the practical ending because practical endings travel best into real life. Build a one-page visit sheet. Put the pain location at the top. Then the main function problem. Then the timeline. Then current medications, including over-the-counter pain relievers. Then prior imaging or surgeries if known. Then the top three questions you need answered.
That one page reduces repetition, sharpens appointments, and helps any sibling or caregiver step in without recreating the family archaeology from scratch.
Bring one family member, one short symptom summary, and one realistic goal for the visit
Too many voices can clutter the room. Too few details can waste it. Aim for one support person, one short summary, and one realistic goal. Think “help her get in and out of the shower safely,” not “fix everything before summer.” Ambition is lovely. Specificity is lovelier.
Good caregiving starts with a clearer question, not a louder scramble
This is the curiosity loop from the beginning, tied shut neatly at last. The families who do this best are not always the most medically knowledgeable. They are the ones who learn to ask better questions, observe function honestly, respect urgency when it appears, and keep the next step small enough to carry.
In the next 15 minutes, make the page. Write the goal. List the meds. Note the safety concern. That tiny act turns vague worry into usable traction. And in caregiving, traction is a beautiful thing.
Last reviewed: 2026-04.
This article is for educational purposes and care-navigation support only. It is not diagnosis or individualized medical advice. Orthopedic pain in older adults can overlap with neurological, vascular, infectious, medication-related, and balance-related issues, so families should use clinical evaluation when needed and seek urgent care for warning signs.
