
Beyond the Temporary: Navigating the Cortisone Decision
Relief can make a bad plan look smart for about a week. That is the quiet risk when a cortisone injection starts to feel like the next obvious move.
If you are weighing orthopedic pain management before deciding on cortisone injection, you are probably already in the hardest part of the process: the gray zone where pain is real, daily function is shrinking, and certainty is in short supply. Maybe rest helped a little. Maybe physical therapy stalled. Maybe joint pain, swelling, or nerve-like symptoms have blurred into one exhausting wish for something that works.
The cost of guessing is not just lingering pain. It is delaying the right diagnosis, masking a problem that needs a different fix, or wasting a short relief window with no rehab plan behind it.
This guide helps you sort the decision more safely and more clearly. You will be able to tell when conservative care still deserves a fair shot, when imaging or a sharper workup matters, and when a cortisone injection may actually fit the problem instead of merely interrupting it.
It stays grounded in the real decision points clinicians use: diagnosis, inflammation, timing, function, and what happens after relief.
Because this is where the choice gets better.
Not louder.
Just clearer.
Before the shot, name the problem. Then decide what the pain relief is actually for.
Table of Contents

Before the Shot, Ask What Problem You Are Actually Treating
Why “pain relief” and “correct diagnosis” are not the same job
Pain has a talent for blurring categories. A swollen knee after overuse, a catching shoulder, and sciatica that feels like a firewire down the leg can all end up in the same exhausted sentence: “I just need this to stop.” But pain relief and diagnosis are different jobs. One calms the alarm. The other finds the wiring problem.
A cortisone injection can be useful when inflammation is part of the picture. It is less magical when the main issue is instability, a large tear, infection, fracture, or a nerve problem that needs a different plan. Mayo Clinic’s patient guidance is very plain about this point: cortisone shots can reduce inflammation and symptoms, but they also carry risks and do not repair tissue simply because the pain drops.
I have seen this logic trap in ordinary life far from medicine. A door that squeaks gets oil. A door with a cracked hinge needs a screwdriver and sometimes a new hinge. Both are “door problems,” but one is maintenance and the other is structure. Joints, tendons, bursae, and spines are annoyingly similar. They share a ZIP code. They do not share the same fix.
How orthopedic pain management changes when the pain is inflammatory, mechanical, or nerve-related
A good orthopedic evaluation quietly sorts pain into buckets. Inflammatory pain often comes with swelling, warmth, stiffness, or a flare pattern that responds to anti-inflammatory treatment. Mechanical pain acts more like a protest during specific movements, loads, or positions.
Nerve-related pain travels, burns, tingles, or produces weakness that feels out of proportion to ordinary soreness. The category matters because cortisone is strongest as an anti-inflammatory tool, not a universal translator for every kind of pain. AAOS explains that these injections are intended to reduce inflammation in a targeted area, which is helpful when the diagnosis and target are reasonably clear.
Why a cortisone injection can feel decisive even when the diagnosis is still blurry
The shot feels decisive because it is concrete. It has a date, a needle, a room, a bill, a story. Rehab, load management, and diagnostic patience feel less cinematic. Yet the less dramatic steps are often where the real information lives. Does pain improve when stairs, overhead reaching, gripping load, or sitting time change? Does strength improve when movement is modified? Does a brace shift symptoms or merely hide them? Those clues matter.
Sometimes an injection is used partly as a diagnostic aid, but even that only answers a narrow question about pain origin. It does not automatically reveal the full “why.” AAOS notes that, in some shoulder conditions, a corticosteroid injection may help reduce inflammation and can aid diagnosis if the source of pain is unclear.
- Pain relief is not the same as tissue repair
- The diagnosis should shape the timing
- Inflammatory, mechanical, and nerve pain behave differently
Apply in 60 seconds: Write down whether your pain is worse with load, with rest, with certain positions, or with swelling. Bring that pattern to your visit.
Who This Is For, and Who Should Not Use This as Their Main Decision Tool
Best for adults weighing a cortisone injection for joint, tendon, bursa, or spine-related pain
This guide fits adults stuck in the gray zone: too symptomatic to ignore, not yet certain that an injection is the right move, and trying to avoid a reflex decision made on a bad pain day. It is especially useful if you have already tried some combination of rest, medication, or physical therapy and still do not know whether the next move should be injection, more conservative care, or a stronger diagnostic workup.
Useful for patients who have already tried rest, medication, or physical therapy and still feel stuck
“Stuck” is a real clinical state even if it sounds like a diary entry. Maybe the pain is not catastrophic, but it keeps stealing walks, sleep, stairs, training, childcare, or basic work tasks. Maybe you improved 20 percent and then plateaued for weeks. That is often the moment when people start shopping for certainty. Fair enough. The trick is not to confuse discomfort with direction. A better question is this: what information is still missing?
Not enough for medical emergencies, major trauma, infection concerns, or rapidly worsening neurologic symptoms
This should not be your main decision tool if the problem may be urgent. A hot, red, swollen joint with fever is not a “maybe later” situation. Rapid weakness, loss of bowel or bladder control, new numbness in the groin area, or inability to bear weight after a real injury is not a slow blog-read problem either. Even reputable patient guidance warns about joint infection and nerve-related concerns as situations that need prompt attention rather than casual symptom suppression.
- Yes / No: Has a clinician clearly named the likely structure involved?
- Yes / No: Have you tried at least one meaningful conservative step for long enough to judge it?
- Yes / No: Are you free of red-flag symptoms like fever, major trauma, or progressive weakness?
- Yes / No: Do you know what the injection is supposed to accomplish if it works?
Neutral next step: If you answered “no” to two or more items, the better next move may be diagnostic clarification rather than a fast injection decision.
Red Flags First, When “Wait and See” Is the Wrong Move
Signs the pain may be more than routine orthopedic inflammation
There is ordinary orthopedic pain, and then there is pain behaving badly. Night pain that is severe and escalating, fever with joint pain, a hot swollen joint, sudden major weakness, or inability to bear weight after injury should move you out of self-management mode quickly. These are the moments when a cortisone discussion can become a distraction from the more urgent question of whether something more serious is unfolding. Mayo Clinic lists joint infection among the notable risks and reasons clinicians weigh injections carefully rather than casually.
When swelling, heat, fever, or instability changes the decision tree
Swelling alone does not make the case, but swelling plus heat, redness, fever, or a joint that feels unstable changes the tone of the room. Infection, acute injury, or major internal derangement do not get better simply because inflammation is muted for a while. That is why pain masking too early can occasionally complicate the story. It is not that cortisone is “bad.” It is that timing matters more than people admit.
Why masking pain too early can occasionally delay the right treatment
Here is the unglamorous truth. Pain can be a useful instructor for a short while. Not pleasant. Useful. If you remove the pain before you have established what load, movement, or structure is driving it, you may end up returning to the exact activity that keeps feeding the problem. I once watched a friend take the “great, it feels better” route after a sports injury and celebrate by doing exactly what had irritated it in the first place. The body, ever the dry comedian, responded with a much ruder encore a week later.
Fever, hot joint, major trauma, rapid weakness, bowel or bladder changes, or inability to bear weight push you toward prompt evaluation.
Joint, tendon, bursa, ligament, disc, or referred pain. The target matters more than the pain score alone.
Load change, rehab, medication, bracing, sleep tweaks, and footwear often reveal the pattern.
A shot works best when you know why you are using it and what plan begins the moment relief arrives.
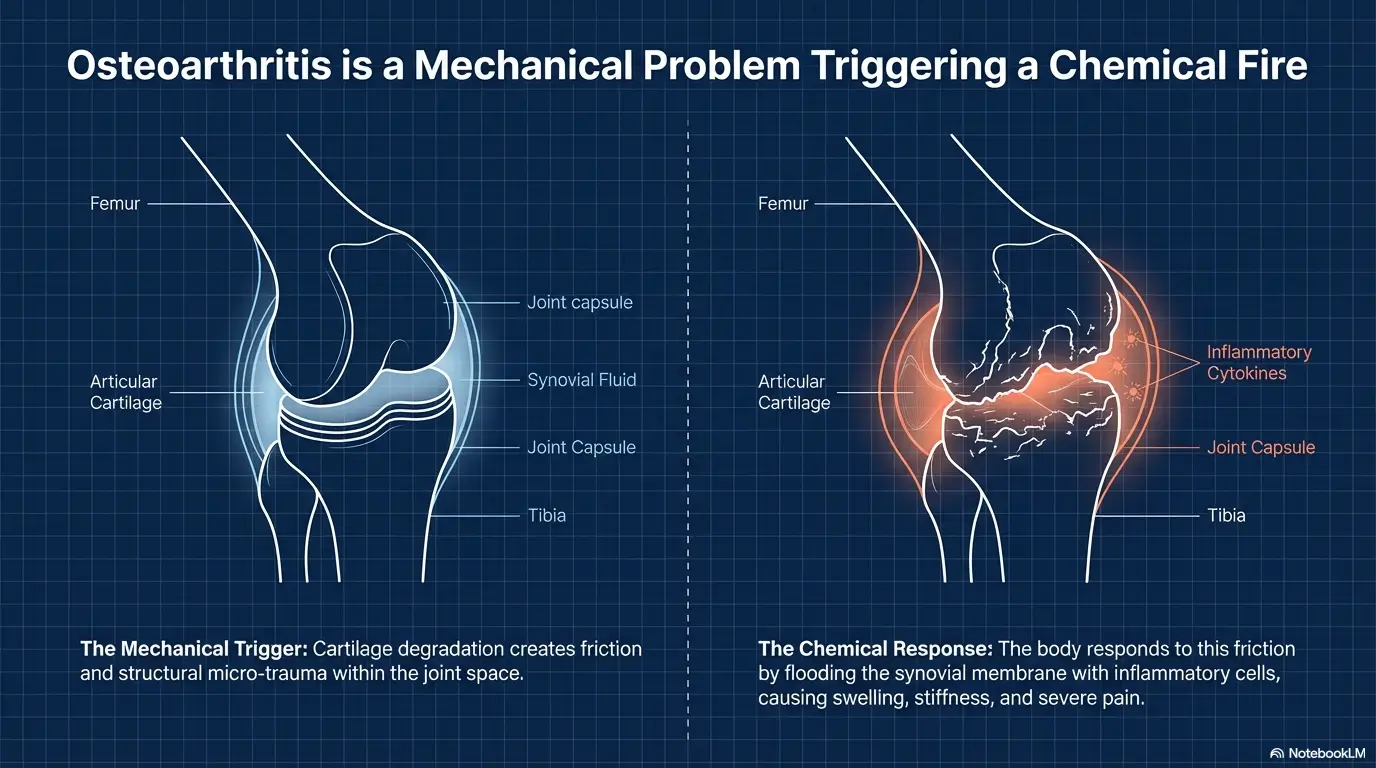
Diagnosis Before Relief, What a Good Workup Should Clarify
Whether the pain source is joint, tendon, bursa, ligament, disc, or referred pain
A useful orthopedic workup does not worship imaging, but it does respect anatomy. The point is to identify the most likely pain generator. Is this a joint full of inflammatory irritation? A tendon that hates load and compression? A bursa inflamed by friction? A disc or nerve root talking through the leg? Referred pain from elsewhere? You do not need a perfect answer on day one, but you do need a working hypothesis strong enough to justify the treatment being proposed.
When exam findings matter more than the pain score alone
Pain scores are helpful in the same way weather apps are helpful. They tell you something real, but not the whole story. A clinician learns a great deal from location, weakness pattern, range-of-motion limits, locking, giving way, numbness, swelling, and which positions reproduce symptoms. That is why the best visits feel slightly old-fashioned. Someone actually watches you move. Elegant, radical stuff.
When imaging helps, and when it only creates noise
Imaging can be useful when the diagnosis is uncertain, red flags are present, trauma matters, or management decisions hinge on structural information. But imaging is not automatically the hero. NICE guidance on osteoarthritis is notably cautious, explaining that routine imaging often does not guide non-surgical management and can add noise when the clinical picture is already clear. In other words, a scan can be important, but a scan can also become a fancy detour. If your next step depends on documenting failed conservative care or understanding how scans can mislead as much as they clarify, it can help to review what “failed conservative care” usually means before MRI approval and why MRI findings and pain do not always match cleanly.
Here’s what no one tells you… a shot can sometimes answer “where” the pain is, but that does not automatically answer “why”
If a well-placed injection calms pain in one structure, that may support the idea that the structure mattered. Helpful, yes. Complete, no. You can still have an underlying loading error, degenerative process, tear, movement deficit, or instability issue that needs a broader plan. Pain reduction can tell you where the smoke is. It does not always tell you what lit the match.
Show me the nerdy details
Image findings and pain do not always move in lockstep. Some structural changes show up in people with little pain, while some intense pain states have relatively modest imaging findings. That is why orthopedic decision-making often combines symptom pattern, exam, duration, function loss, and response to initial care rather than chasing one “perfect” picture.
Conservative First, What Orthopedic Pain Management Usually Tries Before Injection
Activity modification, unloading, and why “rest” is often too vague to be useful
“Rest” sounds wise and turns useless surprisingly fast. Does it mean no gym? Fewer stairs? No kneeling? Different shoes? Less overhead work? Shorter walks? Better sleep positioning? If the advice is vague, the results are usually vague too. Conservative care works best when it becomes specific enough to test. Change the aggravating load, protect the structure just enough, then reintroduce demand with intention.
Physical therapy, mobility work, and strength rebuilding as decision-making tools, not just treatment
Physical therapy is not merely something you try before “the real thing.” Often it is part of the diagnostic process. If hip strength changes knee pain, if scapular mechanics change shoulder pain, if nerve-glide work alters leg symptoms, the body is giving you information. Even when the injection still ends up being useful, therapy can tell you how to use the post-injection window wisely instead of wasting it on unplanned optimism. For readers trying to place this in a broader framework, a fuller guide to orthopedic pain management can help connect the injection question to the larger treatment sequence.
Oral or topical anti-inflammatory options and their tradeoffs
Oral and topical anti-inflammatory treatments can reduce pain enough to support rehab and function, but they also come with tradeoffs. Some people cannot use them easily because of stomach, kidney, bleeding, blood pressure, or medication issues. This is where a clinician’s judgment matters. A shot is not automatically “stronger and smarter.” Sometimes it is simply different. NICE guidance for osteoarthritis places topical and oral options within a broader stepped plan rather than treating injections as the first dramatic move.
Bracing, footwear, sleep position, and other low-drama fixes that quietly matter
These are the almost insulting fixes because they look too small to be important. Then they matter. A brace can alter load. Footwear can calm a grumpy chain reaction from foot to knee to hip. A pillow between the knees or under the arm can make the night less punitive. No one likes admitting that a 30-second setup change helped more than a heroic internet rabbit hole, but bodies are often practical before they are poetic. If pain is stealing sleep, the pattern may overlap with the problems described in hip pain at night, where positioning and nighttime mechanics often matter more than people expect.
| Situation | Usually worth prioritizing |
|---|---|
| Diagnosis still fuzzy | Exam, rehab trial, targeted workup |
| Pain tied to predictable movement or load | Activity change plus therapy |
| Short-term inflammation flare blocking rehab | Consider injection as a bridge |
Neutral next step: Match the tool to the job. Ask whether the goal is diagnosis, symptom control, or access to rehab.
Not So Fast, When a Cortisone Injection May Be Too Early
Why injecting before rehab, diagnosis, or load management can backfire
When a shot happens before the care plan is ready, it can create a shiny pause and very little progress. Pain improves. Nothing else changes. Then the same movement, same overload, same sleep setup, same weakness pattern, or same training mistake comes back to collect rent. The problem is not the injection itself. The problem is the emptiness around it.
Situations where short-term relief may tempt patients into overuse
This is a common script. The injection calms pain. The patient feels grateful and slightly invincible. Daily tasks expand. Rehab gets skipped because the body seems “fixed.” Then symptoms return because what improved was irritability, not necessarily capacity. If a clinician suspects that pain relief will trigger overuse in a vulnerable tendon or joint, timing the shot without clear restrictions can be unwise.
How temporary improvement can create false confidence about healing
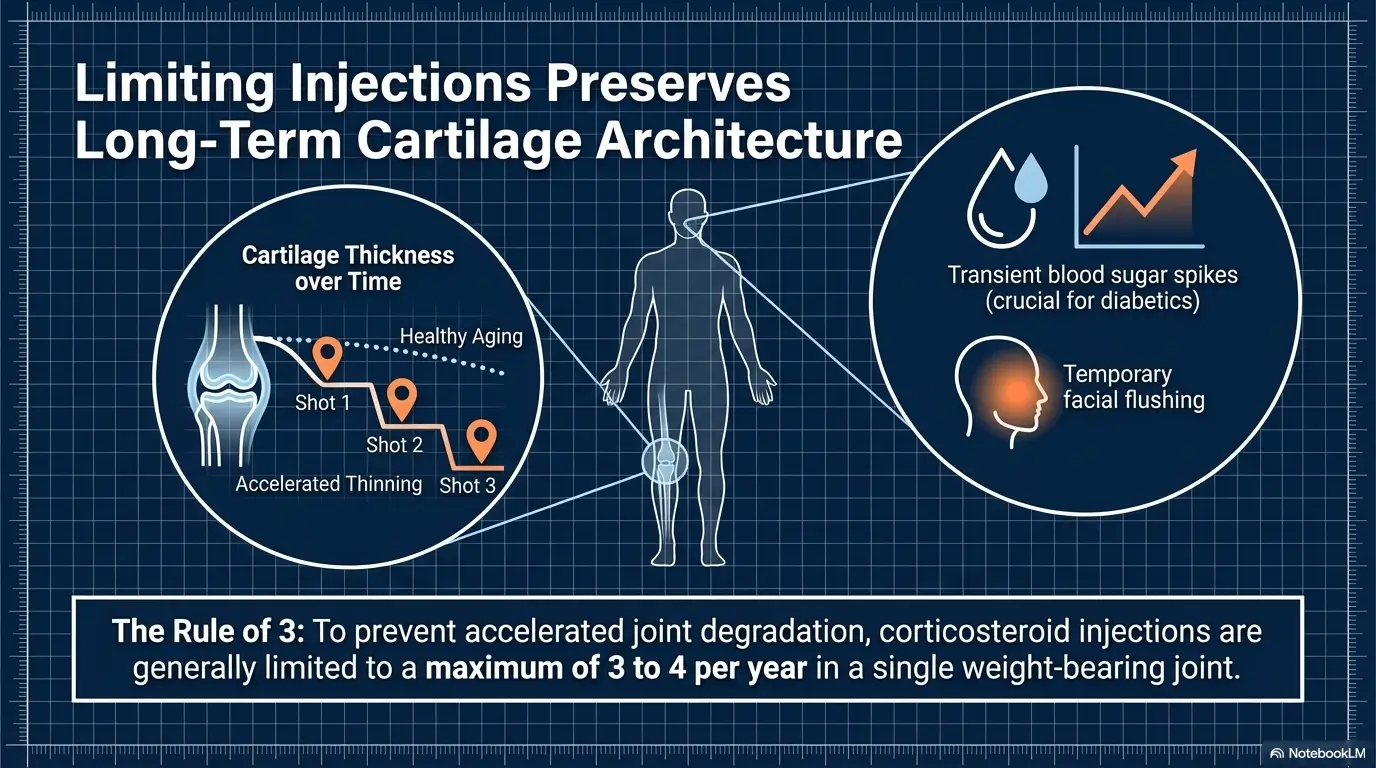
Mayo Clinic notes that relief duration varies, and patient guidance commonly emphasizes that repeated injections are limited because of side-effect concerns. That matters because a good response does not prove the tissue has healed. It proves the biology responded in a way that reduced symptoms for a while. Important difference. Large difference. Sometimes frustratingly expensive difference.
- Do not treat numb pain as recovered tissue
- Pair symptom relief with a load strategy
- Know what you will avoid after the shot
Apply in 60 seconds: Before the injection, write one sentence: “If this helps, I will use the relief window to ______.”
Relief vs Repair, What a Cortisone Injection Can and Cannot Do
What cortisone is usually meant to calm
Cortisone is usually meant to calm inflammation in or around a targeted structure. That may reduce swelling, ease pain, and create enough breathing room for sleep, daily activity, or rehab. In the right case, that is not small. It can be the difference between limping through the week and actually rebuilding function.
Why decreased pain does not always mean tissue recovery
But symptom change and tissue healing are not synonyms. Mayo Clinic lists cartilage damage, infection, post-injection flare, and tendon weakening or rupture among possible risks. AAOS is especially direct that cortisone injections generally should not be used for tendinitis in certain tendons because rupture risk can rise, and it specifically warns against Achilles tendon injection for this reason. That is a bright, practical reminder that the target matters enormously. It also helps to know that a steroid flare after injection can briefly muddy the picture rather than clarify it.
How expectations shape whether patients feel the injection “worked”
Patients often judge a shot by a simple emotional formula: “Am I better than yesterday?” Clinicians judge it more strategically: Was the right structure targeted? Did relief arrive in the expected way? Did function improve? Was the response brief, partial, or absent? Did the next step become easier? These are not contradictory questions. They are just playing in different leagues.
Let’s be honest… sometimes patients want certainty more than they want the shot itself
And that makes sense. Pain is tiring. Tired people often want a clean answer more than a perfect mechanism. I do too. Most of us do. But the body is less courtroom and more weather system. The honest win is not always certainty. Sometimes it is a better map.
Short Story: A woman I once knew through a community walking group had shoulder pain that made hair-washing feel like a hostile event. She wanted a cortisone shot immediately because a coworker had one and “was fine in two days.” Her clinician slowed the moment down. They checked strength, range, night pain, and what movements actually reproduced symptoms.
She did a short course of targeted therapy first, changed how she lifted groceries, and used anti-inflammatory treatment carefully. Two weeks later the plan had become clearer: the shot was still on the table, but now it had a job. It was no longer a prayer bead. It was a bridge. That difference changed everything. She did get the injection later, but she also knew exactly how to use the relief. She called that the first time her treatment felt like a plan instead of a coin toss.
Common Mistakes That Make the Decision Harder
Chasing quick relief before identifying the pain generator
This is the classic shortcut that quietly lengthens the road. If the pain generator is not clear enough, the treatment conversation gets distorted. You end up comparing treatments that solve different problems. A shot for bursitis is not the same decision as a shot near a tendon with degenerative change. A shot for spinal radicular irritation is not the same decision as a shot for a swollen osteoarthritic joint.
Comparing your case to someone else’s shoulder, knee, or back story
One of the sneakiest traps is borrowing certainty from somebody else’s body. Your neighbor’s knee story is not your knee story. Your cousin’s frozen shoulder is not your shoulder. Even within the same joint, the relevant structure, stage, and goal can differ wildly. That is why good orthopedic care feels slightly annoying in a useful way. It refuses lazy comparison.
Treating temporary pain reduction as proof that the problem is solved
The body can be generous for a few days and still be unconvinced overall. A quieter symptom level is useful data, but it is not the closing argument. Relief that fades quickly, relief that changes behavior without restoring capacity, or relief that never reaches the main functional problem should all be interpreted carefully.
Waiting too long to report weakness, locking, instability, or night pain
Some symptoms deserve faster escalation than people think. Weakness, giving way, locking, fever, major swelling, or pain that keeps waking you up should not be treated as background noise for weeks on end. The longer that kind of information sits unreported, the less tidy the decision becomes.
Give yourself 1 point for each “yes.”
- Do I still not know which structure is being treated?
- Would I return immediately to the same aggravating activity if pain eased?
- Have I not yet built a rehab or load-management plan?
Result: 0 to 1 points means the decision may be more organized. 2 to 3 points means the injection may be carrying too much of the plan by itself.
Neutral next step: Bring the score to your appointment and ask what gaps need closing first.
Don’t Skip These Questions Before Saying Yes to the Injection
What exactly is being injected, and into which structure
This sounds basic because it is basic. Still, many patients leave without a clean answer. Ask what medication is being used, which structure is being targeted, and whether image guidance is planned. AAOS notes that if the injection misses the joint space, it may not effectively reach the intended target, and ultrasound guidance can help reduce that risk in some settings.
What outcome should happen if the injection is appropriate
Not “Will this fix me?” Better: “If this is the right treatment, what change should I expect in pain, movement, or function?” The answer tells you whether the plan is thoughtful or improvised. You want an if-then logic chain, not a shrug wrapped in confidence.
How long relief might last, and what happens if it does not help
Duration varies. That is normal. What matters more is whether there is a next-step plan if it fails, partially helps, or helps only briefly. A serious visit should have a branch diagram in the background. If this works, do X. If it does not, do Y. If it makes things worse, call immediately.
What activity limits or rehab steps should follow afterward
This question is gold because it reveals whether the shot is being treated as a bridge or a finale. You want to know what to avoid for the next few days, what rehab timeline makes sense, and which activities could tempt overuse. That post-injection instruction is often where the real value hides. Practical readers who are also weighing the money side of the visit may want to review what a joint injection consultation can cost before saying yes on the spot.
- Name the structure
- Name the expected outcome
- Name the backup plan
Apply in 60 seconds: Put these three questions into your phone notes before the appointment.
If It Helps, Then What, Making a Plan for the Window After Pain Relief
Why the post-injection period should be used strategically, not casually
This is where many good injections go to waste. Relief arrives, but no one has decided what to do with it. The smarter move is to treat lower pain as borrowed opportunity. Use it to improve gait, mobility, sleep, strength, mechanics, or tolerance for a specific rehab task. Do not spend it all in one glorious weekend of house projects and optimism.
How to pair symptom relief with therapy, gait changes, or strengthening
If the injection calms symptoms enough to move better, that can be a precious opening. Therapy becomes more tolerable. Walking pattern improves. Daily life stops recruiting weird compensations. The goal is not simply to feel good for a while. The goal is to convert symptom relief into capacity. NICE’s osteoarthritis material specifically frames corticosteroid injections as a short-term option that may support therapeutic exercise when other pharmacologic treatments are ineffective or unsuitable. That phrasing is quietly important. Support exercise. Not replace it.
What patients often waste: the brief window when movement becomes more possible
People often waste the relief window by waiting for a perfect future week to “start being careful.” Bodies love schedules about as much as airports love weather. Use the good window now. Even small wins count. Better stairs. Better sleep. Better sit-to-stand control. Better range for grooming and dressing. Function is where the shot earns its keep.
When to Seek Help Instead of Self-Managing One More Week
Pain that is escalating despite rest and basic care
If pain is marching upward despite backing off activity, using medication as advised, and trying basic supportive measures, the “one more week” instinct may stop being sensible. Plateau is one thing. Escalation is another.
Joint locking, giving way, or inability to perform daily tasks
Mechanical symptoms matter. A joint that locks, buckles, or fails during ordinary tasks deserves a proper evaluation. These are the details that often change the management path faster than the pain score itself.
New numbness, weakness, severe swelling, or systemic symptoms
New neurologic symptoms or systemic illness clues should raise the threshold for casual self-management. Patient guidance from Mayo Clinic and hospital-based steroid injection materials consistently flags infection signs, worsening swelling, and neurologic concerns as issues needing prompt attention. In spine-related cases, this threshold rises even faster when symptoms overlap with cauda equina syndrome red flags or other features of a true low-back-pain emergency.
Persistent pain that keeps returning without a clear reason
Recurrent pain without a clear pattern deserves more curiosity, not more resignation. Sometimes the answer is mundane. Sometimes the answer is mechanical. Sometimes it is the treatment plan itself failing to match the real driver. Either way, repeated return trips to the same symptom deserve a better map.
FAQ
Should you try physical therapy before a cortisone injection?
Often, yes, especially when movement, strength, load tolerance, or mechanics seem to be part of the problem. Therapy can reduce symptoms, clarify diagnosis, and make any later injection more strategic rather than impulsive.
Can a cortisone injection hide a more serious orthopedic problem?
It can reduce symptoms that might otherwise push faster evaluation, which is why red flags and diagnosis matter first. Relief is not proof that the underlying issue is minor.
How do you know whether pain is coming from inflammation or structural damage?
You usually do not know from pain intensity alone. Pattern, exam, swelling, weakness, instability, imaging when appropriate, and response to conservative care all help separate the possibilities.
Is a cortisone shot better for joint pain than tendon pain?
It depends on the structure and diagnosis. AAOS specifically warns that cortisone shots generally should not be used for certain tendinitis problems because tendon rupture risk can increase, including Achilles tendinitis.
What should you ask an orthopedist before getting injected?
Ask what structure is being targeted, what medication is being used, what result should happen if the shot is appropriate, what the risks are in your case, and what the next step is if it helps or fails.
If the first injection works, does that confirm the diagnosis?
Not completely. It may support the idea that the injected structure contributed to pain, but it does not always explain the underlying cause or guarantee the broader plan is correct.
Can pain get worse again after a cortisone injection wears off?
Yes. Relief can be temporary. Some people also experience a short-term flare after injection. That is one reason expectations and follow-up planning matter.
What if rest, ice, and medication have not fixed the problem?
That usually means it is time for a more structured review: exam, diagnosis refinement, possible therapy adjustments, possible imaging, and then a discussion of whether injection actually fits the problem.
When should imaging happen before deciding on injection?
When the diagnosis is unclear, trauma matters, red flags exist, or the result would change management. Routine imaging is not always helpful for non-surgical management in conditions like osteoarthritis.
Is it reasonable to delay injection and keep trying conservative care?
Yes, if symptoms are not urgent, diagnosis is still being clarified, and conservative treatment still has a meaningful chance to help. It is not reasonable if red flags are present or function is deteriorating quickly.
Next Step, Build a Decision-Ready Visit Instead of a Relief-Only Visit
Bring a one-page symptom timeline with pain triggers, failed treatments, and function limits
This may be the most useful five-minute prep in the whole article. Write when the pain started, what movements worsen it, what treatments you tried, what helped a little, what failed, and what daily functions you have lost. A clean timeline often improves the visit more than another week of guessing at home.
Write down three questions: what is the diagnosis, why this injection, and what is the plan if it fails
These questions sound modest. They are not. They pull the conversation out of vague relief-seeking and into actual medical decision-making. The goal is not to be difficult. The goal is to be clear.
Leave the visit knowing not just whether to get the shot, but what the shot is supposed to accomplish
This closes the curiosity loop from the beginning. The best decision is rarely “shot or no shot” in the abstract. It is “What problem are we treating, why now, what outcome counts as success, and how will we use the result?” When you can answer those questions, the room gets quieter.
Not because pain has vanished, but because the fog has. Within the next 15 minutes, make your symptom timeline and your three-question list. That is the smallest move with the highest leverage. And if cost, imaging access, or insurance friction is part of the hesitation, related reads on orthopedic pain management with an HDHP and what to do after an MRI denial appeal can make the next conversation less foggy too.
- When the pain began and whether there was an injury
- Top 3 movements or tasks you cannot do well now
- Treatments tried: medication, therapy, brace, rest, footwear, ice or heat
- Red-flag symptoms you do or do not have
- Your main goal: sleep, walking, stairs, work, lifting, sport, or daily function
Neutral next step: Bring this list to the appointment so the decision is built on pattern, not memory haze.
Last reviewed: 2026-03.
