
You may forget yesterday’s pain score,
but your socks remember.
A 0–10 pain number can be useful, but it often misses the part that changes your actual morning: bending for shoes, lifting an arm into a sleeve, balancing into pants, or needing five quiet minutes after getting dressed.
For many living with chronic pain, those small dressing struggles reveal more than a lonely “6 out of 10” ever could.
The method is simple: Observe one repeated morning task, note the pattern, and bring that real-life evidence into the exam room.
The clue is already there. It may be in the sock. Or the jacket. Or the shirt you stopped wearing without realizing why.
This article is for health self-observation and communication only. It does not diagnose the cause of pain or replace medical care. Pain that is new, worsening, unexplained, linked to injury, or paired with weakness, fever, dizziness, breathing trouble, numbness, bowel or bladder changes, falls, or trouble performing routine activities deserves prompt professional attention.
Table of Contents
The Dressing Test: Why Morning Clothes Tell the Truth First
Pain scores measure intensity. Getting dressed reveals interference.
That difference sounds small until you are standing half-awake beside the bed, negotiating with a sock like it has a legal department. A number can say, “My pain is 6.” Dressing says, “I cannot bend forward without holding the dresser, I need 10 extra minutes, and I skip lace-up shoes because the bending makes my back and leg burn.”
Pain scores measure intensity; dressing reveals interference
A 0–10 pain score can help clinicians understand severity, especially when tracking change over time. The CDC’s pain-care guidance emphasizes looking at benefits, risks, function, and the person’s full situation rather than treating a number as the whole story. That matters because pain is not only a sensation. It is a thief of motion, sleep, confidence, work, and patience.
Dressing is useful because it bundles many movements into one familiar ritual:
- Reaching overhead for a shirt
- Bending to pull on socks
- Balancing on one leg for pants
- Pinching buttons, zippers, or clasps
- Tolerating waistbands, straps, seams, and pressure
The “sock moment” that exposes bending, balance, grip, and fear
The sock moment is small, but it is not silly. It asks your back, hips, knees, ankles, hands, balance system, and nerves to cooperate before coffee has even joined the committee.
I once watched someone describe their pain as “not too bad,” then spend 90 seconds trying to get one sock on without holding their breath. The room grew quiet. Not dramatic. Just true. The body had already testified. For older adults, that kind of morning difficulty may also connect with broader orthopedic pain management for older adults, especially when stiffness, balance, and daily self-care start overlapping.
Why morning stiffness can be more useful than yesterday’s number
Morning dressing also captures stiffness, hesitation, and recovery time. Maybe your pain is 4 at rest but 8 when you lift your arm into a sleeve. Maybe it settles after a warm shower. Maybe the first 20 minutes of the day are a tiny obstacle course in cotton.
- Note the task that hurts.
- Note the movement that triggers it.
- Note what you changed to get through it.
Apply in 60 seconds: Tomorrow morning, choose one task, such as socks or shirt, and write one sentence about what happened.
The Number Trap: When a 7 Out of 10 Says Too Little
Two people can say “7 out of 10” and be living very different Tuesdays.
One person’s 7 means they can work, cook, and dress slowly, then collapse with a heating pad at night. Another person’s 7 means they cannot shower safely, cannot fasten clothing, and cannot drive. Same number. Different life. This is where the pain scale starts wearing shoes that are one size too small.
Two people can say “7” and mean completely different lives
The numeric pain rating scale is common because it is quick. A clinician can ask, document, and compare. That speed is useful. But speed can flatten nuance.
People interpret numbers through personal history, pain tolerance, fear, culture, work pressure, family roles, and whether they were raised to say “I’m fine” while their nervous system is waving a tiny red flag from a window.
Pain tolerance is not the same as pain impact
Someone may tolerate pain well and still lose function. Another person may report pain intensely but maintain movement. Neither person is wrong. Pain is personal, but function gives the conversation more shared ground.
Try this comparison:
| Pain report | What it misses | Better add-on |
|---|---|---|
| “It’s a 7.” | Where it appears and what it blocks | “It’s a 7 when I pull on socks.” |
| “It hurts in the morning.” | Duration, stiffness, and recovery | “The first 30 minutes are hardest.” |
| “I can get dressed.” | Effort, help, and workarounds | “I can, but only sitting down.” |
Let’s be honest: nobody lives inside a pain scale
You live inside a kitchen, a car, a workplace, a shower, a bed, a closet. The scale is a tool. It is not a house.
That is why a stronger report sounds like this: “My pain is 6 at rest, but 8 when I bend forward to put on socks. I used to stand while dressing. Now I sit down and need five minutes before walking downstairs.” That gives a clinician something to work with besides a lonely digit. It can also help distinguish whether the issue belongs in a broader pain clinic vs orthopedist conversation, rather than being treated as a vague complaint floating in the exam room.
Functional Pain Clues: What Doctors Often Need to Hear
Clinicians often need to know what pain prevents, delays, changes, or costs you.
Not just “Where does it hurt?” but “What can you no longer do the same way?” The NCBI Bookshelf’s clinical overview of chronic pain notes that clinicians should assess daily activities, mood, sleep, productivity, relationships, mobility, and self-care. In plain English: your closet belongs in the story.
“I can dress, but I need 20 minutes” is clinical gold
Time is data. If dressing once took 7 minutes and now takes 25, that change matters. It may show stiffness, weakness, fear of movement, fatigue, balance concerns, or pain flares after specific motions.
A sentence like “I can still do it” may accidentally hide the problem. A better sentence is: “I can still do it, but it takes three times longer and I need to rest afterward.” That is not complaining. That is reporting. Very different instrument, cleaner sound.
“I stopped wearing jeans” may matter more than “it hurts”
Clothing choices can reveal avoidance. Loose pants may mean waist pressure hurts. Slip-on shoes may mean bending is hard. Front-closure bras may mean shoulder rotation is limited. Button-free shirts may mean hand pain or numbness is interfering.
One reader once told me she thought she had “adapted well” because she found soft clothes that did not bother her hip. Then she realized she had not worn half her closet in 8 months. The wardrobe had become a quiet medical diary with hangers. If hip pain is part of that closet pattern, a guide to hip pain management for seniors may help frame what to discuss with a clinician.
The clue hiding in clothing choices, shoe choices, and shortcuts
Workarounds are not failures. They are often smart, practical, and dignity-preserving. But they also show what your body is avoiding.
- New clothing habits can show movement limits.
- Extra time can show functional decline.
- Recovery time can show the after-cost of a task.
Apply in 60 seconds: Name one clothing item you avoid now and write why.
Decision card: pain score only vs pain score plus function
When to use each report style
| Use this | When it helps | Example |
|---|---|---|
| Pain score only | Quick check, trend tracking, urgent triage conversation | “My pain is 8/10 today.” |
| Pain score plus function | Appointments, therapy visits, chronic pain tracking | “It is 8/10 when I lift my arm into a jacket.” |
Neutral action: Use the pain score for speed, then add one real-life anchor for clarity.
Getting Dressed Map: Which Body Movements Point Where
Getting dressed is not a diagnosis. It is a map.
Maps do not tell you everything, but they prevent wandering in circles. When you describe the exact dressing movement that triggers pain, your clinician may better understand which region, movement pattern, or daily limitation needs attention.
Overhead shirts: shoulder, neck, rib, and upper-back clues
If overhead shirts hurt, notice whether pain appears when the arm lifts, rotates, or lowers. Does it pinch at the shoulder? Pull along the neck? Wrap around the ribs? Does it feel sharp, dull, burning, tight, or weak?
Useful phrases include:
- “I cannot raise my arm above shoulder height.”
- “I can lift it, but lowering it hurts more.”
- “I avoid jackets because reaching backward is worse.”
- “I need help getting my right arm into a sleeve.”
When shoulder support enters the conversation, it may be worth asking about the difference between a shoulder immobilizer vs sling, especially if dressing, sleeping, or post-injury movement feels confusing.
Socks and shoes: hip, knee, back, nerve, and balance clues
Socks and shoes are the tiny courtroom where bending gets cross-examined. If bending forward causes back pain, hip pinching, leg symptoms, dizziness, or balance loss, say that clearly.
Do not just report “my back hurts.” Try: “When I bend to pull on socks, pain travels from my low back into my left leg, and I need to sit for 3 minutes before standing.” That sentence has location, trigger, radiation, and recovery. It has little work boots on.
If the pain travels down the leg, your dressing note may also help you explain patterns that overlap with L4, L5, or S1 sciatica symptoms, especially when bending, shoes, stairs, or walking all tell the same small story.
Buttons, zippers, and clasps: hand strength, dexterity, and coordination clues
Small fasteners can reveal hand stiffness, thumb pain, numbness, tremor, weakness, or coordination changes. If you avoid buttons or drop small items more often, mention it. Especially mention new numbness, new weakness, or sudden coordination problems.
Dressing Pain Clue Map
Reaching, shoulder rotation, neck tension, rib or upper-back strain.
Bending, hip motion, knee load, low-back symptoms, balance.
Grip, finger motion, thumb pain, numbness, coordination.
Pressure sensitivity, skin tenderness, abdominal, hip, or nerve irritation.
Show me the nerdy details
Pain assessment becomes more useful when it separates intensity, location, trigger, duration, interference, and recovery. A numeric score captures intensity at a moment. A dressing task adds movement context. This is why many pain and rehabilitation conversations include function: walking, sleeping, working, self-care, mood, and household tasks. The body’s response during a repeated daily task can reveal patterns that a single resting pain score may blur.
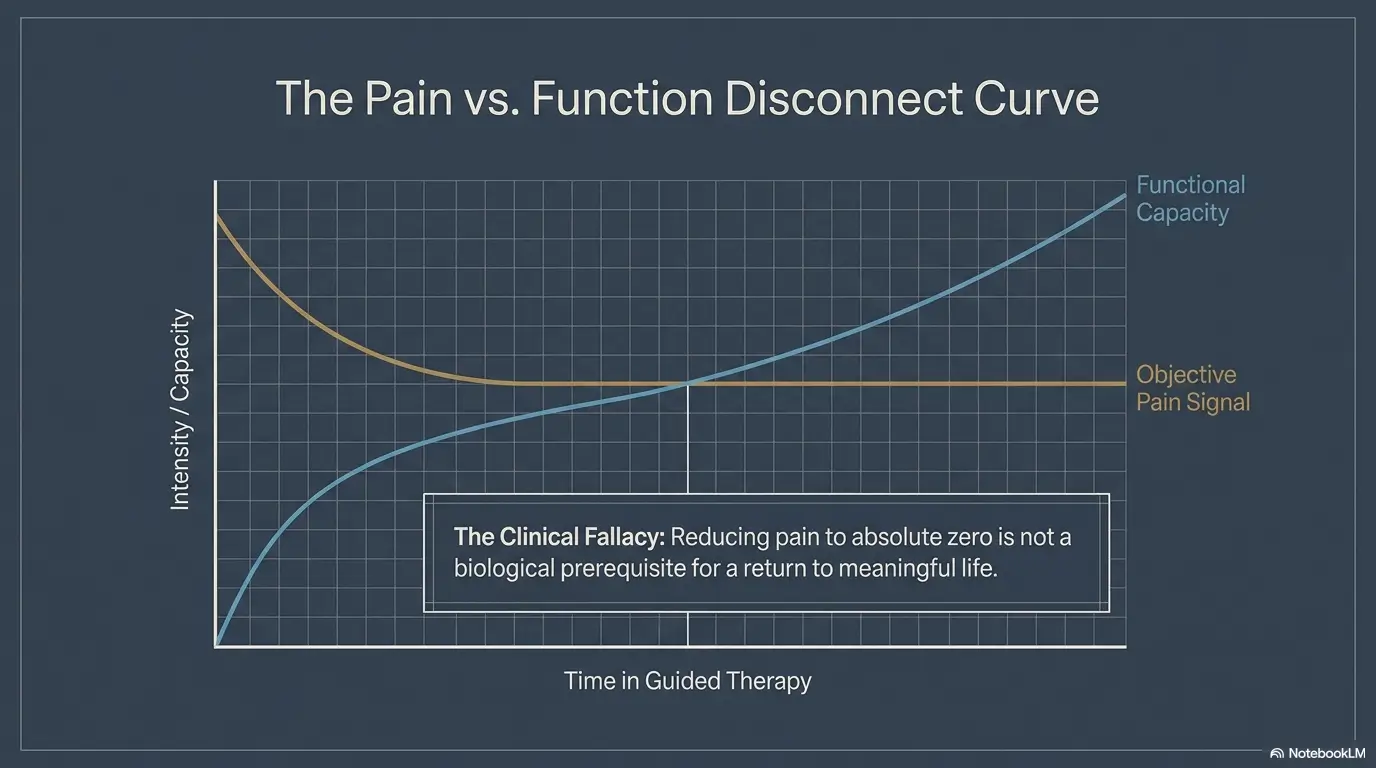
Don’t Do This: Reporting Pain Like a Weather Forecast
“It was bad this week” is understandable. It is also foggy.
Foggy pain reports happen because most people are tired, rushed, and trying not to sound dramatic. I get it. Nobody wants to enter a medical appointment carrying a 47-tab spreadsheet and the emotional energy of a courtroom stenographer. But a little structure can save everyone time.
Mistake 1: giving only the highest pain score of the week
The worst moment matters, especially if it was severe or frightening. But it may not represent your usual function. Tell your clinician both:
- Worst pain this week
- Average pain during a daily task
- What triggered the worst spike
- How long it took to settle
Example: “Worst was 9/10 after carrying laundry. Usual is 5/10 at rest and 7/10 while putting on shoes.”
Mistake 2: saying “fine” because you technically got dressed
Technically getting dressed is not the same as dressing normally. If you needed a chair, a grabber tool, help from a partner, a brace, pain medicine, heat, or 20 minutes of bargaining with gravity, that counts.
“Fine” is often a social word, not a medical one. It keeps conversations smooth, but it can sand down the useful edges.
Mistake 3: forgetting the workaround your body invented
The workaround may be the clue. Maybe you stopped reaching into high closets. Maybe you dress the painful arm first. Maybe you buy shoes that do not need tying. Maybe you choose soft waistbands because pressure feels unbearable by noon.
Eligibility checklist: should you track dressing pain?
- Yes if dressing takes longer than it used to.
- Yes if you avoid certain clothing because of pain.
- Yes if you need help, tools, medication, heat, or rest to finish.
- No as a substitute for urgent care when red flags appear.
Neutral action: If two or more “yes” items fit, track one dressing task for 3 days.
The Workaround Diary: Your Body Has Been Leaving Breadcrumbs
Your body is clever. Sometimes too clever.
It creates little detours so you can keep living: sitting to dress, choosing slip-ons, avoiding tight sleeves, using the wall for balance, skipping jewelry clasps, buying softer clothes. These adjustments can protect your day. They can also hide the fact that your function has changed.
Sitting down to dress when you used to stand
Sitting may be safer and wise, especially if balance is uncertain. But a new need to sit can reveal pain, weakness, dizziness, stiffness, or fear of falling. That detail belongs in your appointment note. If sitting, showering, or transfers are becoming harder, the same observation can guide conversations about orthopedic home care equipment that supports daily routines without turning the home into a medical warehouse.
Try: “I started sitting to put on pants because standing on one leg feels unstable.” That is clearer than “getting dressed is harder.”
Choosing slip-on shoes because bending became a negotiation
Slip-on shoes are a beautiful invention. Tiny engineering poem. But if you switched because bending triggers pain, numbness, or breath-holding, the reason matters.
There is a difference between “I like convenience” and “I cannot bend forward without leg pain.” One is shopping preference. The other is clinical context.
Here’s what no one tells you: adaptations can hide decline
Adaptations are often healthy. They preserve independence. But when every adaptation gets filed under “I’m managing,” decline can become invisible.
Quiet clue: If your closet has changed more than your pain score, bring the closet story to the visit.
Short Story: The Jacket That Finally Explained the Shoulder
Mara kept telling her clinician her shoulder pain was “around a 5.” That sounded manageable, and in a way it was. She could type. She could sleep if she stacked pillows like a small architectural project. But one chilly morning, she stood by the door for nearly 4 minutes trying to get her right arm into a jacket.
She laughed at first, then got quiet. The pain was not only pain. It was delay, awkwardness, dependence, and a tiny fear of leaving the house. At her next visit, she said, “I can work, but I cannot put on a jacket without help.” That sentence changed the conversation. Her clinician asked better movement questions, checked range of motion, and adjusted the plan. The pain score had whispered. The jacket had spoken in full paragraphs.
Who This Is For / Not For: Use the Clue Wisely
The dressing clue is practical, but it is not magic. It is a flashlight, not a verdict.
Use it to communicate clearly. Do not use it to diagnose yourself at midnight while scrolling with one eye open and the other eye bargaining with anxiety. The internet is very talented at turning a sore shoulder into a thunderstorm.
For chronic pain patients trying to explain daily limitations
If you live with chronic pain, you may already know the odd problem of sounding either too calm or too intense. Functional examples help. They let you say, “Here is how pain affects my morning,” without needing to perform suffering like theater.
This can be useful for primary care, physical therapy, pain medicine, rheumatology, orthopedics, neurology, occupational therapy, and rehabilitation visits. If you are deciding where the conversation should start, a broader overview of orthopedic pain management can help you sort symptoms, conservative care, imaging questions, and referral timing.
For caregivers tracking changes without interrogating someone
Caregivers can use dressing observations gently. The goal is not surveillance. It is support.
Instead of asking, “How bad is your pain now? Now? Now?” try noticing patterns: “I saw shoes were harder this week. Would it help to write that down for your appointment?” That lands softer. Less police siren, more porch light.
Not for self-diagnosing sudden, severe, or dangerous symptoms
Do not use a dressing log to wait out symptoms that need urgent care. Severe injury, new weakness, numbness, falls, trouble breathing, dizziness, fever with stiff neck, or bowel/bladder changes are not “track for 3 days” moments.
The 3-Day Dressing Log: A Better Note for Your Appointment
You do not need a perfect journal. You need 3 ordinary mornings and a note short enough to survive real life.
The goal is not to impress your clinician with stationery. The goal is to bring clear, usable details into a short visit. Most appointments do not have time for a novel. They do have time for a clean pattern.
Track the task, body area, workaround, and recovery time
Use this format:
| What to track | Example |
|---|---|
| Task | Putting on socks |
| Body area | Low back and left leg |
| Pain score | 6/10 while bending, 3/10 at rest |
| Workaround | Sat on bed, used wall to stand |
| Recovery | Needed 5 minutes before walking normally |
Use plain language your clinician can act on
Plain language is powerful. “My hip catches when I lift my foot into pants” is better than “my musculoskeletal experience is complex.” True, perhaps. But also wearing a lab coat made of fog.
Try these sentence starters:
- “I used to be able to…”
- “Now I have to…”
- “The hardest movement is…”
- “It changes my day because…”
Add one sentence: “This changed my day because…”
This sentence translates pain into impact. It may reveal missed work, skipped exercise, mood changes, sleep loss, fear of leaving home, or dependence on another person. If the appointment is about persistent back or leg pain and conservative care has not helped, this kind of function-first detail may also support a clearer MRI referral for orthopedic pain discussion.
Mini calculator: dressing impact score
Use this simple self-check. No storage, no fancy machinery, no tiny robot judging your socks.
- Give 1 point if the task took more than twice as long as usual.
- Give 1 point if you used a workaround or help.
- Give 1 point if you needed recovery time afterward.
Output: 0–1 points means “minor change to watch.” 2–3 points means “bring this to your clinician or therapist.”
Neutral action: Track the same task tomorrow and compare the score.
Pain Score Plus Function: The Stronger Combo
This is not an argument against pain scores. It is an argument against lonely pain scores.
A number with a functional anchor becomes much more useful. It tells your clinician not only how much pain you feel, but when it shows up, what it blocks, and whether your daily life is shrinking around it.
Keep the 0–10 number, but attach a real-life anchor
Use this formula:
“My pain is ___/10 when I ___, and I have to ___ afterward.”
Examples:
- “My pain is 7/10 when I put on socks, and I have to sit before walking.”
- “My pain is 6/10 when I fasten my bra, and I need help with the clasp.”
- “My pain is 5/10 at rest but 8/10 when I lift my arm into a coat.”
Compare “pain at rest” with “pain while dressing”
Pain at rest and pain with movement can tell different stories. If rest pain is low but dressing pain is high, the issue may be tied to movement, load, position, or pressure. If both are high, the conversation may shift toward overall control, sleep, safety, and next-step evaluation.
Do not force an interpretation. Just report the contrast.
Why function can show progress before pain disappears
Sometimes progress is not “my pain is gone.” Sometimes progress is “I can put on my shirt without help,” “I can tie shoes again,” or “I recover in 2 minutes instead of 20.”
That kind of progress matters. It is not glamorous, but neither is flossing, and apparently civilization depends on these small faithful acts. It can also be especially useful when physical therapy is not helping orthopedic pain in the way you expected, because function can reveal whether the plan needs adjusting or the goal needs sharpening.
- Use the number for severity.
- Use the task for context.
- Use recovery time for impact.
Apply in 60 seconds: Write one sentence using: “My pain is ___/10 when I ___.”
Common Mistakes: Small Reporting Gaps That Can Cost You Clarity
Pain reports do not need to be perfect. They need to be honest enough to be useful.
Here are the gaps that often make a real problem look smaller than it is.
Mistake 1: describing pain only when sitting still
Resting pain can be important, especially if it is severe, constant, or wakes you at night. But many people feel worse during movement. If you only report pain while sitting in the exam room, the clinician may miss the morning obstacle course.
Mistake 2: ignoring fatigue after the task is over
Fatigue counts. If dressing drains you before the day begins, say so. That may affect treatment goals, pacing, therapy planning, work accommodations, or home safety conversations.
Try: “After dressing, I need 10 minutes before I can make breakfast.” Simple. Useful. No violin section required.
Mistake 3: underreporting because you completed the task anyway
Completion is not the only metric. Effort matters. Help matters. Avoidance matters. Pain afterward matters.
If you crawled across the finish line, it is still a finish line, but the crawling is relevant.
Mistake 4: forgetting medications, braces, heat, ice, or help used beforehand
Before-task support changes the interpretation. Dressing after medication, heat, a brace, or help from another person is different from dressing independently with no support. If you rely on a brace or support to get through the morning, it may be worth reviewing whether HSA-eligible braces and supports fit your care plan and budget.
Quote-prep list: what to gather before a pain visit
- Your 3-day dressing log
- Current medications and timing
- Braces, supports, heat, ice, or tools used
- Recent injuries, falls, infections, or activity changes
- Top 2 daily tasks you most want back
Neutral action: Put these details in one phone note before the appointment.
When to Seek Help: Red Flags Beyond the Closet Door
Most dressing-related pain clues are not emergencies. But some symptoms should not be turned into a home tracking project.
Mayo Clinic guidance says to get medical care right away for muscle pain with trouble breathing or dizziness, extreme muscle weakness with problems doing routine activities, high fever with stiff neck, or severe injury that prevents movement. That is the part where the sock diary closes and real-time care takes the stage.
Get urgent care for pain with breathing trouble, dizziness, fever with stiff neck, severe injury, or extreme weakness
Seek urgent help if pain appears with symptoms that suggest a serious systemic, neurologic, or injury-related problem. Do not wait 3 days to see whether your jacket becomes more cooperative.
Call a clinician when pain is worsening, persistent, unexplained, or interfering with normal daily life
If pain keeps changing your routine, sleep, mood, work, caregiving, walking, dressing, or bathing, call a licensed clinician. You do not need to wait until you are in crisis. Early conversations can prevent small problems from becoming large, expensive, highly theatrical problems. When symptoms are persistent but not clearly urgent, comparing urgent care vs orthopedic clinic options can help you choose a reasonable next step.
Don’t wait if dressing problems come with numbness, new weakness, falls, or loss of bladder/bowel control
New weakness, numbness, falls, or bowel/bladder changes deserve prompt medical guidance. These are not “maybe I slept funny” details to quietly file away. They are important. For severe low-back or leg symptoms, it is especially important to know cauda equina syndrome red flags, because some warning signs should be treated as urgent.
- Use logs for patterns, not emergencies.
- Report daily-life interference early.
- Take new weakness, numbness, falls, and bowel/bladder changes seriously.
Apply in 60 seconds: Save your clinic’s phone number and local urgent care option before you need them.
Next Step: Try the One-Shirt Check Tomorrow Morning
Do not start with a complicated tracker. Start with one shirt.
The one-shirt check is simple enough to do before your day begins and specific enough to help later. Choose one dressing task you repeat daily. Then notice what changed. No drama. No detective hat. Just a small lantern in the morning.
Pick one dressing task you do every day
Choose one:
- Putting on socks
- Pulling on pants
- Putting on a shirt
- Fastening a bra, belt, button, or zipper
- Tying shoes or choosing slip-ons
Write down what changed: time, pain, workaround, help, and recovery
Use this 5-line note:
Task: Shirt
Pain: 6/10 when lifting right arm
Workaround: Put painful arm in first
Help/tool: None today
Recovery: Shoulder ached for 15 minutes afterward
Bring that note to your next visit, not just your pain score
Your clinician does not need a perfect autobiography. They need a clear pattern. A 3-day log can help shape better questions: What movement triggers it? Is it improving? What makes it worse? What daily goal matters most?
Coverage tier map: how detailed should your note be?
| Tier | Detail level | Best for |
|---|---|---|
| Tier 1 | Pain score only | Quick check-ins |
| Tier 2 | Pain score plus one task | Routine appointments |
| Tier 3 | Task, workaround, recovery time | Physical therapy or chronic pain visits |
| Tier 4 | 3-day pattern plus triggers | Worsening or unclear pain |
| Tier 5 | Pattern plus red flags or safety concerns | Prompt medical contact |
Neutral action: For most visits, Tier 3 is the sweet spot: clear, short, and useful.
FAQ
Is getting dressed really a useful pain clue?
Yes. Getting dressed combines reaching, bending, gripping, balancing, twisting, and tolerating clothing pressure. That makes it a compact daily-function test. It does not diagnose the cause of pain, but it can show how pain changes real life.
Should I stop using a pain score?
No. A pain score can still be useful, especially for tracking intensity over time. The stronger approach is to pair the number with function: “My pain is 6/10 when I pull on socks, and I need to sit down afterward.”
What should I tell my doctor if dressing hurts?
Describe the specific task, body movement, workaround, and effect on your day. For example: “I can’t lift my right arm into a jacket without help,” or “I stopped wearing lace-up shoes because bending triggers back and leg pain.” If the visit involves senior mobility, arthritis, or recovery planning, you may also want to ask how your note fits into senior orthopedic pain management.
What if I can still get dressed, but it takes much longer?
That still matters. Time, effort, fatigue, and avoidance are functional clues. “I can do it, but it takes 25 minutes and I need to rest afterward” gives more useful context than “I’m okay.”
Can clothing choices reveal pain patterns?
Yes. Switching to slip-on shoes, loose pants, front-closure bras, elastic waistbands, or button-free shirts may reveal pain avoidance. These changes are not failures. They are data with sleeves.
When is pain while dressing serious?
Pain may need prompt medical attention if it is sudden, severe, worsening, linked to injury, or paired with weakness, numbness, fever, dizziness, breathing trouble, falls, or trouble with routine daily activities. When in doubt, contact a clinician.
How many days should I track dressing problems?
Three ordinary days can be enough to reveal a pattern. Track the same task each day, such as socks, shoes, shirt, jacket, or bra or clasp. Note pain level, movement difficulty, workaround, and recovery time.
Can this help with physical therapy?
Yes. Functional details can help a physical therapist understand which movements matter most in daily life. “Overhead shirts hurt” is more actionable than “my shoulder hurts sometimes.”
Conclusion: Bring the Morning Into the Exam Room
The morning closet tells a quiet truth. Not because clothing is medically mystical, but because getting dressed is one of the first daily tests of movement, balance, grip, flexibility, pressure tolerance, fatigue, and independence.
A pain score can still help. Keep it. But do not let it stand alone like a single chair in an empty room. Pair it with function. Say what happened when you pulled on socks, lifted your arm into a sleeve, fastened a clasp, tied shoes, or needed to rest afterward.
Tomorrow morning, try the one-shirt check. In 15 minutes or less, write one note: task, pain score, workaround, and recovery time. Bring that note to your next appointment. It may be the small, ordinary detail that finally helps your clinician see the whole picture.
Last reviewed: 2026-05
Tags: pain communication, chronic pain, functional pain assessment, patient notes, daily living
Meta description: Learn why getting dressed can reveal pain patterns better than a pain score and how to track useful clues for your clinician.
