
Shoulder Immobilizer vs. Sling: Choosing the Path to Real Recovery
A shoulder immobilizer versus sling sounds like a small equipment choice until it starts stealing sleep in 45-minute chunks and turning basic tasks like dressing, bathing, or standing up from bed into a clumsy little crisis. In shoulder pain management, the real issue is rarely which device feels nicer for ten minutes.
It is which one reduces the right kind of pain without creating a fresh parade of neck strain, elbow stiffness, swelling, or accidental movement. This distinction matters more than most people expect. A sling can ease the dead-weight drag of the arm, while an immobilizer better limits the tiny motions that make post-op or post-injury pain flare.
The Precision Method
- ● Start with the pain pattern.
- ● Look at the hidden trade-offs.
- ● Notice what daily life is trying to tell you.
Because sometimes the device is not wrong. Just the fit. Or the timing. Or the reason you are wearing it in the first place.
Fast Answer: Orthopedic pain management with a shoulder immobilizer versus a sling is not only about support. It changes posture, sleep, elbow stiffness, hand swelling, skin irritation, and how much the shoulder is truly protected from accidental movement. In general, an immobilizer restricts motion more and may be used when protection matters most, while a sling often allows easier daily function but can invite more unwanted movement. The right choice depends on diagnosis, surgeon instructions, pain pattern, and recovery stage.
Table of Contents
Start With the Real Question: What Pain Are You Trying to Prevent?
Rest pain and movement pain are not the same problem
Many people talk about “shoulder pain” as if it were a single weather system. It is not. Some pain shows up when you are perfectly still, especially late at night when the room goes quiet and the shoulder begins its own sad violin solo. Other pain only appears when the joint shifts, when the arm hangs, when you turn too quickly, or when you reach without meaning to. Those are different problems, and they do not always respond to the same device.
A sling may reduce the heavy dragging sensation that comes from letting the arm dangle. An immobilizer may reduce the sharper, more alarming pain that comes from tiny shoulder motions after surgery or instability. The device is not the goal. The goal is to match the device to the kind of pain that keeps ruining your day.
Protection pain versus pressure pain: one device can solve one and worsen the other
Here is the annoying truth: the thing protecting your shoulder can also irritate your neck, elbow, wrist, or skin. That is why some people say, “The immobilizer helps my shoulder, but now everything else is filing complaints.” They are not imagining it. A more protective setup can calm motion pain and still create pressure pain from straps, posture, heat, and stillness.
Why “more support” does not always feel better by nightfall
Early in recovery, “more support” sounds obviously better. By 9:30 p.m., after your neck has been pulling overtime and your elbow feels like a stiff hinge, it may not feel so noble. I have seen people assume the device failed when the real problem was more specific: the shoulder felt safer, but the rest of the arm had been parked too long in an awkward position. Recovery is often less dramatic than people expect. It is a long negotiation with position, timing, and patience.
- Sharp pain after tiny movements usually points toward a protection problem
- Dull ache, neck tension, or swelling may point toward a fit or positioning problem
- “More support” is not automatically “less pain” across the whole arm
Apply in 60 seconds: Write down whether your pain is worse at rest, with accidental movement, or after wearing the device for two hours.
Device First, Pain Second? That Is Where People Get Stuck
A shoulder immobilizer limits more motion, but may increase neck, elbow, or wrist discomfort
An immobilizer usually holds the arm more securely against the body and limits shoulder movement more than a basic sling. That extra control can matter after certain surgeries, fractures, or instability episodes, when even a small motion can feel like a rude telegram from the joint. But extra control has a cost. The elbow stays bent longer. The forearm stays parked. The neck may start bracing. Fingers may puff up if the arm sits too dependent or the straps are off.
A sling can feel simpler, yet it sometimes allows the exact small movements that keep pain simmering
A sling often feels friendlier. It is quicker to put on, easier to tolerate, and less like you have been strapped into a cautious origami project. But simple is not always sufficient. Some slings allow subtle shoulder movement during walking, turning in bed, or rising from a chair. Those motions may look trivial from the outside. The shoulder may disagree quite strongly.
Let’s be honest… the most comfortable setup in minute one may not be the safest by day three
This is the trap. People often choose the device that feels nicer in the first 20 minutes rather than the one that protects the tissue best over 3 days, 2 weeks, or the full healing window. In some cases, a sling that feels less annoying can invite more accidental movement and a longer pain spiral. In other cases, an immobilizer that is theoretically correct becomes miserable because it is fitted badly and never adjusted.
The right answer is often boring: it depends on the diagnosis, timing, fit, and what your orthopedic team actually told you to do. If you are still earlier in the decision chain and trying to build a calmer baseline first, it helps to review a broader framework for orthopedic pain management before treating the device as the only lever you have.
Decision card: When A versus B
More likely to need an immobilizer now: pain spikes with tiny shoulder motion, recent surgery, recent dislocation, fracture care, strong surgeon emphasis on protection.
More likely to tolerate a sling better: the arm feels heavy when unsupported, the main misery is fatigue or neck strain, and your clinician has said that simpler support is appropriate for this stage.
Neutral action: Match the device to the recovery phase, not to impatience.
Shoulder Immobilizer Versus Sling: What Actually Changes in Daily Life
Sleeping posture, recliner setups, and why nighttime is often the tiebreaker
Night is where theories go to be tested. A device can seem manageable at noon and completely intolerable at 2 a.m. because sleep adds stillness, swelling, awkward turning, and the strange vulnerability of half-waking with the urge to roll over. An immobilizer may protect better if your problem is accidental movement during sleep. A sling may feel less claustrophobic but sometimes leaves the arm less secure.
Mayo Clinic’s shoulder replacement guidance notes that an immobilizer is used to keep the shoulder from moving after surgery, and it advises supporting the elbow slightly in front of the body with towels or blankets during rest or sleep for comfort.
Dressing, bathing, and toileting: the quiet tasks that expose the real burden
Daily life is where dignity and engineering meet, often without adequate rehearsal. Getting dressed with one arm can feel like folding a fitted sheet while mildly offended. A more restrictive device can protect you beautifully and still make bathing, toileting, and clothing changes much harder. That matters, because pain management is not only about pain intensity. It is also about compliance. If a setup is so frustrating that you keep removing it during high-risk moments, the protection advantage starts to leak away.
Walking around the house: balance, arm weight, and the tug on your neck
Walking seems simple until the shoulder joins the conversation. If the arm hangs and tugs, a sling may bring immediate relief by taking weight off the shoulder. If walking causes subtle joint motion and zings of pain, an immobilizer may feel more secure.
The best setup is often the one that makes you walk normally again instead of curling around the shoulder like you are protecting a secret. When posture collapses, pain tends to spread north and south. That is one reason readers who are also fighting desk-triggered neck tension may recognize overlap with neck and shoulder pain from laptop work.
AAOS explains that some shoulder trauma is treated with a sling or shoulder immobilizer along with icing and pain medication, and that choice reflects the injury pattern rather than a one-size-fits-all rule.
Eligibility checklist
- Yes / No: Does your pain jump mainly with accidental shoulder movement?
- Yes / No: Does your current device create finger swelling, neck guarding, or skin burn?
- Yes / No: Are you removing the device during bathing, dressing, or nighttime turns more than instructed?
Neutral action: If you answered “yes” to two or more, bring those exact problems to your orthopedic follow-up instead of saying only, “It hurts.”
Pain Pattern Clues: When the Immobilizer May Feel More Necessary
Post-op instability fears and accidental reaching
Some recoveries are less about comfort and more about protection. After certain repairs or acute injuries, the shoulder is not asking for freedom. It is asking for stillness. If you keep getting sudden pain when you forget yourself and reach, brace, push up from a chair, or turn quickly, that is a clue. The immobilizer may feel more necessary because it does more of the behavioral policing for you.
I once watched a family member insist she was “barely moving it” while using the hand to steady a bathroom door. The shoulder had a different opinion. Tiny motions can matter a lot when tissue is fresh and irritated. Recovery has a talent for punishing confidence before it rewards it.
Sharp pain with tiny shoulder motions rather than dull ache at rest
This is an important distinction. If the shoulder hurts in a sharp, bright way when the joint shifts even slightly, more rigid protection may be helping for a reason. A sling can support arm weight, but in some cases it does not stop the particular motions that provoke pain. An immobilizer often aims at that problem more directly.
Why “I only moved a little” can still matter in early recovery
Early healing does not care whether the motion felt small to you. It cares whether the tissue was ready for it. That is why week one and week four can feel like different countries, not neighboring streets. A person may feel better enough to get casual right before the shoulder is actually ready for that casualness. This is where rebound pain begins: not with a dramatic accident, but with a dozen tiny liberties.
Show me the nerdy details
After shoulder surgery or instability treatment, pain can reflect both tissue irritation and protective muscle guarding. A more restrictive device may reduce micro-movements that the patient barely notices but that still trigger pain. The trade-off is prolonged elbow flexion, altered scapular posture, and pressure from straps. “Less pain right now” and “better protection this week” are not always the same metric.
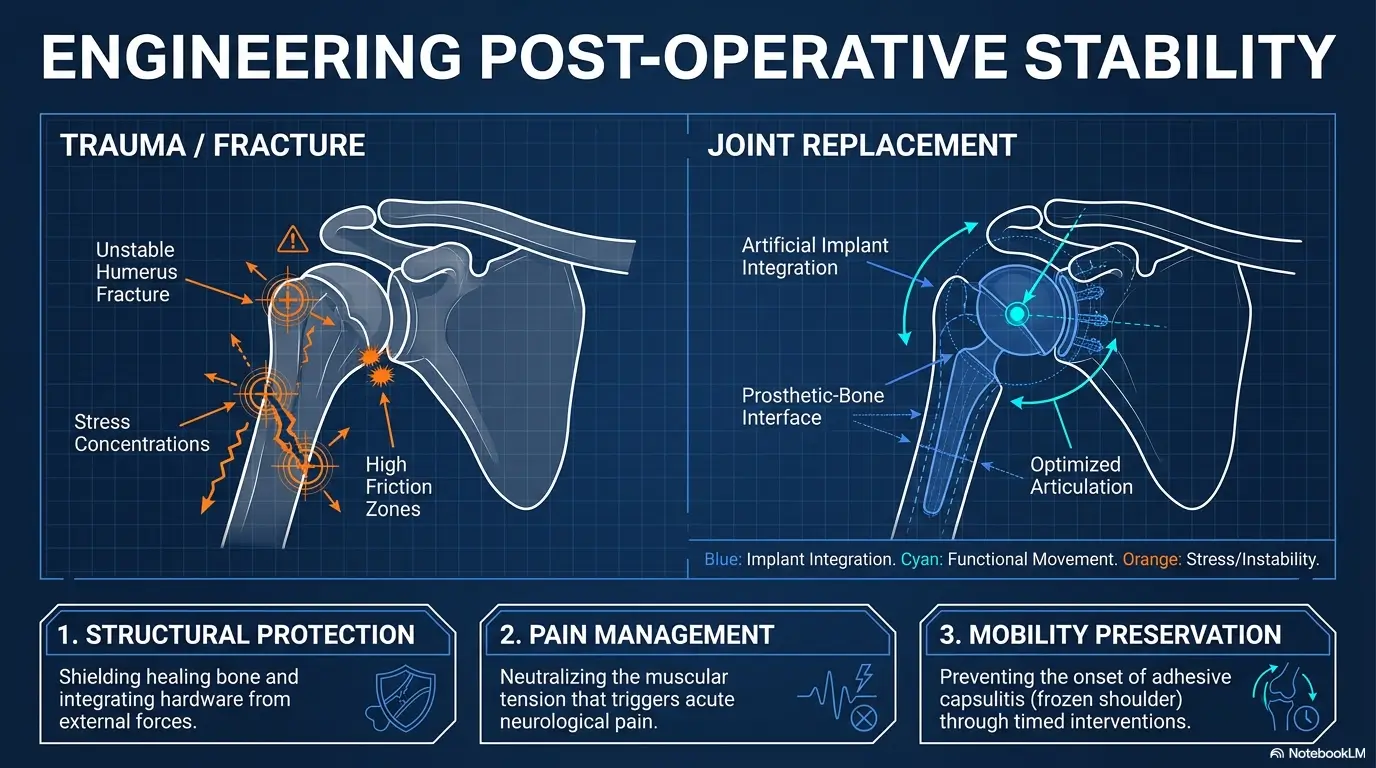
Pain Pattern Clues: When a Sling May Feel More Manageable
When the bigger issue is arm heaviness, fatigue, and strain from letting the arm hang
Sometimes the shoulder is less angry about motion than it is exhausted by gravity. The arm feels heavy, the upper back tightens, the neck starts clenching, and by afternoon you are tired in the very specific way that only prolonged guarding can create. In those moments, a sling can feel more manageable because it solves the drag problem without the full burden of a bulkier immobilizer.
When swelling, skin irritation, or neck tension becomes the louder complaint
If the shoulder itself is calmer but your fingers are swelling, your neck is hard as a broom handle, or your skin is hot and irritated under straps, the current setup may be creating secondary misery that now deserves attention. That does not automatically mean the device type is wrong.
It may mean the fit is wrong, the position is wrong, or the arm needs better support under the forearm and wrist. Still, in the right recovery stage, a sling may indeed be the more manageable option. If your home workstation or daily posture is also feeding the neck side of the problem, articles on neck pain from laptop work can help separate device strain from background strain.
Why simpler support sometimes improves compliance
This part is not glamorous, but it matters. A device only works when it is worn correctly and consistently. If a setup is so maddening that you keep loosening it, removing it, or cheating during routine tasks, the theoretical benefit shrinks. A simpler sling may produce better real-world results when the clinical situation allows it because the patient will actually use it the way the plan intended.
- Better comfort can improve compliance
- Better compliance can reduce avoidable flare-ups
- Comfort alone is not proof the shoulder is ready for less protection
Apply in 60 seconds: Ask yourself whether your main pain is “the shoulder moved” or “everything around the shoulder is getting overworked.”
Who This Is For, and Who It Is Not For
This is for patients comparing shoulder immobilizer versus sling after injury, surgery, or orthopedic evaluation
If you are trying to understand why one device seems to help one kind of pain but worsen another, you are in the right place. This article is for the person who is doing their best, still confused, and a little tired of being told “just wear the sling” as if that sentence answered anything meaningful.
This is for caregivers trying to reduce pain flare-ups without guessing
Caregivers often see the practical problems first. They notice the midnight struggle in bed, the way the fingers look puffier after dinner, the grimace during dressing, or the sudden pain after an “easy” trip to the bathroom. Good caregiving in shoulder recovery is rarely dramatic. It is mostly noticing patterns before those patterns become setbacks.
This is not for replacing surgeon-specific instructions after repair, fracture, or dislocation
This matters enough to say clearly. If your surgeon, orthopedic PA, or fracture clinic gave device-specific instructions, those instructions outrank generic internet wisdom every time. Different procedures and injuries have different motion restrictions, timelines, and risk profiles. Shoulder repair, fracture care, and instability treatment do not share one universal script, and pretending otherwise is how people get into avoidable trouble. For readers who are still deciding where to be seen in the first place, comparing urgent care versus an orthopedic clinic can be a more useful next step than changing devices on your own.
Quote-prep list: What to gather before comparing advice
- Your diagnosis or procedure name
- What week of recovery you are in
- Whether pain is worse at rest, movement, or after device wear
- Any hand swelling, numbness, or skin breakdown
Neutral action: Bring these four items to your next orthopedic call or visit.
The Hidden Trade-Off: Better Protection Can Create New Pain
Elbow stiffness, forearm tightness, and hand swelling from staying still too long
A shoulder device can protect one joint while making the rest of the limb grumpy. Elbow stiffness is common when the arm stays bent for long periods. The forearm can feel tight. The hand may swell, especially if the limb stays dependent or the fit is off. This does not always mean the plan is wrong. It may mean the arm needs better support, more careful positioning, and the exact movement routine your clinician approved for the elbow, wrist, and hand.
Strap pressure, skin heat, and brachial-plexus-style discomfort that should not be brushed off
Straps can dig. Fabric can heat up. The neck can start guarding. Occasionally, patients describe tingling or odd nerve-like discomfort around the shoulder and arm. That is not a detail to shrug off with heroic optimism. “Toughing it out” is not a treatment plan. If the device is leaving marks, worsening symptoms, or making the arm feel wrong in a new way, the fit deserves a second look.
Here’s what no one tells you… sometimes the device is correct, but the fit is wrong
This is one of the most common hidden issues. People assume they are choosing between two concepts, when in practice they are often suffering from one bad fitting. A well-fitted immobilizer and a sloppy immobilizer are almost different experiences. The same is true for slings. The device may be clinically appropriate, but if the forearm is not supported, the shoulder is not positioned well, or the straps are pulling unevenly, pain control gets distorted and everyone blames the wrong villain.
AAOS notes that immobilization devices are meant to hold injured structures in place while they heal, but prolonged immobilization can also contribute to loss of strength and stiffness, which is why timing and follow-up matter.
Infographic: Shoulder Immobilizer vs Sling at a Glance
Shoulder Immobilizer
- Usually more motion restriction
- Often better for accidental-movement pain
- May feel bulkier at sleep and hygiene tasks
- More likely to create elbow/neck complaints if fit is poor
Sling
- Usually easier for daily use
- Often better for arm-heaviness relief
- May allow more small shoulder movement
- Can be easier to wear consistently if allowed clinically
Bottom line: Choose based on the pain pattern, diagnosis, and recovery stage, not on which one annoys you less in the first ten minutes.
Common Mistakes That Make Shoulder Pain Harder to Control
Wearing the device loosely enough that the shoulder still shifts
If the shoulder keeps moving inside a device, you are getting the inconvenience without the full protective benefit. That is a rude bargain. A loose setup can allow the exact tiny motions that trigger pain during walking, transfers, and sleep. Patients often think, “At least it’s on,” but the shoulder is not always impressed by technicalities.
Wearing it so tightly that fingers swell, skin burns, or the neck starts guarding
The opposite mistake is cinching everything down like a suitcase that has offended you personally. Too tight can be just as unhelpful. Swollen fingers, burning pressure, heavy neck guarding, or new numbness are clues that the setup needs review. Good support is firm and stable, not punishing.
Taking it off “just for a minute” during the exact activities most likely to trigger pain
People are often most tempted to remove the device during bathing, clothing changes, transfers, and nighttime repositioning. Unfortunately, those are also the moments when awkward movements multiply. The “just for a minute” logic is how a surprisingly large number of flare-ups begin.
Treating all post-injury shoulder pain as inflammation when posture and device fit may be the real culprit
Not every bad evening means more inflammation. Sometimes it means the forearm was unsupported for hours, the pillow setup was sloppy, or the strap line was pulling the neck into a defensive crouch. Medication matters, ice matters, but mechanical problems often need mechanical fixes. A shoulder does not care how sincerely you believed the issue was only inflammation. That same principle shows up in broader guides on pain management before asking for an injection, where mechanics and timing often matter more than people expect.
- Too loose means more unwanted motion
- Too tight means swelling, guarding, and pressure pain
- Removing it during risky tasks can undo a calm day fast
Apply in 60 seconds: Check whether your fingers look puffier and whether the forearm feels truly supported all the way to the wrist.
Do Not Copy Someone Else’s Recovery Timeline
Rotator cuff repair, fracture, dislocation, and strain do not follow the same rules
This is where internet advice goes slightly feral. One person says they switched to a simple sling at 10 days. Another says they slept flat at 2 weeks. Another claims they were “basically normal” in no time, which is either unusually lucky or suspiciously selective storytelling. Different diagnoses create different rules. A strain is not a dislocation. A fracture is not a repair. A repair is not a replacement. The device choice sits inside that reality.
Week one and week four are different countries, not neighboring streets
It is tempting to think healing is a smooth slope. It often is not. One week may be dominated by protection and swelling. A later week may shift toward stiffness management and function. That is why copying someone else’s timeline is such a poor sport. The calendar matters, but the tissue story matters more.
Why pain improvement does not automatically mean tissue is ready for less protection
Pain is useful information, but it is not the entire vote. A shoulder can feel better before the tissue is truly ready for less support. That is not unfair. It is just biology refusing to read motivational quotes. Feeling better is wonderful. It is not always permission. When people get stuck in that gap between symptom improvement and actual readiness, it can also help to understand why pain can continue even when an X-ray looks normal.
Coverage tier map for your own thinking
Tier 1: Severe pain with tiny movement, fresh injury or surgery, strong need for protection
Tier 2: Protection still matters, but swelling and comfort management become more visible
Tier 3: Transition conversations begin, only if your clinician says the tissue is ready
Neutral action: Ask what stage you are in, not just what device you have.
Sleep, Ice, Medication, Positioning: What Helps No Matter Which Device You Wear
How to support the forearm and wrist so the shoulder is not carrying dead weight
One of the quietest pain-control wins is supporting the forearm and wrist properly. When those are left hanging or poorly propped, the shoulder ends up carrying a dead-weight feeling that can ruin an otherwise decent setup. This is especially noticeable by late afternoon and bedtime, when small mechanical annoyances become large emotional events.
Ice timing, medication timing, and why stacking relief beats chasing pain late
Pain control usually works better when it is planned than when it is heroic. Waiting until pain is already loud often leads to a longer, rougher evening. Many patients do better with a repeatable rhythm around rest, approved medications, icing, and pillow positioning rather than improvising after the shoulder has already become offended. This is not glamorous. It is effective precisely because it is boring. Readers dealing with the financial side of repeat visits, meds, braces, and follow-ups may also want a practical guide to orthopedic pain management with a high deductible plan.
Recliner versus bed: choosing the setup you can repeat, not the one that sounds ideal
Some people sleep better in a recliner for a while because it reduces rolling and makes it easier to protect the shoulder. Others do fine in bed with wedges and pillows. The “best” setup is the one you can repeat for several nights without turning the whole household into an overnight engineering lab. Fancy plans fail when they are too hard to maintain at 1:40 a.m. If sleep setup is becoming the real battleground, a separate guide on recliner versus bed after shoulder surgery can help you think through the trade-offs more carefully.
Short Story: A friend recovering from shoulder surgery kept changing pillow systems every night, convinced the perfect arrangement was one more folded blanket away. By night four, the bedroom looked like a linen closet had exploded. What finally helped was not a miracle wedge. It was a simpler routine. Medication on time.
Ice before the pain ramped up. One pillow supporting the forearm, one behind the trunk, and one rule: no experimental rolling at 3 a.m. Within two nights, the shoulder was not pain-free, but it was far less dramatic. That tiny shift mattered. She stopped waking up angry at the device and started seeing the real issue: the shoulder needed consistency more than novelty.
Show me the nerdy details
Pain control after shoulder injury or surgery is often additive. Positioning reduces mechanical strain. Proper device fit reduces accidental motion. Ice may reduce localized discomfort. Medication timing can prevent pain escalation. None of these alone is magical, but together they can lower the total pain load enough to improve sleep and daily function.
Mistakes People Make When Switching From Immobilizer to Sling
Switching because of annoyance rather than clinical timing
The desire to switch devices is often completely understandable. Recovery gear is rarely chic, elegant, or pleasant. But timing still matters. Changing devices because you are annoyed is emotionally reasonable and medically unreliable. The better question is not, “Am I sick of this?” It is, “Has the reason for stricter protection actually changed?”
Confusing better mobility with true healing progress
Feeling more mobile can be deceptive. The joint may move more easily before it is ready to tolerate that movement well. Patients sometimes interpret freedom as healing proof. Sometimes it is healing. Sometimes it is simply reduced guarding plus increased risk. That is not the same thing.
The rebound pain that appears after a “small freedom” experiment
This pattern is almost theatrical in its predictability. A patient loosens the plan a little, feels fine for an hour, and then gets punished by evening. The conclusion is often, “Something strange happened.” Usually something very ordinary happened.
The shoulder tolerated a bit less protection worse than expected. That rebound pain can be a useful clue, not just a miserable surprise. In that stage, it may also help to understand what it means when physical therapy is not helping orthopedic pain yet, because “not better yet” and “ready for less support” are not the same sentence.
AAOS advises that if you need to be in a sling, you should not drive, which is a reminder that even “simple” sling phases still signal real limitation and incomplete readiness.
When to Seek Help Instead of Adjusting the Device Again
Numbness, tingling, blue fingers, major swelling, or worsening hand symptoms
There comes a point where the correct response is no longer “try another pillow” or “loosen the strap a bit.” If the hand is changing color, the fingers are swelling significantly, or numbness and tingling are worsening, that needs attention. Do not keep re-engineering the setup in silence while hoping the body becomes less interested in circulation and nerves.
Fever, drainage, severe skin breakdown, or pain that suddenly spikes without explanation
These are not details to bury in your own private recovery diary. Fever, drainage, severe skin irritation, or sudden unexplained pain spikes deserve medical contact, especially after surgery. Recovery does include discomfort. It should not include a steady expansion of red flags while everyone pretends the pillows will sort it out.
Inability to control pain even with prescribed measures and correct positioning
If you are using the device as instructed, positioning carefully, taking prescribed measures, and pain is still spiraling, it is time to call. Some problems are fit problems. Some are timeline problems. Some need a clinician’s eyes, not another evening of internet research with your shoulder perched like a reluctant sculpture. If access is part of the delay, it may help to review what to do during orthopedic referral wait times or decide whether telehealth versus in-person orthopedics makes sense for the problem you are seeing.
- Circulation or nerve symptoms deserve prompt attention
- Fever, drainage, and major skin breakdown are not “normal annoyance”
- Uncontrolled pain despite correct use deserves a call, not more guessing
Apply in 60 seconds: If a symptom would worry you in someone you love, treat it as worth reporting in yourself.
FAQ
Is a shoulder immobilizer better than a sling for pain?
Not automatically. An immobilizer may help more when tiny shoulder movements are the main trigger. A sling may feel better when the bigger problem is arm heaviness, fatigue, or strap burden. “Better” depends on the diagnosis, recovery stage, and whether protection or comfort is the main issue.
Why does my neck hurt more in an immobilizer?
Because the device changes posture and how the arm’s weight is carried. If the straps pull awkwardly or the forearm is not well supported, the neck and upper back can start guarding. Sometimes the device is correct but fitted poorly.
Can a sling make shoulder healing slower?
It can be less protective than an immobilizer in some situations, but that does not mean it is wrong. Healing risk depends on the injury or surgery and what your clinician intended the device to do. A sling is not “bad.” It is simply less restrictive in many cases.
How tight should a shoulder immobilizer feel?
Secure enough that the arm is supported and the shoulder is not shifting around, but not so tight that fingers swell, skin burns, or numbness increases. A good fit feels stable, not punishing.
Why does my elbow hurt when I keep my shoulder still?
Because prolonged bent-elbow positioning can create stiffness and tightness downstream from the shoulder. The elbow, forearm, wrist, and hand often notice immobilization even when the shoulder is the original patient.
Can I sleep flat with a sling or immobilizer?
Some people can later in recovery, but many do better at first with a more upright setup such as a recliner or extra pillows. Sleep position depends heavily on the procedure or injury and the timing. Feeling brave at bedtime is not the same as being ready.
Is more pain normal when switching from immobilizer to sling?
It can happen. Sometimes the shoulder reacts to the change in support with rebound pain, especially if the switch happened too early or the shoulder still needed stricter protection. Increased pain is useful information, not a moral failure.
Should I ice over or under the sling?
Follow your clinician’s directions and protect the skin. In general, many people find they need to position the cold source so it reaches the painful area without creating awkward pressure. What matters is safe use and consistent timing, not theatrical dedication to being cold.
Next Step: Do This Before Changing Devices on Your Own
Write down your pain in three buckets today: at rest, during accidental movement, and after wearing the device for two hours
This tiny exercise is more useful than another hour of vague worry. You are trying to identify the real driver: resting pain, motion pain, or device-related discomfort. Once you separate those, the conversation with your orthopedic team gets dramatically better. Suddenly you are not just saying, “It hurts.” You are saying, “It is worst after two hours in the device,” or, “It spikes when the shoulder shifts even a little.” That is actionable.
Check for fit problems before assuming the device itself is wrong
Before you decide the entire category of device is failing you, check the simpler culprits. Is the forearm fully supported? Is the wrist hanging? Are the fingers swelling by evening? Does the shoulder still shift when you walk?
Is the strap line pulling your neck into a knot? A surprising number of bad device experiences are really bad fit experiences in disguise. And if you are at the stage where device questions are starting to blend into imaging questions, it can help to read about orthopedic pain management before asking for an MRI or when an MRI referral for orthopedic pain is more likely to make sense.
Bring that pain pattern to your orthopedic visit so the discussion starts with function, not guesswork
The goal is not to win an argument with the device. It is to get a recovery setup that protects healing and makes daily life livable. In the next 15 minutes, jot down your three pain buckets, note any swelling or skin issues, and list the top two activities that cause flare-ups. That turns the next visit from a foggy complaint session into a useful clinical conversation. The curiosity loop from the beginning closes here: the question was never “Which device is better in general?” It was “Which problem is my shoulder actually having right now?”
Mini calculator: Is your current setup costing you sleep?
If your shoulder wakes you 3 times a night and each wake-up costs roughly 15 minutes to settle again, that is 45 minutes of lost rest. Over 5 nights, that becomes nearly 4 hours.
Neutral action: Treat better positioning and better fit as recovery tools, not optional luxuries.
Last reviewed: 2026-04.
Safety / Disclaimer
This article is for educational purposes only and is not medical advice. Shoulder injury and post-op instructions in the United States vary by diagnosis, procedure, surgeon protocol, and timing. For sudden worsening pain, numbness, color change, fever, drainage, chest symptoms, major swelling, or other concerning symptoms, contact your orthopedic team promptly or seek urgent care.
