Restoring Confidence in Every Step:
A Function-First Guide to Knee Osteoarthritis
Knee osteoarthritis usually does not announce itself with drama. It shows up as a chair that suddenly feels too low, a staircase that needs negotiation, or a 2 a.m. bathroom trip that no longer feels harmless.
Orthopedic pain management for seniors must be bigger than “how much does it hurt?” The real problem is walking confidence, morning stiffness, and the small home frictions that quietly make every movement more expensive.
This guide helps you spot where knee pain is really coming from in daily life, allowing you to make safer, simpler changes before a bad day becomes a bad week. Learn to manage movement, pacing, home setup, and support tools with an approach grounded in how older adults actually move at home.
Change the one friction point the knee keeps complaining about.
Fast Answer: Orthopedic pain management for seniors with knee osteoarthritis works best when the goal is not just lowering pain, but protecting walking, standing, sleep, and confidence at home. The most effective day-to-day approach usually combines joint-friendly movement, pacing, supportive footwear, targeted heat or ice, clinician-guided medication use, and home setup changes that reduce strain before pain quietly turns into instability.
Table of Contents
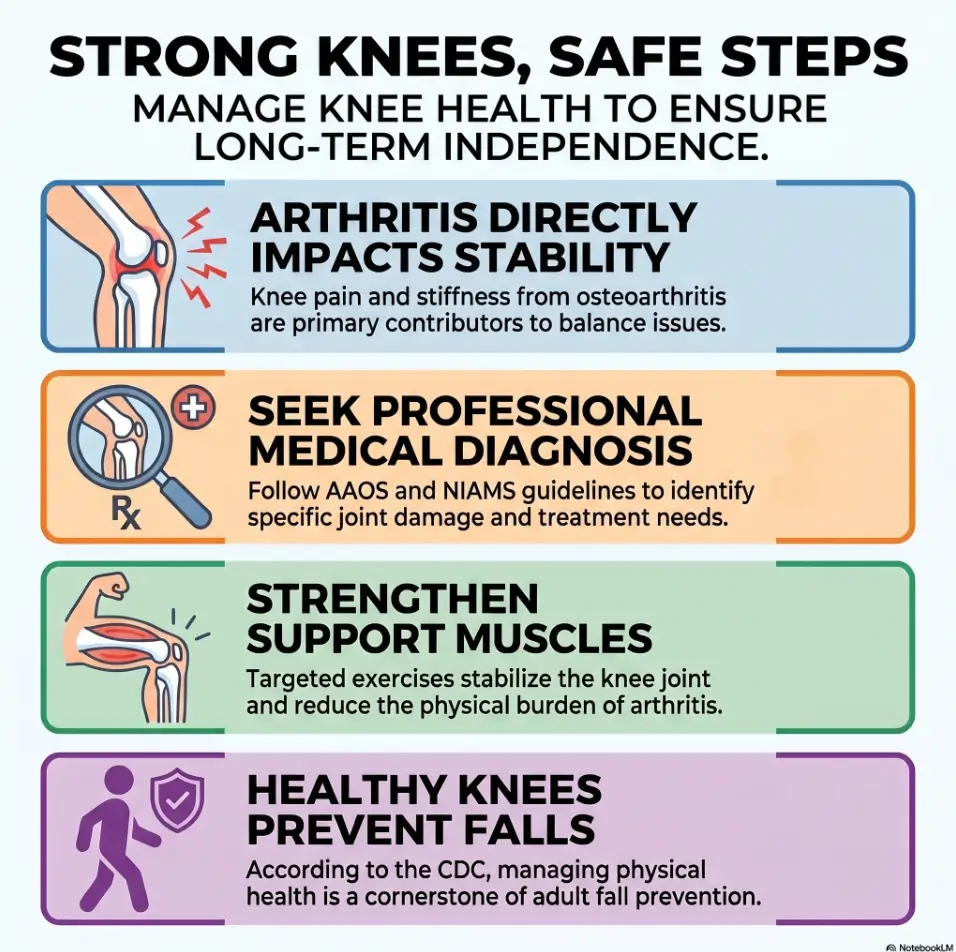
Start Here: Knee Pain Is Not Just Pain, It Is a Function Problem
Why knee osteoarthritis changes ordinary tasks before people fully notice it
Many people describe knee osteoarthritis as if the only question is how much the knee hurts. Real life is less tidy. Often the first losses are hidden inside ordinary motion: standing from a chair takes one extra push, turning in the kitchen feels less fluid, carrying laundry becomes a small strategic event. The knee does not only send pain. It edits behavior.
I have seen this pattern in countless home routines. A person says, “It’s fine, I can still do everything,” while quietly using both hands to rise from the sofa, avoiding the back steps, or standing at the sink in two-minute installments. The body starts making private bargains long before the mind writes the memo.
How stairs, chairs, bathrooms, and kitchen standing become the real pain map
That is why the useful pain map is rarely a pain score alone. It is a place map. Which chair? Which stair? Which time of day? Which turn near the bathroom door? Knee osteoarthritis becomes most visible where the home asks for repeated bending, rising, pivoting, or standing still. Those are the moments that decide whether the day feels manageable or expensive.
Why “I can still do it” may hide rising effort, slower recovery, and less safety
There is a world of difference between “I can do it” and “I can do it safely, repeatedly, and without paying for it tomorrow.” That difference matters more in older adults, where pain, balance changes, fatigue, and medication effects can pile into one another like badly stacked plates. The Centers for Disease Control and Prevention states that more than 1 in 4 older adults report falling each year, and falls are the leading cause of injury for adults 65 and older.
- Track painful places, not just painful numbers.
- Notice where rising effort is replacing easy movement.
- Assume repeated strain matters more than one dramatic episode.
Apply in 60 seconds: Pick one daily task and ask: does this feel painful, slow, unstable, or all three?
Who This Is For, and Who It Is Not For
Best for older adults with knee osteoarthritis trying to stay mobile, steady, and independent at home
This guide fits the person who wants fewer bad days, not fantasy knees. Maybe you are trying to keep walking the hall without that odd hitch. Maybe you want to get off the toilet without feeling like the room is watching. Maybe you want to keep doing your own meals without the kitchen turning into a negotiation chamber. For a wider senior-focused framework, this connects closely with elderly orthopedic pain management that protects independence instead of chasing comfort alone.
Helpful for adult children and caregivers noticing walking changes, slower transfers, or pain-related withdrawal
It also fits family members. Often a daughter or son notices the change first: fewer outings, slower standing, a hand lingering on furniture, a little more irritation when the topic of pain comes up. Those are not minor details. They are field notes.
Not for sudden knee injuries, major swelling after trauma, or possible infection
This is not the right playbook for a sudden injury after a fall, twisting event, or blow to the knee. It is also not a substitute for prompt evaluation when the joint becomes hot, red, rapidly swollen, or fever enters the scene.
Not for severe new calf pain, chest symptoms, or sudden inability to bear weight
New calf pain, chest symptoms, or sudden inability to bear weight belongs in the “get help now” basket, not the “let’s manage this at home” basket. A wise home routine is humble about its limits.
Eligibility checklist
- Yes: Pain and stiffness have been building gradually over time.
- Yes: The main problem is day-to-day walking, standing, rising, or sleep disruption.
- Yes: You want practical home changes and safer relief habits.
- No: There is sudden trauma, fever, major redness, or abrupt loss of weight-bearing.
- No: Symptoms now include chest pain or severe calf pain.
Next step: If you checked any “No,” use urgent medical guidance instead of a home-management plan.
Pain First, or Function First? The Better Way to Think About Relief
Why chasing lower pain scores alone can miss the real daily problem
A pain score can be useful, but it is a blunt instrument. Two people can both say “six out of ten” and live radically different days. One can still get to the bathroom safely, make lunch, and sleep. The other feels the knee buckle while turning and stops going outside. Same number. Different life.
How better orthopedic pain management protects walking, standing, turning, and sleep
That is why better orthopedic pain management asks function questions first. Can you rise from a chair without a dramatic push? Can you turn without grabbing? Can you stand long enough to brush your teeth or prep a meal? Can you get to the bathroom at night without the knee feeling like a bad rumor? The point of pain relief is not to win a scoreboard. It is to protect these acts while reducing fear and strain.
Why a tolerable day with safe movement often matters more than a perfectly numb knee
NIAMS notes that treatment goals include reducing symptoms and improving joint function. That pairing matters. A totally pain-free day is not always available. A tolerable day with safer movement often is.
In practice, that means you may choose the strategy that lets a person walk more steadily over the strategy that merely feels soothing for twenty minutes. It means the right shoe matters because it changes the whole day, while the wrong gadget can feel impressive and do almost nothing. It means a bathroom setup tweak may outperform a drawer full of hopeful purchases. The humble fix is often the adult in the room. For readers comparing options before imaging or escalation, orthopedic pain management before asking for MRI offers a useful companion lens: improve the daily pattern first, then decide what needs deeper investigation.
Show me the nerdy details
Function-first management is a behaviorally grounded approach: reduce painful loading, preserve strength and motion, and shrink moments of instability. For knee OA, symptom severity and functional limitation do not always move in perfect lockstep, which is why transfer ability, gait quality, and activity tolerance can be more actionable than a pain score alone.
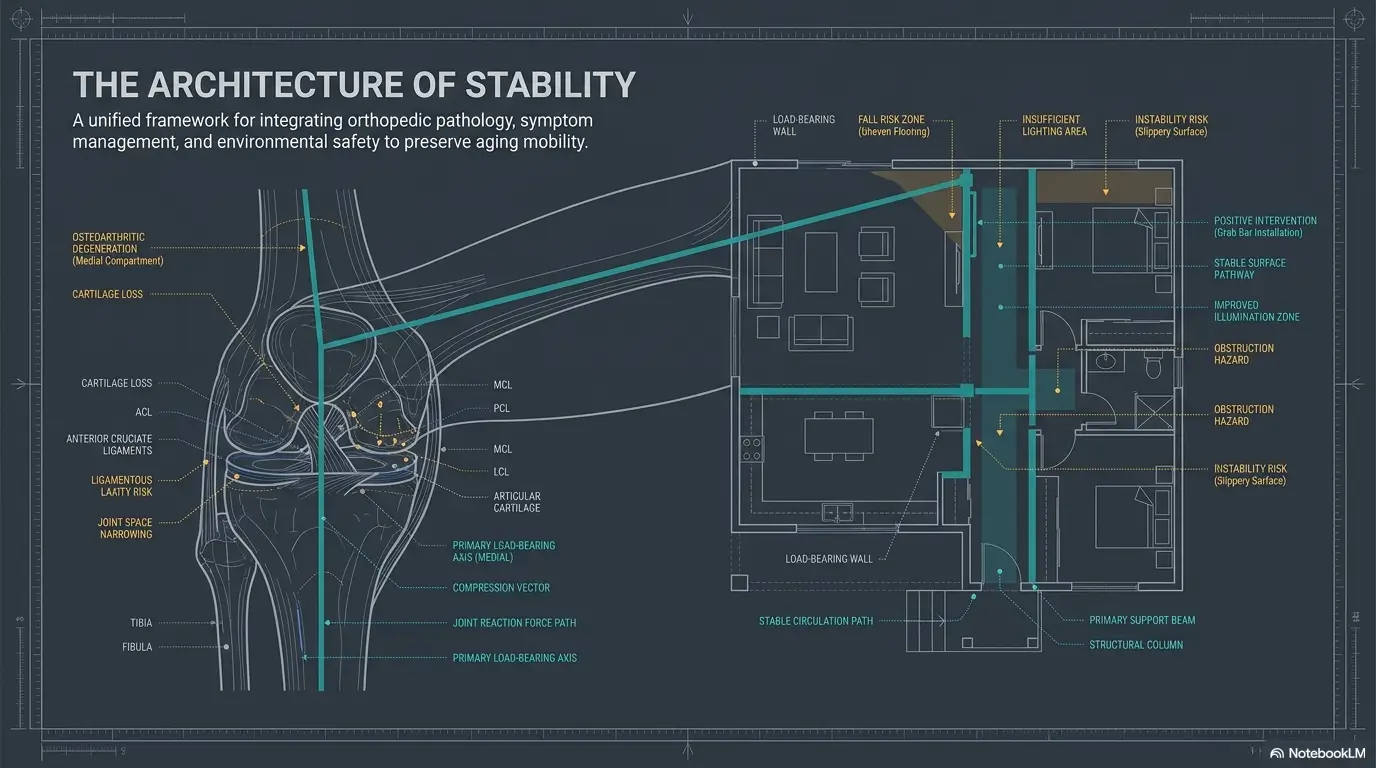
Morning Knee Stiffness Has a Plot Twist
Why the first steps of the day often feel worse than the afternoon
Morning stiffness has a special talent for making reasonable people feel 104 years old for three minutes. NIAMS notes that osteoarthritis often causes pain and stiffness after rest or inactivity. That is why the first steps can feel like the knee was replaced overnight with a rusty hinge and a legal disclaimer.
How warm-up routines can reduce the “rusted hinge” feeling without overdoing it
The answer is usually not brute force. A brief warm-up routine works better: a minute or two at the edge of the bed, gentle ankle pumps, a few slow knee bends within comfort, a steady stand, then short steps before launching into the full opera of the morning. Heat can help some people before movement. A cool pack can help others when swelling is louder. NIAMS says heat and cold therapies can lower joint pain, with heat improving blood flow and cold helping numb nerves around the joint and reduce swelling.
Let’s be honest: many bad days begin in the first ten minutes after getting out of bed
This is one of the least glamorous truths in home care: many bad days are not born at noon. They hatch in the first ten minutes. I remember an older relative who was “fine by breakfast” but looked uncertain every morning between bed and bathroom. That narrow passage, not the whole day, was the real clinical story.
Decision card: Morning stiffness
When A works better: If the knee feels stiff but not swollen, try 3 to 5 minutes of gentle movement and warmth before longer walking.
When B works better: If the knee feels puffy, hot, or more swollen after yesterday’s activity, use brief cooling and a shorter first walking block.
Trade-off: Warmth can improve ease; cooling can calm swelling. The right choice depends on what the knee is doing, not on household folklore.
Neutral action: Test one approach for two mornings and compare the first 15 minutes, not the whole day.
Movement Medicine: The Right Kind Helps, the Wrong Kind Collects Interest
Why gentle, regular movement often beats heroic exercise bursts
Knees with osteoarthritis usually prefer consistency over heroism. AAOS says exercise is recommended to improve pain and function, and lower-impact activity can help people stay active while putting less stress on the knee. NIAMS likewise says treatment commonly begins with exercise.
That is why a calm daily pattern often beats the famous “good day overreach.” A 10-minute walk most days is frequently more useful than a 45-minute push once the sun comes out and optimism starts making poor managerial decisions.
How walking, range-of-motion work, and leg strengthening support the knee without punishing it
The three broad lanes are simple. First, easy range-of-motion work so the knee does not feel seized by inactivity. Second, strengthening of the muscles that help support the joint, especially around the legs and hips. Third, walking or other low-impact movement in tolerable doses. You do not need a dramatic gym montage. You need a repeatable routine that your Tuesday self can actually tolerate.
Why rest alone can quietly make the knee less trustworthy over time
Rest matters, but total retreat has a cost. Too much underuse can make the knee feel even less dependable because strength, confidence, and movement tolerance start thinning out. The result is cruelly ironic: you rest to protect the knee, then the knee feels worse when asked to do ordinary work.
Here’s what no one tells you: underuse can make a painful knee feel even more fragile
Underuse is quiet. It does not announce itself as a mistake. It disguises itself as caution. But caution without circulation, motion, and strength can leave the joint feeling more brittle in daily life. The trick is not to force through pain. It is to keep the joint in conversation with movement.
A simple starting pattern: 5 to 10 minutes of walking, once or twice a day, plus brief seated or supported leg work, is often more sustainable than one “productive” session that ruins tomorrow. Ask a clinician or physical therapist to tailor specifics if pain is moderate to severe, balance is shaky, or other conditions complicate the picture. If therapy already feels stalled, it may help to review why physical therapy is not helping orthopedic pain before deciding the knee has simply “failed” the plan.
Home Friction Points: Where Knee Osteoarthritis Quietly Wins
Why low chairs, deep sofas, and awkward toilet heights make pain management harder
Homes often function like silent co-authors of knee pain. Low chairs demand deeper bending and a harder rise. Deep sofas swallow the hips and ask for a minor engineering project to get back out. Toilet height matters more than people expect because it combines bending, balance, urgency, and repeated daily use. The knee does not care whether the furniture was expensive. It only cares about angles and load.
How bathroom layout, bed height, and kitchen standing time shape the whole day
Bathrooms deserve special attention because they collect risk: slick surfaces, turning, urgency, dim light, and middle-of-the-night grogginess. Bed height matters because every morning starts there. Kitchens matter because they turn “just standing a little” into 15 or 20 minutes surprisingly fast. Pain loves accumulated standing more than many people realize.
Why reducing repeated strain matters more than buying random support gadgets
One sturdy adjustment that removes repeated strain can outperform three gadgets bought in a hopeful blur. A higher seat cushion, a more supportive chair, a reorganized kitchen counter, or a place to sit for meal prep can reduce daily load in ways the body actually notices. Good pain management is often an editing job.
- Low surfaces increase strain during transfers.
- Bathrooms and kitchens are high-frequency trouble spots.
- One environmental fix can beat several comfort products.
Apply in 60 seconds: Sit in the chair used most often and notice whether standing requires rocking, pushing, or a second attempt.
Home setup review list
- Chair height in the main sitting area
- Toilet height and grab support availability
- Bed height from floor to mattress top
- Time spent standing in the kitchen without breaks
- Night path lighting from bed to bathroom
Neutral action: Gather these details before comparing equipment or asking a clinician what change would help most.
Common Mistakes That Make Knee Osteoarthritis Harder to Live With
Waiting until pain spikes before changing pace, posture, or routine
By the time pain is shouting, the day is already more expensive. Many people wait until the knee flares before sitting, changing tasks, or slowing down. Earlier adjustment works better. Think of it as steering, not surrendering.
Doing too much on a “good knee day” and paying for it the next morning
This one is almost universal. A better day appears, and suddenly the house becomes a to-do list with a pulse. Floors get cleaned, laundry gets conquered, the pantry gets reorganized, and the next morning arrives with a bill. Good days are for wise progress, not revenge productivity.
Using unsupportive shoes because they are easy to slip on
Easy-on shoes can be helpful, but there is a line between convenient and flimsy. Unsupportive footwear can change how the whole leg manages load. A shoe that saves ten seconds but makes standing and walking less steady is a poor bargain.
Treating every flare like a sign that all movement should stop
Some flares do call for backing off. But many call for smarter dosing, shorter movement bouts, and better recovery, not complete shutdown. That difference matters. A flare is information. It is not always a command to freeze.
A small personal rule helps here: after any unusually active day, ask not “Was I strong enough?” but “Was that repeatable?” The body prefers repeatable.
Don’t Build the Day Around Pain Alone
Why orthopedic pain management works better when built around movement windows
Most people with knee osteoarthritis do not have a uniform day. They have windows. A better hour after warming up. A slump after errands. A rough patch after too much standing. A quieter stretch in late afternoon. Pain management gets smarter when the day is built around these windows instead of pretending the knee behaves the same at 8 a.m. and 8 p.m.
How to time chores, errands, walking, and rest before the knee starts bargaining back
Try putting the most bend-heavy or stand-heavy task into the best window, not merely the earliest convenient slot. Break chores into short blocks with pauses before symptoms spike. Pair movement with recovery on purpose. That might look unambitious on paper. In real life, it keeps the knee from turning one large task into a 36-hour argument.
Why shorter, repeatable effort blocks often beat one exhausting productivity burst
Three 10-minute effort blocks with short resets often beat one 30-minute grind, especially for cooking, tidying, or light housework. The mind sometimes resists this because it feels less heroic. The knee, however, is not hiring for heroism.
Infographic: A calmer daily rhythm for knee osteoarthritis
Warm up first. Let the knee join the day before asking it to negotiate stairs.
Do the most demanding task during the easiest movement period, not by the clock alone.
Use short effort blocks and sit before the knee starts demanding interest payments.
Set up lighting, support, and an uncluttered route before 2 a.m. makes everything less rational.
Support Tools That Help, and the Ones That Just Add Clutter
When canes, walkers, braces, or compression may actually reduce strain
Support tools are not moral tests. They are load-management tools. Used well, a cane, walker, brace, or compression option may reduce strain and help a person move more safely. NIAMS says a cane or walker can help with safe movement, stability, and lower pain when needed. AAOS patient guidance notes moderate evidence that using a cane can help improve pain and function in knee osteoarthritis.
Why the wrong device height or poor fit can create fresh pain in the back, hips, or hands
But the wrong tool or poor fit can simply move the problem upstream. Suddenly the back complains, the hand aches, the shoulder tenses, and the user blames aging when the real villain is poor setup. Fit matters. Height matters. Instruction matters. A device should reduce compensation, not create a new parade of it.
How to think about shoes, insoles, and flooring without turning the house into a rehab warehouse
Shoes deserve more respect than they get. They are daily infrastructure. Flooring matters too, especially slick transitions and surfaces that increase cautious walking. Yet this does not mean turning the home into a rehab warehouse. The useful question is always: does this change reduce strain, improve steadiness, or make movement more repeatable? When cost or reimbursement enters the picture, it can be useful to understand HSA-eligible braces and supports before buying another item that may not solve the real movement problem.
Short Story: A man in his late seventies kept saying his knee brace “didn’t do much.” When his daughter described his day, the real problem emerged. He wore the brace only after the knee had already flared, shuffled around in worn slip-ons, and used a cane that was mostly a decorative object leaning by the door. Once the routine changed, the story changed. Shoes went by the bed.
The cane was fitted and used during the long hallway walk, not only on dramatic days. Meal prep happened seated for part of the task. Nothing looked miraculous. But within a week, the family stopped talking about pain as if it were random weather. They started talking about which choices made the knee cooperate. That shift was not small. It restored a sense of authorship, which is often half the battle in a house where pain has been setting the schedule.
Sleep, Swelling, and the Night Shift Nobody Plans For
Why knee osteoarthritis often feels louder at night even after a manageable day
Night pain has a cruel theatrical flair. The house is finally quiet, distractions are gone, and the knee steps into the spotlight. Sometimes evening discomfort reflects the day’s accumulated load. Sometimes swelling is part of the picture. Sometimes the problem is not pure pain but the combination of fatigue, stiffness after sitting, and awkward sleep positions.
How sleep position, evening activity, and swelling control affect next-morning pain
Evening pacing matters. So does the last hour before bed. A late burst of chores can echo into the night. Some people do better with a lighter evening routine, a brief reset after dinner, and a calmer transition before sleep. If swelling tends to build, it helps to notice patterns rather than guessing. The knee often leaves clues. Sleep problems after joint procedures can follow a different pattern, so readers recovering from surgery may also want to compare this with knee replacement pain management rather than treating every night ache as routine arthritis.
Why the trip to the bathroom at 2 a.m. is part of pain management too
This is where practical dignity matters. The night path is part of orthopedic pain management. Good lighting, a clear route, proper footwear or stable slippers, and a bed height that does not demand a squat at midnight are not cosmetic details. They are protective design. CDC fall-prevention guidance emphasizes that older adult falls are common and preventable.
- Reduce late evening overuse.
- Notice whether swelling is part of the pattern.
- Treat the bed-to-bathroom route like a safety project.
Apply in 60 seconds: Stand at the bedside tonight and check whether the route to the bathroom is lit, clear, and steady.
When the Problem Is Bigger Than the Knee
How fear of pain can shrink walking distance, confidence, and social life
Sometimes the knee is no longer the whole story. Fear enters. A person stops walking far because they dread the return trip. They decline outings because standing in line feels risky. Their world grows smaller not only from pain, but from anticipation of pain. That is a real loss, and it deserves real attention.
Why slower movement may reflect balance loss, fatigue, or medication effects, not just arthritis
It is also worth remembering that slower movement can reflect more than osteoarthritis. Balance changes, vision problems, medication effects, fatigue, deconditioning, low confidence, and other joint pain may all be woven in. When families attribute every change to “the knee,” they may miss solvable pieces of the puzzle. If symptoms keep showing up despite a reassuring image, normal X-ray but pain continues is a useful reminder that daily function and clinical context still matter.
When knee pain starts changing mood, independence, and willingness to leave the house
This is the threshold where a home plan should widen its lens. The question becomes not only “How do we calm the knee?” but “How do we protect independence and keep life from shrinking?” Sometimes that means clinical reassessment. Sometimes it means physical therapy. Sometimes it means reviewing medication effects. Sometimes it means admitting that a chair, a hallway, or a bathroom has become part of the diagnosis.
Show me the nerdy details
Knee OA often behaves as a systems problem in older adults. Pain can alter gait and reduce activity, which can reduce strength and confidence, which can raise fall risk and social withdrawal. The practical consequence is that intervention often works best when it targets several linked frictions at once rather than chasing a single symptom in isolation.
When to Seek Help Instead of Just “Managing It Better”
Rapid swelling, redness, heat, or fever that could signal something more serious
There is a difference between a rough arthritis day and a problem that needs prompt evaluation. Rapid swelling, redness, heat, fever, or dramatic worsening deserves attention sooner rather than later.
Pain that sharply worsens, buckling that increases, or a new inability to walk safely
Repeated buckling, increasing instability, or a new inability to walk safely should move the situation out of the casual-management category. The same goes for a fall, a sudden twist, or pain that feels distinctly different from the usual pattern. When the choice is unclear, comparing urgent care vs orthopedic clinic can help families decide where the problem belongs.
Repeated near-falls, sleep-breaking pain, or medication side effects that make daily life less safe
If pain keeps waking a person, if medication seems to worsen confusion or steadiness, or if near-falls are becoming a recurring plotline, it is time to escalate. These are not minor inconveniences. They are safety data.
Why “manageable” pain is no longer manageable when it starts stealing function
Here is the cleanest rule: pain stops being manageable when it steals function faster than your routine can protect it. That is the moment to bring in a clinician, therapist, or specialist rather than endlessly refining the same home tricks.
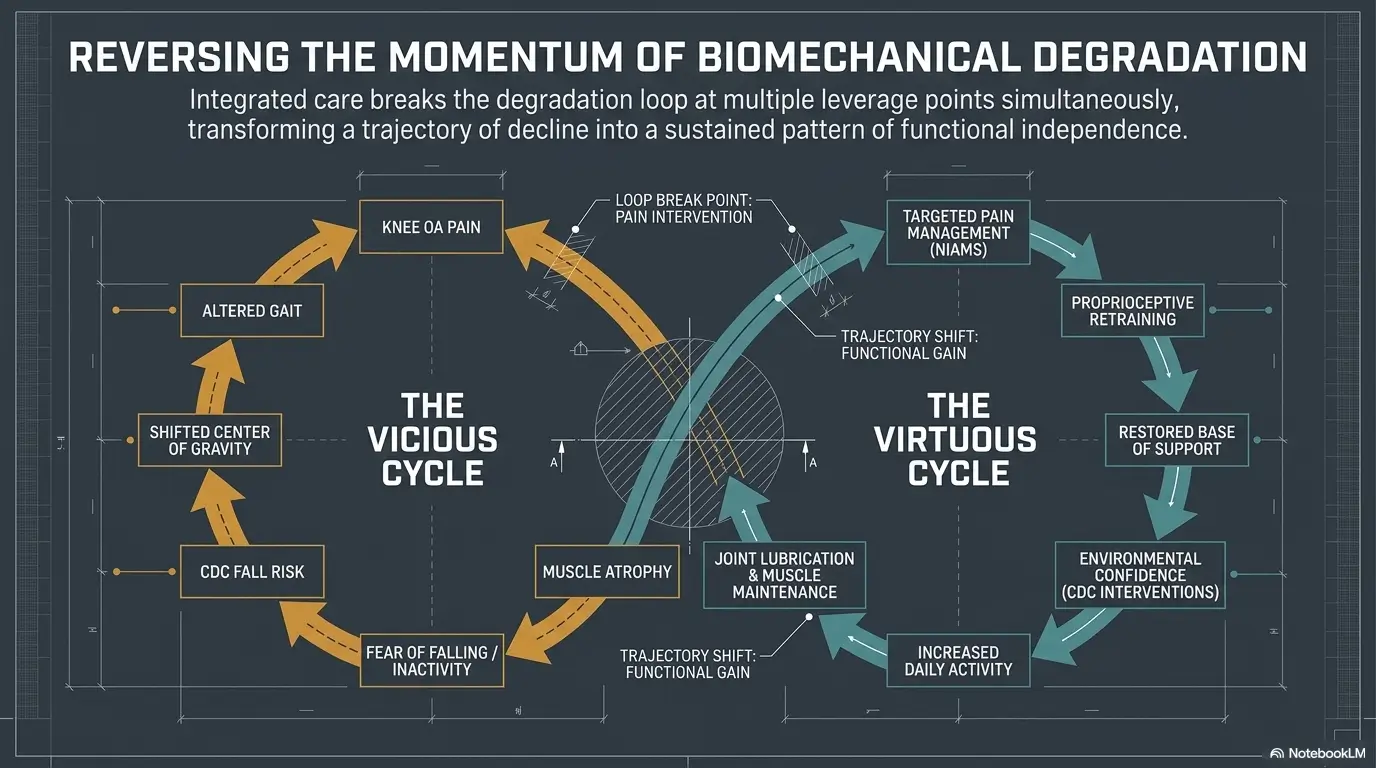
Next Step: Change One Friction Point Today
Pick the single daily moment that hurts or destabilizes the knee most, such as getting out of bed, rising from the toilet, or standing in the kitchen, and redesign that one moment first before trying to fix everything at once
The biggest trap in knee osteoarthritis management is trying to fix everything in one noble weekend. Better results usually come from choosing one friction point and making it noticeably easier. Not theoretically better. Actually easier.
Maybe the best first target is bed-to-bathroom. Maybe it is the main chair. Maybe it is kitchen standing during dinner prep. Pick the moment that most often causes pain, hesitation, or instability. Then redesign that moment with shameless practicality. Change the setup. Shorten the task. Add support. Adjust timing. Make the better choice the easier choice.
This closes the loop from the beginning: the real story was never only the knee. It was the chair, the turn, the darkness, the overlong standing block, the morning stiffness, the “good day” overreach. When you change one of those, you often change far more than one symptom. For people waiting on a bigger joint-care decision, pain management for seniors waiting on joint care can help turn that waiting period into a safer, more deliberate home plan.
- Choose the highest-frequency friction point first.
- Prefer boring fixes that work every day.
- Measure success by steadier function, not by drama.
Apply in 60 seconds: Write down one sentence: “The knee struggles most when I ______.” Start there.
Safety / Disclaimer: This content is informational and should not replace medical advice, diagnosis, or treatment. In older adults, knee pain management should balance relief with walking safety, medication safety, and fall prevention. New swelling, redness, fever, injury, severe calf pain, chest symptoms, or sudden trouble bearing weight should be evaluated promptly.
FAQ
What is the safest way for seniors to relieve knee osteoarthritis pain at home?
The safest home approach is usually a combination, not one trick: gentle movement, pacing, supportive footwear, heat or cold based on the knee’s pattern, and medication use reviewed with a clinician when needed. The aim is to reduce pain while protecting walking, transfers, and steadiness.
Is walking good or bad for seniors with knee osteoarthritis?
Walking is often helpful when the dose is reasonable. Both NIAMS and AAOS support exercise as part of osteoarthritis management, and lower-impact activity is generally favored over high-impact loading. Walking becomes less helpful when the dose is too large, the surface is poor, footwear is weak, or the knee is being asked to absorb a whole day’s ambition in one burst.
Should older adults use heat or ice for knee osteoarthritis pain?
Either may help, depending on the moment. Heat often works better for stiffness, especially first thing in the morning or before movement. Cold may help more when swelling or a “hot, puffy” feeling is part of the problem. NIAMS notes that both heat and cold therapies can lower joint pain.
What kind of shoes are best for seniors with arthritic knee pain?
The best shoes are usually supportive, stable, and easy to use without being floppy or slick. Look for steadiness, grip, and a fit that makes standing and walking feel more secure. A convenient shoe that increases wobble is not really convenient.
Can a knee brace actually help with osteoarthritis pain?
Sometimes, yes, but the result depends on the type of brace, the fit, and whether the brace is solving the real problem. A brace may help some people feel more supported during activity, but it is not a universal answer. It works best as part of a larger plan rather than as a lone hero prop. For stairs specifically, a hinged knee brace for stairs may be worth discussing if instability, confidence, and fit are the real issues.
When does knee osteoarthritis pain mean it is time to see a specialist?
Consider specialist evaluation when pain or stiffness keeps worsening, walking becomes less safe, the knee buckles more often, sleep is repeatedly disrupted, or home strategies and routine medical care are no longer preserving function. If symptoms change sharply or bring swelling, heat, redness, or fever, seek prompt evaluation rather than waiting.
How can seniors reduce knee pain when getting up from a chair?
Start with the chair itself. A higher, firmer seat usually makes rising easier than a low, soft one. Scoot forward, place feet under the body, use arm support if needed, and avoid twisting as you stand. If rising from one particular chair is always the problem, the chair may be the treatment target.
Why does knee osteoarthritis hurt more in the morning or at night?
Morning pain often reflects stiffness after rest or inactivity. Night pain can reflect the day’s accumulated load, swelling, and a less forgiving environment. If nighttime symptoms are frequent, look at evening pacing, sleep setup, and the night path to the bathroom rather than blaming the clock alone.
Last reviewed: 2026-04.
