
Beyond the Needle: Solving the Sciatica Label Trap
Two trigger point injections. A day of relief. Then the same electric line down the leg, right on schedule, like your nervous system is keeping receipts.
If you’re chasing “sciatica” with needles, the problem often isn’t the clinician’s aim. It’s the address. Trigger point injections can be a clean win when the pain is myofascial—meaning a specific glute or hip muscle spot reliably recreates your exact referral pattern.
But when the real driver is lumbar radiculopathy from a disc herniation or spinal stenosis, you can end up with a perfectly executed procedure that never had a chance to fix the main generator.
Keep guessing and you risk the expensive loop: repeat shots, shrinking walking tolerance, creeping numbness, and rehab that starts too late or in the wrong direction.
This post helps you sort “muscle mimic” from “nerve-root headline” using practical clinic clues:
- • Physical Screens: Straight leg raise vs. Slump test.
- • Neurological Mapping: Understanding dermatomes and myotomes.
- • Strategic Next Steps: PT with a hypothesis, imaging timing, or ESI conversations.
No heroics. Just pattern data, clearer targets, and fewer wasted visits.
Keep reading. The first section fixes the label trap.
This is educational, not medical advice. “Sciatica” has multiple causes, and injections carry risks (infection, bleeding, nerve injury, medication side effects). If you have new weakness, numbness in the groin/saddle area, loss of bladder/bowel control, fever, history of cancer, major trauma, or severe unrelenting pain, seek urgent evaluation.
Fast Answer: Trigger point injections can help myofascial pain that mimics sciatica, but they often miss the mark when symptoms come from nerve root irritation (like a herniated disc or spinal stenosis). If pain shoots below the knee with numbness, tingling, or weakness, you may need a different workup and treatment plan. The key is matching the injection target to the pain generator, not the label “sciatica.”
Table of Contents
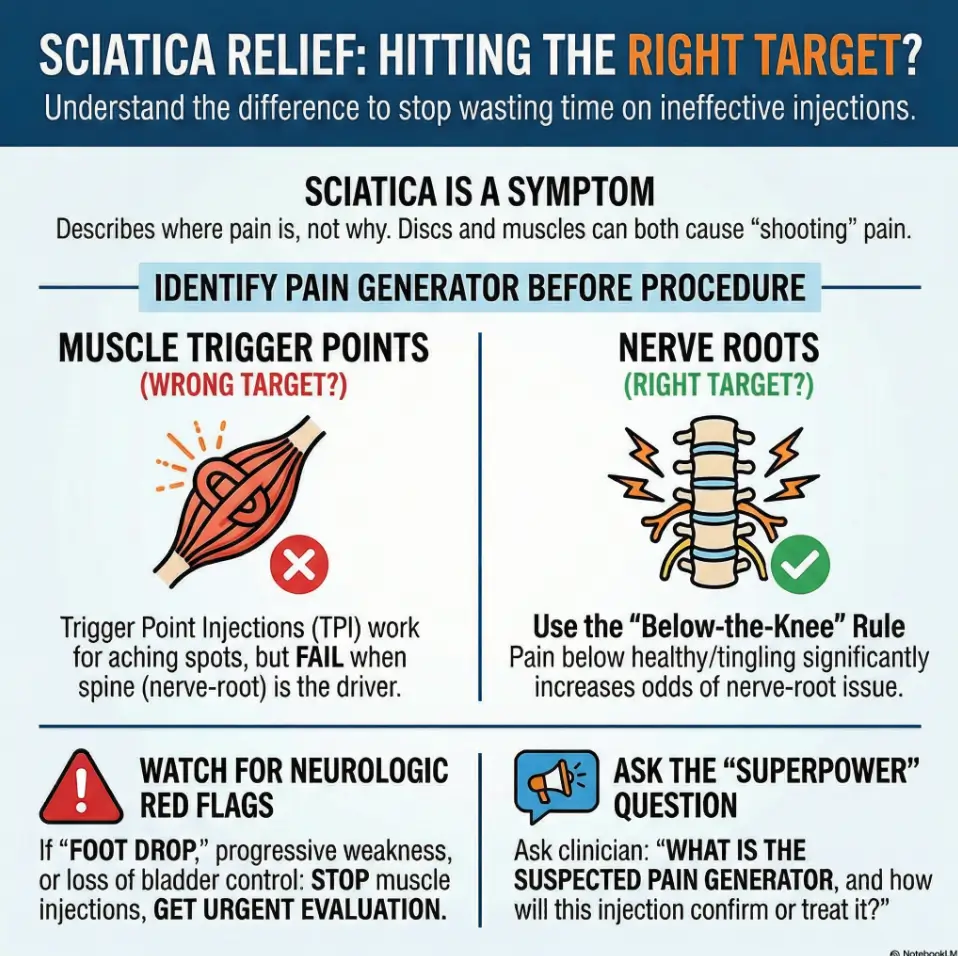
Wrong target first: Why “sciatica” is a nickname, not a diagnosis
Label trap: “Sciatica” describes a route, not a root cause
“Sciatica” is one of those words that sounds precise, like a GPS coordinate. But in real clinics it’s more like “stomachache”: it describes where the problem shows up, not why it’s happening. The sciatic nerve is a big cable. Lots of things can irritate it or imitate it. That’s why two people can both say “sciatica” and need totally different care.
Quick lived-experience note: I’ve watched patients walk into a visit saying “I need the sciatica shot,” and walk out with a procedure that technically happened… but didn’t match the mechanism. It’s not because anyone is careless. It’s because the label is vague, and pain can be a talented impersonator.
Two look-alikes: nerve pain vs referred muscle pain (and why they get confused)
Here’s the basic split that matters for injections:
- Nerve-root driven pain (radiculopathy): typically comes from irritation/compression near the spine (disc herniation, stenosis). Often includes numbness, tingling, weakness, and pain that behaves like an electric line. If you want a clean anatomy compass, see L4 vs L5 vs S1 sciatica patterns.
- Referred myofascial pain: comes from muscle trigger points (commonly deep glute muscles, hip rotators). It can radiate and feel surprisingly “nervy,” but it’s not the nerve root as the main driver.
Why the confusion? Because both can “shoot.” Both can flare with sitting. Both can make you limp like you’re auditioning for a pirate movie. And both can exist together. The trick is deciding what’s primary today.
Curiosity gap: The one question that changes the entire plan
Can you reproduce your leg pain by pressing a specific muscle spot, and does that pressure create a familiar referral pattern?
If a clinician can press a deep glute trigger point and you say, “That’s it, that’s the exact line,” trigger point injections become more plausible. If you can’t reproduce it that way, but you can reproduce it with nerve-tension tests (like a straight leg raise), the story starts pointing away from a muscle-first approach. (If you want to practice the basics safely, see how to do a straight leg raise test at home.)
- Muscle trigger points can mimic sciatica.
- Nerve-root irritation often needs a different plan.
- Your job is to bring pattern data, not just a label.
Apply in 60 seconds: Write one sentence: “My pain starts in ___ and travels to ___, and it changes most with ___.”

Pain map clues: When trigger points are likely the right tool
Local-to-radiating patterns: glute/hip trigger points that imitate nerve pain
Trigger points are cranky muscle fibers that behave like a bad roommate: loud, persistent, and weirdly influential. Deep glute muscles (including piriformis and friends) can refer pain into the buttock, hip, and sometimes down the thigh. When a clinician palpates a tender band and it produces a recognizable pain line, that’s meaningful. (If you’re stuck in the “piriformis vs spine” debate, this comparison can help you frame it as a hypothesis, not a religion: sciatica vs piriformis syndrome.)
Personal anecdote, the small kind: I’ve seen people show up terrified they “blew a disc,” then a careful exam finds a deep glute trigger point that recreates the whole complaint. A few targeted treatments plus rehab later, they’re back to walking without doing the “protective penguin shuffle.” It happens. Not always, but enough to respect it.
“Below the knee” matters: a simple boundary with big implications
This isn’t a perfect rule, but it’s a useful one: pain that consistently travels below the knee, especially with numbness/tingling, raises the odds that a nerve root is involved. Trigger points can refer far, yes. But classic nerve patterns love the below-knee zone. If you’re trying to pin down whether this is more “disc story” or “sciatica label,” see sciatica vs herniated disc.
Curiosity gap: Why your calf can hurt even when your back feels fine
Nerves are dramatic. You can have minimal back pain and still get strong leg symptoms because the nerve root irritation is “upstream,” while the sensation is “downstream.” That’s why the absence of back pain doesn’t automatically make it muscular.
Show me the nerdy details
Referred pain from myofascial trigger points is thought to involve local ischemia, sensitized nociceptors, and central sensitization patterns that can “project” pain beyond the muscle itself. Nerve-root pain involves mechanosensitivity and inflammatory mediators around the dorsal root ganglion and nerve root, which can produce distal symptoms even when the spine doesn’t feel acutely painful.
- YES if pressing a specific muscle spot reliably reproduces your leg pain pattern.
- YES if symptoms are mostly aching/tightness and fluctuate with posture, stress, or prolonged sitting.
- NO / PAUSE if you have progressive weakness, clear numbness, or foot drop.
Apply in 60 seconds: Ask your clinician: “Which muscle trigger point reproduces my symptoms, and what referral pattern do you expect?”
Red flags for the wrong needle: Signs it’s not primarily myofascial
Neurologic hints: numbness, tingling, weakness, reflex changes
Muscles can hurt fiercely without harming nerve function. When you start seeing neurologic changes, the plot thickens:
- Persistent numbness or tingling in a dermatomal pattern (a “stripe” down the leg/foot).
- Weakness (tripping, toe dragging, difficulty with heel/toe walking).
- Reflex changes a clinician can detect.
Function tells the truth: walking tolerance, foot drop, and sleep disruption
I’m a big believer that function is a better witness than pain intensity. Pain can exaggerate. Function tends to testify under oath.
- Walking tolerance collapsing (you can’t walk as far as last week) can suggest stenosis or significant irritation. If walking is the trigger, this deep dive may help you spot patterns worth bringing to a clinician: sciatica pain when walking.
- Foot drop is a “stop and get evaluated” sign.
- Night pain that is severe and unrelenting deserves careful medical attention, especially with systemic symptoms.
Pattern-interrupt micro: Let’s be honest… if you’re losing strength, “tight muscles” isn’t the full story
This is where people get accidentally gaslit by optimism. Everyone wants the easy answer. But progressive weakness is not a place to bargain. It’s a place to get assessed.
- Muscle pain is common, but weakness is not “just tightness.”
- Walking tolerance changes can be diagnostic gold.
- Short-lived relief is information, not proof you should repeat the same shot.
Apply in 60 seconds: Test heel-walk and toe-walk for 10 steps each side and note any asymmetry.
The “mimic lineup”: 6 common sources of sciatica-like pain (ranked by injection relevance)
Lumbar disc herniation: when the nerve root is the headline
Disc herniations can irritate a nerve root and create classic radiating symptoms. If this is your primary driver, trigger point injections might calm secondary muscle guarding, but they rarely fix the core issue by themselves. If you’re trying to understand conservative options and escalation triggers, see herniated disc sciatica treatment.
Natural authority note: orthopedic guidance commonly discusses epidural steroid injections as a short-term option for nerve-root inflammation after weeks of conservative care, not as a first reflex for every leg pain episode. If you’re weighing injection types, this comparison helps people ask sharper questions: SI joint injection vs lumbar epidural steroid injection.
Spinal stenosis: when standing and walking rewrite your symptoms
Stenosis often shows up as “I’m fine sitting, but walking/standing is brutal.” People describe needing to lean forward on a cart like it’s a mobility device disguised as grocery shopping. Trigger points can coexist, but the pattern often demands a broader plan.
Piriformis/deep gluteal syndrome: the controversial middle ground
This is the messy middle: sometimes it’s truly a deep glute entrapment; sometimes it’s myofascial referral; sometimes it’s a nerve root problem wearing a piriformis mask. Tenderness alone isn’t proof. The best clinicians treat this like a hypothesis, not a religion.
SI joint referral: pain that borrows the sciatic storyline
SI joint issues can refer into the buttock and posterior thigh. Sometimes you’ll feel it like a “beltline” ache with flares during transitions: getting out of a car, rolling in bed, standing from a chair. Trigger point injections may reduce nearby muscle spasm, but SI-directed assessment may matter more.
Hip pathology: when the joint frames the whole plot
Hip problems can masquerade as back/leg pain. If you have groin pain, clicking, reduced hip range, or pain with certain hip movements, it’s worth including the hip in the differential. I’ve seen patients spend months on spine treatments while the hip quietly ran the show. If you want a practical “is this hip or spine?” sorting tool, see hip vs spine pain.
Pure myofascial pain: when trigger point injections can be a clean win
This is the “clean win” scenario: clear trigger points, reproducible referral, minimal neurologic symptoms, and a plan that pairs injections with rehab so the muscle stops re-learning the same bad habit.
Show me the nerdy details
“Sciatica-like” symptoms can be produced by different mechanisms: mechanical nerve-root compression, chemical irritation from inflammatory mediators, peripheral nerve entrapment, joint referral patterns, and myofascial trigger point referral. The more your plan can state a primary mechanism, the less you rely on repeated trial-and-error procedures.
A patient I’ll call Jen had textbook “sciatica” down to the vocabulary: shooting pain, sitting intolerance, the whole soundtrack. She got two trigger point injections because the buttock was exquisitely tender, and each time she felt a brief, hopeful thaw, then the pain snapped back like a rubber band. The third visit was different: the clinician mapped the symptoms, tested strength, did a straight leg raise, and asked one annoying question: “Where exactly does the tingling start?”
It turned out the tingling lived in a very specific foot distribution, and her heel-walk on one side looked subtly weaker. The plan changed: imaging was discussed, rehab became more directional, and the injection conversation shifted from “more trigger points” to “confirming a nerve-root driver.” She didn’t magically heal overnight. But she stopped spending time on treatments that couldn’t logically solve her main problem.
Test-before-you-inject: Quick clinic checks that reduce “wrong target” treatments
Straight leg raise vs slump: what they suggest (and what they don’t)
These are “nerve tension” style tests. A positive result can support a nerve-root irritation story, but it’s not a divine verdict. What matters is the pattern: does the maneuver reproduce the familiar leg symptoms (not just hamstring tightness)? Does changing head/ankle position change the symptoms? Clinicians look for consistency and specificity.
Dermatomes and myotomes: matching symptoms to anatomy without overconfidence
Dermatomes are sensory maps. Myotomes are muscle-function maps. A skilled examiner uses them like a compass, not like a courtroom gavel. If your numbness and weakness line up neatly, it increases suspicion of nerve-root involvement. If it’s fuzzy, it doesn’t prove “it’s muscular.” It just means the story is mixed, or the nervous system is noisy.
Movement signature: flexion vs extension bias as a compass
Some patterns worsen with bending forward (flexion), others with arching/standing (extension). This can guide physical therapy strategies and help separate stenosis-like features from disc-like features. You don’t need to self-diagnose. You just need to notice what reliably changes symptoms.
Curiosity gap: Why a “normal MRI” can still mean real nerve pain
MRI is a snapshot, not a truth serum. Symptoms can outpace imaging. And imaging can show “bulges” that are not causing symptoms. That’s why good care uses imaging as a tool within a clinical picture, not as a scoreboard. If you’re stuck in the “my MRI is weirdly dramatic (or weirdly boring)” zone, see MRI pain mismatch and the practical breakdown of sciatica MRI vs X-ray.
- Input 1: Pain goes below the knee? (Yes/No)
- Input 2: Numbness/tingling or weakness? (Yes/No)
- Input 3: Walking tolerance shrinking week to week? (Yes/No)
Apply in 60 seconds: If you answered “Yes” to two or more, ask your clinician what the suspected nerve-level diagnosis is and how you’ll confirm it (exam, imaging, or referral).
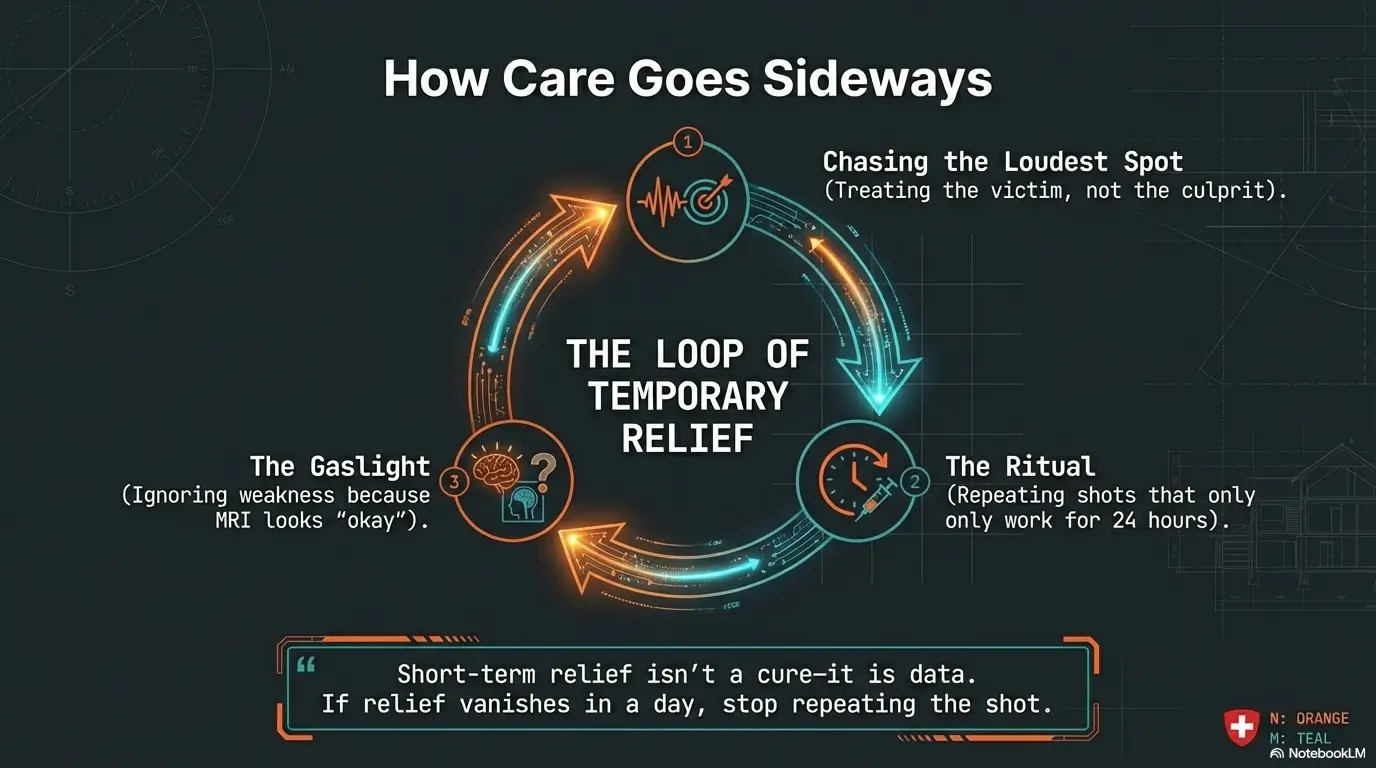
Common mistakes: How sciatica care goes sideways (even with good intentions)
Mistake #1: Treating the loudest tender spot instead of the pain generator
The loudest tender spot is often a bystander. Muscles guard. They spasm around pain. They become tender because they’re compensating. Treating them can feel good, but if the nerve root is the driver, relief may be brief.
Mistake #2: Repeating injections because “something should work eventually”
Repeat procedures without a clearer diagnosis can become an expensive ritual. If the first injection gives only hours or a day of relief, that can mean: wrong target, wrong technique, or a mixed condition. It’s not “failure.” It’s data. If you’re trying to interpret a flare after an injection (and not spiral into doom-searching), see steroid flare after injection.
Mistake #3: Skipping rehab and expecting the needle to do all the lifting
Even when trigger point injections help, they tend to work best as a window: reduce pain enough to restore movement, strength, and tolerance. Without that, the muscle often returns to its old job description: “Protect everything by tightening forever.” If you want the “what good PT actually looks like” version, see physical therapy for sciatica.
Pattern-interrupt micro: Here’s what no one tells you… relief that vanishes in 48 hours is data, not failure
Short relief can be diagnostic. It can reveal that part of your pain is muscular, but not the whole story. It can also reveal that you’re sensitized and need a plan that calms the system, not just the spot. (If PT makes symptoms feel “more nervy,” that’s a common fork in the road. See nerve pain vs muscle soreness after physical therapy.)
Show me the nerdy details
In procedure-heavy care, confirmation bias can creep in: if a tender point exists, it’s tempting to assume it’s the primary generator. A better model is Bayesian: each test, response, and functional change updates probability. A short-lived response may increase the likelihood of a mixed pain state or a non-targeted driver.
Don’t do this: 7 “looks helpful” moves that waste time (or increase risk)
Don’t chase pain with injections without a working diagnosis
It’s okay to start with a hypothesis. It’s not okay to keep poking without updating the hypothesis.
Don’t ignore progressive symptoms because you got “temporary relief”
Temporary relief can coexist with worsening weakness. If strength is declining, that’s a priority.
Don’t stack steroids/NSAIDs without discussing total risk load
This is especially important if you have diabetes, kidney issues, GI bleeding risk, or you’re on anticoagulants. Total exposure matters.
Don’t delay imaging/referral when red flags or deficits appear
Multiple medical bodies emphasize that imaging isn’t routinely helpful early for uncomplicated low back pain, but red flags and progressive neurologic deficits change that conversation. If you want a plain-language red-flag checklist that’s easy to hand to a worried family member, see cauda equina syndrome red flags.
Don’t confuse piriformis tenderness with proven nerve entrapment
Tenderness is common. Entrapment is specific. Demand a testable rationale.
Don’t let one negative test overrule the whole clinical picture
A negative straight leg raise doesn’t automatically equal “not nerve-related.” Patterns win, not single moments.
Don’t accept a plan that can’t explain your pain pattern
If the plan can’t clearly say, “We think it’s X because Y,” it’s not a plan. It’s a shrug in a lab coat.
- Trigger point injection when a muscle spot reproduces your symptoms and neuro signs are minimal.
- Epidural steroid injection discussion when symptoms follow a nerve pattern with numbness/tingling, weakness, or a strong positive nerve-tension test. If you’re comparing approach types, see TFESI vs interlaminar ESI for sciatica.
- Physical therapy-first when symptoms are improving, no deficits, and you need a movement strategy more than a procedure.
Apply in 60 seconds: Ask: “If this doesn’t help, what exact next step happens and what will it confirm or rule out?”
Who this is for / not for
For: sciatica-like pain with clear muscle tenderness and reproducible referral patterns
If you can point to a specific region (often deep buttock/hip) where pressure reliably recreates your leg discomfort, you’re in the zone where trigger point injections can make sense, especially as part of a broader plan.
For: people trying to decide between trigger point injection, epidural, PT, or imaging
This article is built for decision-making, not just symptom descriptions. If you’re trying to avoid the “random walk through procedures,” you’re the intended reader.
Not for: new weakness, bowel/bladder changes, fever, trauma, cancer history, or severe constant pain
If any of these are present, you need real-time medical evaluation. This is not a DIY zone.
Not for: anyone needing urgent evaluation or specialist-guided decision-making
If you’re unsure, default to safety. Get assessed.
When to seek help: The “don’t wait it out” checklist
ER now: saddle numbness, bowel/bladder dysfunction, rapidly worsening weakness
These symptoms can be associated with serious conditions like cauda equina syndrome. Don’t negotiate with your calendar about them.
Same-week evaluation: persistent numbness/weakness, significant walking limitation, night pain
If you’re losing function or symptoms are escalating quickly, waiting “to see if it calms down” can cost time you wish you’d used differently.
Ask about imaging: symptoms beyond 6 weeks or earlier if deficits/red flags
In the U.S., many primary care and evidence-based recommendations caution against early imaging for uncomplicated low back pain because it often doesn’t improve outcomes, but they also emphasize that red flags and neurologic deficits are different. In other words: timeline plus symptoms determines the imaging conversation.
Medication safety: who needs extra caution (blood thinners, diabetes, immunosuppression)
Injection decisions change if you’re on anticoagulants (blood thinners), have diabetes (steroids can raise glucose), or are immunosuppressed. Bring a med list. Ask about infection and bleeding risk. This is also where payer requirements can matter.
Commercial reality, neutral and practical: If you’re dealing with Medicare or large insurers (UnitedHealthcare, Aetna, Cigna, Blue Cross Blue Shield), coverage for injections often depends on documentation of exam findings, duration, conservative care attempted, and sometimes prior authorization. That’s not a reason to delay care. It’s a reason to show up prepared.
Better matching: What to consider instead of (or before) trigger point injections
Physical therapy with a hypothesis: nerve mobility, directional preference, core/hip strategy
PT works best when it’s not random YouTube stretching. A good plan has a hypothesis: “Your symptoms improve with X and worsen with Y, so we’ll bias movement toward what calms the nerve and rebuild tolerance.”
Small anecdote: I’ve seen “generic core exercises” irritate people for weeks, then a therapist changes one variable (directional preference, nerve glide dosage, pacing) and suddenly the nervous system stops throwing tantrums.
Epidural steroid injections: when nerve root inflammation is the likely driver
These are not magic, and they’re not risk-free. But when your pattern fits nerve-root irritation, an epidural steroid injection can be discussed as a tool for short-term relief that helps you engage in rehab and regain function. If you’re trying to set expectations in a non-doom, non-hype way, see epidural steroid injection relief timeline.
Diagnostic blocks: when the goal is confirmation, not just symptom relief
Sometimes the most valuable “injection” is one that clarifies the target. Diagnostic blocks can help confirm or refute a suspected source, reducing the risk of repeating the wrong treatment.
Lifestyle levers: sleep positions, pacing, walking strategy, and flare plans
- Sleep: experiment with pillow placement (between knees side-lying, under knees back-lying) to reduce nerve tension.
- Pacing: break sitting into chunks and stand before symptoms spike.
- Walking strategy: short frequent walks can beat one heroic stroll that triggers a two-day flare.
Shared decision-making: choosing the lowest-risk next step with the best signal
The best clinicians will talk in probabilities: “Most likely X, less likely Y; here’s the next step that gives us the best information with the lowest risk.” That’s the energy you deserve.
- Spot pressure recreates familiar pain line
- Aching/tightness dominates
- Minimal numbness/weakness
- Improves with heat/massage/movement
- Pain below knee with tingling/numbness
- Weakness, reflex changes, foot drop
- Nerve-tension tests reproduce symptoms
- Walking/standing pattern suggests stenosis
- Some muscle tenderness + some neuro signs
- Response to injections is brief/inconsistent
- Hip/SI features overlap
- “Normal MRI” but symptoms persist
Next step: One concrete action you can take today
Write a 7-day symptom log that forces clarity (location, below-knee, numbness, weakness, triggers, walking tolerance)
Make it painfully simple. Seven rows. Same time each day if possible. Track:
- Where it starts (back, buttock, hip)
- Where it travels (thigh, calf, foot)
- Below knee? (yes/no)
- Numbness/tingling (yes/no, where)
- Weakness (yes/no, what task)
- Walking tolerance (minutes or blocks)
- Top 2 triggers (sitting, bending, standing, coughing, etc.)
Bring one “pain map” diagram to your appointment and ask: “What is the suspected pain generator, and how will we confirm it?”
This question is your polite superpower. It forces specificity. It invites shared decision-making. It also quietly filters out vague plans.
- Your 7-day symptom log (one page).
- A current medication list (include blood thinners and diabetes meds).
- Prior imaging reports (if any) and prior procedure notes (what was injected and where).
- Your insurance card + whether you need prior authorization for injections.
- One sentence goal: “I want to walk ___ minutes without flare,” or “I need to sit ___ minutes for work.”
Apply in 60 seconds: Call ahead and ask: “Do you need prior authorization for CPT-coded injections, and what documentation do you require?”
FAQ
Can trigger point injections help sciatica pain down the leg?
They can help if the leg pain is primarily referred from muscle trigger points (myofascial pain) or if muscle guarding is a major amplifier. If your symptoms are driven by nerve-root irritation (disc herniation, stenosis), trigger point injections may provide partial or brief relief but often won’t address the main driver.
How do I know if my pain is sciatica or a muscle trigger point?
Look for pattern clues: pain consistently below the knee with numbness/tingling or weakness leans nerve-root. Pain that can be reproduced by pressing a specific muscle spot and creates a familiar referral pattern leans myofascial. Many cases are mixed, which is why exam findings and functional tests matter.
Why does my MRI show a disc bulge but my doctor says it’s muscular?
Because imaging findings are common even in people without symptoms. A disc bulge on MRI doesn’t automatically mean it’s the pain generator. Clinicians try to match imaging to your specific symptom map, neurologic exam, and provocation tests. Sometimes muscle pain is primary; sometimes it’s secondary guarding around a nerve issue.
What’s the difference between a trigger point injection and an epidural steroid injection?
A trigger point injection targets a specific tight, painful muscle area to reduce myofascial pain and spasm. An epidural steroid injection targets inflammation around spinal nerve roots in the epidural space, aiming to reduce nerve-related radiating pain. Different target, different mechanism, different risk profile.
Can piriformis syndrome cause true sciatica symptoms?
It can, but it’s often over-diagnosed based on tenderness alone. Deep glute pain can refer down the leg (myofascial), and in some cases the sciatic nerve can be irritated in the deep glute region. The key is a testable hypothesis and an exam that rules in or out a spine-driven nerve-root story.
Should pain that goes below the knee change my treatment plan?
It should change the questions you ask. Below-knee pain, especially with tingling/numbness or weakness, increases suspicion of nerve involvement and may justify a nerve-focused evaluation. It doesn’t automatically mean surgery or an epidural. It means your target selection should be more careful.
How long should trigger point injection relief last if it’s the right target?
It varies. Some people feel immediate improvement from local anesthetic and then a more sustained change when rehab follows. If relief lasts only hours to a day and symptoms quickly return at full intensity, that can be a clue that the trigger point wasn’t the primary driver or that the overall plan needs adjustment.
When should I get imaging for sciatica-like pain?
Many evidence-based recommendations caution against routine early imaging for uncomplicated low back pain because it often doesn’t improve outcomes. But red flags, progressive neurologic deficits, or persistent symptoms (often discussed around the 6-week mark) can change that. Discuss your specific pattern and risks with a clinician.
Are trigger point injections safe if I’m on blood thinners or have diabetes?
They can be done in some cases, but risk assessment matters. Blood thinners can raise bleeding risk; steroids can affect glucose control. Always disclose medications and conditions. Your clinician may coordinate timing, adjust medications, or recommend alternatives depending on your situation.
What kind of physical therapy is best for sciatica vs referred pain?
Best PT is hypothesis-driven: symptom mapping, movement testing, and a plan that adjusts based on response. Nerve-root patterns may focus on directional preference, nerve mobility, graded exposure, and function goals. Myofascial patterns may emphasize trigger point management, hip mechanics, and strength with pacing.
Conclusion
Let’s close the loop from the hook: the step that sets off the lightning is often the step that reveals the truth. Not “I have sciatica,” but what exactly triggers it, where exactly it travels, and what function it steals. Trigger point injections are great when the pain generator is muscular. When they’re not, repeating them can become an expensive form of hope.
Your best next move is simple and doable in 15 minutes: draw a pain map, write a 7-day log, and bring the one question that forces clarity: “What is the suspected pain generator, and how will we confirm it?” That question turns the appointment from a procedure menu into a plan.
Last reviewed: 2026-02-25.
