
Beyond the Diagnosis:
Mapping the Hidden Friction of Daily Mobility
Orthopedic pain management for seniors using walkers at home usually fails in the tiny moments nobody photographs: the push from a low chair, the half-turn into the bathroom, the midnight shuffle when the room feels wider than it did at noon.
“That is where pain stops being a diagnosis and becomes a daily negotiation.”
The real problem often isn’t the walker itself—it’s the hidden strain of poor lighting, unsafe footwear, or a room layout that asks sore joints to do too much. Stop guessing, and stop spending on the wrong equipment.
The Strategy: Watch the day like a map, not a mystery.
- 1. Start with the movement
- 2. Find the high-strain room
- 3. Fix the repeatable moment
Table of Contents
Stand up, turn, reach, rush, or stand too long.
Hunching, leaning, gripping harder, shuffling, twisting.
Joint pain, shoulder ache, wrist strain, fatigue, fear.
Fit the walker, change the room, pace the task, rest sooner.
The point: pain management works better when you fix the moment that causes the strain, not just the pain after it appears.

Start With the Real Problem: Pain Is Usually Triggered by Movement, Not Just Condition
Why walker-related pain often shows up during transitions, not quiet sitting
Many families describe the pain in broad terms: arthritis, knee pain, back pain, recovery pain. But the body tells a more specific story. A senior may look comfortable while seated and then wince during the exact three seconds it takes to stand, steady, and reach the walker. That is not a contradiction. It is the difference between static comfort and dynamic strain.
The most painful parts of the day often live inside transitions: bed to standing, chair to hallway, toilet to sink, kitchen counter to dining chair. In those moments, joints must accept load, muscles must coordinate quickly, and balance has to keep up. A walker helps, but only after the body is upright enough to use it well. Before that, the body is still doing the hardest part.
I have seen families think, “But she walked to the kitchen, so maybe the pain is not that bad.” Then you watch the first push from the recliner, and the truth walks into the room wearing orthopedic shoes. The walking was not easy. It was simply less painful than the launch sequence.
How knees, hips, back, shoulders, and wrists each create a different home-care problem
Knee pain tends to protest during rising, turning, and short-distance walking on stiff mornings. Hip pain often flares with pivoting, uneven weight-bearing, or sitting down a little too hard. Back pain may worsen with hunching over a walker, reaching forward, or prolonged standing. Shoulder and wrist pain can sneak in when a walker is too low, the grip is too hard, or the user leans heavily through the arms. One household may call all of this “mobility trouble,” but the fix depends on which body part is doing the complaining.
That is why vague advice often fails. “Use the walker more carefully” is not a plan. “Pain spikes when standing from the toilet and turning left into the hall” is a plan. It sounds less glamorous, but it works better. Pain has an address. Your job is to find it.
Why “using a walker” does not automatically mean the setup is helping
A walker can be the right tool and still be used in the wrong environment, at the wrong height, with the wrong habits. That is not user failure. It is just how home care often unfolds. Real homes are full of low chairs, crowded paths, rugs with secret opinions, and counters that invite too much standing. The National Institute on Aging notes that canes and walkers help prevent falls when they are used correctly and are the right size. That “when” matters more than people think.
- Map pain to a specific task
- Notice whether the spike happens before, during, or after walking
- Separate joint pain from arm-overload pain
Apply in 60 seconds: Ask, “What exact movement makes the face change?” and write down the answer.
Who This Is For, and Who It Is Not For
Best for seniors using a walker at home with orthopedic pain from arthritis, joint strain, surgery recovery, or mobility decline
This guide is for older adults using a walker at home and for family caregivers trying to make daily movement safer and less miserable. It fits common situations: osteoarthritis, chronic joint stiffness, generalized mobility decline, back pain aggravated by posture, or recovery after a joint procedure when the household is trying to follow the basic plan without turning the house into a warehouse of random equipment. For a broader starting point, see this guide to elderly orthopedic pain management.
Helpful for adult children and family caregivers trying to reduce daily pain friction
Caregivers are often doing detective work with no badge and no lunch break. They know something is going wrong, but they do not always know whether the problem is the walker, the room, the timing, or the task. This article helps untangle that knot. It is not about turning a family member into a rehab professional. It is about making fewer painful mistakes on ordinary Tuesdays.
Not for sudden severe pain, new numbness, chest symptoms, or possible medical emergencies
If pain is suddenly much worse, sharply different, linked to a fall, paired with new weakness, fever, redness, chest symptoms, trouble breathing, or inability to bear weight, this is not a “read one more blog post” situation. It is a seek-help situation. Calm is good. Delay is not always good.
Not for replacing a clinician’s diagnosis, medication plan, or post-surgical instructions
Home strategies are useful, but they are not a substitute for individual medical guidance. If a surgeon, physical therapist, orthopedist, or primary care clinician has given specific movement restrictions or recovery instructions, those instructions outrank general internet advice every time. The body did not sign up for democracy on that point.
One quiet truth here: a good article should reduce confusion, not increase confidence beyond what is earned. That is especially important with older adults, fall risk, and pain that may be evolving.
Pain Hides in the Routine: Where Home Walking Hurts More Than Families Expect
The stand-up moment from bed, sofa, or toilet
Standing up is a joint-loading event disguised as a simple movement. From a soft sofa, the knees and hips may have to work harder because the seat is low and the body sinks. From bed, the issue may be stiffness plus poor leverage. From the toilet, it can become a perfect storm of pain, urgency, cramped space, and awkward arm placement. Families often focus on the hallway walk, but the pain spike may have started before the first step.
The hallway turn that twists the hip or knee more than expected
Straight-line walking is not the whole story. Turning is where many seniors leak comfort. A narrow hallway, bathroom doorway, or bed corner can force half-turns and hesitant pivots. That is where knees complain, hips object, and the walker suddenly feels less like a helper and more like a piece of furniture with opinions.
The kitchen task that quietly turns walker use into prolonged standing strain
The kitchen is sneaky. It looks domestic and ordinary, but it is a stamina trap. Making tea, rinsing fruit, preparing a sandwich, or waiting for the microwave can turn into 8 to 15 minutes of static standing, subtle leaning, repeated reaching, and arm pressure through the walker. Pain may not spike instantly. It may bloom afterward like a slow invoice.
The night trip to the bathroom that combines pain, urgency, and risk
Nighttime compresses all the problems into one small corridor: stiffness, dim light, urgency, slower reaction time, and less patience. The CDC emphasizes that falls in older adults are common and preventable, and home hazards plus balance challenges can stack the odds in the wrong direction. For many seniors, the bathroom trip is the most revealing mobility test of the day because it strips away adrenaline and daylight confidence.
In one family I know, the daughter kept buying supports for daytime pain, but the real trouble lived between 1:30 and 3:00 a.m. Once they improved lighting, reduced bedside clutter, raised the toilet seat, and moved the walker to the same exact parking spot each night, the pain complaints did not vanish, but the fear dropped sharply. Sometimes safety is the first pain reliever because tension itself had been making the movement worse.
- Yes / No: Does pain spike during one specific transfer?
- Yes / No: Is nighttime walking harder than daytime walking?
- Yes / No: Does the senior avoid a room because it “hurts too much” to use?
- Yes / No: Does the walker get parked differently every day?
Next step: If you answered “Yes” to two or more, start with room setup and transfer analysis before shopping.
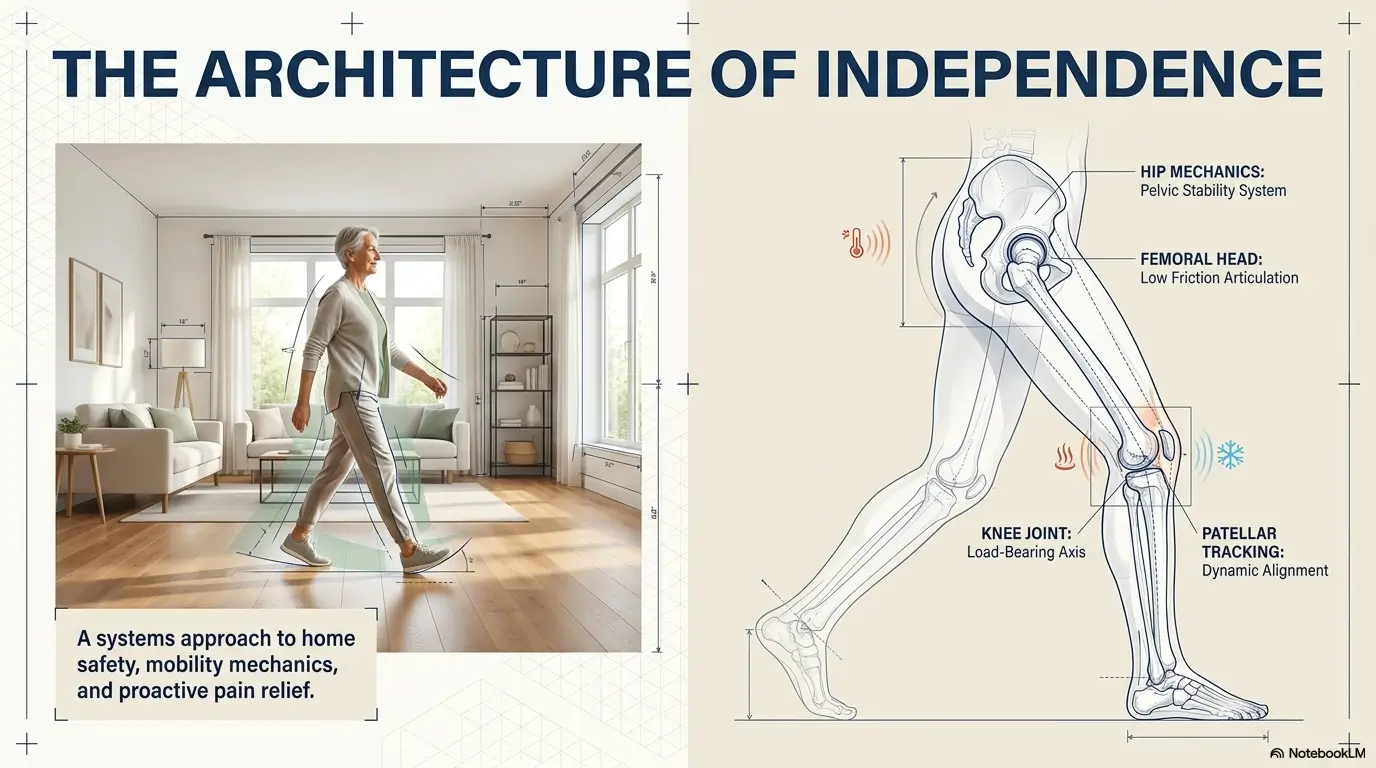
Walker Fit First: The Small Adjustment That Can Change Everything
Why a too-low walker can shift pain into the back, shoulders, and wrists
When a walker is too low, people often hunch. Their shoulders rise, their back rounds, and their wrists take more pressure. Over time, this can turn walking support into an upper-body strain generator. It is a little like using the right word in the wrong sentence. Technically present. Functionally troublesome.
A low walker also encourages looking down more, which can worsen posture and make movement feel more uncertain. That uncertainty changes gait. The person grips harder. The arms work more. The whole body becomes tense before it even crosses the room.
Why a too-high walker can make balance worse instead of better
A walker that sits too high can leave the arms awkwardly elevated and the shoulders tense. It may also reduce effective support because the person cannot comfortably transfer weight through it when needed. Instead of feeling grounded, they may feel as though they are negotiating with a slippery ladder that never actually agreed to the job.
How handgrip comfort, arm position, and posture affect orthopedic pain
Good fit is not only about height. It is also about whether the hands can rest naturally, whether the elbows are slightly bent rather than locked, and whether the body stays relatively upright instead of folded forward. A senior with arthritis in the hands may need thicker or softer grip solutions. A senior with shoulder pain may need a fuller review of how much body weight is being dumped into the arms. The goal is not a perfect pose from a brochure. It is a repeatable setup that reduces strain in real rooms.
Here’s what no one tells you: the walker may not be the only problem in the room
Sometimes the walker is innocent. The real villain is the low couch, the twisting route around a coffee table, the slippery slide-on shoe, or the habit of carrying things while walking. The National Institute on Aging also notes that borrowed walkers should be checked for correct size and safety. That matters because hand-me-down equipment can feel economical but create costly pain if the fit is off.
Show me the nerdy details
Small changes in device height alter trunk angle, shoulder loading, wrist extension, and how weight is distributed during gait. In practical terms, that means a walker that “mostly works” can still create meaningful stress during dozens of daily repetitions.
- Low walkers often create hunching and wrist load
- High walkers can reduce stable support
- Room layout can sabotage even a well-fitted walker
Apply in 60 seconds: Watch one full stand-and-walk sequence from the side and look for hunching, shrugging, or over-gripping.
Don’t Chase Pain Blindly: Match the Relief Method to the Trigger
When rest and pacing help more than “pushing through”
There is a difference between useful movement and stubborn overdoing. Many seniors feel better with shorter, steadier sessions rather than one heroic effort followed by an afternoon of regret. Pacing is not laziness in nicer clothing. It is a joint-protection strategy. If pain rises predictably after 10 minutes of kitchen standing, the answer may be a stool, a seated prep step, or two shorter kitchen visits instead of one longer one.
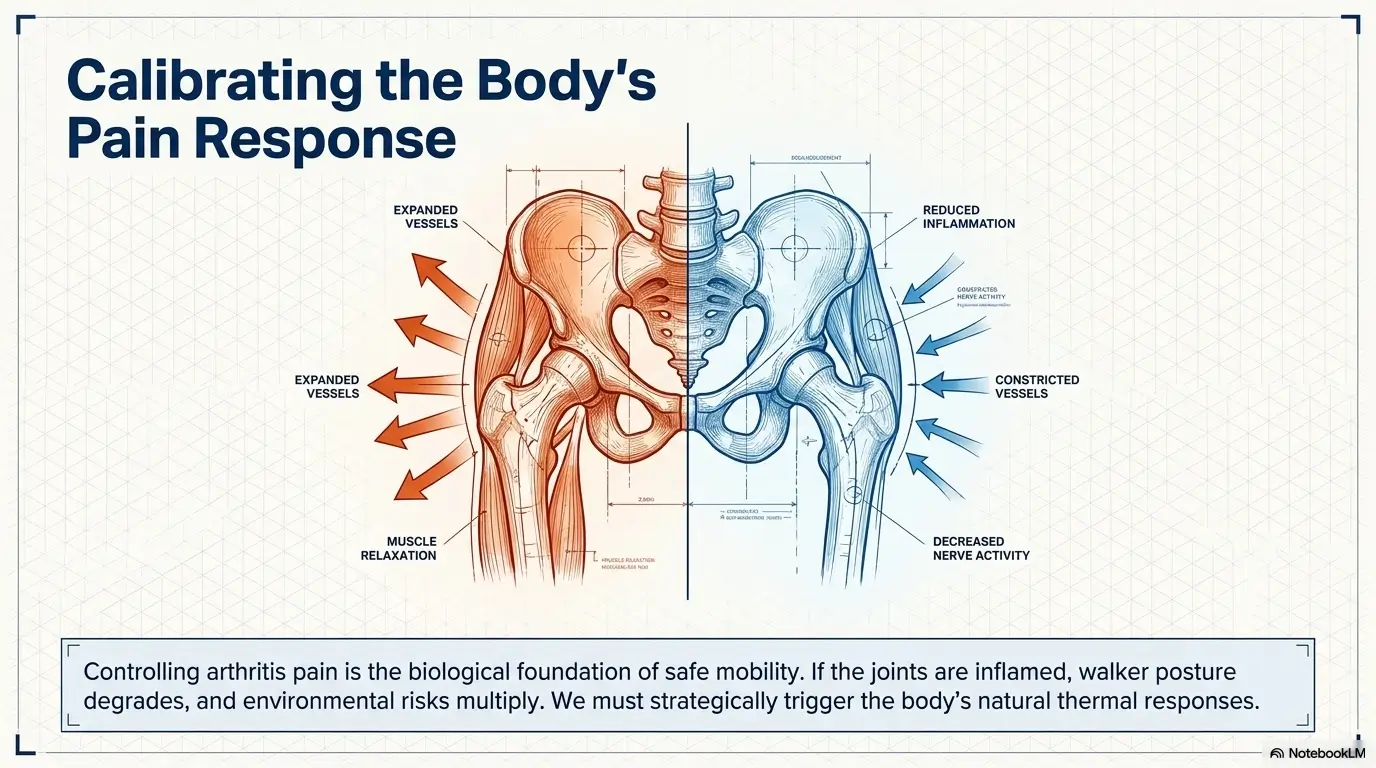
When ice may make sense for flare-ups and swelling
Cold often makes more sense when swelling, heat, or post-activity flare-ups are part of the picture. The Arthritis Foundation explains that cold can reduce swelling and help with pain during flares or after exertion. That does not mean icing everything on principle like a household religion. It means matching the tool to the pattern.
When heat may feel better for stiffness before movement
Heat is often more comforting for stiffness, especially before movement. Warmth can help loosen tight muscles and make joints feel more willing at the start of the day. A warm shower, a warm compress used as advised, or a bit of planned warmth before the first walking block can sometimes turn a grim start into a manageable one.
Why timing matters more than families think
People often ask, “Is ice or heat better?” The more useful question is, “Better for what, and when?” Heat before movement may help stiffness. Cold after an overdone task may help swelling. Rest before pain spikes may prevent a worse flare than rest after the damage is already done. Timing turns generic advice into functional advice. If the pain pattern remains unclear, this practical piece on orthopedic pain management can help readers think through conservative options before jumping to bigger decisions.
I once watched a family member insist heat “never works,” but what she meant was that heat after 25 minutes of painful meal prep did not undo the whole mistake. When she tried warmth before the first morning movement and cold after a swollen afternoon flare, the body stopped arguing quite so loudly. Same tools. Better timing.
| When this sounds familiar | Often worth considering | Why |
|---|---|---|
| “Morning stiffness is the worst part” | Heat before movement | May ease stiffness and help the first steps feel less hostile |
| “It swells or throbs after activity” | Cold after the task | May help with flare-up discomfort and swelling |
| “Everything hurts because the task went on too long” | Pacing plus seated breaks | Prevents the overuse spiral before it starts |
Neutral action: Try one method for one repeatable pain pattern and judge it by function, not hope.
Room by Room Relief: Make the House Easier Before the Body Gives Up
Bedroom fixes that reduce the first painful steps of the day
The bedroom should not begin the day with an ambush. Keep the walker parked in the same reachable spot, clear the floor, improve lighting, and reduce the need for twisting to reach glasses, slippers, or medication. If the first steps are always miserable, think sequence. Can the person sit first, gather themselves, warm up a little, then stand? Small order changes matter.
Bathroom changes that lower strain during transfers
Bathrooms compress difficulty into a tiny footprint. A raised toilet seat, grab bars installed appropriately, non-slip surfaces, and a more direct route can reduce both pain and risk. The CDC’s fall-prevention materials repeatedly emphasize home hazard reduction because seemingly small environmental fixes can lower fall risk. The bathroom is where those fixes often earn their paycheck fastest.
Living room layout choices that reduce awkward turns and reach distance
Low sofas, cluttered side tables, cords, throw rugs, and decorative stools all have one thing in common: they were probably not designed by people doing painful transfers at dusk. Try widening the route, raising the preferred seat height when appropriate, and keeping the most-used items within easy reach. The living room should support recovery, not audition for obstacle-course duty.
Kitchen edits that help seniors do small tasks without paying for them later
Place daily-use items at waist to chest height when possible. Reduce the need to carry, bend, or stand in one place for too long. A sturdy perch or seated prep station can help some seniors conserve joints without giving up the task. The goal is not to erase activity. It is to make activity less expensive to the body.
Short Story: The Cup of Tea Test
A son told me his mother insisted she was “fine in the kitchen,” and technically she was. She could still make tea. But when he watched the whole sequence, the truth was sitting in plain sight. She stood too long waiting for the kettle, twisted to reach mugs above shoulder height, then shuffled the last few steps with a face that had gone tight and quiet.
They changed three things only: moved the mugs down, put a chair near the counter, and set up a small tray on the table before she started. The next morning she made the same tea in nearly the same time, but without the small collapse afterward. It was not dramatic. No orchestra played. Yet the room had stopped charging interest on every movement. That is what a good home setup often looks like: less pain, less pride-wounded frustration, and a little more ordinary life.
- Standardize where the walker rests
- Reduce turning and reach distance
- Make the bathroom and kitchen less punishing first
Apply in 60 seconds: Remove one floor hazard and relocate one high-use item closer to the body’s easiest reach zone.
Common Mistakes That Make Walker Pain Worse at Home
Using the walker while hunched, rushed, or half-turned
Rushing changes mechanics. So does trying to move while half-turned toward a person, a pet, a countertop, or a conversation. The walker works best when movement is intentional and aligned. When the body twists away from the frame while still relying on it, pain and instability both rise.
Keeping frequently used items just far enough away to trigger strain
This is one of the great household ironies. The remote is nearby, but not nearby enough. The tissues are on the wrong side table. The phone charger is reachable only through a lean that turns into a tug-of-war with the back. Tiny distances create repeated strain. Homes often hurt people through repetition, not drama.
Wearing the wrong shoes on “just a quick trip” across the room
Unsupportive or slippery footwear is a classic “it’ll only take a second” mistake. The CDC lists foot pain and poor footwear among fall-related concerns for older adults. A quick trip across the room is still a trip. The floor does not care that the intention was brief.
Treating all pain as identical instead of noticing the pattern
When families label every complaint as “bad arthritis,” they miss the clues. Is pain worse after standing still? During turning? Only from low seats? Mostly in the evening? More in the hands after a longer walk? Patterns are not trivia. They are instructions in disguise. When symptoms continue even after basic conservative steps, it may also help to understand why physical therapy may not be helping orthopedic pain in the way families expected.
- The three most painful movements of the day
- Whether swelling, stiffness, or fatigue is part of the pattern
- Which room triggers the most trouble
- Whether arm, wrist, shoulder, knee, hip, or back pain dominates
- Any recent fall, near-fall, or major change in walking confidence
Neutral action: Bring this list to a clinician, therapist, or equipment conversation instead of only saying “walking hurts.”
Do Not Do This: The Home Habits That Quietly Backfire
Don’t let the walker become a tray, laundry rack, or unstable carrying tool
Walkers are mobility aids, not tiny delivery trucks. Using them to carry laundry, balance a cup of coffee, or transport unstable items changes how the device is controlled and can pull the body into awkward positions. It is understandable. It is practical-looking. It is also often a bad bargain.
Don’t wait until pain spikes before resting
Reactive rest is usually less effective than planned rest. If pain reliably surges after a certain task duration, build in the break earlier. The body is not a customer-service desk that only opens after the complaint gets dramatic.
Don’t keep using a worsening setup because “it has always been this way”
Older adults and families often adapt quietly. They normalize too much. The chair becomes impossible, but everyone keeps using it. The bathroom turn gets harder, but people just grip tighter and hope. Familiarity is not proof of safety. Sometimes it is just proof that human beings are astonishingly willing to cope until coping becomes expensive.
Let’s be honest: many homes are asking the body to work harder than necessary
That is not a moral failure. It is an architecture problem, a habit problem, and a timing problem wearing ordinary clothes. Once you see it that way, the emotional weather changes. The senior is not “being difficult.” The room is being difficult.
Pain Management Beyond Products: The Daily Rhythm That Often Matters More
Why shorter, steadier movement sessions can beat one exhausting effort
Many older adults do better with movement spread through the day rather than one ambitious push. The National Institute on Diabetes and Digestive and Kidney Diseases notes that older adults are often encouraged to build activity gradually. In home life, that translates into something simple: less boom-and-bust. A few steady walking bouts and task blocks may preserve function better than one long effort followed by hours of pain and avoidance.
How seated task breaks protect joints without promoting total inactivity
There is a sweet spot between overdoing and freezing. Seated breaks can reduce joint load, lower fatigue, and make activity sustainable. The risk, of course, is that every pause turns into full retreat. The answer is not to avoid breaks. It is to use them deliberately. Sit. Reset. Continue if safe. The point is rhythm, not surrender.
Why morning stiffness and evening fatigue need different strategies
Morning may call for warmth, slower starts, and simpler first tasks. Evening may call for less standing, brighter lighting, and fewer rushed trips. Treating the whole day as one identical block is one reason pain plans fail. Bodies have clocks, and orthopedic pain often respects them with annoying punctuality.
The role of simple tracking: what hurts, when, and after which task
A three-day log can reveal more than a month of vague frustration. Write down the time, task, pain location, and what happened right before it. Not poetry. Not a dissertation. Four plain facts. Patterns emerge fast. Maybe the problem is not walking distance. Maybe it is standing at the sink. Maybe it is every left turn after getting off the toilet. This is the kind of boring data that quietly rescues people.
Show me the nerdy details
Orthopedic pain patterns are often task-specific because different movements change joint loading, muscle demand, balance requirements, and upper-extremity compensation. Tracking helps identify which variable actually changes outcomes.
Count how many times the senior does the most painful movement in one day.
- Transfer count: ___ times
- Average pain after each: low / medium / high
- One environmental fix added: yes / no
Output: If the same painful movement happens 8 to 12 times a day, even a small setup improvement can reduce a surprising amount of total strain.
Neutral action: Fix the highest-frequency painful movement first, not the most emotionally dramatic one.
When Family Help Works Best, and When It Accidentally Reduces Independence
Support the task, not every movement
Good help makes the movement easier without taking over the person’s whole body or whole day. Sometimes that means setting up the room, placing the chair, cueing the sequence, or moving an object out of the way. It does not always mean physically grabbing. In fact, unplanned grabbing often increases tension and throws off balance.
How cueing, setup, and pacing can help more than grabbing or hovering
Simple verbal cues can be more useful than urgent hands. “Pause.” “Bring the walker close.” “Turn in small steps.” “Sit back slowly.” These are small sentences, but they preserve agency. Hovering, by contrast, can make people rush, resist, or feel less stable because they are reacting to your anxiety rather than their own movement pattern.
When caregiver urgency increases pain and instability
Nothing tightens a room like a rushed helper saying, “Come on, just stand up.” Older adults often feel that urgency in their muscles before they even move. The result is harder pushing, faster turning, poorer form, and more pain. Helping faster can absolutely make the transfer worse. This is one of the strangest lessons in caregiving because it feels backward until you watch it happen.
Here’s the strange part: “helping faster” can sometimes make the transfer worse
I remember a caregiver who was excellent in every visible way: organized, loving, alert. But every transfer had a countdown energy to it, and the older adult grew more rigid each time. When the caregiver slowed down and stopped narrating urgency into the room, the transfer improved. Same bodies. Same walker. Different tempo. Pain is often less tolerant of hurry than families are.
- Set up the task
- Use calm cues
- Reduce urgency in the room
Apply in 60 seconds: Replace one physical assist today with one setup change and one calm cue.
What to Watch Before Buying Anything Else
Whether the real issue is transfer pain, walking pain, standing pain, or recovery pain
Before buying anything, identify which category you are actually trying to solve. Transfer pain suggests seat height, grab support, and sequencing issues. Walking pain may point to fit, endurance, footwear, or turning mechanics. Standing pain often points to task design and pacing. Recovery pain after activity may suggest overuse, swelling, or poor timing of rest.
Which add-ons may help, and which only add clutter
Useful add-ons are the ones that reduce strain in a specific repeatable moment. Clutter-products are the ones that sound reassuring but do not clearly improve a task. This is how households end up with padded mysteries, baskets no one likes, unstable trays, and objects that seemed wise online at midnight. Homes do not need more equipment. They need more honesty. When equipment costs are part of the decision, families may also want to review HSA eligible braces and supports before buying accessories that may or may not fit the actual pain pattern.
How to judge usefulness by one test: does this reduce strain in a specific moment?
That is the test. Not “Is it highly rated?” Not “Did it look good in an ad?” Not “Would it make me feel like I’m doing something?” The real test is narrower and smarter: does this reduce strain in a specific moment we can name?
Why expensive equipment often fails when the pain pattern was misunderstood
Expensive mistakes are often diagnosis mistakes in disguise. If the actual problem is low-seat transfer pain, a fancy walker add-on will disappoint. If the problem is prolonged kitchen standing, a new grip cover may not touch it. The wallet suffers first, but the deeper cost is discouragement. People start thinking nothing helps, when really the wrong problem got all the attention.
| Tier | Example | Best for |
|---|---|---|
| 1 | Declutter, better lighting, item placement | Most homes, low-cost wins |
| 2 | Footwear, grip comfort, walker check | Pain linked to use habits |
| 3 | Raised seating, bathroom transfer support | Transfer-focused pain |
| 4 | Structured pacing, therapist input | Persistent function loss |
| 5 | Medical reassessment | Pain that is worsening, unusual, or unsafe |
Neutral action: Start at the lowest tier that matches the real pain trigger.
When to Seek Help
Pain that is suddenly worse, sharply different, or linked to a possible fall
A sudden jump in pain deserves respect. If the pain is new, severe, sharply different from baseline, or follows a slip, stumble, or fall, seek clinical guidance promptly. The body changes its story for a reason. If the decision is whether to go somewhere now or schedule specialty care, this comparison of urgent care vs. an orthopedic clinic may help frame the next step.
New swelling, redness, fever, numbness, weakness, or inability to bear weight
These are not “maybe later” clues. New swelling, redness, fever, numbness, clear weakness, or inability to bear weight can signal a problem that needs proper evaluation rather than household improvisation.
Pain that keeps increasing despite rest, setup changes, and proper walker use
If you have improved the environment, checked fit, changed timing, reduced overuse, and the pain still trends upward, that is meaningful. Home friction may have been part of the problem, but not the whole problem. If imaging questions begin to surface, readers may benefit from understanding orthopedic pain management before asking for an MRI instead of treating the scan as the first and only milestone.
Post-surgical concerns that do not match the expected recovery instructions
After surgery, the surgeon’s instructions define the lane. If the pain level, swelling pattern, mobility ability, or function decline does not seem to match the expected course, contact the clinical team. It is always better to clarify than to build a home strategy on a false assumption. For knee-specific recovery concerns, this guide to knee replacement pain management can give families a more focused context.
The good news is that not every pain problem is a crisis. The better news is that some are improved dramatically by smarter setup. The responsible news is that red flags still matter. Wisdom in caregiving is often the ability to tell those categories apart.
FAQ
Why does my parent have more pain using a walker than sitting still?
Because sitting and moving place different demands on the body. Standing, turning, and walking require joint loading, balance, grip, and posture adjustments. A senior can look calm in a chair yet still have real pain during transitions.
Can a walker cause shoulder, wrist, or back pain if it is the wrong height?
Yes. A walker that is too low can encourage hunching and increased wrist pressure. One that is too high can feel awkward and reduce support. Fit, grip comfort, and posture all matter.
Is ice or heat better for orthopedic pain in seniors at home?
It depends on the pattern. Heat is often more comforting for stiffness before movement. Cold may be more useful after overuse, during a flare, or when swelling is part of the picture. When in doubt, match the method to the trigger and follow any clinician guidance.
What is the safest way to reduce pain when getting up from bed or a chair?
Make the setup easier before the movement begins. Improve seat height when appropriate, place the walker consistently, reduce twisting, allow a pause before standing, and avoid rushing. If transfers are repeatedly painful, that specific movement deserves focused attention.
Should seniors with arthritis walk through the pain or rest more often?
Usually neither extreme works well. Total avoidance can reduce function, while pushing through escalating pain can worsen the day. Many seniors do better with shorter, paced activity and earlier breaks rather than one exhausting effort.
What rooms in the house usually cause the most walker-related pain?
Bathrooms, bedrooms, and kitchens are common trouble zones. Bathrooms stress transfers and turning. Bedrooms challenge the first steps of the day and nighttime walking. Kitchens often create prolonged standing and repeated reaching.
How can I help a senior use a walker without making them more dependent?
Support the setup and the sequence rather than taking over every movement. Clear the path, cue calmly, reduce urgency, and preserve the person’s role in the movement whenever safe.
What are signs that home pain management is not enough anymore?
Red flags include sudden severe change, new weakness, fever, redness, major swelling, inability to bear weight, repeated near-falls, or worsening pain despite sensible home adjustments and correct walker use.
Next Step
Walk through one full day at home and note the three exact moments when pain spikes most: standing up, turning, reaching, bathroom transfer, meal prep, or nighttime walking. Build the article around those moments first, because that is where readers will feel seen and where the outline becomes genuinely useful.
Here is the honest next move, and it can happen within 15 minutes. Do not start with shopping. Do not start with guilt. Start with observation. Follow one normal day and write down the top three pain moments in plain language. For example:
- “Pain spikes when standing from the recliner before lunch.”
- “Left knee hurts most when turning into the bathroom.”
- “Shoulders ache after 10 minutes in the kitchen.”
That tiny list closes the loop from the opening of this article. The problem was never just “pain at home.” It was pain living inside very particular moments. Once you name those moments, the home becomes more editable. The walker becomes more understandable. And the next decision gets smaller, cheaper, and smarter.
If you do only one thing today, do that. Walk the day. Find the three spikes. Then change the one that happens most often. The best home pain management plan usually begins there: not with a miracle, but with a map.
Last reviewed: 2026-04.
Safety / Disclaimer
This article is educational and practical, not a diagnosis, medication plan, or substitute for personal medical advice. Use extra caution with recent surgery, fast-changing pain, fall risk, weakness, numbness, fever, redness, chest symptoms, or inability to bear weight. Follow the instructions from the senior’s own clinician, surgeon, or therapist when they differ from general guidance. When symptoms are severe, new, or worrisome, seek medical help promptly.
